Abstract
Introduction
Owing to several therapeutic advancements, more patients with biliary atresia now survive into adulthood while retaining their native liver. However, the optimal strategy for long-term management of such patients remains unclear.
Methods
Aiming to establish the current management strategies, we reviewed previous reports of long-term outcome of BA who underwent surgery at our institution as well as the relevant literature, focusing particularly on the treatment of late complications.
Results
Approximately 30–40% of long-term survivors of biliary atresia who retain their native liver exhibit late sequelae such as cholangitis and portal hypertension. Early and appropriate intervention with Kasai portoenterostomy is essential for ensuring long-term survival with good quality of life. In our hospital, the current standard for Kasai portoenterostomy involves dissecting the fibrous remnants along the porta hepatis, just on the level of the liver capsule. Cholangitis is an important late complication in biliary atresia, and the possibility of mechanical obstruction of the biliary drainage route or deformity of the intrahepatic bile ducts with or without gallstones should be thoroughly evaluated in patients with intractable cholangitis. Regarding portal hypertension, appropriate interventions such as endoscopic variceal treatment and partial splenic embolization are considered to provide good quality of life when hepatic function is preserved.
Conclusion
Appropriate therapeutic management is strongly recommended in selected patients with late complications.




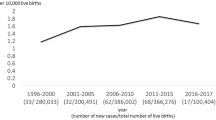
This figure was adapted from Nio M (2016) [19]

This figure was adapted from Sasaki H (2016) [25]
Similar content being viewed by others
References
Bijl EJ, Bharwani KD, Houwen RHJ, de Man RA (2013) The long-term outcome of the Kasai operation in patients with biliary atresia: a systematic review. Neth J Med 71:170–173
Lykavieris P, Chardot C, Sokhn M, Gauthier F, Valayer J, Bernard O (2005) Outcome in adulthood of biliary atresia: a study of 63 patients who survived for over 20 years with their native liver. Hepatology 41:366–371
Shinkai M, Ohhama Y, Take H, Kitagawa N, Kudo H, Mochizuki K, Hatata T (2009) Long-term outcome of children with biliary atresia who were not transplanted after the Kasai operation: > 20-year experience at a children’s hospital. J Pediatr Gastroenterol Nutr 48:443–450
Nio M, Ohi R, Shimaoka S, Iwami D, Sano N (1997) The outcome of surgery for biliary atresia and the current status of long-term survivors. Tohoku J Exp Med 181:235–244
de Vries W, Homan-Van der Veen J, Hulscher JB, Hoekstra-Weebers JE, Houwen RH, Verkade HJ, Netherlands Study Group of Biliary Atresia Registry (2011) Twenty-year transplant-free survival rate among patients with biliary atresia. Clin Gastroenterol Hepatol 9:1086–1091
Toyosaka A, Okamoto E, Okasora T, Nose K, Tomimoto Y (1993) Outcome of 21 patients with biliary atresia living more than 10 years. J Pediatr Surg 28:1498–1501
Shimizu Y, Hashimoto T, Otobe Y, Ueda N, Matsuo Y, Manabe T (1997) Long-term survivors in biliary atresia—findings for a 20-year survival group. Tohoku J Exp Med 181:225–233
Pintér AB, Farkas A, Pár A, Kövesi T, Appelshoffer S (2004) A long-term follow-up of five patients with atresia of the common bile duct. J Pediatr Surg 39:1050–1054
Watanabe Y, Todani T, Toki A, Noda T, Sato Y, Ogura K, Yoshikawa M, Yamamoto S, Wang ZQ (1997) Changes of hepatic volume after successful Kasai operation. Tohoku J Exp Med 181:185–191
Hung PY, Chen CC, Chen WJ, Lai HS, Hsu WM, Lee PH, Ho MC, Chen TH, Ni YH, Chen HL, Hsu HY, Chang MH (2006) Long-term prognosis of patients with biliary atresia: a 25 year summary. J Pediatr Gastroenterol Nutr 42:190–195
Takahashi Y, Matsuura T, Saeki I, Zaizen Y, Taguchi T (2009) Excellent long-term outcome of hepaticojejunostomy for biliary atresia with a hilar cyst. J Pediatr Surg 44:2312–2315
Raffensperger JG (1991) A long-term follow-up of three patients with biliary atresia. J Pediatr Surg 26:176–177
Hol L, van den Bos IC, Hussain SM, Zondervan PE, de Man RA (2008) Hepatocellular carcinoma complicating biliary atresia after Kasai portoenterostomy. Eur J Gastroenterol Hepatol 20:227–231
