Abstract
Background
Early bowel resection (EBR) in ileocolonic Crohn’s disease (CD) may be associated with more durable remission compared with initial medical therapy (IMT) even when biologic therapy is included.
Aim
To compare the efficacy of EBR versus IMT for ileocolonic CD
Methods
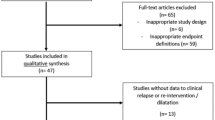
A systematic search was performed to identify studies that compared EBR (performed < 1 year from initial diagnosis) or IMT for the management of ileocolonic CD. Log hazard ratios (InHR) for relapse-free survival (RFS) and their standard errors were calculated from Kaplan-Meier plots and pooled using the inverse-variance method. Dichotomous variables were pooled as odds ratios (OR). Quality assessment of the included studies was performed using the Newcastle-Ottawa (NOS) and Jadad scales.
Results
A total of 7 studies with 1863 CD patients (EBR n = 581, 31.2%; IMT n = 1282, 68.8%) were eligible for inclusion. There was a moderate-to-high risk of bias. The median NOS was 8 (range 7–9). There was a reduced likelihood of overall (OR, 0.53; 95% confidence interval (95% CI), 0.34, 0.83; p = 0.005) and surgical (OR, 0.47; 95% CI, 0.24, 0.91; p = 0.03) relapse with EBR. There was also a less requirement for maintenance biologic therapy (OR, 0.24; 95% CI, 0.14, 0.42; p < 0.0001). Patients who underwent EBR had a significantly improved RFS than those who underwent IMT (HR, 0.62; 95% CI, 0.52, 0.73; p < 0.001). There was no difference in morbidity (OR, 1.67; 95% CI, 0.44, 6.36; p = 0.45) between the groups.
Conclusion
EBR may be associated with less relapse and need for maintenance biologic therapy than IMT. ‘Upfront’ or early resection may represent a reasonable and cost-effective alternative to biologic therapy, especially in biologic-resistant subpopulations.
Trial registration




Similar content being viewed by others
References
Duricova D, Burisch J, Jess T, Gower-Rousseau C, Lakatos PL (2014) Age-related differences in presentation and course of inflammatory bowel disease: an update on the population-based literature. J Croh’s Colitis 8(11):1351–1361
Odes S, Vardi H, Friger M, Wolters F, Russel MG, Riis L, Munkholm P, Politi P, Tsianos E, Clofent J, Vermeire S, Monteiro E, Mouzas I, Fornaciari G, Sijbrandij J, Limonard C, van Zeijl G, O’morain C, Moum B, Vatn M, Stockbrugger R, European Collaborative Study on Inflammatory Bowel Disease (2006) Cost analysis and cost determinants in a European inflammatory bowel disease inception cohort with 10 years of follow-up evaluation. Gastroenterology. 131(3):719–728
Gomollon F, Dignass A, Annese V et al (2017) 3rd European evidence-based consensus on the diagnosis and management of Crohn’s disease 2016: part 1: diagnosis and medical management. J Crohns Colitis. 11(1):3–25
D’Haens G, Baert F, van Assche G et al (2008) Early combined immunosuppression or conventional management in patients with newly diagnosed Crohn’s disease: an open randomised trial. Lancet (London, England) 371(9613):660–667
Baert F, Moortgat L, Van Assche G et al (2010) Mucosal healing predicts sustained clinical remission in patients with early-stage Crohn’s disease. Gastroenterology 138(2):463–468 quiz e410–461
Colombel JF, Sandborn WJ, Reinisch W, Mantzaris GJ, Kornbluth A, Rachmilewitz D, Lichtiger S, D’Haens G, Diamond RH, Broussard DL, Tang KL, van der Woude C, Rutgeerts P, SONIC Study Group (2010) Infliximab, azathioprine, or combination therapy for Crohn’s disease. N Engl J Med 362(15):1383–1395
Murthy SK, Begum J, Benchimol EI et al (2019) Introduction of anti-TNF therapy has not yielded expected declines in hospitalisation and intestinal resection rates in inflammatory bowel diseases: a population-based interrupted time series study. Gut.
