Abstract
Purpose
Maintaining an appropriate hydration level by ingesting fluid in a hot environment is a measure to prevent heat-related illness. Caffeine-containing beverages, including green tea (GT), have been avoided as inappropriate rehydration beverages to prevent heat-related illness because caffeine has been assumed to exert diuretic/natriuretic action. However, the influence of caffeine intake on urine output in dehydrated individuals is not well documented. The aim of the present study was to examine the effect of fluid replacement with GT on body fluid balance and renal water and electrolyte handling in mildly dehydrated individuals.
Methods
Subjects were dehydrated by performing three bouts of stepping exercise for 20 min separated by 10 min of rest. They were asked to ingest an amount of water (H2O), GT, or caffeinated H2O (20 mg/100 ml; Caf-H2O) that was equal to the volume of fluid loss during the dehydration protocol; fluid balance was measured for 2 h after fluid ingestion.
Results
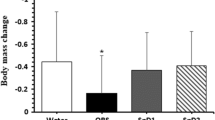
The dehydration protocol induced hypohydration by ~ 10 g/kg body weight (~ 1% of body weight). Fluid balance 2 h after fluid ingestion was significantly less negative in all trials, and the fluid retention ratio was 52.2 ± 4.2% with H2O, 51.0 ± 5.0% with GT, and 47.9 ± 6.2% with Caf-H2O; those values did not differ among the trials. After rehydration, urine output, urine osmolality, and urinary excretions of osmotically active substances, sodium, potassium and chloride were not different among the trials.
Conclusion
The data indicate that ingestion of GT or an equivalent caffeine amount does not worsen the hydration level 2 h after ingestion and can be effective in reducing the negative fluid balance for acute recovery from mild hypohydration.
Trial registration
ISRCTN53057185; retrospectively registered.




Similar content being viewed by others
Data availability
The data will be available from the corresponding author upon reasonable request.
References
Zhao Q, Guo Y, Ye T et al (2021) Global, regional, and national burden of mortality associated with non-optimal ambient temperatures from 2000 to 2019: a three-stage modelling study. Lancet Planet Heal 5:e415–e425. https://doi.org/10.1016/s2542-5196(21)00081-4
Gasparrini A, Guo Y, Hashizume M et al (2015) Mortality risk attributable to high and low ambient temperature: a multicountry observational study. Lancet 386:369–375. https://doi.org/10.1016/s0140-6736(14)62114-0
Nadel ER, Fortney SM, Wenger CB (1980) Effect of hydration state of circulatory and thermal regulations. J Appl Physiol Respir Environ Exerc Physiol 49:715–721
Mack GW, Cordero D, Peters J (2001) Baroreceptor modulation of active cutaneous vasodilation during dynamic exercise in humans. J Appl Physiol 90:1464–1473. https://doi.org/10.1152/jappl.2001.90.4.1464
Tokizawa K, Yasuhara S, Nakamura M et al (2010) Mild hypohydration induced by exercise in the heat attenuates autonomic thermoregulatory responses to the heat, but not thermal pleasantness in humans. Physiol Behav 100:340–345. https://doi.org/10.1016/j.physbeh.2010.03.008
Takamata A (2012) Modification of thermoregulatory response to heat stress by body fluid regulation. J Phys Fitness Sports Med 1:479–489
McKinley MJ, Martelli D, Pennington GL et al (2018) Integrating competing demands of osmoregulatory and thermoregulatory homeostasis. Physiology 33:170–181. https://doi.org/10.1152/physiol.00037.2017
Sawka MN, Burke LM, Eichner ER et al (2007) Exercise and fluid replacement. Medicine Sci Sports Exerc 39:377–390. https://doi.org/10.1249/mss.0b013e31802ca597
Casa DJ, Armstrong LE, Hillman SK et al (2000) National athletic trainers’ association position statement: fluid replacement for athletes. J Athl Training 35:212–224
