Abstract
Objectives
To investigate the normal-appearing white matter (NAWM) susceptibility in a cohort of newly diagnosed multiple sclerosis (MS) patients and to evaluate possible correlations between NAWM susceptibility and disability progression.
Methods
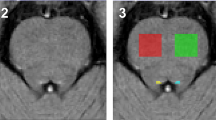
Fifty-nine patients with a diagnosis of MS (n = 53) or clinically isolated syndrome (CIS) (n = 6) were recruited and followed up. All participants underwent neurological examination, blood sampling for serum neurofilament light chain (sNfL) level assessment, lumbar puncture for the quantification of cerebrospinal fluid (CSF) β-amyloid1-42 (Aβ) levels, and brain MRI. T2-weighted scans were used to quantify white matter (WM) lesion loads. For each scan, we derived the NAWM volume fraction and the WM lesion volume fraction. Quantitative susceptibility mapping (QSM) of the NAWM was calculated using the susceptibility tensor imaging (STI) suite. Susceptibility maps were computed with the STAR algorithm.
Results
Primary progressive patients (n = 9) showed a higher mean susceptibility value in the NAWM than relapsing-remitting (n = 44) and CIS (n = 6) (p = 0.01 and p = 0.02). Patients with a higher susceptibility in the NAWM showed increased sNfL concentration (ρ = 0.38, p = 0.004) and lower CSF Aβ levels (ρ = −0.34, p = 0.009). Mean NAWM susceptibility turned out to be a predictor of the expanded disability status scale (EDSS) worsening at follow-up (β = 0.41, t = 2.66, p = 0.01) and of the MS severity scale (MSSS) (β = 0.38, t = 2.43, p = 0.019).
Conclusions
QSM in the NAWM seems to predict the EDSS increment over time. This finding might provide evidence on the role of QSM in identifying patients with an increased risk of early disability progression.
Key Points
• NAWM-QSM is higher in PPMS patients than in RRMS.
• NAWM-QSM seems to be a predictor of EDSS worsening over time.
• Patients with higher NAWM-QSM show increased sNfL concentration and lower CSF Aβ levels.



Similar content being viewed by others
Abbreviations
- Aβ:
-
β-Amyloid1-42
- CIS:
-
Clinically isolated syndrome
- CSF:
-
Cerebrospinal fluid
- EDSS:
-
Expanded disability status scale
- MRI:
-
Magnetic resonance imaging
- MS:
-
Multiple sclerosis
- MSSS:
-
Multiple sclerosis severity score
- NAWM:
-
Normal-appearing white matter
- NAWM-QSM:
-
mean QSM value in the NAWM mask
- NAWM-VF:
-
NAWM volume fraction
- PPMS:
-
Primary progressive MS
- QSM:
-
Quantitative susceptibility mapping
- RRMS:
-
Relapsing remitting MS
- sNfL:
-
Serum neurofilament light chain
- WM:
-
White matter
- WMLs:
-
White matter lesions
- WMLs-QSM:
-
Mean QSM value in the lesion mask
References
Reich DS, Lucchinetti CF, Calabresi PA (2018) Multiple sclerosis. N Engl J Med 378(2):169–180
Frischer JM, Bramow S, Dal-Bianco A et al (2009) The relation between inflammation and neurodegeneration in multiple sclerosis brains. Brain 132(Pt 5):1175–1189
Lassmann H (2014) Multiple sclerosis: lessons from molecular neuropathology. Exp Neurol 262(Pt A):2–7
LeVine SM (1997) Iron deposits in multiple sclerosis and Alzheimer’s disease brains. Brain Res 760(1-2):298–303
Franklin RJ, Ffrench-Constant C (2008) Remyelination in the CNS: from biology to therapy. Nat Rev Neurosci 9(11):839–855
Thompson AJ, Banwell BL, Barkhof F et al (2018) Diagnosis of multiple sclerosis: 2017 revisions of the McDonald criteria. Lancet Neurol 7(2):162–173
Bodini B, Louapre C, Stankoff B (2015) Advanced imaging tools to investigate multiple sclerosis pathology. Presse Med 44(4 Pt 2):e159–e167
Stankoff B, Freeman L, Aigrot MS et al (2011) Imaging central nervous system myelin by positron emission tomography in multiple sclerosis using [methyl-11C]-2-(4’-methylaminophenyl)- 6-hydroxybenzothiazole. Ann Neurol 69(4):673–680
Filippi M, Paty DW, Kappos L et al (1995) Correlations between changes in disability and T2-weighted brain MRI activity in multiple sclerosis: a follow-up study. Neurology 45(2):255–260
Cree BAC, Hollenbach JA, Bove R et al (2019) Silent progression in disease activity-free relapsing multiple sclerosis. Ann Neurol 85(5):653–666
Langkammer C, Schweser F, Krebs N et al (2012) Quantitative susceptibility mapping (QSM) as a means to measure brain iron? A post mortem validation study. Neuroimage 62(3):1593–1599
Stüber C, Morawski M, Schäfer A et al (2014) Myelin and iron concentration in the human brain: a quantitative study of MRI contrast. Neuroimage 93(Pt 1):95–106
Gaeta M, Cavallaro M, Vinci SL et al (2021) Magnetism of materials: theory and practice in magnetic resonance imaging. Insights Imaging 12(1):179
Liu C, Li W, Tong KA et al (2015) Susceptibility-weighted imaging and quantitative susceptibility mapping in the brain. J Magn Reson Imaging 42(1):23–41
