Abstract
Background
Depression is more common in females than in males and is 3–5 times more prevalent in patients with heart failure (HF) than in the general population. The 9-item Patient Health Questionnaire (PHQ-9) is a validated depression screening instrument; higher sum-scores predict adverse clinical outcomes. Sex- and gender differences in PHQ-9 symptom profile, diagnostic and prognostic properties, and impact on health-related quality of life (HRQOL) have not been comprehensively studied in HF patients.
Methods and results
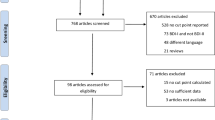
This post hoc analysis from the Interdisciplinary Network Heart Failure program enrolled 852/1022 participants (67 ± 13 years, 28% female) who completed the PHQ-9 at hospital discharge after cardiac decompensation. All had a left ventricular ejection fraction ≤ 40%. Women had a higher mean PHQ-9 sum-score than men (8.4 ± 5.6 vs. 7.4 ± 5.5; p = 0.027), and higher proportions rated the following items ≥ 2 (i.e., present on ≥ 50% of days): ‘feeling down, hopeless’ (25.8 vs. 18.0%; p = 0.011); ‘fatigue’ (51.9 vs. 37.2%; p < 0.001); and ‘trouble concentrating’ (21.6 vs. 15.4%; p = 0.032). A PHQ-9 sum-score ≥ 10 predicted increased mortality in women [hazard ratio 1.91 (95% confidence interval 1.06–3.43); p = 0.030] and men [2.10 (1.43–3.09); p < 0.001] and was associated with worse HRQOL (p < 0.001 for all comparisons). Sum-scores ≥ 10 predicted higher re-hospitalization rates in men only [1.35 (1.08–1.69); p = 0.008].
Conclusions
Differences in several PHQ-9 items indicated sex- or gender-specific depression symptomatology in HF. For both sexes, HRQOL and survival were worse when PHQ-9 sum-score was ≥ 10, but higher sum-scores predicted higher re-hospitalization rates in men only. Considering these specific aspects might help optimize care strategies in HF.



Similar content being viewed by others
References
Bleumink GS, Knetsch AM, Sturkenboom MC, Straus SM, Hofman A, Deckers JW, Witteman JC, Stricker BH (2004) Quantifying the heart failure epidemic: prevalence, incidence rate, lifetime risk and prognosis of heart failure The Rotterdam Study. Eur Heart J 25:1614–1619
Jessup M, Pina IL (2004) Is it important to examine gender differences in the epidemiology and outcome of severe heart failure? J Thorac Cardiovasc Surg 127:1247–1252
Peters SA, Huxley RR, Sattar N, Woodward M (2015) Sex differences in the excess risk of cardiovascular diseases associated with type 2 diabetes: potential explanations and clinical implications. Curr Cardiovasc Risk Rep 9:36
Levy D, Larson MG, Vasan RS, Kannel WB, Ho KK (1996) The progression from hypertension to congestive heart failure. JAMA 275:1557–1562
Vitale C, Fini M, Spoletini I, Lainscak M, Seferovic P, Rosano GM (2017) Under-representation of elderly and women in clinical trials. Int J Cardiol 232:216–221
Meyer S, Teerlink JR, Metra M, Ponikowski P, Cotter G, Davison BA, Felker GM, Filippatos G, Greenberg BH, Hua TA, Severin T, Qian M, Voors AA (2017) Sex differences in early dyspnea relief between men and women hospitalized for acute heart failure: insights from the RELAX-AHF study. Clin Res Cardiol 106:280–292
Clark AM, Wiens KS, Banner D, Kryworuchko J, Thirsk L, McLean L, Currie K (2016) A systematic review of the main mechanisms of heart failure disease management interventions. Heart 102:707–711
Murray JLLA (1996) The global burden of disease: a comprehensive assessment of mortality and disability from diseases, injuries and risk factors in 1990 and projected to 2020. Summary. Harvard School of Public Health, World Health Organization, Boston