Ishikawa T, Tamura H, Ishiguro H et al (2010) Effect of oral rehydration solution on fatigue during outdoor work in a hot environment: a randomized crossover study. J Occup Health 52:209–215. https://doi.org/10.1539/joh.l9156
Sorensen C, Hess J (2022) Treatment and prevention of heat-related illness. New Engl J Med 387:1404–1413. https://doi.org/10.1056/nejmcp2210623
Allen MD, Springer MB, Burg MB et al (2019) Suboptimal hydration remodels metabolism, promotes degenerative diseases, and shortens life. Jci Insight 4:e130949. https://doi.org/10.1172/jci.insight.130949
Stookey JD, Kavouras SA, Suh H, Lang F (2020) Underhydration is associated with obesity, chronic diseases, and death within 3 to 6 years in the U.S. population aged 51–70 years. Nutrients 12:905. https://doi.org/10.3390/nu12040905
Fukushima Y, Ohie T, Yonekawa Y et al (2009) Coffee and green tea as a large source of antioxidant polyphenols in the Japanese population. J Agr Food Chem 57:1253–1259. https://doi.org/10.1021/jf802418j
Musial C, Kuban-Jankowska A, Gorska-Ponikowska M (2020) Beneficial properties of green tea catechins. Int J Mol Sci 21:1744. https://doi.org/10.3390/ijms21051744
Abe SK, Inoue M (2021) Green tea and cancer and cardiometabolic diseases: a review of the current epidemiological evidence. Eur J Clin Nutr 75:865–876. https://doi.org/10.1038/s41430-020-00710-7
Zamani M, Kelishadi MR, Ashtary-Larky D et al (2023) The effects of green tea supplementation on cardiovascular risk factors: a systematic review and meta-analysis. Frontiers Nutrition 9:1084455. https://doi.org/10.3389/fnut.2022.1084455
Suzuki T, Pervin M, Goto S et al (2016) Beneficial effects of tea and the green tea catechin epigallocatechin-3-gallate on obesity. Molecules 21:1305. https://doi.org/10.3390/molecules21101305
Pervin M, Unno K, Ohishi T et al (2018) Beneficial effects of green tea catechins on neurodegenerative diseases. Molecules 23:1297. https://doi.org/10.3390/molecules23061297
Shirley DG, Walter SJ, Noormohamed FH (2002) Natriuretic effect of caffeine: assessment of segmental sodium reabsorption in humans. Clin Sci 103:461–466
Reyes CM, Cornelis MC (2018) Caffeine in the diet: country-level consumption and guidelines. Nutrients 10:1772. https://doi.org/10.3390/nu10111772
Dehydration and Heat Stroke. https://www.hopkinsmedicine.org/health/conditions-and-diseases/dehydration-and-heat-stroke#:~:text=These%20include%20the%20following%3A,these%20can%20lead%20to%20dehydration. Accessed 7 Mar 2023
Maughan RJ, Griffin J (2003) Caffeine ingestion and fluid balance: a review. J Hum Nutr Diet 16:411–420. https://doi.org/10.1046/j.1365-277x.2003.00477.x
Armstrong LE, Casa DJ, Maresh CM, Ganio MS (2007) Caffeine, fluid-electrolyte balance, temperature regulation, and exercise-heat tolerance. Exercise Sport Sci R 35:135–140. https://doi.org/10.1097/jes.0b013e3180a02cc1
Killer SC, Blannin AK, Jeukendrup AE (2014) No evidence of dehydration with moderate daily coffee intake: a counterbalanced cross-over study in a free-living population. PLoS ONE 9:e84154. https://doi.org/10.1371/journal.pone.0084154
Seal AD, Bardis CN, Gavrieli A et al (2017) Coffee with high but not low caffeine content augments fluid and electrolyte excretion at rest. Front Nutr 4:492–496. https://doi.org/10.3389/fnut.2017.00040
Maughan RJ, Watson P, Cordery PA et al (2015) A randomized trial to assess the potential of different beverages to affect hydration status: development of a beverage hydration index. Am J Clin Nutrition 103:717–723. https://doi.org/10.3945/ajcn.115.114769
Maughan RJ, Watson P, Cordery PAA et al (2017) Sucrose and sodium but not caffeine content influence the retention of beverages in humans under euhydrated conditions. Int J Sport Nutr Exe 29:51–60. https://doi.org/10.1123/ijsnem.2018-0047
