Abstract
Purpose
The aim of this study is to review the current literature that reports outcomes of Peyronie’s disease (PD) reconstructive surgery using the collagen fleece TachoSil® (Baxter, CA, USA), a novel graft that has self-adhesive properties and gained popularity in recent years.
Methods
A literature review was performed through PubMed between 2013 and 2018 regarding the use of TachoSil® in PD penile reconstructive surgery. Keywords used for the search were: Peyronie’s disease, surgical therapy, surgical outcomes, grafting techniques, graft materials, collagen fleece, surgical patch, and TachoSil.
Results
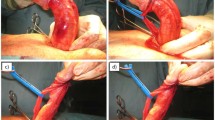
Grafting procedures are indicated for men with PD and preserved erectile function. TachoSil® is a novel graft used for defect closure after tunical incision or partial plaque excision. Long-term results of this technique are encouraging and reliable. One major advantage over other grafts is that the TachoSil® does not require suture fixation leading to significantly decreased operative times. Another indication is residual curvature correction by plaque incision and grafting/sealing with TachoSil® during penile prosthesis implantation in patients with PD and severe erectile dysfunction. Besides reduced operative times, the major advantage is that there is no risk of device puncture because of the self-adhesive properties of the TachoSil®.
Conclusions
The TachoSil® has emerged as a safe, reliable, and promising graft in PD reconstructive surgery. Until now, this graft has met the expectations as a durable and effective graft, not only for grafting techniques but also for residual curvature correction during penile prosthesis implantation. However, future research is encouraged, preferably within prospective multicenter studies.




Similar content being viewed by others
References
Chung E, Ralph D, Kagioglu A, Garaffa G, Shamsodini A, Bivalacqua T, Glina S, Hakim L, Sadeghi-Nejad H, Broderick G (2016) Evidence-based management guidelines on Peyronie’s disease. J Sex Med 13:905–923
Hatzichristodoulou G, Osmonov D, Kübler H, Hellstrom WJG, Yafi FA (2017) Contemporary review of grafting techniques for the surgical treatment of Peyronie’s disease. Sex Med Rev 5:544–552
Brimley S, Yafi FA, Greenberg J, Hellstrom WJG, Tue Nguyen HM, Hatzichristodoulou G (2018) Review of management options for active-phase Peyronie’s disease. Sex Med Rev. https://doi.org/10.1016/j.sxmr.2018.09.007
Yafi F, Diao L, DeLay KJ, DeYoung L, Talib R, Alzweri L, Brock G, Hellstrom WJG, Hatzichristodoulou G (2018) Multi-institutional prospective analysis of intralesional injection of collagenase Clostridium histolyticum, tunical plication, and partial plaque excision and grafting for the management of Peyronie’s disease. Urology 120:138–142
Garcia-Gomez B, Ralph D, Levine L, Moncada-Iribarren I, Djinovic R, Albersen M, Garcia-Cruz E, Romero-Otero J (2018) Grafts for Peyronie’s disease: a comprehensive review. Andrology 6:117–126
Hatzichristodoulou G (2016) Grafting techniques for Peyronie’s disease. Transl Androl Urol 5:334–341
Siemer S, Lahme S, Altziebler S, Machtens S, Strohmaier W, Wechsel HW, Goebell P, Schmeller N, Oberneder R, Stolzenburg JU, Becker H, Lüftenegger W, Tetens V, Van Poppel H (2007) Efficacy and safety of TachoSil as haemostatic treatment versus standard suturing in kidney tumour resection: a randomised prospective study. Eur Urol 52:1156–1163
Simonato A, Varca V, Esposito M, Venzano F, Carmignani G (2009) The use of a surgical patch in the prevention of lymphoceles after extraperitoneal pelvic lymphadenectomy for prostate cancer: a randomized prospective pilot study. J Urol 182:2285–2290
Hatzichristodoulou G, Gschwend JE, Lahme S (2013) Surgical therapy of Peyronie’s disease by partial plaque excision and grafting with collagen fleece: feasibility study of a new technique. Int J Impot Res 25:183–187