Feagan BG, Panaccione R, Sandborn WJ, D’Haens GR, Schreiber S, Rutgeerts PJ, Loftus EV Jr, Lomax KG, Yu AP, Wu EQ, Chao J, Mulani P (2008) Effects of adalimumab therapy on incidence of hospitalization and surgery in Crohn’s disease: results from the CHARM study. Gastroenterology. 135(5):1493–1499
Peters CP, Eshuis EJ, Toxopeus FM et al (2014) Adalimumab for Crohn’s disease: long-term sustained benefit in a population-based cohort of 438 patients. J Crohns Colitis. 8(8):866–875
Schwartz DA, Loftus EV Jr, Tremaine WJ et al (2002) The natural history of fistulizing Crohn’s disease in Olmsted County, Minnesota. Gastroenterology 122(4):875–880
Silverstein MD, Loftus EV, Sandborn WJ, Tremaine WJ, Feagan BG, Nietert PJ, Harmsen WS, Zinsmeister AR (1999) Clinical course and costs of care for Crohn’s disease: Markov model analysis of a population-based cohort. Gastroenterology. 117(1):49–57
Bernklev T, Jahnsen J, Aadland E, Sauar J, Schulz T, Lygren I, Henriksen M, Stray N, Kjellevold O, Vatn M, Moum B, IBSEN Study Group (2004) Health-related quality of life in patients with inflammatory bowel disease five years after the initial diagnosis. Scand J Gastroenterol 39(4):365–373
van der Have M, van der Aalst KS, Kaptein AA, Leenders M, Siersema PD, Oldenburg B, Fidder HH (2014) Determinants of health-related quality of life in Crohn’s disease: a systematic review and meta-analysis. J Crohns Colitis 8(2):93–106
Feagan BG, Reinisch W, Rutgeerts P, Sandborn WJ, Yan S, Eisenberg D, Bala M, Johanns J, Olson A, Hanauer SB (2007) The effects of infliximab therapy on health-related quality of life in ulcerative colitis patients. Am J Gastroenterol 102(4):794–802
Wright EK, Kamm MA (2015) Impact of drug therapy and surgery on quality of life in Crohn’s disease: a systematic review. Inflamm Bowel Dis 21(5):1187–1194
Eshuis EJ, Peters CP, van Bodegraven AA, Bartelsman JF, Bemelman W, Fockens P, D’Haens GR, Stokkers PC, Ponsioen CY (2013) Ten years of infliximab for Crohn’s disease: outcome in 469 patients from 2 tertiary referral centers. Inflamm Bowel Dis 19(8):1622–1630
Gionchetti P, Dignass A, Danese S, Magro Dias FJ, Rogler G, Lakatos PL, Adamina M, Ardizzone S, Buskens CJ, Sebastian S, Laureti S, Sampietro GM, Vucelic B, van der Woude C, Barreiro-de Acosta M, Maaser C, Portela F, Vavricka SR, Gomollón F, ECCO (2017) 3rd European evidence-based consensus on the diagnosis and management of Crohn’s disease 2016: part 2: surgical management and special situations. J Crohns Colitis. 11(2):135–149
Kistner L, Doll D, Holtorf A, Nitsche U, Janssen KP (2017) Interferon-inducible CXC-chemokines are crucial immune modulators and survival predictors in colorectal cancer. Oncotarget. 8(52):89998–90012
Lapidus A, Bernell O, Hellers G, Lofberg R (1998) Clinical course of colorectal Crohn’s disease: a 35-year follow-up study of 507 patients. Gastroenterology. 114(6):1151–1160
Aratari A, Papi C, Leandro G, Viscido A, Capurso L, Caprilli R (2007) Early versus late surgery for ileo-caecal Crohn’s disease. Aliment Pharmacol Ther 26(10):1303–1312
Latella G, Cocco A, Angelucci E, Viscido A, Bacci S, Necozione S, Caprilli R (2009) Clinical course of Crohn’s disease first diagnosed at surgery for acute abdomen. Dig Liver Dis 41(4):269–276