Giersch GEW, Colburn AT, Morrissey MC et al (2020) Effects of sex and menstrual cycle on volume-regulatory responses to 24-h fluid restriction. AJP Regul Integr Comp Physiol 319:R560–R565. https://doi.org/10.1152/ajpregu.00173.2020
Maughan RJ, Leiper JB, Shirreffs SM (1997) Factors influencing the restoration of fluid and electrolyte balance after exercise in the heat. Brit J Sport Med 31:175. https://doi.org/10.1136/bjsm.31.3.175
Seery S, Jakeman P (2016) A metered intake of milk following exercise and thermal dehydration restores whole-body net fluid balance better than a carbohydrate–electrolyte solution or water in healthy young men. Brit J Nutr 116:1013–1021. https://doi.org/10.1017/s0007114516002907
Chang C-Q, Chen Y-B, Chen Z-M, Zhang L-T (2010) Effects of a carbohydrate-electrolyte beverage on blood viscosity after dehydration in healthy adults. Chin Med J-Peking 123:3220–3225
STANDARD TABLES OF FOOD COMPOSITION IN JAPAN (2020) (Eighth Revised Edition). Ministry of Education, Culture, Sports, Science and Technology-Japan, in Japanese
Takamata A, Mack GW, Gillen CM, Nadel ER (1994) Sodium appetite, thirst, and body fluid regulation in humans during rehydration without sodium replacement. Am J Physiol-Regul Integr Comp Physiol 266:R1493–R1502. https://doi.org/10.1152/ajpregu.1994.266.5.r1493
Nose H, Mack GW, Shi XR, Nadel ER (1988) Role of osmolality and plasma volume during rehydration in humans. J Appl Physiol 65:325–331
Kamijo Y-I, Ikegawa S, Okada Y et al (2012) Enhanced renal Na+ reabsorption by carbohydrate in beverages during restitution from thermal and exercise-induced dehydration in men. AJP Regul Integr Comp Physiol 303:R824–R833. https://doi.org/10.1152/ajpregu.00588.2011
Sawka MN, Montain SJ (2000) Fluid and electrolyte supplementation for exercise heat stress. Am J Clin Nutr 72:564S-S572
Greenleaf JE (1992) Problem: thirst, drinking behavior, and involuntary dehydration. Med Sci Sports Exerc 24:645. https://doi.org/10.1249/00005768-199206000-00007
Kanashima H, Yamane T, Takubo T et al (2005) Evaluation of noninvasive hemoglobin monitoring for hematological disorders. J Clin Lab Anal 19:1–5. https://doi.org/10.1002/jcla.20046
Clarke MM, Stanhewicz AE, Wolf ST et al (2019) A randomized trial to assess beverage hydration index in healthy older adults. Am J Clin Nutr 109:1640–1647. https://doi.org/10.1093/ajcn/nqz009
Mack GW, Weseman CA, Langhans GW et al (1994) Body fluid balance in dehydrated healthy older men: thirst and renal osmoregulation. J Appl Physiol 76:1615–1623. https://doi.org/10.1152/jappl.1994.76.4.1615
Funding
This study was funded by ITO EN, Ltd. and by Nara Women’s University.
Author information
Authors and Affiliations
Contributions
Conception and design were performed by AT, KM and TT; material, data collection and analysis were performed by AT, AO, MN, NK, SE, NS, AT, YN, MN, and TT; the first draft of the manuscript was written by AT; and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
T.T. is an employee of ITO EN, and this study was funded, in part, by ITO EN, Ltd. The study was conducted as a collaborative study, and the company had no influence over the scientific interpretation of the collected data or the publication of this article.
Ethics approval
All experimental protocols and procedures in the present study were approved by the Review Board on Human Experiments of Nara Women’s University (Approval #20–37).
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Takamata, A., Oka, A., Nagata, M. et al. Effect of fluid replacement with green tea on body fluid balance and renal responses under mild thermal hypohydration: a randomized crossover study. Eur J Nutr 62, 3339–3347 (2023). https://doi.org/10.1007/s00394-023-03236-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-023-03236-3