Abstract
Introduction
Bladder cancer (BCa) is three-to-four times more common in men than in women. To explain this gender gap, several theories have been proposed, including the impact of androgen hormones. The aim of this study was to investigate the differential impact of androgen deprivation therapy (ADT) on subsequent risk of developing BCa in men with prostate cancer (PCa).
Methods
A total of 196,914 patients diagnosed with histologically confirmed localized PCa between 2000 and 2009 were identified in the SEER-Medicare insurance program-linked database. Competing-risk regression analyses were performed to assess the risk of developing BCa adjusting for the risk of all-cause mortality. Univariable and multivariable competing-risk regression analyses were performed to test the effect of ADT on BCa incidence for each PCa treatment modality.
Results
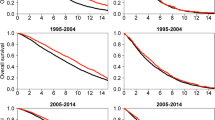
Of the 196,914 individuals included in the study, 68,421 (34.7%) received ADT. Median (IQR) follow-up was 59 (29–95) months. Overall, a total of 2495 (1.3%) individuals developed BCa during follow-up. After stratification according to ADT, the 10-year cumulative incidence rate was 1.75% (95% CI 1.65–1.85). In the untreated group, the 10-year cumulative incidence rate was 1.99% (95% CI 1.83–2.15). In multivariable competing-risk regression, the use of ADT was not associated with BCa, after accounting for the risk of dying from any cause (p = 0.1).
Conclusion
We failed to identify any impact of ADT on the risk of developing a subsequent BCa even after stratifying according to the type of treatment. Further studies are required to explain the gender gap in BCa incidence and outcomes.

Similar content being viewed by others
References
Fajkovic H, Halpern JA, Cha EK, Bahadori A, Chromecki TF, Karakiewicz PI et al (2011) Impact of gender on bladder cancer incidence, staging, and prognosis. World J Urol 29:457–463. https://doi.org/10.1007/s00345-011-0709-9
Kluth LA, Rieken M, Xylinas E, Kent M, Rink M, Rouprêt M et al (2014) Gender-specific differences in clinicopathologic outcomes following radical cystectomy: an international multi-institutional study of more than 8000 patients. Eur Urol 66:913–919. https://doi.org/10.1016/j.eururo.2013.11.040
Messer JC, Shariat SF, Dinney CP, Novara G, Fradet Y, Kassouf W et al (2014) Female gender is associated with a worse survival after radical cystectomy for urothelial carcinoma of the bladder: a competing risk analysis. Urology 83:863–867. https://doi.org/10.1016/j.urology.2013.10.060
Dobruch J, Daneshmand S, Fisch M, Lotan Y, Noon AP, Resnick MJ et al (2016) Gender and bladder cancer: a collaborative review of etiology, biology, and outcomes. Eur Urol 69:300–310. https://doi.org/10.1016/j.eururo.2015.08.037
Cumberbatch MGK, Cox A, Teare D, Catto JWF (2015) Contemporary occupational carcinogen exposure and bladder cancer. JAMA Oncol 1(9):1282–1290. https://doi.org/10.1001/jamaoncol.2015.3209
Zhuang YH, Bläuer M, Tammela T, Tuohimaa P (1997) Immunodetection of androgen receptor in human urinary bladder cancer. Histopathology 30:556–562
Salmi S, Santti R, Gustafsson JA, Mäkelä S (2001) Co-localization of androgen receptor with estrogen receptor beta in the lower urinary tract of the male rat. J Urol 166:674–677
Waliszewski P, Waliszewska MK, Hemstreet GP, Hurst RE (1997) Expression of sex steroid receptor genes and comodulation with retinoid signaling in normal human uroepithelial cells and bladder cancer cell lines. Urol Oncol 3:141–147
Miyamoto H, Yang Z, Chen Y-T, Ishiguro H, Uemura H, Kubota Y et al (2007) Promotion of bladder cancer development and progression by androgen receptor signals. J Natl Cancer Inst 99:558–568. https://doi.org/10.1093/jnci/djk113
Bertram JS, Craig AW (1972) Specific induction of bladder cancer in mice by butyl-(4-hydroxybutyl)-nitrosamine and the effects of hormonal modifications on the sex difference in response. Eur J Cancer 8:587–594
Pour PM, Stepan K (1987) Induction of prostatic carcinomas and lower urinary tract neoplasms by combined treatment of intact and castrated rats with testosterone propionate and N-nitrosobis(2-oxopropyl)amine. Cancer Res 47:5699–5706
Terada S, Suzuki N, Uchide K, Akasofu K, Nishida E (1992) Effect of testosterone on the development of bladder tumors and calculi in female rats. Gynecol Obstet Invest 34:105–110
Matsuki K, Akaza H, Aso Y (1992) Effects of luteinizing hormone-releasing hormone agonist on bladder carcinogenesis in male rats. Nihon Hinyōkika Gakkai Zasshi Jpn J Urol 83:1452–1458
