Abstract
Introduction
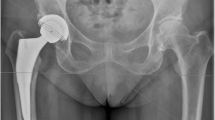
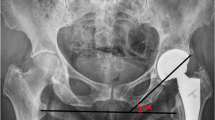
Total hip arthroplasty (THA) after rotational acetabular osteotomy (RAO) is technically demanding because of the characteristic acetabular morphology after RAO. The present study aimed to investigate the differences in the three-dimensional cup position between THA after RAO and primary THA.
Materials and methods
We analysed the pre-operative and post-operative computed tomography (CT) data of 120 patients (20 patients after RAO and 100 patients without a history of RAO) who underwent THA between January 2017 and June 2018. We evaluated radiographic parameters, including acetabular anteversion, antero-posterior distance at the level of the femoral head centre, the presence of anterior acetabular osteophyte and/or rotated fragment during RAO from the CT data. Additionally, operative data and clinical scores were also evaluated.
Results
Although we found no significant differences in any clinical parameters, there were significant differences in radiographic parameters and operative data. The morphology of the acetabulum was significantly retroverted, and the antero-posterior distance was longer in patients after RAO, compared to the implanted cup. Additionally, longer operative time was necessary for such patients. These results reflect the atypical acetabular morphology after RAO, and emphasize that care should be taken to avoid anterior bony impingement and post-operative dislocation.
Conclusion
For cup implantation during THA after RAO, surgeons should acknowledge the atypical morphology of the acetabulum and not be misled by its visual shape.






Similar content being viewed by others
References
Ninomiya S, Tagawa H (1984) Rotational acetabular osteotomy for the dysplastic hip. J Bone Joint Surg Am 66:430–436. https://doi.org/10.2106/00004623-198466030-00017
Ninomiya S (1989) Rotational acetabular osteotomy for the severely dysplastic hip in the adolescent and adult. Clin Orthop Relat Res 247:127–137. https://doi.org/10.1097/00003086-198910000-00022
Nakamura S, Ninomiya S, Takatori Y, Morimoto S, Umeyama T (1998) Long-term outcome of rotational acetabular osteotomy; 145 hips followed for 10–23 years. Acta Orthop Scand 69:259–265. https://doi.org/10.3109/17453679809000926
Takatori Y, Ninomiya S, Nakamura S, Morimoto S, Moro T, Nagai I, Mabuchi A (2001) Long-term results of rotational acetabular osteotomy in patients with slight narrowing of the joint space on pre-operative radiographic findings. J Orthop Sci 6:137–140. https://doi.org/10.1007/s007760100061
Yasunaga Y, Ochi M, Shimogaki K, Yamamoto S, Iwamori H (2004) Rotational acetabular osteotomy for hip dysplasia: 61 hips followed for 8–15 years. Acta Orthop Scand 75:10–15. https://doi.org/10.1080/00016470410001708020
Yasunaga Y, Ochi M, Yamasaki T, Shoji T, Izumi S (2016) Rotational acetabular osteotomy for pre- and early osteoarthritis secondary to dysplasia provides durable results at 20 years. Clin Orthop Relat Res 474:2145–2153. https://doi.org/10.1007/s11999-016-4854-8
Yuasa T, Maezawa K, Kaneko K, Nozawa M (2017) Rotational acetabular osteotomy for acetabular dysplasia and osteoarthritis: a mean follow-up of 20 years. Arch Orthop Trauma Surg 137:465–469. https://doi.org/10.1007/s00402-017-2636-8
Okano K, Yamada K, Takahashi K, Enomoto H, Osaki M, Shindo H (2010) Joint congruency in abduction before surgery as an indication for rotational acetabular osteotomy in early hip osteorothritis. Int Orthop 34:27–32. https://doi.org/10.1007/s00264-009-0734-09
Yasunaga Y, Yamasaki T, Ochi M (2012) Patient selection criteria for periacetabular osteotomy or rotational acetabular osteotomy. Clin Orthop Relat Res 470:3342–3354. https://doi.org/10.1007/s11999-012-2516-z
Tanaka T, Moro T, Ishikura H, Hashikura K, Kaneko T, Tanaka S (2021) Characteristics of three-dimensional acetabular morphology of patients with excellent outcome after rotational acetabular osteotomy over 20 years. J Orthop Surg Res 16:192. https://doi.org/10.1186/s13018-021-02346-0
Inaba Y, Kobayashi N, Ike H, Kubota S, Saito T (2016) Computer-assisted rotational acetabular osteotomy for patients with acetabular dysplasia. Clin Orthop Surg 8:99–105. https://doi.org/10.4055/cios.2016.8.1.99
Kaneuji A, Sugimori T, Ichiseki T, Fukui K, Takahashi E, Matsumoto T (2015) Rotational acetabular osteotomy for osteoarthritis with acetabular dysplasia: conversion rate to total hip arthroplasty within twenty years and osteoarthritis progression after a minimum of twenty years. J Bone Joint Surg Am 97:726–732. https://doi.org/10.2106/JBJS.N.00667
Ito H, Takatori Y, Moro T, Oshima H, Oka H, Tanaka S (2015) Total hip arthroplasty after rotational acetabular osteotomy. J Arthroplasty 30:403–406. https://doi.org/10.1016/j.arth.2014.10.002
