Abstract
Purpose
To compare the short-term postoperative functional outcomes and severity of irritative symptoms following holmium and thulium fiber laser enucleation (HoLEP and ThuFLEP).
Methods
This prospective randomized single-blinded study was performed in accordance with CONSORT. The inclusion criteria were IPSS > 20 or Qmax < 10 ml/s. Patients were randomized between HoLEP and ThuFLEP. Demographics, objective data (PSA, prostate volume, etc.), data on urinary and sexual function (IPSS, IIEF, QoL, QUID, Qmax, ICIQ-MLUTS) were collected. Detailed perioperative information and postoperative data on functional outcomes at 1, 2, 3, 4, 6, 8, 10, 12 weeks and 6 months were collected.
Results
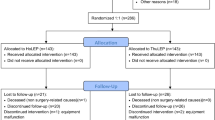
Data on 163 participants were included (77—HoLEP, 86—ThuFLEP). No differences were found in surgery duration; number of postoperative complications (Clavien–Dindo I-III), catheterization time and hospital stay. Functional outcomes up to 6 months didn’t differ between the groups (IPPS, IIEF, QoL, QUID, ICIQ-MLUTS, Qmax, p > 0.05). Total ICIQ‐MLUTS, bother and voiding scores at 1 and 3 months significantly increased compared with the baseline in both groups (p < 0.05). No difference between the groups were observed. In HoLEP the SUI series rate was 1.3% and 1.3% after 3 and 6 months following the procedure; in ThuFLEP: it was 3.5% and 2.3% respectively (p = 0.35 and p = 0.54).
Conclusion
The preliminary results of the study showed no apparent differences in functional outcomes (IPSS, Qmax), rate of SUI or irritative symptoms. Both ThuFLEP and HoLEP are efficient ways of treating benign prostatic obstruction. Both surgeries are comparable in terms of duration and postoperative complication rates.
Similar content being viewed by others
Availability of data and materials
On demand.
Code availability (software application or custom code)
On demand.
References
EAU Guidelines: management of non-neurogenic Male LUTS | Uroweb n.d. https://uroweb.org/guideline/treatment-of-non-neurogenic-male-luts/#5 (Accessed February 5, 2021)
Kuntz RM, Lehrich K, Ahyai SA (2008) Holmium laser enucleation of the prostate versus open prostatectomy for prostates greater than 100 grams: 5-Year Follow-Up Results of a Randomised Clinical Trial. Eur Urol 53:160–168. https://doi.org/10.1016/j.eururo.2007.08.036
Benign Prostatic Hyperplasia (BPH) Guideline - American Urological Association n.d. https://www.auanet.org/guidelines/guidelines/benign-prostatic-hyperplasia-(bph)-guideline (Accessed July 27, 2021)
Cornu J-NN, Ahyai S, Bachmann A, De La Rosette J, Gilling P, Gratzke C, et al (2015) A systematic review and meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic obstruction: An update. vol. 67. Elsevier https://doi.org/10.1016/j.eururo.2014.06.017
Tooher R, Sutherland P, Costello A, Gilling P, Rees G, Maddern G (2004) A systematic review of holmium laser prostatectomy for benign prostatic hyperplasia. J Urol 171:1773–1781. https://doi.org/10.1097/01.ju.0000113494.03668.6d
Ahyai SA, Gilling P, Kaplan SA, Kuntz RM, Madersbacher S, Montorsi F et al (2010) Meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic enlargement. Eur Urol 58:384–397. https://doi.org/10.1016/j.eururo.2010.06.005
Enikeev D, Glybochko P, Okhunov Z, Alyaev Y, Rapoport L, Tsarichenko D et al (2018) Retrospective analysis of short-term outcomes after monopolar versus laser endoscopic enucleation of the prostate: a single center experience. J Endourol 32:417–423. https://doi.org/10.1089/end.2017.0898
Enikeev D, Rapoport L, Gazimiev M, Allenov S, Inoyatov J, Taratkin M et al (2020) Monopolar enucleation versus transurethral resection of the prostate for small- and medium-sized (< 80 cc) benign prostate hyperplasia: a prospective analysis. World J Urol 38:167–173. https://doi.org/10.1007/s00345-019-02757-z
Peyronnet B, Robert G, Comat V, Rouprêt M, Gomez-Sancha F, Cornu J-NN, et al (2017) Learning curves and perioperative outcomes after endoscopic enucleation of the prostate: a comparison between GreenLight 532-nm and holmium lasers. World J Urol 35:973–983. https://doi.org/10.1007/s00345-016-1957-5.
