Abstract
Introduction
Bisphosphonates (BPs) are one of the most often used drugs to lower fracture risk in osteoporosis patients; nonetheless, BPs have been linked to atypical femoral fracture (AFF). Teriparatide (TPTD) is a parathyroid hormone analogue and anabolic drug that may accelerate fracture repair. TPTD has been considered as a possible treatment for AFF, particularly those caused by BP use. We evaluate the effect of TPTD on AFF in this systematic review and meta-analysis.
Materials and methods
A thorough search of: Web of Science, Scopus, PubMed, and Cochrane was conducted on August 2, 2023. Trials evaluating the effect of TPTD on the incidence of: complete bone healing, non-union, early and delayed bone union, progression of incomplete AFF to complete AFF, and time to bone union were included. Using Review Manager (RevMan) version 5.4, the risk ratio (RR) and mean difference (MD) with the corresponding 95% confidence interval (CI) were estimated for dichotomous and continuous outcomes, respectively. The Newcastle–Ottawa Scale was used to assess the quality of studies.
Results
Eight studies met the eligibility criteria and were included in our analysis. TPTD significantly increased the incidence of early bone union (RR = 1.45, 95% CI [1.13, 1.87], P = 0.004) and time to bone union (MD = −1.56, 95% CI [−2.86, −0.26], P = 0.02) compared to the control group. No significant differences were observed in terms of complete bone healing (RR = 1.09, 95% CI [0.99, 1.13], P = 0.12), non-union (RR = 0.48, 95% CI [0.22, 1.04], P = 0.06), and progression of incomplete AFF to complete AFF (RR = 0.27, 95% CI [0.04, 1.97], P = 0.19).
Conclusions
TPTD is an effective therapy for enhancing and hastening healing following AFF, particularly in postoperative settings. Future large randomized clinical trials are needed to confirm or dispute the results.
Similar content being viewed by others
Introduction
Atypical femur fractures (AFFs) are a rare complication of anti-resorptive bisphosphonates; such as alendronate or zoledronic acid (BPs). They are used to treat osteoporosis and decrease hip and vertebral fractures. Long-term BP treatment has been linked to decreased bone turnover and remodeling, impairing healing capacity, and predisposing to AFF [1, 2]. The American Society for Bone and Mineral Research (ASBMR) [3] defines AFF; as a fracture that is located distal to the lesser trochanter and just proximal to the supracondylar flare and meets four of the five major criteria: (1) The fracture is associated with minimal or no trauma; (2) the fracture line originates from the lateral cortex and extends transversely or obliquely medially; (3) complete fractures involve both cortices with a medial spike or incomplete fractures involve only the lateral cortex; and (4) the fracture is non-comminuted or minimally comminuted; (5) The fracture site has localized periosteal or endosteal thickening of the lateral cortex (“beaking” or “flaring”).
AFF is frequently resistant to therapy, resulting in poor bone union and a high rate of implant failure [4, 5]. Therefore, AFF is considered a serious health issue with a difficult management and a financial burden on the patients. Patient concern about AFF complications has reduced bisphosphonate use by roughly half in the last decade [6, 7]. The benefits of bisphosphonate therapy in lowering fracture risk, however, outweigh the risk of the AFF. Bisphosphonate therapy reduces bone loss and fracture risk in osteoporosis patients by up to 50% [8]. Therefore, a more effective treatment for such a devastating complication should be sought.
The standard treatment for complete AFF, or intractable pain, is surgery with intramedullary nailing in addition to medical management which includes BPs cessation and assessing dietary calcium and vitamin D status and prescribing adequate supplementation [3]. For incomplete AFF with mild to moderate pain, a trial of conservative therapy with limited weight-bearing could be trialed first [3, 9]. However, surgical treatment is associated with delayed healing and a high rate of revision surgery, whereas conservative treatment typically yields poor results [10, 11].
Teriparatide (TPTD) is an anabolic agent and parathyroid hormone analogue that promotes fracture healing. It is the only FDA-approved anabolic bone in the United States that has been shown to stimulate bone formation and remodeling, thereby accelerating typical fracture healing [12, 13]. TPTD may be a promising treatment for promoting healing of atypical femoral fractures, either alone or in combination with surgical fixation or conservative therapy.
