Abstract
Background
No consensus exists on the optimal treatment of proximal humeral fractures (PHFx). Uncertainty about surgical treatment in the older adults using locking plates (e.g., PHILOS) has emerged, due to a high number of complications. This study aimed to assess the impact of non-operative versus operative treatment of a PHFx on the level of self-dependence in our older population.
Methods
We included patients aged over 65 years with some level of self-dependence, treated at our hospital between 5/2011 and 4/2013 for isolated PHFx of AO subtypes A2, A3, and B1 for which either non-operative or surgical treatment using a PHILOS plate had been applied. The patients were questioned, examined, or interviewed via phone; AO fracture patterns and treatment were documented as well as level of self-dependence, complications, constant score (CSM), subjective shoulder value (SSV), quality of life (EQ-5D), and shoulder pain and disability index (SPADI).
Results
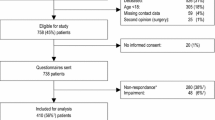
Patients with PHFx of AO subtypes A2, A3, or B1 that were either treated non-operative (n = 50) or operative by insertion of the PHILOS plate (n = 63) were included. Operative-treated patients were 3.3 times as likely to lose some level of independence (95% CI 0.39–28, p = 0.271). Shoulder motion, strength, and functional outcomes tended to be lower in operative-treated patients, with adjusted differences of, − 11 CMS points (95% CI – 23 to 2), − 9 SPADI points (95% CI − 18 to 0), and − 6% in SSV (95% CI − 17 to 5). Quality-of-life EQ-5D utility index was similar in both groups (mean − 0.04; 95% CI − 0.18 to 0.10).
Conclusion
In our study population, non-operatively treated older adults with an AO type A2, A3, B1 fracture of the proximal humerus tended to have a high chance to return to their premorbid level of independence, compared to patients treated with a locking plate. A change in the treatment algorithm for these PHFx may be carefully considered and further investigated in clinical practice.
Similar content being viewed by others
References
Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: a review. Injury 37:691–697
Palvanen M, Kannus P, Niemi S, Parkkari J (2006) Update in the epidemiology of proximal humeral fractures. Clin Orthop Relat Res 442:87–92
Hintermann B, Trouillier H, Schäfer D (2000) Rigid internal fixation of fractures of the proximal humerus in older patients. J Bone Jt Surg Br 82:1107–1112
Kristiansen B, Christensen SW (1986) Plate fixation of proximal humeral fractures. Acta Orthop Scand 57:320–323
Fu T, Xia C, Li Z, Wu H (2014) Surgical versus conservative treatment for displaced proximal humeral fractures in elderly patients: a meta-analysis. Inter J Clini Exp Med 7:4607
den Hartog D, de Haan J, Schep NW, Tuinebreijer WE (2010) Primary shoulder arthroplasty versus conservative treatment for comminuted proximal humeral fractures: a systematic literature review. Open Orthop J 4:87
Brorson S, Olsen BS, Frich LH, Jensen SL, Johannsen HV, Sørensen AK et al (2009) Effect of osteosynthesis, primary hemiarthroplasty, and non-surgical management for displaced four-part fractures of the proximal humerus in elderly: a multi-centre, randomised clinical trial. Trials 10:51
Brorson S, Rasmussen JV, Olsen BS, Frich LH, Jensen SL, Hrobjartsson A (2013) Reverse shoulder arthroplasty in acute fractures of the proximal humerus: a systematic review. Int J Shoulder Surg 7:70–78
Wanner GA, Wanner-Schmid E, Romero J, Hersche O, von Smekal A, Trentz O et al (2003) Internal fixation of displaced proximal humeral fractures with two one-third tubular plates. J Trauma 54:536–544
Kralinger F, Blauth M, Goldhahn J, Käch K, Voigt C, Platz A et al (2014) The influence of local bone density on the outcome of one hundred and fifty proximal humeral fractures treated with a locking plate. JBJS 96:1026–1032
Südkamp N, Bayer J, Hepp P, Voigt C, Oestern H, Kääb M et al (2009) Open reduction and internal fixation of proximal humeral fractures with use of the locking proximal humerus plate: results of a prospective, multicenter, observational study. JBJS 91:1320–1328
Meier RA, Messmer P, Regazzoni P, Rothfischer W, Gross T (2006) Unexpected high complication rate following internal fixation of unstable proximal humerus fractures with an angled blade plate. J Orthop Trauma 20:253–260
Brorson S, Frich LH, Winther A, Hróbjartsson A (2011) Locking plate osteosynthesis in displaced 4-part fractures of the proximal humerus: a systematic review of benefits and harms. Acta Orthop 82:475–481
Brorson S, Rasmussen JV, Frich LH, Olsen BS, Hróbjartsson A (2012) Benefits and harms of locking plate osteosynthesis in intraarticular (OTA type C) fractures of the proximal humerus: a systematic review. Injury 43:999–1005
Beks RB, Ochen Y, Frima H, Smeeing DPJ, van der Meijden O, Timmers TK et al (2018) Operative versus nonoperative treatment of proximal humeral fractures: a systematic review, meta-analysis, and comparison of observational studies and randomized controlled trials. J Am Shoulder Elbow Surg 27:1526–1534
Constant CR, Gerber C, Emery RJ, Sojbjerg JO, Gohlke F, Boileau P (2008) A review of the constant score: modifications and guidelines for its use. J Shoulder Elbow Surg 17:355–361
Rasanen P, Roine E, Sintonen H, Semberg-Konttinen V, Ryynanen OP, Roine R (2006) Use of quality-adjusted life years for the estimation of effectiveness of health care: a systematic literature review. Int J Technol Ass Health Care 22:235–241
Grobet C, Marks M, Tecklenburg L, Audige L (2018) Application and measurement properties of EQ-5D to measure quality of life in patients with upper extremity orthopaedic disorders: a systematic literature review. Arch Orthop Trauma Surg 138(7):953–961
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG (2009) Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42:377–381
Austin PC (2009) Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 28(3083):3107
Jawa A, Burnikel D (2016) Treatment of proximal humeral fractures: a critical analysis review. JBJS Rev 4:1–4
Xie L, Ding F, Zhao Z, Chen Y, Xing D (2015) Operative vs. non-operative treatment in complex proximal humeral fractures: a meta-analysis of randomized controlled trials. Springerplus 4:728
Handoll HH, Brorson S (2015) Interventions for treating proximal humeral fractures in adults. Cochrane Database Syste Rev 203:9
Frima H, Michelitsch C, Beks RB, Houwert RM, Acklin YP, Sommer C (2019) Long-term follow-up after MIPO Philos plating for proximal humerus fractures. Arch Orthop Trauma Surg 139:203–209
Ludwig K, von der Schulenburg JMG, Greiner W (2018) German value set for the EQ-5D–5L. Pharmacoeconomics 36:663–674
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Feissli, S., Audigé, L., Steinitz, A. et al. Treatment options for proximal humeral fractures in the older adults and their implication on personal independence. Arch Orthop Trauma Surg 140, 1971–1976 (2020). https://doi.org/10.1007/s00402-020-03452-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03452-0