Golovics PA, Lakatos L, Nagy A, Pandur T, Szita I, Balogh M, Molnar C, Komaromi E, Lovasz BD, Mandel M, Veres G, Kiss LS, Vegh Z, Lakatos PL (2013) Is early limited surgery associated with a more benign disease course in Crohn’s disease? World J Gastroenterol 19(43):7701–7710
An V, Cohen L, Lawrence M, Thomas M, Andrews J, Moore J (2016) Early surgery in Crohn’s disease a benefit in selected cases. World J Gastrointest Surg 8(7):492–500
Lee JM, Lee KM, Kim JS, Kim YS, Cheon JH, Ye BD, Kim YH, Han DS, Lee CK, Park HJ (2018) Postoperative course of Crohn disease according to timing of bowel resection: results from the CONNECT Study. Medicine (Baltimore) 97(16):e0459
Ponsioen CY, de Groof EJ, Eshuis EJ, Gardenbroek TJ, Bossuyt PMM, Hart A, Warusavitarne J, Buskens CJ, van Bodegraven A, Brink MA, Consten ECJ, van Wagensveld B, Rijk MCM, Crolla RMPH, Noomen CG, Houdijk APJ, Mallant RC, Boom M, Marsman WA, Stockmann HB, Mol B, de Groof AJ, Stokkers PC, D’Haens GR, Bemelman WA, LIR!C study group (2017) Laparoscopic ileocaecal resection versus infliximab for terminal ileitis in Crohn’s disease: a randomised controlled, open-label, multicentre trial. Lancet Gastroenterol Hepatol 2(11):785–792
Eshuis EJ, Stokkers PC, Bemelman WA (2010) Decision-making in ileocecal Crohn’s disease management: surgery versus pharmacotherapy. Expert Rev Gastroenterol Hepatol 4(2):181–189
Eshuis EJ, Slors JF, Stokkers PC, Sprangers MA, Ubbink DT, Cuesta MA, Pierik EG, Bemelman WA (2010) Long-term outcomes following laparoscopically assisted versus open ileocolic resection for Crohn’s disease. Br J Surg 97(4):563–568
Rijcken E, Mennigen R, Argyris I, Senninger N, Bruewer M (2012) Single-incision laparoscopic surgery for ileocolic resection in Crohn’s disease. Dis Colon Rectum 55(2):140–146
Raskin ER, Gorrepati ML, Mehendale S, Gaertner WB (2018) Robotic-assisted ileocolic resection for Crohn’s disease: outcomes from an early national experience. J Robot Surg
Yamamoto T (2005) Factors affecting recurrence after surgery for Crohn’s disease. World J Gastroenterol 11(26):3971–3979
Latella G, Caprilli R, Travis S (2011) In favour of early surgery in Crohn’s disease: a hypothesis to be tested. J Crohns Colitis. 5(1):1–4
Tierney JF, Stewart LA, Ghersi D, Burdett S, Sydes MR (2007) Practical methods for incorporating summary time-to-event data into meta-analysis. Trials. 8:16
Satsangi J, Silverberg MS, Vermeire S, Colombel J-F (2006) The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications. Gut. 55(6):749–753
Gasche CSJ, Brynskov J, D’Haens G, Hanauer SB, Irvine EJ, Jewell DP, Rachmilewitz D, Sachar DB, Sandborn WJ, Sutherland LR (1998) A simple classification of Crohn’s disease: report of the Working Party for the World Congresses of Gastroenterology, Vienna 1998. Inflamm Bowel Dis 6(1):8–15
Regueiro M, Velayos F, Greer JB et al (2017) American Gastroenterological Association Institute technical review on the management of Crohn’s disease after surgical resection. Gastroenterology 152(1):277–295.e273
Bernell O, Lapidus A, Hellers G (2000) Risk factors for surgery and recurrence in 907 patients with primary ileocaecal Crohn’s disease. Br J Surg 87(12):1697–1701
Buisson A, Chevaux JB, Allen PB, Bommelaer G, Peyrin-Biroulet L (2012) Review article: the natural history of postoperative Crohn’s disease recurrence. Aliment Pharmacol Ther 35(6):625–633
