Abstract
Introduction
The aim of this study is to assess the association between the psoas muscle index (PMI) and total hip arthroplasty (THA) outcomes. This is a critical issue as sarcopenia has been associated with poor patient satisfaction post-THA.
Materials and methods
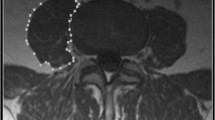
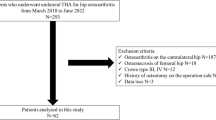
This was a retrospective case–control study of 205 THAs, with a mean follow-up of 3.6 (range, 2.0–5.5) years. Age, sex, serum immune markers, spinopelvic parameters, PMI (quantified as the cross-sectional area of the psoas, bilaterally, at L3 divided by the individual’s height squared), and patient-reported outcomes were compared between patients ‘with’ (n = 118) and ‘without’ (n = 87) achievement of a minimum clinically important difference (MCID) improvement in the EuroQol 5-Dimension (EQ-5D), post-THA. Logistic regression and receiver operating characteristic curve analyses were used to identify predictive factors.
Results
A ≥ MCID improvement in the EQ-5D was associated with the PMI (odds ratio, 0.75; 95% confidence interval, 0.63–0.91; P = 0.028), prognostic nutritional index (odds ratio, 0.85; 95% confidence interval, 0.45–0.94; P = 0.043), and age (odds ratio, 1.09; 95% confidence interval, 1.01–1.18; P = 0.044). After adjusting the PMI threshold to 4.0 cm2/m2 for females and 6.4 cm2/m2 for males, there were significant differences in serum factors (P = 0.041 for albumin and P = 0.016 for a prognostic nutritional index < 40), MCID (P < 0.001 for EQ-5D, P < 0.001 for low back pain, and P = 0.008 for the Hip Disability and Osteoarthritis Outcome Score Joint Replacement score), patient satisfaction (P = 0.003), and T1 pelvic angle (P = 0.030).
Conclusion
The PMI, which is associated with nutritional status and global sagittal spinal deformity, does predict THA outcomes. Therefore, it can be useful when discussing THA expectations with patients.





Similar content being viewed by others
Data availability
The datasets used and/or analyzed in this study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Hamaguchi Y, Kaido T, Okumura S et al (2016) Proposal for new diagnostic criteria for low skeletal muscle mass based on computed tomography imaging in Asian adults. Nutrition 32:1200–1205. https://doi.org/10.1016/j.nut.2016.04.003
Rollins KE, Gopinath A, Awwad A, Macdonald IA, Lobo DN (2020) Computed tomography-based psoas skeletal muscle area and radiodensity are poor sentinels for whole L3 skeletal muscle values. Clin Nutr 39:2227–2232. https://doi.org/10.1016/j.clnu.2019.10.003
Takiguchi K, Furuya S, Sudo M et al (2021) Prognostic effect of sarcopenia in colorectal cancer recurrence. Nutrition 91–92:111362. https://doi.org/10.1016/j.nut.2021.111362
Yasueda A, Sekido Y, Takeda T et al (2022) Sarcopenia hinders the decline in disease activity after surgery for people with Crohn’s disease: preliminary results. Nutrition 94:111526. https://doi.org/10.1016/j.nut.2021.111526
Kajiki Y, Tsuji H, Misawa H et al (2022) Psoas muscle index predicts osteoporosis and fracture risk in individuals with degenerative spinal disease. Nutrition 93:111428. https://doi.org/10.1016/j.nut.2021.111428
Bahat G, Turkmen BO, Aliyev S, Catikkas NM, Bakir B, Karan MA (2021) Cut-off values of skeletal muscle index and psoas muscle index at L3 vertebra level by computerized tomography to assess low muscle mass. Clin Nutr 40:4360–4365. https://doi.org/10.1016/j.clnu.2021.01.010
Ebbeling L, Grabo DJ, Shashaty M et al (2014) Psoas:lumbar vertebra index: central sarcopenia independently predicts morbidity in elderly trauma patients. Eur J Trauma Emerg Surg 40:57–65. https://doi.org/10.1007/s00068-013-0313-3
Mak D, Chisholm C, Davies AM, Botchu R, James SL (2020) Psoas muscle atrophy following unilateral hip arthroplasty. Skeletal Radiol 49:1539–1545. https://doi.org/10.1007/s00256-020-03447-3
Okamoto Y, Wakama H, Matsuyama J, Nakamura K, Otsuki S, Neo M (2023) Association of the psoas muscle index and sagittal spinal alignment with patient-reported outcomes after total hip arthroplasty: a minimum 5-year follow-up. J Arthroplasty 37:1111–1117. https://doi.org/10.1016/j.arth.2022.02.012
Anakwe RE, Jenkins PJ, Moran M (2011) Predicting dissatisfaction after total hip arthroplasty: a study of 850 patients. J Arthroplasty 26:209–213. https://doi.org/10.1016/j.arth.2010.03.013