Silverstein B, Levin E (2014) Differences in the developmental patterns of depression with and without additional somatic symptoms. Psychiatry Res 220:254–257
Rutledge T, Reis VA, Linke SE, Greenberg BH, Mills PJ (2006) Depression in heart failure a meta-analytic review of prevalence, intervention effects, and associations with clinical outcomes. J Am Coll Cardiol 48:1527–1537
Heo S, Moser DK, Widener J (2007) Gender differences in the effects of physical and emotional symptoms on health-related quality of life in patients with heart failure. Eur J Cardiovasc Nurs 6:146–152
Eastwood JA, Moser DK, Riegel BJ, Albert NM, Pressler S, Chung ML, Dunbar S, Wu JR, Lennie TA (2012) Commonalities and differences in correlates of depressive symptoms in men and women with heart failure. Eur J Cardiovasc Nurs 11:356–365
Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16:606–613
Kohlmann S, Gierk B, Murray AM, Scholl A, Lehmann M, Lowe B (2016) Base rates of depressive symptoms in patients with coronary heart disease: an individual symptom analysis. PLoS One 11:e0156167
Lichtman JH, Bigger JT Jr, Blumenthal JA, Frasure-Smith N, Kaufmann PG, Lesperance F, Mark DB, Sheps DS, Taylor CB, Froelicher ES (2009) AHA science advisory. Depression and coronary heart disease. Recommendations for screening, referral, and treatment. A science advisory from the American Heart Association Prevention Committee to the Council on Cardiovascular Nursing, Council on Clinical Cardiology, Council on Epidemiology and Prevention, and Interdisciplinary Council on Quality of Care Outcomes Research. Endorsed by the American Psychiatric Association. Prog Cardiovasc Nurs 24:19–26
Faller H, Stork S, Schowalter M, Steinbuchel T, Wollner V, Ertl G, Angermann CE (2007) Depression and survival in chronic heart failure: does gender play a role? Eur J Heart Fail 9:1018–1023
Moraska AR, Chamberlain AM, Shah ND, Vickers KS, Rummans TA, Dunlay SM, Spertus JA, Weston SA, McNallan SM, Redfield MM, Roger VL (2013) Depression, healthcare utilization, and death in heart failure: a community study. Circ Heart Fail 6:387–394
Piepenburg SM, Faller H, Gelbrich G, Stork S, Warrings B, Ertl G, Angermann CE (2015) Comparative potential of the 2-item versus the 9-item patient health questionnaire to predict death or rehospitalization in heart failure. Circ Heart Fail 8:464–472
Angermann CE, Stork S, Gelbrich G, Faller H, Jahns R, Frantz S, Loeffler M, Ertl G, Competence Network Heart F (2012) Mode of action and effects of standardized collaborative disease management on mortality and morbidity in patients with systolic heart failure: the Interdisciplinary Network for Heart Failure (INH) study. Circ Heart Fail 5:25–35
Faller H, Steinbuchel T, Schowalter M, Spertus JA, Stork S, Angermann CE (2005) [The Kansas City Cardiomyopathy Questionnaire (KCCQ)—a new disease-specific quality of life measure for patients with chronic heart failure]. Psychother Psychosom Med Psychol 55:200–208
Stork S, Handrock R, Jacob J, Walker J, Calado F, Lahoz R, Hupfer S, Klebs S (2017) Epidemiology of heart failure in Germany: a retrospective database study. Clin Res Cardiol 106:913–922
Opasich C, Tavazzi L, Lucci D, Gorini M, Albanese MC, Cacciatore G, Maggioni AP (2000) Comparison of one-year outcome in women versus men with chronic congestive heart failure. Am J Cardiol 86:353–357
Angermann CE, Gelbrich G, Stork S, Schowalter M, Deckert J, Ertl G, Faller H (2011) Somatic correlates of comorbid major depression in patients with systolic heart failure. Int J Cardiol 147:66–73
Faller H, Stork S, Schuler M, Schowalter M, Steinbuchel T, Ertl G, Angermann CE (2009) Depression and disease severity as predictors of health-related quality of life in patients with chronic heart failure—a structural equation modeling approach. J Card Fail 15:286–292 e282