Yuasa T, Maezawa K, Nozawa M, Kaneko K (2015) Total hip arthroplasty after previous rotational acetabular osteotomy. Eur J Orthop Surg Traumatol 25:1057–1060. https://doi.org/10.1007/s00590-015-1657-7
Crowe JF, Mani VJ, Ranawat CS (1979) Total hip replacement in congenital dislocation and dysplasia of the hip. J Bone Joint Am 61:15–23
Lee YK, Kim KC, Ha YC, Koo KH (2015) Combined anterior and posterior approach in total hip arthroplasty for Crowe IV dysplasia or ankylosed hips. J Arthroplasty 30:797–802. https://doi.org/10.1016/j.arth.2014.12.025
Kuribayashi M, Takahashi KA, Fujioka M, Ueshima K, Inoue S, Kubo T (2010) Reliability and validity of the Japanese Orthopaedic Association hip score. J Orthop Sci 15:452–458. https://doi.org/10.1007/s00776-010-1490-0
Peters CL, Beck M, Dunn HK (2001) Total hip arthroplasty in young adults after failed triple innominate osteotomy. J Arthroplasty 16:188–195. https://doi.org/10.1054/arth.2001.2090319
Hashemi-Nejad A, Haddad FS, Tong KM, Muirhead-Allwood SK, Catterall A (2002) Does Chiari osteotomy compromise subsequent total hip arthroplasty? J Arthroplasty 17:731–739. https://doi.org/10.1054/arth.2002.31974
Minoda Y, Kadowaki T, Kim M (2006) Total hip arthroplasty of dysplastichip after previous Chiari pelvic osteotomy. Arch Orthop Trauma Surg 126:394–400. https://doi.org/10.1007/s00402-006-0141-6
Tokunaga K, Aslam N, Zdero R, Schemitsch EH, Waddel JP (2011) Effect of prior salter or chiari osteotomy on THA with developmental hip dysplasia. Clin Orthop Relat Res 469:237–243. https://doi.org/10.1007/s11999-010-1375-8
Amanatullah DF, Stryker L, Schoenecker P, Taunton MJ, Clohisy JC, Trousdale RT, Sierra RJ (2015) Similar clinical outcomes for THAs with and without prior periacetabular osteotomy. Clin Orthop Relat Res 473:685–691. https://doi.org/10.1007/s11999-014-4026-7
Osawa Y, Hasegawa Y, Seki T, Amano T, Higuchi Y, Ishiguro N (2016) Significantly poor outcomes of total hip arthroplasty after failed periacetabular osteotomy. J Arthroplasty 31:1904–1909. https://doi.org/10.1016/j.arth.2016.02.056
Tamaki T, Oinuma K, Miura Y, Shiratsuchi H (2016) Total hip arthroplasty after previous acetabular osteotomy: comparison of three types of acetabular osteotomy. J Arthroplasty 31:172–175. https://doi.org/10.1016/j.arth.2015.07.018
Widmer KH, Zurfluh B, Morscher EW (2002) Load transfer and fixation mode of press-fit acetabular sockets. J Arthroplasty 17:926–935. https://doi.org/10.1054/arth.2002.34526
Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW (1988) Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol 15:1833–1840
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36): I. Conceptual framework and item selection. Med Care 30:473–483. https://doi.org/10.1097/00005650-199206000-00002
Dawson J, Fitzpatrick R, Carr A, Murray D (1996) Questionnaire on the perceptions of patients about total hip replacement. J Bone Joint Surg Br 78:185–190. https://doi.org/10.1302/0301-620X.78B2.0780185
Matsumoto T, Kaneuji A, Hiejima Y, Sugiyama H, Akiyama H, Atsumi T, Ishii M, Izumi K, Ichiseki T, Ito H, Okawa T, Ohzono K, Otsuka H, Kishida S, Kobayashi S, Sawaguchi T, Sugano N, Nakajima I, Nakamura S, Hasegawa Y, Fukuda K, Fujii G, Mawatari T, Mori S, Yasunaga Y, Yamaguchi M (2012) Japanese Orthopaedic Association Hip Disease Evaluation Questionnaire (JHEQ): a patient-based evaluation tool for hip-joint disease. The Subcommittee on Hip Disease Evaluation of the Clinical Outcome Committee of the Japanese Orthopaedic Association. J Orthop Sci 17:25–38. https://doi.org/10.1007/s00776-011-0166-8
Acknowledgments
No funding was received for this study. We would like to thank Editage (www.editage.com) for English language editing.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analyses were performed by Takeyuki Tanaka, Shin Asai, Kazuaki Hashikura, and Hisatoshi Ishikura. The first draft of the manuscript was written by Takeyuki Tanaka, and all authors commented on previous versions of the manuscript. Toru Moro and Sakae Tanaka supervised the study. All authors read and approved the final manuscript
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflict of interest to declare that are relevant to the content of this article
Ethics approval
The study was approved by the institutional review board of the University of Tokyo Hospital (number 2674-(3)). All investigations were conducted in conformity with ethical principles of research.
Informed consent
Informed consent was obtained from all patients prior to their participation in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tanaka, T., Moro, T., Asai, S. et al. Comparison between cup implantations during total hip arthroplasty with or without a history of rotational acetabular osteotomy. Arch Orthop Trauma Surg 142, 3539–3547 (2022). https://doi.org/10.1007/s00402-021-04253-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-04253-9