Abstract
Purpose
To compare the pain control efficacies of the pelvic plexus block (PPB), periprostatic nerve block (PNB), and controls during a 14-core basal and apical core prostate biopsy.
Methods
This randomized controlled study, performed between January 2015 and January 2016, included patients with an abnormal serum prostate-specific antigen (PSA > 3 ng/mL) level or a palpable nodule on digital rectal examination. The enrolled patients were randomized into three groups: Group 1, intrarectal local anesthesia (IRLA, 10 mL of 2% lidocaine jelly) and PPB with 3.0 mL of 2% lidocaine injected at the bilateral pelvic plexus; Group 2, IRLA and PNB with 3.0 mL of 2% lidocaine injected at both periprostatic nerves; and Group 3, only IRLA. Patients answered the visual analog scale (VAS) questionnaire at 6 time points.
Results
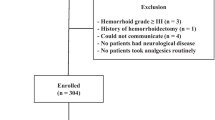
This study consisted of 163 patients (Group 1 = 55, Group 2 = 55, and Group 3 = 53). Pain at the apical biopsy location was less in Groups 1 and 2 than in Group 3 (p < 0.001, p < 0.001) and between the two local anesthetic groups (PNB + IRLA vs PPB + IRLA). Group 2 patients reported less pain than Group 1 patients (p = 0.022). Pain during the basal core biopsy was significantly less in Groups 1 and 2 than in Group 3 (p = 0.002, p < 0.001), but there were no significant differences in pain control between the two methods (PNB + IRLA vs PPB + IRLA, p = 0.054) during basal core biopsy.
Conclusions
PNB + IRLA is an effective local anesthetic method for reducing pain when performing apical biopsies compared with PPB + IRLA or IRLA alone.

Similar content being viewed by others
References
Eastham J (2017) Prostate cancer screening. Investig Clin Urol 58:217–219. https://doi.org/10.4111/icu.2017.58.4.217
Heidenreich A, Bastian PJ, Bellmunt J, Bolla M, Joniau S, van der Kwast T, Mason M, Matveev V, Wiegel T, Zattoni F, Mottet N (2014) EAU guidelines on prostate cancer. part 1: screening, diagnosis, and local treatment with curative intent—update 2013. Eur Urol 65:124–137. https://doi.org/10.1016/j.eururo.2013.09.046
Akduman B, Akduman D, Tokgoz H, Erol B, Turker T, Ayoglu F, Mungan NA (2011) Long-term fluoroquinolone use before the prostate biopsy may increase the risk of sepsis caused by resistant microorganisms. Urology 78:250–255. https://doi.org/10.1016/j.urology.2011.02.065
Gaylis F, Nasseri R, Fink L, Calabrese R, Dato P, Cohen E (2016) Prostate biopsy complications: a dual analysis. Urology 93:135–140. https://doi.org/10.1016/j.urology.2016.03.035
Nash PA, Bruce JE, Indudhara R, Shinohara K (1996) Transrectal ultrasound guided prostatic nerve blockade eases systematic needle biopsy of the prostate. J Urol 155:607–609. https://doi.org/10.1016/S0022-5347(01)66464-4
Li M, Wang Z, Li H, Yang J, Rao K, Wang T, Wang S, Liu J (2017) Local anesthesia for transrectal ultrasound-guided biopsy of the prostate: a meta-analysis. Sci Rep 7:40421. https://doi.org/10.1038/srep40421
Adamakis I, Mitropoulos D, Haritopoulos K, Alamanis C, Stravodimos K, Giannopoulos A (2004) Pain during transrectal ultrasonography guided prostate biopsy: a randomized prospective trial comparing periprostatic infiltration with lidocaine with the intrarectal instillation of lidocaine-prilocain cream. World J Urol 22:281–284. https://doi.org/10.1007/s00345-003-0386-4
Alavi AS, Soloway MS, Vaidya A, Lynne CM, Gheiler EL (2001) Local anesthesia for ultrasound guided prostate biopsy: a prospective randomized trial comparing 2 methods. J Urol 166:1343–1345. https://doi.org/10.1016/S0022-5347(05)65765-5
Autorino R, De Sio M, Di Lorenzo G, Damiano R, Perdona S, Cindolo L, D’Armiento M (2005) How to decrease pain during transrectal ultrasound guided prostate biopsy: a look at the literature. J Urol 174:2091–2097. https://doi.org/10.1097/01.ju.0000181212.51025.06
Wu CL, Carter HB, Naqibuddin M, Fleisher LA (2001) Effect of local anesthetics on patient recovery after transrectal biopsy. Urology 57:925–929. https://doi.org/10.1016/S0090-4295(01)00930-X
Akpinar H, Tufek I, Atug F, Esen EH, Kural AR (2009) Doppler ultrasonography-guided pelvic plexus block before systematic needle biopsy of the prostate: a prospective randomized study. Urology 74:267–271.e261. https://doi.org/10.1016/j.urology.2009.01.082
