Abstract
Purpose
To estimate the risk of lower gastrointestinal bleeding (LGIB) caused by malignant lesion in patients presenting with per-rectal bleeding (PRB), by using visual aid as an objective measurement of PRB colour.
Methods
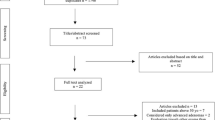
This was a prospective observational study on patients presented with PRB to Family Medicine Specialty Clinic, who undergo flexible sigmoidoscopy (FS) or colonoscopy (CLN) from December 2012 to September 2013. Patients aged 40 years old or above, haemodynamically stable, with normal haemoglobin level were included. Patients with a history of previous colonic surgery, refused to have FS or CLN, with ophthalmologic diseases such as colour blindness were excluded. Parameters including subjective description of PRB colour, number of chosen red colour by patients, source and distance of bleeding from anal verge were recorded for analysis. Receiver operating characteristic (ROC) curve was used to identify the optimal cutoff level of colour for diagnosing colonic lesion. Diagnostic accuracy was assessed by area under the ROC curve (AUC). Accountability of this model was assessed by logistic regression.
Results
The dark PRB colour was associated with diagnosis of tumour (p < 0.001) and advanced neoplastic polyp (p < 0.001). The light PRB colour was associated with the diagnosis of piles (p < 0.001). The performance of our model to predict tumour or advanced neoplastic polyps by colour (AUC, 0.798) had a better discriminative power than that to predict colonic lesion alone (AUC, 0.610) by ROC curve analysis.
Conclusion
Objective measurement of PRB colour accurately estimated the risk of LGIB caused by malignant lesion in patients presenting with PRB.





Similar content being viewed by others
References
Ghassemi KA (2013) Lower GI bleeding: epidemiology and management. Curr Gastroenterol Rep 15(7):333
Wauters H, Van Casteren V, Buntinx F (2000) Rectal bleeding and colorectal cancer in general practice: diagnostic study. BMJ 321(7267):998–999
Hamilton W, Sharp D (2004) Diagnosis of colorectal cancer in primary care: the evidence base for guidelines. Fam Pract 21(1):99–106
Thompson MR, Perera R, Senapati A et al (2007) Predictive value of common symptom combinations in diagnosing colorectal cancer. Br J Surg 94(10):1260–1265
Shapley M, Mansell G, Jordan JL et al (2010) Positive predictive values of >5 % in primary care for cancer: systemic review. Br J Gen Pract 60(578):e366–e377
Zuckerman GR, Trellis DR, Sherman TM et al (1995) An objective measure of stool color for differentiating upper from lower gastrointestinal bleeding. Dig Dis Sci 40(8):1614–1621
Zuckerman GR, Prakash C (1998) Acute lower intestinal bleeding: part I: clinical presentation and diagnosis. Gastrointest Endosc 48(6):606–617
Talley NJ, O’Connor S (2001) Clinical examination: a systematic guide to physical diagnosis, 4th edn. Wiley-Blackwell
Vander A, Sherman J, Luciano D (2001) Human physiology, 7th edn. WCB McGraw-Hill
Choi HK, Law WL, Chu KW (2003) The value of flexible sigmoidoscopy for patients with bright red rectal bleeding. Hong Kong Med J 9(3):171–174
Adelstein BA, Macaskill P, Chan SF et al (2011) Most bowel cancer symptoms do not indicate colorectal cancer and polyps: a systematic review. BMC Gastroenterol 11:65
Kent KJ, Woolf D, McCue J et al (2010) The use of symptoms to predict colorectal cancer site. Can we reduce the pressure on our endoscopy services? Color Dis 12(2):114–118
Nikpour S, Ali AA (2008) Colonoscopic evaluation of minimal rectal bleeding in average-risk patients for colorectal cancer. World J Gastroenterol 14(42):6536–6540
Hippisley-Cox J, Coupland C (2012) Identifying patients with suspected colorectal cancer in primary care: derivation and validation of an algorithm. Br J Gen Pract 62(594):29–37
Hsieh FY, Bloch DA, Larsen MD (1998) A simple method of sample size calculation for linear and logistic regression. Stat Med 17(14):1623–1634
Wong MC, Tsoi KK, Ng SS et al (2010) A comparison of the acceptance of immunochemical faecal occult blood test and colonoscopy in colorectal cancer screening: a prospective study among Chinese. Aliment Pharmacol Ther 32:74–82
Basaranoglu M, Celebi S, Ataseven H et al (2008) Prevalence and consultation behavior of self-reported rectal bleeding by face-to-face interview in an Asian community. Digestion 77(1):10–15
Adelstein BA, Irwig L, Macaskill P et al (2010) Who needs colonoscopy to identify colorectal cancer? Bowel symptoms do not add substantially to age and other medical history. Aliment Pharmacol Ther 32(2):270–281
Strate LL (2005) Lower GI bleeding: epidemiology and diagnosis. Gastroenterol Clin N Am 34(4):643–664
Ellis H, Calne R, Watson C (1998) Lecture notes on general surgery, 9 edn. Blackwell Science
Acknowledgments
I would like to thank the whole surgical team of the Family Medicine Specialty Clinic for identifying and recruiting patients and the patients who participated.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research ethics of this study was approved by the Kowloon West Cluster Research Ethics Committee, Hong Kong.
Competing interest
The authors declare that they have no competing interests.
Additional information
What does this paper add to the literature?
Objective measurement of per-rectal bleeding colour is a valid and non-invasive tool for estimating the risk of lower gastrointestinal bleeding caused by malignant lesions.
Rights and permissions
About this article
Cite this article
Lai, PY., Chan, KW., Wong, C.KH. et al. Can the colour of per-rectal bleeding estimate the risk of lower gastrointestinal bleeding caused by malignant lesion?. Int J Colorectal Dis 31, 335–342 (2016). https://doi.org/10.1007/s00384-015-2414-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-015-2414-4