Wright EK, Kamm MA, De Cruz P et al (2015) Measurement of fecal calprotectin improves monitoring and detection of recurrence of Crohn’s disease after surgery. Gastroenterology 148(5):938–947. e931
Schnitzler F, Fidder H, Ferrante M, Noman M, Arijs I, van Assche G, Hoffman I, van Steen K, Vermeire S, Rutgeerts P (2009) Mucosal healing predicts long-term outcome of maintenance therapy with infliximab in Crohn’s disease. Inflamm Bowel Dis 15(9):1295–1301
Lowney JK, Dietz DW, Birnbaum EH, Kodner IJ, Mutch MG, Fleshman JW (2006) Is there any difference in recurrence rates in laparoscopic ileocolic resection for Crohn’s disease compared with conventional surgery? A long-term, follow-up study. Dis Colon Rectum 49(1):58–63
Pariente B, Cosnes J, Danese S, Sandborn WJ, Lewin M, Fletcher JG, Chowers Y, D’Haens G, Feagan BG, Hibi T, Hommes DW, Irvine EJ, Kamm MA, Loftus EV Jr, Louis E, Michetti P, Munkholm P, Oresland T, Panés J, Peyrin-Biroulet L, Reinisch W, Sands BE, Schoelmerich J, Schreiber S, Tilg H, Travis S, van Assche G, Vecchi M, Mary JY, Colombel JF, Lémann M (2011) Development of the Crohn’s disease digestive damage score, the Lemann score. Inflamm Bowel Dis 17(6):1415–1422
Schreiber S, Colombel JF, Bloomfield R, Nikolaus S, Schölmerich J, Panés J, Sandborn WJ, PRECiSE 2 Study Investigators (2010) Increased response and remission rates in short-duration Crohn’s disease with subcutaneous certolizumab pegol: an analysis of PRECiSE 2 randomized maintenance trial data. Am J Gastroenterol 105(7):1574–1582
El-Hussuna A, Krag A, Olaison G, Bendtsen F, Gluud LL (2013) The effect of anti-tumor necrosis factor alpha agents on postoperative anastomotic complications in Crohn’s disease: a systematic review. Dis Colon Rectum 56(12):1423–1433
Billioud V, Ford AC, Tedesco ED, Colombel JF, Roblin X, Peyrin-Biroulet L (2013) Preoperative use of anti-TNF therapy and postoperative complications in inflammatory bowel diseases: a meta-analysis. J Crohns Colitis. 7(11):853–867
Ippoliti A, Devlin S, Mei L, Yang H, Papadakis KA, Vasiliauskas EA, McGovern D, Abreu MT, Melmed G, Shaye O, Enayati P, Chen G, Choi J, Taylor K, Landers CJ, Rotter JI, Targan SR (2010) Combination of innate and adaptive immune alterations increased the likelihood of fibrostenosis in Crohn’s disease. Inflamm Bowel Dis 16(8):1279–1285
Coffey JC, O’Leary DP, Kiernan MG, Faul P (2016) The mesentery in Crohn’s disease: friend or foe? Curr Opin Gastroenterol 32(4):267–273
Borley NR, Mortensen NJ, Jewell DP, Warren BF (2000) The relationship between inflammatory and serosal connective tissue changes in ileal Crohn’s disease: evidence for a possible causative link. J Pathol 190(2):196–202
Guedj K, Abitbol Y, Cazals-Hatem D et al (2019) Adipocytes orchestrate the formation of tertiary lymphoid organs in the creeping fat of Crohn’s disease affected mesentery. J Autoimmun
Coffey CJ, Kiernan MG, Sahebally SM, Jarrar A, Burke JP, Kiely PA, Shen B, Waldron D, Peirce C, Moloney M, Skelly M, Tibbitts P, Hidayat H, Faul PN, Healy V, O’Leary PD, Walsh LG, Dockery P, O’Connell RP, Martin ST, Shanahan F, Fiocchi C, Dunne CP (2018) Inclusion of the mesentery in ileocolic resection for Crohno’s disease is associated with reduced surgical recurrence. J Crohns Colitis. 12(10):1139–1150
Crohn BB, Ginzburg L, Oppenheimer GD (1932) Regional ileitis: a pathologic and clinical entity. JAMA. 99(16):1323–1329