TPTD has been evaluated in several reports; however, the population in most of the available evidence is small, making it difficult to draw firm conclusions about the efficacy of TPTD treatment of AFF patients. In this paper, we conduct a systematic review (SR) and meta-analysis (MA) to determine whether (TPTD) has a significant impact on the incidence of bone union and time to bone union in cases with AFF and to aid in the development of clear guidelines for its use and management of AFF.
Methods
The authors followed the PRISMA standards for reporting systematic reviews and meta-analyses of randomized controlled trials (RCTs) [14]. This systematic review was registered in the International Prospective Register of Systematic Reviews (PROSPERO), registration identifier CRD42023460067.
Eligibility criteria
This SR and MA included studies based on the PICOS criteria: patients, intervention, control, outcomes, and study design. The patients of interest were patients with AFFs. The control group consisted of patients who received everything in the intervention group except for TPTD. The studies must report the results of the outcomes of interest to be included. Given the scarcity of controlled studies on the effect of TPTD on AFFs, we searched for studies whose designs were randomized controlled trials as well as comparative observational, prospective, and retrospective studies. There were no restrictions on race, country, publication date, or follow-up duration. To increase our sample size, we included groups with complete or incomplete AFFs, unilateral or bilateral AFFs, and regardless of the site of the femur fracture, such as subtrochanteric or diaphyseal. We included only studies that assessed TPTD after the occurrence of AFFs and were either treated with surgery or conservatively, such as with BP cessation, dietary calcium, and vitamin D.
We excluded single-arm studies, animal studies, conference abstracts, non-English papers, and studies that did not report our outcomes of interest separately for the TPID group.
Information sources
Relevant articles were identified through a comprehensive search of the PubMed, Web of Science, Cochrane, and Scopus databases from inception to August 2, 2023. Other relevant studies were found by searching the reference lists of the eligible papers.
Search strategy
A search was conducted in PubMed, Web of Science, Scopus, and Cochrane for comparative studies published using a combination of the following terms: “teriparatide”, “atypical”, “femur”, and “fracture”. There were no filters applied. Supplementary Table 1 contains the complete search strategy for each database.
Selection process
All records were pooled using Endnote. The data were exported to an Excel sheet, which was subsequently submitted in two stages to find the eligible studies. The title and abstract screening step was carried out first, and records that passed this stage were moved to the full-text screening stage. It is worth noting that the eligibility of each article in each phase was independently examined by two authors. Any disagreements were settled by a third senior author.
Data collection process
The lead author prepared formatted Excel sheets in which the review authors extracted baseline data and study characteristics, as well as quality assessment and outcomes of interest. Two authors extracted data from each study independently and then discussed it. Any disagreements were settled by a third senior author. Any incomplete or incompatible data were handled using the Cochrane Handbook’s suggested methods [15]
Data items (outcomes)
The primary outcomes were the incidence of complete bone healing and the time to bone union. Complete bone healing was defined as bridging across three or four cortices and/or disappearance of a visible fracture line on standard antero-posterior and lateral femoral radiographs, and/or a clinical lack of pain at the fracture site on palpation and weight-bearing [16, 17]. It included the incidence of bone healing as reported at the end of the study, regardless of how long it took for the healing to occur. Secondary outcomes included the incidence of early bone union, the incidence of delayed union, the incidence of progression to a complete fracture, and the incidence of non-union. Early bone union was defined if the fracture healed within 6 months. Delayed union was defined as the lack of evidence of bone union within 6 months. Non-union was defined as a fracture that did not achieve union at the end of the study.
Data items (other variables)
Two authors independently extracted study characteristics and baseline data. Study characteristics included: study ID, study design, follow-up duration, AFF diagnostic criteria applied by each study, laterality, degree, and site of the AFF, AFF treatment employed by the studies, such as surgery or conservative treatment, and description of the intervention group and control group. Baseline data included sample size, age, gender, duration of BP use, number of patients who used BP, number of patients who stopped BP after AFFs, and BP agent used.
