Abstract
Introduction
Screw cut out and varus collapse are the most common complication of locked plate fixation of proximal humerus fractures. The purpose of this study was to compare dual plating and endosteal fibular allograft struts as augmentation strategies to prevent varus collapse.
Materials and methods
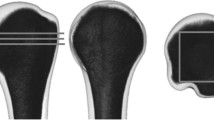
A trapezoidal osteotomy was created at the metaphysis to create a 2-part proximal humerus model in 18 paired shoulder specimens. Each specimen was assigned to group A, B, or C and was fixed with either a lateral locking plate, a lateral locking plate and anterior one-third tubular plate in an orthogonal 90/90 configuration, or a lateral locking plate with intramedullary fibular strut, respectively. The specimens were stressed in axial compression to failure. Displacement, elastic limit, ultimate load, and stiffness were recorded and calculated.
Results
There was no difference in mean cyclic displacement between the three groups (0.71 mm vs 0.89 mm vs 0.61 mm for Group A, B, C, respectively). Lateral plating demonstrated the greatest absolute and relative displacement at the elastic limit (5.3 mm ± 1.5 and 4.4 mm ± 1.3) without significance. The elastic limit or yield point was greatest for fibular allograft, Group C (1223 N ± 501 vs 1048 N ± 367 for Group B and 951 N ± 249 for Group A) without significance.
Conclusions
Dual plating of proximal humerus fractures in a 90–90 configuration demonstrates similar biomechanical properties as endosteal fibular strut allograft. Both strategies demonstrate superior stiffness to isolated lateral locked plating.





Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Mellstrand Navarro C, Brolund A, Ekholm C et al (2018) Treatment of humerus fractures in the elderly: a systematic review covering effectiveness, safety, economic aspects and evolution of practice. PLoS ONE 13(12):e0207815
Bell JE, Leung BC, Spratt KF et al (2011) Trends and variation in incidence, surgical treatment, and repeat surgery of proximal humeral fractures in the elderly. J Bone Joint Surg Am 93(2):121–131
Court-Brown CM, Garg A, McQueen MM (2001) The epidemiology of proximal humeral fractures. Acta Orthop Scand 72(4):365–371
Iglesias-Rodríguez S, Domínguez-Prado DM, García-Reza A et al (2021) Epidemiology of proximal humerus fractures. J Orthop Surg Res 16(1):402
Chandrappa MH, Hajibandeh S, Hajibandeh S (2017) Postoperative outcomes of initial varus versus initial valgus proximal humerus fracture: a systematic review and meta-analysis. J Clin Orthop Trauma 8(1):14–20
Sabesan VJ, Lombardo D, Petersen-Fitts G, Weisman M, Ramthun K, Whaley J (2017) National trends in proximal humerus fracture treatment patterns. Aging Clin Exp Res 29(6):1277–1283
Dey Hazra RO, Illner J, Szewczyk K et al (2022) Age-independent clinical outcome in proximal humeral fractures: 2-year results using the example of a precontoured locking plate. J Clin Med 11(2):408
Meier RA, Messmer P, Regazzoni P, Rothfischer W, Gross T (2006) Unexpected high complication rate following internal fixation of unstable proximal humerus fractures with an angled blade plate. J Orthop Trauma 20(4):253–260
Agudelo J, Schürmann M, Stahel P et al (2007) Analysis of efficacy and failure in proximal humerus fractures treated with locking plates. J Orthop Trauma 21(10):676–681
Lorenz G, Schönthaler W, Huf W, Komjati M, Fialka C, Boesmueller S (2021) Complication rate after operative treatment of three- and four-part fractures of the proximal humerus: locking plate osteosynthesis versus proximal humeral nail. Eur J Trauma Emerg Surg 47(6):2055–2064
Jost B, Spross C, Grehn H, Gerber C (2013) Locking plate fixation of fractures of the proximal humerus: analysis of complications, revision strategies and outcome. J Shoulder Elbow Surg 22(4):542–549
Dauwe J, Walters G, Van Eecke E, Vanhaecht K, Nijs S (2021) Osteosynthesis of proximal humeral fractures: a 1-year analysis of failure in a Belgian level-1 trauma centre. Eur J Trauma Emerg Surg 47(6):1889–1893