Shiota M, Takeuchi A, Yokomizo A, Kashiwagi E, Tatsugami K, Kuroiwa K et al (2012) Androgen receptor signaling regulates cell growth and vulnerability to doxorubicin in bladder cancer. J Urol 188:276–286. https://doi.org/10.1016/j.juro.2012.02.2554
Lombard AP, Mudryj M (2015) The emerging role of the androgen receptor in bladder cancer. Endocr Relat Cancer 22:R265–R277. https://doi.org/10.1530/erc-15-0209
Lucca I, Fajkovic H, Klatte T (2014) Sex steroids and gender differences in nonmuscle invasive bladder cancer. Curr Opin Urol 24:500–505. https://doi.org/10.1097/mou.0000000000000092
Izumi K, Ito Y, Miyamoto H, Miyoshi Y, Ota J, Moriyama M et al (2016) Expression of androgen receptor in non-muscle-invasive bladder cancer predicts the preventive effect of androgen deprivation therapy on tumor recurrence. Oncotarget 1:1–8. https://doi.org/10.18632/oncotarget.7358
Shiota M, Yokomizo A, Takeuchi A, Imada K, Kiyoshima K, Inokuchi J et al (2015) Secondary bladder cancer after anticancer therapy for prostate cancer: reduced comorbidity after androgen-deprivation therapy. Oncotarget 6:14710–14719
Warren JL, Klabunde CN, Schrag D, Bach PB, Riley GF (2002) Overview of the SEER-Medicare data: content, research applications, and generalizability to the United States elderly population. Med Care 40:IV3–IV18. https://doi.org/10.1097/01.mlr.0000020942.47004.03
Wong Y-N, Mitra N, Hudes G, Localio R, Schwartz JS, Wan F et al (2006) Survival associated with treatment vs observation of localized prostate cancer in elderly men. JAMA 296:2683. https://doi.org/10.1001/jama.296.22.2683
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619. https://doi.org/10.1016/0895-4356(92)90133-8
McGrath M, Michaud DS, De Vivo I (2006) Hormonal and reproductive factors and the risk of bladder cancer in women. Am J Epidemiol 163:236–244. https://doi.org/10.1093/aje/kwj028
Boorjian S, Ugras S, Mongan NP, Gudas LJ, You X, Tickoo SK et al (2004) Androgen receptor expression is inversely correlated with pathologic tumor stage in bladder cancer. Urology 64:383–388. https://doi.org/10.1016/j.urology.2004.03.025
Mashhadi R, Pourmand G, Kosari F, Mehrsai A, Salem S, Pourmand MR et al (2014) Role of steroid hormone receptors in formation and progression of bladder carcinoma: a case-control study. Urol J 11:1968–1973
Mir C, Shariat SF, van der Kwast TH, Ashfaq R, Lotan Y, Evans A et al (2011) Loss of androgen receptor expression is not associated with pathological stage, grade, gender or outcome in bladder cancer: a large multi-institutional study. BJU Int 108:24–30. https://doi.org/10.1111/j.1464-410x.2010.09834.x
Sathianathen NJ, Fan Y, Jarosek SL, Lawrentschuk NL, Konety BR (2018) Finasteride does not prevent bladder cancer: a secondary analysis of the medical therapy for prostatic symptoms study. Urol Oncol 36:338.e13–338.e17. https://doi.org/10.1016/j.urolonc.2018.03.020
Morales EE, Grill S, Svatek RS, Kaushik D, Thompson IM, Ankerst DP et al (2016) Finasteride reduces risk of bladder cancer in a large prospective screening study. Eur Urol 69:407–410. https://doi.org/10.1016/j.eururo.2015.08.029
Moschini M, D’Andrea D, Korn S, Irmak Y, Soria F, Compérat E et al (2017) Characteristics and clinical significance of histological variants of bladder cancer. Nat Rev Urol 14:11. https://doi.org/10.1038/nrurol.2017.125
Ma JL, Hennessey DB, Newell BP, Bolton DM, Lawrentschuk N (2018) Radiotherapy-related complications presenting to a urology department: a more common problem than previously thought? BJU Int 121:28–32. https://doi.org/10.1111/bju.14145
Author information
Authors and Affiliations
Contributions
MM: data collection, statistical analysis, manuscript writing; EZ: data collection, statistical analysis, manuscript writing; PK: project development, manuscript writing; AM: project development, manuscript writing; GG: data collection; NF: data collection; FM: data collection; AB: data collection; SFS: project development, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
All participants gave their informed consent to use their data for this retrospective study involving human participants.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Moschini, M., Zaffuto, E., Karakiewicz, P. et al. The effect of androgen deprivation treatment on subsequent risk of bladder cancer diagnosis in male patients treated for prostate cancer. World J Urol 37, 1127–1135 (2019). https://doi.org/10.1007/s00345-018-2504-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2504-3