Cantiello F, Cicione A, Autorino R, Cosentino C, Amato F, Damiano R (2012) Pelvic plexus block is more effective than periprostatic nerve block for pain control during office transrectal ultrasound guided prostate biopsy: a single center, prospective, randomized, double arm study. J Urol 188:417–422. https://doi.org/10.1016/j.juro.2012.04.003
Jindal T, Mukherjee S, Sinha RK, Kamal MR, Ghosh N, Saha B, Mitra N, Sharma PK, Mandal SN, Karmakar D (2015) Transrectal ultrasonography (TRUS)-guided pelvic plexus block to reduce pain during prostate biopsy: a randomised controlled trial. BJU Int 115:892–896. https://doi.org/10.1111/bju.12872
Hollabaugh RS Jr, Dmochowski RR, Steiner MS (1997) Neuroanatomy of the male rhabdosphincter. Urology 49:426–434. https://doi.org/10.1016/s0090-4295(96)00497-9
Stirling BN, Shockley KF, Carothers GG, Maatman TJ (2002) Pain perception during transrectal ultrasound guided prostate needle biopsy: an objective analysis of local anesthesia use. Prostate Cancer Prostatic Dis 5:209–211. https://doi.org/10.1038/sj.pcan.4500598
Berger AP, Frauscher F, Halpern EJ, Spranger R, Steiner H, Bartsch G, Horninger W (2003) Periprostatic administration of local anesthesia during transrectal ultrasound-guided biopsy of the prostate: a randomized, double-blind, placebo-controlled study. Urology 61:585–588. https://doi.org/10.1016/S0090-4295(02)02406-8
Stirling BN, Shockley KF, Carothers GG, Maatman TJ (2002) Comparison of local anesthesia techniques during transrectal ultrasound-guided biopsies. Urology 60:89–92. https://doi.org/10.1016/S0090-4295(02)01671-0
Moussa AS, Meshref A, Schoenfield L, Masoud A, Abdel-Rahman S, Li J, Flazoura S, Magi-Galluzzi C, Fergany A, Fareed K, Jones JS (2010) Importance of additional “extreme” anterior apical needle biopsies in the initial detection of prostate cancer. Urology 75:1034–1039. https://doi.org/10.1016/j.urology.2009.11.008
Soloway MS, Obek C (2000) Periprostatic local anesthesia before ultrasound guided prostate biopsy. J Urol 163:172–173. https://doi.org/10.1016/S0022-5347(05)67997-9
Yan P, Wang XY, Huang W, Zhang Y (2016) Local anesthesia for pain control during transrectal ultrasound-guided prostate biopsy: a systematic review and meta-analysis. J Pain Res 9:787–796. https://doi.org/10.2147/jpr.S117451
Bastide C, Lechevallier E, Eghazarian C, Ortega JC, Coulange C (2003) Tolerance of pain during transrectal ultrasound-guided biopsy of the prostate: risk factors. Prostate Cancer Prostatic Dis 6:239–241. https://doi.org/10.1038/sj.pcan.4500664
Ochiai A, Babaian RJ (2004) Update on prostate biopsy technique. Curr Opin Urol 14:157–162
Bjurlin MA, Carter HB, Schellhammer P, Cookson MS, Gomella LG, Troyer D, Wheeler TM, Schlossberg S, Penson DF, Taneja SS (2013) Optimization of initial prostate biopsy in clinical practice: sampling, labeling and specimen processing. J Urol 189:2039–2046. https://doi.org/10.1016/j.juro.2013.02.072
Guo LH, Wu R, Xu HX, Xu JM, Wu J, Wang S, Bo XW, Liu BJ (2015) Comparison between ultrasound guided transperineal and transrectal prostate biopsy: a prospective, randomized, and controlled trial. Sci Rep 5:16089. https://doi.org/10.1038/srep16089
Pepe P, Aragona F (2014) Prostate biopsy: results and advantages of the transperineal approach—twenty-year experience of a single center. World J Urol 32:373–377. https://doi.org/10.1007/s00345-013-1108-1
Funding
This work was supported by Gangneung Asan Hospital Medical Institute and was funded by the Asan Foundation (2014-009).
Author information
Authors and Affiliations
Contributions
SJK: data management, data analysis, manuscript writing/editing. JL: data collection, data analysis. DHA: data collection data analysis. CP: data analysis. JHL: project development. HGK: manuscript writing/editing. JYP: project development, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kim, S.J., Lee, J., An, D.H. et al. A randomized controlled comparison between periprostatic nerve block and pelvic plexus block at the base and apex of 14-core prostate biopsies. World J Urol 37, 2663–2669 (2019). https://doi.org/10.1007/s00345-019-02722-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-019-02722-w