Quality assessment
Two authors independently assessed the quality of the included studies using Newcastle–Ottawa Scale [18]. The quality of the studies was determined by the overall score they received, which was as follows: very good (9–10 points), good (7–8 points), satisfactory (5–6 points), and unsatisfactory (0–4 points).
Effect measures and synthesis methods
Review Manager (RevMan) version 5.4 [28] was used to conduct all the analyses. All the data was collected as means ± standard deviation (SD), or event and total for continuous and dichotomous outcomes, respectively. The continuous outcome data of time to union was measured using the inverse variance statistic method and reported as mean differences with a 95% confidence interval (CI), and the Mantel–Haensze equation to calculate the pooled RR and 95% CI was used for the remaining dichotomous outcomes. Cochrane’s Q test and the I2 statistic were used to assess heterogeneity. Significant heterogeneity was considered if the P value was less than 0.1 and the I2 was greater than 60%. We used the random effects model regardless of heterogeneity due to differences in studies and patient characteristics, as well as limited data, which did not justify assuming the presence of a true effect size among the included studies and using the fixed effects model. To solve and identify the source of heterogeneity, the leave-one-out strategy was employed. Subgroup analyses were carried out to determine the impact of TPTD on surgically treated cases and cases with complete fractures.
Results
Study selection
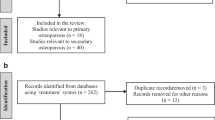
The database search yielded a total of 333 records. After duplicates were removed, 206 records were entered into the selection process and evaluated for eligibility criteria. Finally, our study included eight eligible studies [16, 17, 19,20,21,22,23,24]. Figure 1 shows the detailed process of search strategy results and study selection.

From: Page et al. [25]
A flowchart shows the detailed process of the search strategy and study selection.
Study characteristics
The meta-analysis included six retrospective studies [17, 19,20,21,22,23,24] and one prospective study [16], representing a total of 238 patients, 86 of whom received teriparatide and 152 of whom did not. The majority of the included studies were conducted on Asian populations, with the exception of Shin et al. [21] and Chiang et al. [16], which were conducted in the USA and Australia, respectively. One study [22] included patients with incomplete fractures; three studies [17, 19, 24] included patients with complete AFFs; and one study [21] included patients with complete AFFs; however, six patients suffered from contralateral incomplete fractures. In two studies [17, 23], the site of the fracture was diaphyseal, while the majority of the rest of the studies included both diaphyseal and subtrochanteric fractures. Except for Cho et al. [17], which addressed only unilateral fractures, all other studies included both unilateral and bilateral fractures. All patients were treated surgically in five studies [17, 19,20,21, 24], conservatively in one [22], and surgically or conservatively in the remaining two [16, 23], one of which reported the results separately for patients treated conservatively or surgically [23]. The summary of the study characteristics are shown in Table 1. Almost all of the patients were old females who had been taking BPs prior to the onset of AFFs but had stopped taking them after the onset of AFFs. The most commonly used BP drug was alendronate. The patients characteristics are summarised in Table 2.
Quality assessment
All of the studies included were of good quality (7–8 points). Seven studies had a total of eight points [16, 17, 19,20,21, 23, 24], while only one study received seven points [22]. The quality assessment of the studies included is shown in Supplementary Table 2.
Results of syntheses
Incidence of complete healing
The analysis included eight studies [16, 17, 19,20,21,22,23,24], with a total of 91 patients in the teriparatide arm and 154 patients in the non-teriparatide arm. The analysis showed insignificant increase in the incidence of complete bone healing in patients who received teriparatide compared to those who didn’t (RR = 1.09, 95% CI [0.99, 1.13], P = 0.12). The pooled analysis was homogenous (P = 0.56, I2 = 0%) (Fig. 2).