Herrmann TRWW (2016) Enucleation is enucleation is enucleation is enucleation. World J Urol 34:1353–1355. https://doi.org/10.1007/s00345-016-1922-3
Pallauf M, Kunit T, Ramesmayer C, Deininger S, Herrmann TRW, Lusuardi L. Endoscopic enucleation of the prostate (EEP). The same but different—a systematic review. World J Urol 2021. https://doi.org/10.1007/s00345-021-03705-6.
Fried NMM, Murray KEE (2005) New technologies in endourology: High-power thulium fiber laser ablation of urinary tissues at 1.94 μm. J Endourol 19:25–31. https://doi.org/10.1089/end.2005.19.25
Enikeev D, Netsch C, Rapoport L, Gazimiev M, Laukhtina E, Snurnitsyna O et al (2019) Novel thulium fiber laser for endoscopic enucleation of the prostate: A prospective comparison with conventional transurethral resection of the prostate. Int J Urol 26:1138–1143. https://doi.org/10.1111/iju.14115
Sealed Envelope | Power calculator for binary outcome non-inferiority trial n.d. https://www.sealedenvelope.com/power/binary-noninferior/ (Accessed February 5, 2021)
Enikeev D, Taratkin M, Laukhtina E, Alekseeva T, Snurnitsyna O, Potoldykova N et al (2019) En bloc and two-lobe techniques for laser endoscopic enucleation of the prostate: retrospective comparative analysis of peri- and postoperative outcomes. Int Urol Nephrol 51:1969–1974. https://doi.org/10.1007/s11255-019-02259-2
Taratkin M, Kovalenko A, Laukhtina E, Paramonova N, Spivak L, Wachtendorf LJJ et al (2020) Ex vivo study of Ho:YAG and thulium fiber lasers for soft tissue surgery: which laser for which case? Lasers Med Sci. https://doi.org/10.1007/s10103-020-03189-7
Bach T, Wendt-Nordahl G, Michel MS, Herrmann TRW, Gross AJ (2009) Feasibility and efficacy of Thulium:YAG laser enucleation (VapoEnucleation) of the prostate. World J Urol 27:541–545. https://doi.org/10.1007/s00345-008-0370-0
Becker B, Herrmann TRW, Gross AJ, Netsch C (2018) Thulium vapoenucleation of the prostate versus holmium laser enucleation of the prostate for the treatment of large volume prostates: preliminary 6-month safety and efficacy results of a prospective randomized trial. World J Urol 36:1663–1671. https://doi.org/10.1007/s00345-018-2321-8
Herrmann TRW, Bach T, Imkamp F, Georgiou A, Burchardt M, Oelke M et al (2010) Thulium laser enucleation of the prostate (ThuLEP): Transurethral anatomical prostatectomy with laser support. Introduction of a novel technique for the treatment of benign prostatic obstruction. World J Urol 28:45–51. https://doi.org/10.1007/s00345-009-0503-0
Enikeev D, Glybochko P, Rapoport L, Gahan J, Gazimiev M, Spivak L et al (2018) A randomized trial comparing the learning curve of 3 endoscopic enucleation techniques (HoLEP, ThuFLEP, and MEP) for BPH Using Mentoring Approach—Initial Results. Urology 121:51–57. https://doi.org/10.1016/j.urology.2018.06.045
Fried NM (2006) Therapeutic applications of lasers in urology: an update. Expert Rev Med Devices 3:81–94. https://doi.org/10.1586/17434440.3.1.81
Romero-Otero J, García-Gómez B, García-González L, García-Rojo E, Abad-López P, Justo-Quintas J et al (2020) Critical analysis of a multicentric experience with holmium laser enucleation of the prostate for benign prostatic hyperplasia: outcomes and complications of 10 years of routine clinical practice. BJU Int 126:177–182. https://doi.org/10.1111/bju.15028
