Abstract
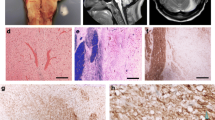
Osmotic demyelination syndrome (ODS) is a very rare condition in childhood occurring usually secondary to the rapid increase of serum sodium levels. This situation occurring secondary to the rapid correction of hyponatremia can be seen more rarely in the form of extrapontine myelinolysis and even the coexistence of these two conditions besides central pontine demyelinolysis. However, osmotic demyelination syndrome due to the rapid correction of hyponatremia in chronic renal failure (CRF) patients is very rare depending on existing uremia. In this article, we present an extremely rare case of pontine and extrapontine myelinolysis, which occurred in a pediatric patient with chronic renal failure, secondary to the rapid correction of hyponatremia. In the diffusion and cranial magnetic resonance imaging (MRI), bilateral symmetrical caudate, putamen, and thalamus involvements and hyperintense linear lesions at the pons, cortical, and subcortical areas were revealed. It was evaluated as pontine and extrapontine myelinolysis. This clinical situation presents that the presence of severe hyponatremia and extremely rapid correction of it can develop pontine and extrapontine myelinolysis even though it is very rare in uremic patients.




Similar content being viewed by others
Abbreviations
- CRF:
-
chronic renal failure
- DTR:
-
deep tendon reflexes
- GCS:
-
Glasgow Coma Scale
- MRI:
-
magnetic resonance imaging
- ODS:
-
osmotic demyelination syndrome
References
Karp BI, Laureno L (1993) Pontine and extrapontine myelinolysis: a neurologic disorder following rapid correction of hyponatremia. Medicine 72:359–373
Adams RD, Victor M, Mancall EL (1959) Central pontine myelinolysis, a hitherto undescribed disease occurring in alcoholic and malnourished patients. Arch Neurol Psychiatr 81:154e172
Berry K, Olszewski J (1963) Central pontine myelinolvsis: a case report. Neurology 13:531
Vakharia JD, Goldsweig B, Rogg JM, Topor LS (2017) Extrapontine myelinolysis in a child with salt intoxication. J Pediatr 186:207–207.e1
Aoki R, Morimoto T, Takahashi Y, Saito H, Fuchigami T, Takahashi S (2016) Extrapontine myelinolysis associated with severe hypernatremia in infancy. Pediatr Int 58:936–939
Sugimura Y, Murase T, Takefuji S (2005) Protective effect of dexamethasone on osmotic-induced demyelination in rats. Exp Neurol 192:178e183
Murase T, Sugimura Y, Takefuji S, Oiso Y, Murata Y (2006) Mechanisms and therapy of osmotic demyelination. Am J Med 119:69e73
Kim J, Song T, Park S, Choi IS (2007) Cerebellar peduncular myelinolysis in a patient receiving hemodialysis. J Neurol Sci 253:66–68
Soupart A, Silver S, Schroeder B (2002) Rapid (24-hr) reaccumulation of brain organic osmolytes (particularly myo-Inositol) in azotemic rats after correction of chronic hyponatremia. J Am Soc Nephrol 13:1433–1441
Huang WY, Weng WC, Peng TI, Ro LS, Yang CW, Chen KH (2007) Central pontine and extrapontine myelinolysis after rapid correction of hyponatremia by hemodialysis in a uremic patient. Ren Fail 29:635–638
Peces R, Ablanedo P, Alvarez J (1988) Central pontine and extrapontine myelinolysis following correction of severe hyponatremia. Nephron 49:160–163
Spasovski G, Vanholder R, Allolio B, Annane D, Ball S, Bichet D, et.al (2014) Clinical practice guideline on diagnosis and treatment of hyponatraemia. Nephrol Dial Transplant 29:1-39.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethics approval and consent to participate
The presentation of the case was approved by the Clinical Research Ethics Committee of the Adana City Education and Research Hospital. Informed consent was obtained.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sarigecili, E., Taner, S., Ucar, H.K. et al. A rare case of pontine and extrapontine myelinolysis in a pediatric patient with chronic renal failure. Childs Nerv Syst 37, 1025–1027 (2021). https://doi.org/10.1007/s00381-020-04720-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-020-04720-5