Time to bone union (months)
The analysis included six studies [17, 19,20,21, 23, 24], with a total of 83 patients in the teriparatide arm and 106 patients in the non-teriparatide arm. The time required for bone union to occur was significantly reduced by TPTD (MD = −1.56, 95% CI [−2.86, −0.26], P = 0.02) (Fig. 3a). The pooled analysis was heterogeneous (P = 0.04, I2 = 57%), which was resolved after the exclusion of Cho et al. [17] (P = 0.17, I2 = 38%) without significant effect on the overall estimate (MD = −2.36, 95% CI [−4.08, −0.63], P = 0.007) (Fig. 3b).
A forest plot shows the mean difference in the time to bone union (a). b The results after exclusion Cho et al. [17] study
Incidence of non-union
The analysis included seven studies [16, 19,20,21,22,23,24], with a total of 85 patients in the teriparatide arm and 142 patients in the non-teriparatide arm. The analysis showed that TPTD insignificantly reduced the incidence of bone non-union (RR = 0.48, 95% CI [0.22, 1.04], P = 0.06). The pooled analysis was homogenous (P = 0.78, I2 = 0%) (Fig. 4).
Incidence of early and delayed union
The analysis included three studies [19, 23, 24] with a total of 43 patients in the teriparatide arm and 63 patients in the non-teriparatide arm. The analysis found that the incidence of bone healing within 6 months of TPTD treatment in patients who received TPTD was significantly higher than that in the control group (RR = 1.45, 95% CI [1.13, 1.87], P = 0.004). The pooled analysis was homogenous (P = 0.97, I2 = 0%) (Fig. 5). The incidence of delayed bone healing, on the other hand, was significantly lower in the TPTD group compared to the control group (RR = 0.47, 95% CI [0.22, 0.99], P = 0.05). The pooled analysis was homogenous (P = 0.55, I2 = 0%) (Fig. 5).
Incidence of progression to complete fracture
The analysis included three studies [22,23,24] with a total of 12 patients in the teriparatide arm and 80 patients in the non-teriparatide arm. TPTD lowered the incidence of progression to complete fracture but insignificantly (RR = 0.27, 95% CI [0.04, 1.97], P = 0.19). The pooled analysis was homogenous (P = 0.84, I2 = 0%) (Fig. 6).
Subgroup analysis
Subgroup analysis showed that in patients who received surgical treatment, TPTD demonstrated a significantly shorter time to bone union (MD = −1.72, 95% CI [−3.09, −0.35], P = 0.01). Furthermore, it significantly increased the incidence of early bone union in patients undergoing surgical treatment and those with complete fractures (RR = 1.52 95% CI [1.16, 1.98], P = 0.002) and (RR = 1.54 95% CI [1.18, 2.01], P = 0.001). Table 3 shows the results of subgroup analysis.
Discussion
Osteoporosis is considered the most common bone disease [26]. BP is one of the most widely used medications to reduce fracture risk in osteoporosis patients. Although BP usage has been linked to the development of AFFs, ASBMR estimates the absolute risk of BP-associated AFFs to be low. Ranging from 3.2 to 50 cases per 100,000 person-years [3]. AFFs, if occurred, can be extremely burdensome for the patient and have a negative impact on their social and economic status. Therefore, a treatment should be proposed to cope with AFF situations related to the critical use of BPs. We conducted a systematic review and meta-analysis to look into TPTD as a potential therapy to alleviate this burden.
Teriparatide is a PTH analogue that binds to PTH type 1 receptors, increasing osteoblast survival and quantity, resulting in trabecular and cortical bone formation. This mechanism of action contrasts sharply with that of antiresorptive drugs, such as bisphosphonates, which reduce osteoclast-mediated bone resorption while also inhibiting new bone development because resorption and formation are inextricably linked processes [27]. Therefore, TPTD has been proposed as a potential therapy for BP-associated AFFs.
A previous literature review conducted by Gao et al., which investigated case reports and observational studies, concluded that TPTD enhances AFF healing by shortening the time to bone union and decreasing the incidence of non-union [28]. However, due to the limited data in their study, they didn’t perform a MA. Here, we included more controlled studies and performed the first MA to provide more robust, reliable data. The analysis indicated that TPTD can significantly reduce the time required for bone union while also increasing the likelihood of early bone union within 6 months. However, contrary to the conclusions of Gao et al., the effect of TPTD on reducing the incidence of non-union and increasing the likelihood of complete healing was not statistically significant.