Kasai M, Ohi R, Chiba T, Hayashi Y (1988) A patient with biliary atresia who died 28 years after hepatic portojejunostomy. J Pediatr Surg 23:430–431
Yamanaka J, Iimuro Y, Hirano T, Kosaka H, Fujimoto J (2005) Successful liver resection for biliary atresia with intrahepatic biliary cysts after Kasai procedure. J Pediatr Surg 40:E9–E11
Kumagi T, Drenth JP, Guttman O, Ng V, Lilly L, Therapondos G, Hiasa Y, Michitaka K, Onji M, Watanabe Y, Sen S, Griffiths W, Roberts E, Heathcote J, Hirschfield GM (2012) Biliary atresia and survival into adulthood without transplantation: a collaborative multicentre clinic review. Liver Int 32:510–518
Nio M, Wada M, Sasaki H, Tanaka H, Okamura A (2012) Risk factors affecting late-presenting liver failure in adult patients with biliary atresia. J Pediatr Surg 47:2179–2183
Nio M, Sano N, Ishii T, Sasaki H, Hayashi Y, Ohi R (2004) Cholangitis as a late complication in long-term survivors after surgery for biliary atresia. J Pediatr Surg 39:1797–1799
Nio M, Wada M, Sasaki H, Kazama T, Tanaka H, Kudo H (2016) Technical standardization of Kasai portoenterostomy for biliary atresia. J Pediatr Surg 51:2105–2108
Gomi H, Solomkin JS, Takada T, Strasberg SM, Pitt HA, Yoshida M, Kusachi S, Mayumi T, Miura F, Kiriyama S, Yokoe M, Kimura Y, Higuchi R, Windsor JA, Dervenis C, Liau KH, Kim MH, Tokyo Guideline Revision Committee (2013) TG13 antimicrobial therapy for acute cholangitis and cholecystitis. J Hepatobiliary Pancreat Sci 20:60–70
Houben C, Phelan S, Davenport M (2006) Late-presenting cholangitis and Roux loop obstruction after Kasai portoenterostomy for biliary atresia. J Pediatr Surg 41:1159–1164
Shneider BL, Bosch J, de Franchis R, Emre SH, Groszmann RJ, Ling SC, Lorenz JM, Squires RH, Superina RA, Thompson AE, Mazariegos GV (2012) Portal hypertension in children: expert pediatric opinion on the report of the Baveno V consensus workshop on methodology of diagnosis and therapy in portal hypertension. Pediatr Transplant 16:426–437
Duché M, Ducot B, Ackermann O, Baujard C, Chevret L, Frank-Soltysiak M, Jacquemin E, Bernard O (2013) Experience with endoscopic management of high-risk gastroesophageal varices, with and without bleeding, in children with biliary atresia. Gastroenterology 145:801–807
van Heurn LW, Saing H, Tam PK (2004) Portoenterostomy for biliary atresia: long-term survival and prognosis after esophageal variceal bleeding. J Pediatr Surg 39:6–9
Sasaki H, Tanaka H, Wada M, Kazama T, Nakamura M, Kudo H, Okubo R, Sakurai T, Nio M (2016) Analysis of the prognostic factors of long-term native liver survival in survivors of biliary atresia. Pediatr Surg Int 32:839–843
Nio M, Hayashi Y, Sano N, Ishii T, Sasaki H, Ohi R (2003) Long-term efficacy of partial splenic embolization in children. J Pediatr Surg 38:1760–1762
Shinkai M, Ohhama Y, Take H, Fukuzato Y, Fujita S, Nishi T (2003) Evaluation of the PELD risk score as a severity index of biliary atresia. J Pediatr Surg 38:1001–1004
Ishii T, Nio M, Shimaoka S, Sano N, Sasaki H, Kimura D, Hayashi Y, Ohi R (2003) Clinical significance of 99mTc-DTPA-galactosyl human serum albumin liver scintigraphy in follow-up patients with biliary atresia. J Pediatr Surg 38:1486–1490
Sasaki H, Nio M, Hayashi Y, Ishii T, Sano N, Ohi R (2007) Problems during and after pregnancy in female patients with biliary atresia. J Pediatr Surg 42:1329–1332
Kuroda T, Saeki M, Morikawa N, Fuchimoto Y (2005) Biliary atresia and pregnancy: puberty may be an important point for predicting the outcome. J Pediatr Surg 40:1852–1855
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflict of interest
All authors declare that they have no conflict of interests.
Ethical approval
This review was approved by the ethical committee of our hospital. Informed consent was not required for this type of study.
Rights and permissions
About this article
Cite this article
Sasaki, H., Tanaka, H. & Nio, M. Current management of long-term survivors of biliary atresia: over 40 years of experience in a single center and review of the literature. Pediatr Surg Int 33, 1327–1333 (2017). https://doi.org/10.1007/s00383-017-4163-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-017-4163-7