Schowalter M, Gelbrich G, Stork S, Langguth JP, Morbach C, Ertl G, Faller H, Angermann CE (2013) Generic and disease-specific health-related quality of life in patients with chronic systolic heart failure: impact of depression. Clin Res Cardiol 102:269–278
Doyle F, McGee H, Conroy R, Conradi HJ, Meijer A, Steeds R, Sato H, Stewart DE, Parakh K, Carney R, Freedland K, Anselmino M, Pelletier R, Bos EH, de Jonge P (2015) Systematic review and individual patient data meta-analysis of sex differences in depression and prognosis in persons with myocardial infarction: a MINDMAPS study. Psychosom Med 77:419–428
Angermann CE, Gelbrich G, Stork S, Gunold H, Edelmann F, Wachter R, Schunkert H, Graf T, Kindermann I, Haass M, Blankenberg S, Pankuweit S, Prettin C, Gottwik M, Bohm M, Faller H, Deckert J, Ertl G (2016) Effect of escitalopram on all-cause mortality and hospitalization in patients with heart failure and depression: the MOOD-HF randomized clinical trial. Jama 315:2683–2693
O’Connor CM, Jiang W, Kuchibhatla M, Silva SG, Cuffe MS, Callwood DD, Zakhary B, Stough WG, Arias RM, Rivelli SK, Krishnan R (2010) Safety and efficacy of sertraline for depression in patients with heart failure: results of the SADHART-CHF (Sertraline Against Depression and Heart Disease in Chronic Heart Failure) trial. J Am Coll Cardiol 56:692–699
Heidenreich PA, Spertus JA, Jones PG, Weintraub WS, Rumsfeld JS, Rathore SS, Peterson ED, Masoudi FA, Krumholz HM, Havranek EP, Conard MW, Williams RE, Cardiovascular Outcomes Research C (2006) Health status identifies heart failure outpatients at risk for hospitalization or death. J Am Coll Cardiol 47:752–756
Spertus JA, Jones PG, Kim J, Globe D (2008) Validity, reliability, and responsiveness of the Kansas City Cardiomyopathy Questionnaire in anemic heart failure patients. Qual Life Res 17:291–298
Kosiborod M, Soto GE, Jones PG, Krumholz HM, Weintraub WS, Deedwania P, Spertus JA (2007) Identifying heart failure patients at high risk for near-term cardiovascular events with serial health status assessments. Circulation 115:1975–1981
Sullivan M, Levy WC, Russo JE, Spertus JA (2004) Depression and health status in patients with advanced heart failure: a prospective study in tertiary care. J Card Fail 10:390–396
Manea L, Gilbody S, McMillan D (2012) Optimal cut-off score for diagnosing depression with the Patient Health Questionnaire (PHQ-9): a meta-analysis. CMAJ 184:E191–E196
Lesperance F, Frasure-Smith N, Talajic M, Bourassa MG (2002) Five-year risk of cardiac mortality in relation to initial severity and one-year changes in depression symptoms after myocardial infarction. Circulation 105:1049–1053
Acknowledgements
English language editing assistance was provided by Nicola Ryan, BSc, independent medical writer.
Funding
This study was funded by the Federal Ministry of Education and Research (BMBF), Grant 01GL0304, by the Competence Network Heart Failure Germany (grants 01GI0205 and 01GI1202A), and by the Comprehensive Heart Failure Center Würzburg (Grants 01EO1004 and 01EO1504).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors report any conflicts of interest, including any financial relationship with industry, relevant to this manuscript.
Rights and permissions
About this article
Cite this article
Piepenburg, S.M., Faller, H., Störk, S. et al. Symptom patterns and clinical outcomes in women versus men with systolic heart failure and depression. Clin Res Cardiol 108, 244–253 (2019). https://doi.org/10.1007/s00392-018-1348-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-018-1348-6