Abstract
Purpose
To investigate the benefits of surgery alone and postoperative chemotherapy in elderly and non-elderly patients with appendiceal mixed neuroendocrine non-neuroendocrine neoplasms (MiNENs) and analyze the factors affecting the prognosis of patients with MiNEN of the appendix.
Methods
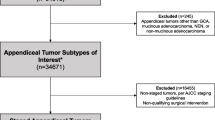
Based on the Surveillance, Epidemiology, and End Results database (SEER) of the National Cancer Institute of the USA, 389 patients with appendiceal MiNENs from 2000 to 2016 were collected. All patients were distributed in the elderly group (≥ 60 years old) and the non-elderly group (< 60 years old) according to their age. The prognosis of the two groups of patients who received simple surgery and postoperative chemotherapy was analyzed and compared. The two treatment methods of the two tranches were matched by propensity score matching method. The effect of different treatment ways on the prognosis of sick persons was compared. The survivorship curves were painted by the Kaplan Meier method, log rank test was used to analyze the subsistence discrepancy of each group, and COX proportional risk model was used to analyze the factors affecting the prognosis of patients with appendiceal MiNENs.
Results
No matter the overall survival rate (OS) or cancer-specific mortality (CSM) of the two treatment schemes, the prognosis of patients in the only surgery group was meaningfully higher than that in the postoperative chemotherapy group, with statistically significant difference in component comparison (χ2 = 16.496, χ2 = 16.860, P < 0.001). After propensity score matching of patients in each group, there was no striking discrepancy in the OS of patients in the only surgery group compared with those in the postoperative chemotherapy group, regardless of whether they were elderly patients or non-elderly patients (χ2 = 3.205, χ2 = 1.521, all P > 0.05), the CSM consequences are fitting in with the OS. The consequences of the multivariate COX regression model showed that age (≥ 60 years old), sex (female), high histological grade, and lymph node positive were all the influencing factors for the poor OS of patients with MiNEN; the CSM results are consistent with the OS.
Conclusion
For patients with appendix MiNEN, whether elderly or non-elderly patients (especially for non-elderly patients), surgical treatment may be a better choice.




Similar content being viewed by others
Data availability
The data is available.
References
Vinagre J, Pinheiro J, Martinho O, Reis RM, Preto J, Soares P et al (2020) A 30-year long-term experience in appendix neuroendocrine neoplasms-granting a positive outcome. Cancers (Basel) 12(6). https://doi.org/10.3390/cancers12061357
Shi H, Qi C, Meng L, Yao H, Jiang C, Fan M et al (2020) Do neuroendocrine carcinomas and mixed neuroendocrine-non-neuroendocrine neoplasm of the gastrointestinal tract have the same prognosis? A seer database analysis of 12,878 cases. Ther Adv Endocrinol Metab 11:1905108416. https://doi.org/10.1177/2042018820938304
Zheng M, Li T, Li Y, Zhang T, Zhang L, Ma W et al (2020) Survival profile and prognostic factors for appendiceal mixed neuroendocrine non-neuroendocrine neoplasms: a seer population-based study. Front Oncol 10:1660. https://doi.org/10.3389/fonc.2020.01660
Brathwaite S, Yearsley MM, Bekaii-Saab T, Wei L, Schmidt CR, Dillhoff ME et al (2016) Appendiceal mixed adeno-neuroendocrine carcinoma: a population-based study of the surveillance, epidemiology, and end results registry. Front Oncol 6:148. https://doi.org/10.3389/fonc.2016.00148
Chinese experts consensus on multidisciplinary comprehensive treatment of appendiceal neoplasm (2021) Colorectal Cancer Committee of Chinese Medical Doctor Association. Chinese Electron J Colorectal Dis 2021;10(3):225–31. https://doi.org/10.3877/cma.j.issn.2095-3224.2021.03.001
Huachong Ma, Jianhao Z, Yuhan L, Yuqing D, Luyin Z, Rui L et al (2021) Analysis of correlation factors and risk prediction for acute appendicitis associated with appendiceal neoplasms. Zhonghua Wai Ke Za Zhi 59(5):343–347. https://doi.org/10.3760/cma.j.cn112139-20210129-00058
de Jonge J, Bolmers M, Musters GD, van Rossem CC, Bemelman WA, van Geloven A (2019) Predictors for interval appendectomy in non-operatively treated complicated appendicitis. Int J Colorectal Dis 34(7):1325–1332. https://doi.org/10.1007/s00384-019-03303-4
Lietzén E, Grönroos JM, Mecklin JP, Leppäniemi A, Nordström P, Rautio T et al (2019) Appendiceal neoplasm risk associated with complicated acute appendicitis-a population based study. Int J Colorectal Dis 34(1):39–46. https://doi.org/10.1007/s00384-018-3156-x