Deckey DG, Verhey JT, Christopher ZK et al (2023) Discordance abounds in minimum clinically important differences in THA: a systematic review. Clin Orthop Relat Res 481:702–714. https://doi.org/10.1097/CORR.0000000000002434
Wyles CC, Heidenreich MJ, Jeng J, Larson DR, Trousdale RT, Sierra RJ (2017) The John Charnley award: redefining the natural history of osteoarthritis in patients with hip dysplasia and impingement. Clin Orthop Relat Res 475:336–350. https://doi.org/10.1007/s11999-016-4815-2
Ostelo RW, de Vet HC (2005) Clinically important outcomes in low back pain. Best Pract Res Clin Rheumatol 19:593–607. https://doi.org/10.1016/j.berh.2005.03.003
Danoff JR, Goel R, Sutton R, Maltenfort MG, Austin MS (2018) How much pain is significant? defining the minimal clinically important difference for the visual analog scale for pain after total joint arthroplasty. J Arthroplasty 33:S71–S75. https://doi.org/10.1016/j.arth.2018.02.029
Lyman S, Lee YY, McLawhorn AS, Islam W, MacLean CH (2018) What are the minimal and substantial improvements in the HOOS and KOOS and JR versions after total joint replacement? Clin Orthop Relat Res 476:2432–2441. https://doi.org/10.1097/CORR.0000000000000456
Goodman SM, Mehta BY, Kahlenberg CA et al (2020) Assessment of a satisfaction measure for use after primary total joint arthroplasty. J Arthroplasty 35:1792–1799. https://doi.org/10.1080/17453674.2019.1685284
Morvan G, Mathieu P, Vuillemin V et al (2011) Standardized way for imaging of the sagittal spinal balance. Eur Spine J 20(Suppl 5):602–608. https://doi.org/10.1007/s00586-011-1927-y
Nakamura K, Okamoto Y, Wakama H et al (2023) T1 pelvic angle is associated with rapid progression of hip arthrosis. Eur Spine J 32:1463–1470. https://doi.org/10.1007/s00586-023-07580-0
Fitzpatrick JA, Basty N, Cule M et al (2020) Large-scale analysis of iliopsoas muscle volumes in the UK Biobank. Sci Rep 10:20215. https://doi.org/10.1038/s41598-020-77351-0
Okuzu Y, Miyahara T, Goto K, Kuroda Y, Kawai T, Matsuda S (2022) Investigating sagittal spinal alignment, low back pain, and clinical outcomes after total hip arthroplasty for lumbar hyperlordosis: a retrospective study. Arch Orthop Trauma Surg 142:4007–4013. https://doi.org/10.1007/s00402-021-04266-4
Okamoto Y, Wakama H, Matsuyama J et al (2023) Clinical significance of relative pelvic version measurement as a predictor of low back pain after total hip arthroplasty [published online ahead of print]. Eur Spine J. https://doi.org/10.1007/s00586-023-07956-2
Hari A, Berzigotti A, Štabuc B, Caglevič N (2019) Muscle psoas indices measured by ultrasound in cirrhosis—preliminary evaluation of sarcopenia assessment and prediction of liver decompensation and mortality. Dig Liver Dis 51:1502–1507. https://doi.org/10.1016/j.dld.2019.08.017
Mjaaland KE, Kivle K, Svenningsen S, Nordsletten L (2019) Do Postoperative results differ in a randomized trial between a direct anterior and a direct lateral approach in THA? Clin Orthop Relat Res 477:145–155. https://doi.org/10.1097/CORR.0000000000000439
Arbanas J, Pavlovic I, Marijancic V et al (2013) MRI features of the psoas major muscle in patients with low back pain. Eur Spine J 22:1965–1971. https://doi.org/10.1007/s00586-013-2749-x
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
Funding
This study was supported by the Grants-in-Aid for Scientific Research of Japan Society KAKENHI for the Promotion of Science, Grant Number 21K09239.
Author information
Authors and Affiliations
Contributions
YO, HW, JM and SO designed the study. JM, KN and TS obtained the data. YO wrote the initial draft. YO and TS performed the statistical analysis. MN and YO ensured the accuracy of the data and analyses. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Consent to participate
Written, informed consent was obtained from all patients prior to study enrolment.
Consent for publication
Written, informed consent was obtained from all patients for the publication of this study.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki (1964) and its subsequent amendments and was approved by the institutional review board of Osaka Medical and Pharmaceutical University hospital (approval number- 2020-098-1).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Okamoto, Y., Wakama, H., Matsuyama, J. et al. The psoas muscle index as a useful predictor of total hip arthroplasty outcomes. Arch Orthop Trauma Surg 144, 1763–1772 (2024). https://doi.org/10.1007/s00402-023-05146-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05146-9