Kristensen MR, Rasmussen JV, Elmengaard B, Jensen SL, Olsen BS, Brorson S (2018) High risk for revision after shoulder arthroplasty for failed osteosynthesis of proximal humeral fractures. Acta Orthop 89(3):345–350
Dauwe J, Walters G, Holzer LA, Vanhaecht K, Nijs S (2020) Failure after proximal humeral fracture osteosynthesis: a one year analysis of hospital-related healthcare cost. Int Orthop 44(6):1217–1221
di Tullio PO, Giordano V, Souto E et al (2019) Biomechanical behavior of three types of fixation in the two-part proximal humerus fracture without medial cortical support. PLoS ONE 14(7):e0220523
Jabran A, Peach C, Ren L (2018) Biomechanical analysis of plate systems for proximal humerus fractures: a systematic literature review. Biomed Eng Online 17(1):47
Katthagen JC, Schwarze M, Meyer-Kobbe J, Voigt C, Hurschler C, Lill H (2014) Biomechanical effects of calcar screws and bone block augmentation on medial support in locked plating of proximal humeral fractures. Clin Biomech (Bristol, Avon) 29(7):735–741
Sproul RC, Iyengar JJ, Devcic Z, Feeley BT (2011) A systematic review of locking plate fixation of proximal humerus fractures. Injury 42(4):408–413
Warnhoff M, Jensen G, Dey Hazra RO, Theruvath P, Lill H, Ellwein A (2021) Double plating - surgical technique and good clinical results in complex and highly unstable proximal humeral fractures. Injury 52(8):2285–2291
Cheng H, Yu J, Dong Z et al (2021) Treatment of 2-part proximal humeral fractures in osteoporotic patients with medial calcar instability using a PHILOS plate plus an allogeneic fibula inserted obliquely—a retrospective study. Geriatr Orthop Surg Rehabil 12:21514593211050156
Court-Brown CM, Clement ND, Duckworth AD, Biant LC, McQueen MM (2017) The changing epidemiology of fall-related fractures in adults. Injury 48(4):819–824
Dey Hazra RO, Blach RM, Ellwein A, Katthagen JC, Lill H, Jensen G (2021) Latest trends in the current treatment of proximal humeral fractures—an analysis of 1162 cases at a level-1 trauma centre with a special focus on shoulder surgery. Z Orthop Unfall 160:287
Seide K, Triebe J, Faschingbauer M et al (2007) Locked vs. unlocked plate osteosynthesis of the proximal humerus—a biomechanical study. Clin Biomech (Bristol, Avon) 22(2):176–182
Egol KA, Ong CC, Walsh M, Jazrawi LM, Tejwani NC, Zuckerman JD (2008) Early complications in proximal humerus fractures (OTA Types 11) treated with locked plates. J Orthop Trauma 22(3):159–164
Dasari SP, Kerzner B, Fortier LM et al (2022) Improved outcomes for proximal humerus fracture open reduction internal fixation augmented with a fibular allograft in elderly patients: a systematic review and meta-analysis. J Shoulder Elbow Surg 31(4):884–894
Bae JH, Oh JK, Chon CS, Oh CW, Hwang JH, Yoon YC (2011) The biomechanical performance of locking plate fixation with intramedullary fibular strut graft augmentation in the treatment of unstable fractures of the proximal humerus. J Bone Joint Surg Br 93(7):937–941
Chow RM, Begum F, Beaupre LA, Carey JP, Adeeb S, Bouliane MJ (2012) Proximal humeral fracture fixation: locking plate construct ± intramedullary fibular allograft. J Shoulder Elbow Surg 21(7):894–901
Cui X, Chen H, Ma B, Fan W, Li H (2019) Fibular strut allograft influences reduction and outcomes after locking plate fixation of comminuted proximal humeral fractures in elderly patients: a retrospective study. BMC Musculoskelet Disord 20(1):511
Mathison C, Chaudhary R, Beaupre L, Reynolds M, Adeeb S, Bouliane M (2010) Biomechanical analysis of proximal humeral fixation using locking plate fixation with an intramedullary fibular allograft. Clin Biomech (Bristol, Avon) 25(7):642–646
Osterhoff G, Baumgartner D, Favre P et al (2011) Medial support by fibula bone graft in angular stable plate fixation of proximal humeral fractures: an in vitro study with synthetic bone. J Shoulder Elbow Surg 20(5):740–746
Neviaser AS, Hettrich CM, Beamer BS, Dines JS, Lorich DG (2011) Endosteal strut augment reduces complications associated with proximal humeral locking plates. Clin Orthop Relat Res 469(12):3300–3306