Wisnieff C, Ramanan S, Olesik J et al (2015) Quantitative susceptibility mapping (QSM) of white matter multiple sclerosis lesions: interpreting positive susceptibility and the presence of iron. Magn Reson Med 74(2):564–570
Bagnato F, Hametner S, Yao B et al (2011) Tracking iron in multiple sclerosis: a combined imaging and histopathological study at 7 Tesla. Brain 134(Pt 12):3602–3615
Lassmann H (2008) The pathologic substrate of magnetic resonance alterations in multiple sclerosis. Neuroimaging Clin N Am 18(4):563–576
Hametner S, Wimmer I, Haider L et al (2013) Iron and neurodegeneration in the multiple sclerosis brain. Ann Neurol 74(6):848–861
Zhang S, Nguyen TD, Hurtado Rúa SM et al (2019) Quantitative susceptibility mapping of time-dependent susceptibility changes in multiple sclerosis lesions. AJNR Am J Neuroradiol 40(6):987–993
Mehta V, Pei W, Yang G et al (2013) Iron is a sensitive biomarker for inflammation in multiple sclerosis lesions. PLoS One 8(3):e57573
Yu FF, Chiang FL, Stephens N et al (2019) Characterization of normal-appearing white matter in multiple sclerosis using quantitative susceptibility mapping in conjunction with diffusion tensor imaging. Neuroradiology 61(1):71–79
Chen W, Zhang Y, Mu K et al (2017) Quantifying the susceptibility variation of normal-appearing white matter in multiple sclerosis by quantitative susceptibility mapping. AJR Am J Roentgenol 209(4):889–894
Rudko DA, Solovey I, Gati JS et al (2014) Multiple sclerosis: improved identification of disease-relevant changes in gray and white matter by using susceptibility-based MR imaging. Radiology 272(3):851–864
Wiggermann V, Hametner S, Hernández-Torres E et al (2017) Susceptibility-sensitive MRI of multiple sclerosis lesions and the impact of normal-appearing white matter changes. NMR Biomed 30(8). https://doi.org/10.1002/nbm.3727
Pietroboni AM, Caprioli M, Carandini T et al (2019) CSF β-amyloid predicts prognosis in patients with multiple sclerosis. Mult Scler 25(9):1223–1231
Filippi M, Preziosa P, Barkhof F et al (2021) Diagnosis of progressive multiple sclerosis from the imaging perspective: a review. JAMA Neurol 78(3):351–364
Kuhle J, Kropshofer H, Haering DA et al (2019) Blood neurofilament light chain as a biomarker of MS disease activity and treatment response. Neurology 92(10):e1007–e1015
Schmidt P, Gaser C, Arsic M et al (2012) An automated tool for detection of FLAIR-hyperintense white-matter lesions in Multiple Sclerosis. Neuroimage 59(4):3774–3783
Li W, Wu B, Liu C (2011) Quantitative susceptibility mapping of human brain reflects spatial variation in tissue composition. Neuroimage 55(4):1645–1656
Schweser F, Deistung A, Lehr BW, Reichenbach JR (2011) Quantitative imaging of intrinsic magnetic tissue properties using MRI signal phase: an approach to in vivo brain iron metabolism? Neuroimage 54(4):2789–2807
Wei H, Dibb R, Zhou Y et al (2015) Streaking artifact reduction for quantitative susceptibility mapping of sources with large dynamic range. NMR Biomed 28(10):1294–1303
Langkammer C, Liu T, Khalil M et al (2013) Quantitative susceptibility mapping in multiple sclerosis. Radiology 267(2):551–559
Vinayagamani S, Sabarish S, Nair SS, Tandon V, Kesavadas C, Thomas B (2021) Quantitative susceptibility-weighted imaging in predicting disease activity in multiple sclerosis. Neuroradiology 63(7):1061–1069
Schweser F, Hagemeier J, Dwyer MG et al (2021) Decreasing brain iron in multiple sclerosis: the difference between concentration and content in iron MRI. Hum Brain Mapp 42(5):1463–1474
Deh K, Ponath GD, Molvi Z et al (2018) Magnetic susceptibility increases as diamagnetic molecules breakdown: Myelin digestion during multiple sclerosis lesion formation contributes to increase on QSM. J Magn Reson Imaging 48(5):1281–1287
Lancione M, Tosetti M, Donatelli G, Cosottini M, Costagli M (2017) The impact of white matter fiber orientation in single-acquisition quantitative susceptibility mapping. NMR Biomed 30(11). https://doi.org/10.1002/nbm.3798
Funding
This study was supported by the Italian Ministry of Health (“Ricerca Corrente” to ES and FT) and Dino Ferrari Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Anna Pietroboni.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• prospective
• observational
• cross-sectional study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pietroboni, A.M., Colombi, A., Contarino, V.E. et al. Quantitative susceptibility mapping of the normal-appearing white matter as a potential new marker of disability progression in multiple sclerosis. Eur Radiol 33, 5368–5377 (2023). https://doi.org/10.1007/s00330-022-09338-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09338-6