Houssin V, Olivier J, Brenier M, Pierache A, Laniado M, Mouton M et al (2020) Predictive factors of urinary incontinence after holmium laser enucleation of the prostate: a multicentric evaluation. World J Urol. https://doi.org/10.1007/s00345-020-03169-0
Fallara G, Capogrosso P, Schifano N, Costa A, Candela L, Cazzaniga W et al (2020) Ten-year follow-up results after holmium laser enucleation of the prostate. Eur Urol Focus 7:5–10. https://doi.org/10.1016/j.euf.2020.05.012
Elmansy HM, Kotb A, Elhilali MM (2011) Holmium laser enucleation of the prostate: Long-term durability of clinical outcomes and complication rates during 10 years of followup. J Urol 186:1972–1976. https://doi.org/10.1016/j.juro.2011.06.065
Enikeev D, Okhunov Z, Rapoport L, Taratkin M, Enikeev M, Snurnitsyna O et al (2019) Novel thulium fiber laser for enucleation of prostate: a retrospective comparison with open simple prostatectomy. J Endourol 33:16–21. https://doi.org/10.1089/end.2018.0791
Herrmann TRW, Gravas S, de la Rosette JJ, Wolters M, Anastasiadis AG, Giannakis I (2020) Lasers in transurethral enucleation of the prostate—Do we really need them. J Clin Med 9:1412. https://doi.org/10.3390/jcm9051412
Morozov A, Taratkin M, Kozlov V, Tarasov A, Bezrukov E, Enikeev M et al (2020) Retrospective assessment of endoscopic enucleation of prostate complications: a single-center experience of more than 1400 patients. J Endourol 34:192–197. https://doi.org/10.1089/end.2019.0630
Nottingham CU, Large T, Agarwal DK, Rivera ME, Krambeck AE (2021) Comparison of newly optimized Moses technology vs standard holmium:YAG for endoscopic laser enucleation of the prostate. J Endourol 35:1393–1399. https://doi.org/10.1089/end.2020.0996
Nevo A, Faraj KS, Cheney SM, Moore JP, Stern KL, Borofsky M et al (2021) Holmium laser enucleation of the prostate using Moses 2.0 vs non-Moses: a randomised controlled trial. BJU Int 127:553–9. https://doi.org/10.1111/bju.15265
Rücker F, Lehrich K, Böhme A, Zacharias M, Ahyai SA, Hansen J (2021) A call for HoLEP: en-bloc vs. two-lobe vs. three-lobe. World J Urol 39:2337–45. https://doi.org/10.1007/s00345-021-03598-5
Acknowledgements
None.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
DE: data analysis, manuscript editing, protocol development, management; MT: manuscript writing/editing, protocol development, data analysis, statistical analysis; DB: manuscript writing/editing, data analysis, statistical analysis; AM: manuscript editing, protocol development, data analysis; VP: manuscript writing/editing, data analysis, statistical analysis; RS: data analysis, manuscript editing, full-text review; ES: data analysis, manuscript editing, full-text review; VM: data analysis, manuscript editing, full-text review; DC: data analysis, manuscript editing, full-text review; ME: data analysis, manuscript editing, full-text review; TH: protocol development, manuscript editing, full-text review.
Corresponding author
Ethics declarations
Conflict of interests
The authors have no competing interests.
Ethical approval
The study was approved by the Sechenov University (Moscow, Russia) Institutional Review Board.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Enikeev, D., Taratkin, M., Babaevskaya, D. et al. Randomized prospective trial of the severity of irritative symptoms after HoLEP vs ThuFLEP. World J Urol 40, 2047–2053 (2022). https://doi.org/10.1007/s00345-022-04046-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-022-04046-8