Nagtegaal ID, Odze RD, Klimstra D, Paradis V, Rugge M, Schirmacher P et al (2020) The 2019 who classification of tumours of the digestive system. Histopathology 76(2):182–188. https://doi.org/10.1111/his.13975
Bednarczuk T, Zemczak A, Bolanowski M, Borowska M, Chmielik E, ćwikła JB et al (2022) Neuroendocrine neoplasms of the small intestine and the appendix - update of the diagnostic and therapeutic guidelines (recommended by the polish network of neuroendocrine tumours) [nowotwory neuroendokrynne jelita cienkiego i wyrostka robaczkowego - uaktualnione zasady diagnostyki i leczenia (rekomendowane przez polską sieć guzów neuroendokrynnych)]. Endokrynol Pol 73(3):549–83. https://doi.org/10.5603/EP.a2022.0052
Frizziero M, Wang X, Chakrabarty B, Childs A, Luong TV, Walter T et al (2019) Retrospective study on mixed neuroendocrine non-neuroendocrine neoplasms from five European centres. World J Gastroenterol 25(39):5991–6005. https://doi.org/10.3748/wjg.v25.i39.5991
Frizziero M, Chakrabarty B, Nagy B, Lamarca A, Hubner RA, Valle JW et al (2020) Mixed neuroendocrine non-neuroendocrine neoplasms: a systematic review of a controversial and underestimated diagnosis. J Clin Med 9(1). https://doi.org/10.3390/jcm9010273
Brathwaite S, Rock J, Yearsley MM, Bekaii-Saab T, Wei L, Frankel WL et al (2016) Mixed adeno-neuroendocrine carcinoma: an aggressive clinical entity. Ann Surg Oncol 23(7):2281–2286. https://doi.org/10.1245/s10434-016-5179-2
Pignon JP, Tribodet H, Scagliotti GV, Douillard JY, Shepherd FA, Stephens RJ et al (2008) Lung adjuvant cisplatin evaluation: a pooled analysis by the lace collaborative group. J Clin Oncol 26(21):3552–3559. https://doi.org/10.1200/JCO.2007.13.9030
Kulke MH, Shah MH, Benson AR, Bergsland E, Berlin JD, Blaszkowsky LS et al (2015) Neuroendocrine tumors, version 1.2015. J Natl Compr Canc Netw 13(1):78–108. https://doi.org/10.6004/jnccn.2015.0011
Jun Z (2021) Study progresses of immunomodulation property of chemotherapeutic drugs and delivery systems. Chongqing Medicine 50(11):1937–1941. https://doi.org/10.3969/j.issn.1671-8348.2021.11.030
Mastrangelo M (2018) Cisplatin-based therapy and cinv: optimal antiemetics during germ cell testicular cancer treatment. Clin J Oncol Nurs 22(2):E31-36. https://doi.org/10.1188/18.CJON.E31-E36
Gebremeskel S, Johnston B (2015) Concepts and mechanisms underlying chemotherapy induced immunogenic cell death: impact on clinical studies and considerations for combined therapies. Oncotarget 6(39):41600–19. https://doi.org/10.18632/oncotarget.6113
Michalska M, Schultze-Seemann S, Kuckuck I, Katzenwadel A, Wolf P (2018) Impact of methadone on cisplatin treatment of bladder cancer cells. Anticancer Res 38(3):1369–75. https://doi.org/10.21873/anticanres.12360
Chen L, Zhou L, Wang C, Han Y, Lu Y, Liu J et al (2019) Tumor-targeted drug and cpg delivery system for phototherapy and docetaxel-enhanced immunotherapy with polarization toward m1-type macrophages on triple negative breast cancers. Adv Mater 31(52):e1904997. https://doi.org/10.1002/adma.201904997
Wu J, Waxman DJ (2018) Immunogenic chemotherapy: dose and schedule dependence and combination with immunotherapy. Cancer Lett 419:210–221. https://doi.org/10.1016/j.canlet.2018.01.050
Author information
Authors and Affiliations
Contributions
Study concepts: Xiaoyang Xing, Ming Li. Study design: Xiaoyang Xing, Yongyan Zhang, Ming Li. Data acquisition: Xiaoyang Xing, Yongyan Zhang, Ming Li. Quality control of data and algorithms: Xiaoyang Xing, Yongyan Zhang, Liwei Wang, Ming Li. Data analysis and interpretation: Xiaoyang Xing, YingXin Wang, Zhenduo Zhang, Ming Li. Statistical analysis: Xiaoyang Xing, Zhong Li, Ming Li. Manuscript preparation: Xiaoyang Xing, Yongyan Zhang, Liwei Wang, Ming Li. ManuSeript editing: Xiaoyang Xing, Yongyan Zhang, Zhenduo Zhang, Liwei Wang, Ming Li. Manuscript review: Xiaoyang Xing, Yongyan Zhang, Liwei Wang, YingXin Wang, Zhenduo Zhang, Zhong Li, Ming Li.
Corresponding author
Ethics declarations
Statement of human rights
For this type of study formal consent is not required.
Statement on the welfare of animals
This article does not contain any studies with animals performed by any of the authors.
Informed consent
This study contains no information that would enable individual patient identity.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xing, X., Zhang, Y., Wang, L. et al. Discussion on the benefits of different treatment strategies in elderly and non-elderly patients with appendix MiNEN: a retrospective study based on SEER database. Int J Colorectal Dis 38, 93 (2023). https://doi.org/10.1007/s00384-023-04384-y
Accepted:
Published:
DOI: https://doi.org/10.1007/s00384-023-04384-y