Pokhvashchev D, Knox R, Herring M, Herfat S, Tibrin Marmor M (2021) Comparison of fibula strut and calcium phosphate cement augmentation of the medial buttress in 2-part proximal humerus fractures reconstruction: a biomechanical study. Eur J Orthop Surg Traumatol (PMID: 34739600)
Manzi JE, Ruzbarsky JJ, Rauck RC, Gulotta LV, Dines JS, Dines DM (2020) Failed proximal humerus osteosynthesis using intramedullary fibular strut allograft conversion to reverse shoulder arthroplasty. Tech Hand Up Extrem Surg 24(1):7–12
Choi S, Kang H, Bang H (2014) Technical tips: dualplate fixation technique for comminuted proximal humerus fractures. Injury 45(8):1280–1282
Wanner GA, Wanner-Schmid E, Romero J et al (2003) Internal fixation of displaced proximal humeral fractures with two one-third tubular plates. J Trauma 54(3):536–544
Cassidy JT, Coveney E, Molony D (2019) “90/90” Plating of proximal humerus fracture-a technical note. J Orthop Surg Res 14(1):41
Li D, Lv W, Chen W et al (2022) Application of a lateral intertubercular sulcus plate in the treatment of proximal humeral fractures: a finite element analysis. BMC Surg 22(1):98
Hettrich CM, Boraiah S, Dyke JP, Neviaser A, Helfet DL, Lorich DG (2010) Quantitative assessment of the vascularity of the proximal part of the humerus. J Bone Joint Surg Am 92(4):943–948
Robinson CM, Stirling PHC, Goudie EB, MacDonald DJ, Strelzow JA (2019) Complications and long-term outcomes of open reduction and plate fixation of proximal humeral fractures. J Bone Joint Surg Am 101(23):2129–2139
Zlotolow DA, Catalano LW 3rd, Barron OA, Glickel SZ (2006) Surgical exposures of the humerus. J Am Acad Orthop Surg 14(13):754–765
Theopold J, Schleifenbaum S, Müller M et al (2018) Biomechanical evaluation of hybrid double plate osteosynthesis using a locking plate and an inverted third tubular plate for the treatment of proximal humeral fractures. PLoS ONE 13(10):e0206349
Acknowledgements
None.
Funding
Materials from DePuy Synthes. No biases related to this study.
Author information
Authors and Affiliations
Contributions
RP, JWM, CB, LV, and PM contributed to conceptualization; JRB, JWM, CB, LV, and PM contributed to methodology; JWM and GJD contributed to formal analysis and investigation; RP, JRB, JWM, GJD, R-ODH, and PM contributed to writing—original draft preparation; RP, JRB, JWM, GJD, R-ODH, and PM contributed to writing—review and editing; RP, JRB, JWM, CB, and PM contributed to funding acquisition; RP, JRB, CB, LV, and PM contributed to Resources; GJD, LV, and PM contributed to supervision.
Corresponding author
Ethics declarations
Conflict of interest
Leslie Vidal MD—Outside the submitted work, she reports receiving royalties and consultant payments from Smith and Nephew. She has affiliation with and receives research support from the Steadman Philippon Research Institute a 501(c)(3) non-profit institution supported financially by private donations and corporate support from the following entities: Arthrex, Ossur, Siemens, Smith & Nephew, DOD, and DJO. Peter Millett MD—Outside the submitted work, he reports receiving royalties and consultant payments from Arthrex and owns stock in Vumedi. He receives IP royalties from MedBridge and Springer Publishing; he is a part owner of ProofPoint Biologics. He has affiliation with and receives research support from the Steadman Philippon Research Institute a 501(c)(3) non-profit institution supported financially by private donations and corporate support from the following entities: Arthrex, Ossur, Siemens, Smith & Nephew, DOD, and DJO. The remaining authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Patel, R., Brown, J.R., Miles, J.W. et al. Preventing varus collapse in proximal humerus fracture fixation: 90–90 dual plating versus endosteal fibular allograft strut. Arch Orthop Trauma Surg 143, 4653–4661 (2023). https://doi.org/10.1007/s00402-022-04738-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04738-1