Lahme S, Götz T, Bichler KH (2001) Collagen fleece for defect coverage following plaque excision in patients with Peyronie’s disease. Eur Urol 41:401–405
Horstmann M, Kwol M, Amend B, Hennenlotter J, Stenzl A (2011) A self-reported long-term follow-up of patients operated with either shortening techniques or a TachoSil grafting procedure. Asian J Androl 13:326–331
Hatzichristodoulou G (2016) Partial plaque excision and grafting with collagen fleece in Peyronie disease. J Sex Med 13:277–281
Hatzichristodoulou G (2016) Surgical therapy of Peyronie’s disease by partial plaque excision and Sealing of tunical defect with collagen fleece: the Sealing technique. Video J Prosth Urol 2:076
Hatzichristodoulou G, Fiechtner S, Gschwend JE, Kübler H, Lahme S (2017) Suture-free sealing of tunical defect with collagen fleece after partial plaque excision in Peyronie’s disease: long-term outcomes of the Sealing technique. Eur Urol Suppl 16(3):e2152
Rosenhammer B, Sayedahmed K, Fritsche HM, Burger M, Kübler H, Hatzichristodoulou G (2018) Long-term outcome after grafting with small intestinal submucosa and collagen fleece in patients with Peyronie’s disease: a matched pair analysis. Int J Impot Res. https://doi.org/10.1038/s41443-018-0071-1
Fabiani A, Fioretti F, Filosa A, Servi L, Mammana G (2015) Patch bulging after plaque incision and grafting procedure for Peyronie’s disease. Surgical repair with a collagen fleece. Arch Ital Urol Androl 87:173–174
Hatzichristodoulou G (2018) Introducing the ventral sealing technique using collagen fleece for surgical therapy of patients with ventral Peyronie’s curvature: initial experience. Int J Impot Res 30:306–311
Mulhall J, Schiff J, Guhring P (2006) An analysis of the natural history of Peyronie’s disease. J Urol 175:2115–2118
Yafi F, Hatzichristodoulou G, Knoedler CJ, Trost LW, Sikka SC, Hellstrom WJ (2015) Comparative analysis of tunical plication vs intralesional injection therapy for ventral Peyronie’s disease. J Sex Med 12:2492–2498
Hatzichristodoulou G, Tsambarlis P, Kübler H, Levine LA (2017) Peyronie’s graft surgery—tips and tricks from the masters in andrologic surgery. Transl Androl Urol 6:645–656
Wilson SK, Delk JR II (1994) A new treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol 152:1121–1123
Anaissie J, Yafi FA (2016) A review of surgical strategies for penile prosthesis implantation in patients with Peyronie’s disease. Transl Androl Urol 5:342–350
Wilson SK, Cleves MA, Delk JR II (2001) Long-term follow-up of treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol 165:825–829
Carlos E, Sexton SJ, Lentz AC (2018) Urethral injury and the penile prosthesis. Sex Med Rev. https://doi.org/10.1016/j.sxmr.2018.06.003
Hatzichristodoulou G (2018) The PICS technique: a novel approach for residual curvature correction during penile prosthesis implantation in patients with severe Peyronie’s disease using the collagen fleece TachoSil. J Sex Med 15:416–421
Hatzichristodoulou G (2018) A novel approach for residual curvature correction during inflatable penile prosthesis implantation in patients with Peyronie’s disease: the PICS technique. Video J Prosth Urol 2:139
Falcone M, Preto M, Ceruti C, Timpano M, Garaffa G, Sedigh O, Sibona M, Oderda M, Gontero P, Rolle L (2018) A comparative study between 2 different grafts used as patches after plaque incision and inflatable penile prosthesis implantation for end-stage Peyronie’s disease. J Sex Med 15:848–852
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that he has no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by the author.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hatzichristodoulou, G. Evolution of the surgical sealing patch TachoSil® in Peyronie’s disease reconstructive surgery: technique and contemporary literature review. World J Urol 38, 315–321 (2020). https://doi.org/10.1007/s00345-019-02792-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-019-02792-w