Heald RJ, Ryall RD (1986) Recurrence and survival after total mesorectal excision for rectal cancer. Lancet (London, England) 1(8496):1479–1482
West NP, Hohenberger W, Weber K, Perrakis A, Finan PJ, Quirke P (2010) Complete mesocolic excision with central vascular ligation produces an oncologically superior specimen compared with standard surgery for carcinoma of the colon. J Clin Oncol 28(2):272–278
de Groof EJ, van der Meer JHM, Tanis PJ, de Bruyn JR, van Ruler O, D’Haens GRAM, van den Brink G, Bemelman WA, Wildenberg ME, Buskens CJ (2019) Persistent mesorectal inflammatory activity is associated with complications after proctectomy in Crohn’s disease. J Crohns Colitis. 13(3):285–293
Ryan JM, Rogers AC, O’Toole A, Burke JP (2019) Meta-analysis of histological margin positivity in the prediction of recurrence after Crohn’s resection. Dis Colon Rectum 62(7):882–892
Jeejeebhoy KN (2002) Short bowel syndrome: a nutritional and medical approach. CMAJ. 166(10):1297–1302
Mitchell JE, Breuer RI, Zuckerman L, Berlin J, Schilli R, Dunn JK (1980) The colon influences ileal resection diarrhea. Dig Dis Sci 25(1):33–41
Wright EK, Kamm MA, De Cruz P et al (2015) Effect of intestinal resection on quality of life in Crohn’s disease. J Crohns Colitis. 9(6):452–462
Ha FJ, Thong L, Khalil H (2017) Quality of life after intestinal resection in patients with Crohn disease: a systematic review. Dig Surg 34(5):355–363
De Groof J, Bemelman W, Eshuis E et al (2017) OP015 Cost-effectiveness of laparoscopic ileocecal resection versus infliximab treatment of terminal ileitis in Crohn’s disease: the LIR! C TRIAL. J Crohns Colitis 11(suppl_1):S9–S10
Feagan BG, McDonald JW, Panaccione R et al (2014) Methotrexate in combination with infliximab is no more effective than infliximab alone in patients with Crohn’s disease. Gastroenterology 146(3):681–688.e681
Khanna R, Bressler B, Levesque BG et al (2015) Early combined immunosuppression for the management of Crohn’s disease (REACT): a cluster randomised controlled trial. Lancet (London, England) 386(10006):1825–1834
Khanna R, Sattin BD, Afif W, Benchimol EI, Bernard EJ, Bitton A, Bressler B, Fedorak RN, Ghosh S, Greenberg GR, Marshall JK, Panaccione R, Seidman EG, Silverberg MS, Steinhart AH, Sy R, van Assche G, Walters TD, Sandborn WJ, Feagan BG (2013) Review article: a clinician’s guide for therapeutic drug monitoring of infliximab in inflammatory bowel disease. Aliment Pharmacol Ther 38(5):447–459
Colombel J-F, Panaccione R, Bossuyt P, Lukas M, Baert F, Vaňásek T, Danalioglu A, Novacek G, Armuzzi A, Hébuterne X, Travis S, Danese S, Reinisch W, Sandborn WJ, Rutgeerts P, Hommes D, Schreiber S, Neimark E, Huang B, Zhou Q, Mendez P, Petersson J, Wallace K, Robinson AM, Thakkar RB, D’Haens G (2017) Effect of tight control management on Crohn’s disease (CALM): a multicentre, randomised, controlled phase 3 trial. Lancet 390(10114):2779–2789
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 247 kb).
Rights and permissions
About this article
Cite this article
Ryan, É.J., Orsi, G., Boland, M.R. et al. Meta-analysis of early bowel resection versus initial medical therapy in patient's with ileocolonic Crohn's disease. Int J Colorectal Dis 35, 501–512 (2020). https://doi.org/10.1007/s00384-019-03479-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-019-03479-9