In 2005, a study was conducted to measure the mean time needed for a typical femoral fracture to heal, which was approximately 3 months [29]. AFFs require a longer period of time. Egol et al. [29] conducted a retrospective study of 41 complete and displaced atypical bisphosphonate-associated femoral fractures treated surgically with intramedullary nails. The mean time of bone healing was 8.3 months. Our analysis suggests that using TPTD, this period could be reduced to less than 6 months.
Peich et al. 2011 employed TPTD to treat pubic bone fractures in elderly osteoporotic patients. According to their findings, the average time to bone union in the TPTD group was roughly 8 weeks, compared to nearly 13 weeks in the control group [30]. Nonetheless, Aspenberg et al. used TPTD to treat distal radius fractures in postmenopausal women in order to reduce the time required for bone union [12]. Therefore, our findings may not be exclusive to femoral fractures.
Gomberg et al. [29] used TPTD along with vitamin D and calcium to treat a 63-year-old postmenopausal female patient in an attempt to accelerate the healing process. And after one year, the patient no longer needed narcotics for her pain. Gomberg et al. [29] stated that the healing process could have been spontaneous and related to time. This is further supported by the fact that we didn’t find significant differences between TPTD and the control in terms of the incidence of complete healing at the end of the follow-up period. Therefore, TPTD may be considered if the healing process needs to be sped up. It should be noted, however, that the incidence of complete bone healing and nonunion in our study favored the teriparatide group, though this did not reach statistical significance, and larger trials are needed to confirm the findings.
Based on our subgroup analysis, teriparatide effectively increased the incidence of early bone healing and decreased the time to bone union in AFF after surgical repair, as well as in those with complete AFF. However, due to a lack of data, the outcomes of conservatively treated patients could not be evaluated. Miyakoshi et al. [23] performed a subgroup analysis based on treatment modality and discovered significant differences in healing time in surgically treated patients receiving TPTD versus the control group, but not in non-surgically treated patients receiving conservative therapy. However, the sample size was too small to draw solid conclusions. Therefore, our findings support the use of TPTD to accelerate bone healing postoperatively, regardless of the extent of the fracture. Future large trials are needed to assess the effect of TPTD on patients receiving conservative therapy instead of surgery.
The analysis revealed that TPTD insignificantly reduced the incidence of the progression of incomplete AFF to complete AFF. This could be attributed to the small sample size included in the analysis. However, it could refer to the inability of TPTD to heal conservatively treated incomplete AFFs and that it is only effective in postoperative settings. Further research is needed to address this question.
The findings have important implications for future guidelines and clinical decision-makers. TPTD can be considered in situations where the healing process of AFFs needs to be sped up. The patients can be given the option that healing may occur spontaneously, but TPTD will shorten the time needed for bone union to occur.
Strengths and limitations
This SR and MA benefit from a thorough search that includes the most recent relevant trials as well as all accessible data, which was either examined as primary, secondary, or exploratory outcomes. Furthermore, all of the pooled analyses were homogeneous, and we performed sensitivity analysis to test the results’ robustness in the presence of heterogeneity. However, our meta-analysis is not without limitations. The small sample size is the main concern. Furthermore, there were variations in the characteristics of the included studies and patients. However, we employed a random effect model to provide more robust results and performed a subgroup account for some of these variations. However, due to limited data, we couldn’t perform further subgroup analyses.
Conclusion
TPTD significantly shortened the time to bone union and increased the incidence of early bone healing compared to the control group. However, the effect on the incidence of overall complete healing or non-union is minimal. We present TPTD as a postoperative treatment to hasten and enhance the healing process. Further studies with a large sample size are required to validate or refute these findings.
Data availability
All data analyzed during this study are included in this published article or listed in references.
