Abstract
Objectives
Due to limited and outdated literature, the role of magnetic resonance imaging (MRI) in the diagnostic work-up of acute colonic diverticulitis (ACD) is still under debate. The purpose of this study was to compare the performance of modern high-field MRI and multidetector computed tomography (MDCT) in the diagnosis and classification of ACD.
Methods
In our prospective study 24 emergency patients with the clinical diagnosis of ACD received MDCT and high-field MRI. Imaging features of ACD were assessed and categorized according to the classification of diverticular disease (CDD) by three independent readers. Results were matched with the final clinical report.
Results
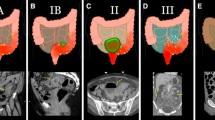
MRI with a specialized examination protocol clearly depicted all relevant findings of ACD. Statistical analysis resulted in an almost perfect strength of agreement between CT and MRI across all readers for the final CDD category (κ = 0.94) and the stage-related image features (κ = 0.98). Moderate agreement was seen for the detection of micro-abscesses (κ = 0.78), with a slight advantage for MRI.
Conclusion
Modern high-field MRI is fully comparable to MDCT in the assessment of ACD and has the potential to serve as a first-line imaging tool.



Similar content being viewed by others
References
Germer CT (2021) Diverticular disease. Chirurg 92:681–682. https://doi.org/10.1007/s00104-021-01451-4
Young-Fadok TM (2018) Diverticulitis. N Engl J Med 379:1635–1642. https://doi.org/10.1056/NEJMcp1800468
Etzioni DA, MacK TM, Beart RW, Kaiser AM (2009) Diverticulitis in the United States: 1998–2005: changing patterns of disease and treatment. Ann Surg 249:210–217. https://doi.org/10.1097/SLA.0b013e3181952888
Schäfer AO (2021) Diverticular disease: stage-related diagnostic imaging. Chirurg 92:688–693. https://doi.org/10.1007/s00104-021-01412-x
Lurz M, Lell MM, Wuest W et al (2015) Automated tube voltage selection in thoracoabdominal computed tomography at high pitch using a third-generation dual-source scanner. Invest Radiol 50:352–360. https://doi.org/10.1097/RLI.0000000000000133
Pustelnik D, Elsholtz FHJ, Bojarski C et al (2017) The CDD system in computed tomographic diagnosis of diverticular disease. RoFo Fortschritte auf dem Gebiet der Rontgenstrahlen und der Bildgebenden Verfahren 189:740–747. https://doi.org/10.1055/s-0043-110770
Lauscher JC, Lock JF, Aschenbrenner K et al (2021) Validation of the German Classification of Diverticular Disease (VADIS)—a prospective bicentric observational study. Int J Colorectal Dis 36:103–115. https://doi.org/10.1007/s00384-020-03721-9
Galetin T, Galetin A, Vestweber KH, Rink AD (2018) Systematic review and comparison of national and international guidelines on diverticular disease. Int J Colorectal Dis 33:261–272. https://doi.org/10.1007/s00384-017-2960-z
Schultz JK, Azhar N, Binda GA et al (2020) European Society of Coloproctology: guidelines for the management of diverticular disease of the colon. Colorectal Dis 22:5–28. https://doi.org/10.1111/codi.15140
Jerjen F, Zaidi T, Chan S et al (2021) Magnetic resonance imaging for the diagnosis and management of acute colonic diverticulitis: a review of current and future use Journal of Medical Radiation Sciences 1–10 https://doi.org/10.1002/jmrs.458
Peery AF, Shaukat A, Strate LL (2021) AGA clinical practice update on medical management of colonic diverticulitis: expert review. Gastroenterology 160:906-911.e1. https://doi.org/10.1053/j.gastro.2020.09.059
Heverhagen JT, Sitter H, Zielke A, Klose KJ (2008) Prospective evaluation of the value of magnetic resonance imaging in suspected acute sigmoid diverticulitis. Dis Colon Rectum 51:1810–1815. https://doi.org/10.1007/s10350-008-9330-4
Ajaj W, Ruehm SG, Lauenstein T et al (2005) Dark-lumen magnetic resonance colonography in patients with suspected sigmoid diverticulitis: a feasibility study. Eur Radiol 15:2316–2322. https://doi.org/10.1007/s00330-005-2862-2
Schreyer AG, Fürst A, Agha A et al (2004) Magnetic resonance imaging based colonography for diagnosis and assessment of diverticulosis and diverticulitis. Int J Colorectal Dis 19:474–480. https://doi.org/10.1007/s00384-004-0587-3
Uyeda JW (2019) Utility of MR imaging in abdominopelvic emergencies. Radiol Clin North Am 57:705–715. https://doi.org/10.1016/j.rcl.2019.02.010
Byott S, Harris I (2016) Rapid acquisition axial and coronal T2 HASTE MR in the evaluation of acute abdominal pain. Eur J Radiol 85:286–290. https://doi.org/10.1016/j.ejrad.2015.10.002
Punwani S, Rodriguez-Justo M, Bainbridge A et al (2009) Mural inflammation in Crohn disease: location-matched histologic validation of MR imaging features. Radiology 252:712–720. https://doi.org/10.1148/radiol.2523082167
Herrmann KA, Paspulati RM, Lauenstein T, Reiser MF (2010) Benefits and challenges in bowel MR imaging at 3.0 T. Top Magn Reson Imaging 21:165–175. https://doi.org/10.1097/RMR.0b013e31822a3294
Stoker J, van Randen A, Laméris W, Boermeester MA (2009) Imaging patients with acute abdominal pain. Radiology 253:31–46. https://doi.org/10.1148/radiol.2531090302
Yu HS, Gupta A, Soto JA, Lebedis C (2016) Emergency abdominal MRI: current uses and trends. Br J Radiol 89:1–12. https://doi.org/10.1259/bjr.20150804
Author information
Authors and Affiliations
Contributions
All authors worked on all 4 aspects of authorship as per ICMJE guidelines.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lurz, M., Gazis, A., Hanschke, S. et al. Value of high-field magnetic resonance imaging for diagnosis and classification of acute colonic diverticulitis. Int J Colorectal Dis 37, 201–207 (2022). https://doi.org/10.1007/s00384-021-04045-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-021-04045-y