References
Geada N, Mafra I, Barroso R, Franco J (2014) Fracturas Femorais Atípicas e o Tratamento com Bifosfonatos: É um Factor de Risco? Acta Med Port 27:704–709. https://doi.org/10.20344/amp.5118
Schilcher J, Koeppen V, Aspenberg P, Michaëlsson K (2014) Risk of atypical femoral fracture during and after bisphosphonate use. N Engl J Med 371:974–976. https://doi.org/10.1056/NEJMc1403799
Shane E, Burr D, Abrahamsen B et al (2014) Atypical subtrochanteric and diaphyseal femoral fractures: second report of a task force of the American Society for bone and mineral research. J Bone Miner Res 29:1–23. https://doi.org/10.1002/jbmr.1998
Weil YA, Rivkin G, Safran O et al (2011) The outcome of surgically treated femur fractures associated with long-term bisphosphonate use. J Trauma Inj Infect Crit Care 71:186–190. https://doi.org/10.1097/TA.0b013e31821957e3
Chun-Man M, Man-Hong C, Wah-Bong W (2015) Surgical difficulties and complications in the treatment of bisphosphonate-related proximal femur fractures. J Orthop Trauma Rehabil 19:83–88. https://doi.org/10.1016/j.jotr.2014.06.002
Solomon DH, Johnston SS, Boytsov NN et al (2014) Osteoporosis medication use after hip fracture in U.S. Patients between 2002 and 2011. J Bone Miner Res 29:1929–1937. https://doi.org/10.1002/jbmr.2202
Jha S, Wang Z, Laucis N, Bhattacharyya T (2015) Trends in media reports, oral bisphosphonate prescriptions, and hip fractures 1996–2012: an ecological analysis. J Bone Miner Res 30:2179–2187. https://doi.org/10.1002/jbmr.2565
Black DM, Cummings SR, Karpf DB et al (1996) Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Lancet 348:1535–1541. https://doi.org/10.1016/S0140-6736(96)07088-2
Koh A, Guerado E, Giannoudis PV (2017) Atypical femoral fractures related to bisphosphonate treatment. Bone Joint J 99-B:295–302. https://doi.org/10.1302/0301-620X.99B3.BJJ-2016-0276.R2
Ha Y-C, Cho M-R, Park KH et al (2010) Is surgery necessary for femoral insufficiency fractures after long-term bisphosphonate therapy? Clin Orthop Relat Res 468:3393–3398. https://doi.org/10.1007/s11999-010-1583-2
Egol KA, Park JH, Prensky C et al (2013) Surgical treatment improves clinical and functional outcomes for patients who sustain incomplete bisphosphonate-related femur fractures. J Orthop Trauma 27:331–335. https://doi.org/10.1097/BOT.0b013e31827240ae
Aspenberg P, Genant HK, Johansson T et al (2010) Teriparatide for acceleration of fracture repair in humans: a prospective, randomized, double-blind study of 102 postmenopausal women with distal radial fractures. J Bone Miner Res 25:404–414. https://doi.org/10.1359/jbmr.090731
Anagnostis P, Gkekas NK, Potoupnis M et al (2019) New therapeutic targets for osteoporosis. Maturitas 120:1–6. https://doi.org/10.1016/j.maturitas.2018.11.010
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. PLoS Med 18:e1003583. https://doi.org/10.1371/journal.pmed.1003583
Higgins JPT, Thomas J, Chandler J et al (2019) Cochrane handbook for systematic reviews of interventions. Wiley, New Jersey
Chiang CY, Zebaze RMD, Ghasem-Zadeh A et al (2013) Teriparatide improves bone quality and healing of atypical femoral fractures associated with bisphosphonate therapy. Bone 52:360–365. https://doi.org/10.1016/j.bone.2012.10.006
Cho Y, Byun Y-S, Jo S, Shin J (2022) Plate fixation for atypical fractures of the femoral diaphysis. Clin Orthop Surg 14:178. https://doi.org/10.4055/cios21173
Luchini C, Stubbs B, Solmi M, Veronese N (2017) Assessing the quality of studies in meta-analyses: advantages and limitations of the Newcastle Ottawa Scale. World J Meta-Anal 5:80. https://doi.org/10.13105/wjma.v5.i4.80
Lee KJ, Yoo JJ, Oh KJ et al (2017) Surgical outcome of intramedullary nailing in patients with complete atypical femoral fracture: a multicenter retrospective study. Injury 48:941–945. https://doi.org/10.1016/j.injury.2017.02.036
Takakubo Y, Ohta D, Ishi M et al (2017) The incidence of atypical femoral fractures in patients with rheumatic disease: Yamagata prefectural committee of atypical femoral fractures (YamaCAFe) study. Tohoku J Exp Med 242:327–334. https://doi.org/10.1620/tjem.242.327
Shin WC, Moon NH, Jang JH et al (2019) A retrospective bicenter comparative study of surgical outcomes of atypical femoral fracture: potential effect of teriparatide on fracture healing and callus formation. Bone 128:115033. https://doi.org/10.1016/j.bone.2019.08.006
Png MA, Koh JSB, Mohan PC et al (2023) Factors affecting healing and progression of conservatively treated incomplete atypical femoral fractures: retrospective observational study. J Bone Miner Metab 41:61–73. https://doi.org/10.1007/s00774-022-01378-8
Miyakoshi N, Aizawa T, Sasaki S et al (2015) Healing of bisphosphonate-associated atypical femoral fractures in patients with osteoporosis: a comparison between treatment with and without teriparatide. J Bone Miner Metab 33:553–559. https://doi.org/10.1007/s00774-014-0617-3
Yeh WL, Su CY, Chang CW et al (2017) Surgical outcome of atypical subtrochanteric and femoral fracture related to bisphosphonates use in osteoporotic patients with or without teriparatide treatment. BMC Musculoskelet Disord 18:4–10. https://doi.org/10.1186/s12891-017-1878-5
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Sozen T, Ozisik L, Calik Basaran N (2017) An overview and management of osteoporosis. Eur J Rheumatol 4:46–56. https://doi.org/10.5152/eurjrheum.2016.048
Hodsman AB, Bauer DC, Dempster DW et al (2005) Parathyroid hormone and teriparatide for the treatment of osteoporosis: a review of the evidence and suggested guidelines for its use. Endocr Rev 26:688–703. https://doi.org/10.1210/er.2004-0006
Gao J, Liu X, Wu X et al (2023) A brief review and clinical evidences of teriparatide therapy for atypical femoral fractures associated with long-term bisphosphonate treatment. Front Surg. https://doi.org/10.3389/fsurg.2022.1063170
Gomberg SJ, Wustrack RL, Napoli N et al (2011) Teriparatide, vitamin D, and calcium healed bilateral subtrochanteric stress fractures in a postmenopausal woman with a 13-year history of continuous alendronate therapy. J Clin Endocrinol Metab 96:1627–1632. https://doi.org/10.1210/jc.2010-2520
Peichl P, Holzer LA, Maier R, Holzer G (2011) Parathyroid hormone 1–84 accelerates fracture-healing in pubic bones of elderly osteoporotic women. J Bone Jt Surg 93:1583–1587. https://doi.org/10.2106/JBJS.J.01379
Acknowledgements
Not applicable.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB).
Author information
Authors and Affiliations
Contributions
HMS validated the idea, conducted the search, took part in the analysis and wrote the results and methods section, formulated the extraction sheets, drafted the tables and figures, prepared the final manuscript version. KAA took part in the screening, data extraction, and quality assessment. SKK wrote the introduction, discussion, and conclusion sections. HAM took part in the screening, data extraction, and quality assessment. AA took part in the data extraction and quality assessment. MAF took part in the data extraction and quality assessment. DM reviewed and proofread the manuscript. HE supervised, reviewed, and edited the manuscript. All authors revised and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Salamah, H.M., Abualkhair, K.A., Kamal, S.K. et al. The effect of teriparatide on patients with atypical femur fractures: a systematic review and meta-analysis. Arch Orthop Trauma Surg 144, 1091–1106 (2024). https://doi.org/10.1007/s00402-023-05171-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05171-8