Abstract
Objectives
To assess the outcomes of transjugular intrahepatic portosystemic shunt (TIPS) creation using PTFE-covered stents in liver transplant (LT) recipients and to analyze the technical result of TIPS creation in split grafts (SG) compared with whole liver grafts (WG).
Methods and materials
Single-center, retrospective study, analyzing LT patients who underwent TIPS using PTFE-covered stents. Clinical and technical variables were analyzed.
Results
Between 2005 and 2021, TIPS was created using PTFE-covered stents in 48 LT patients at a median of 43 months (range, 0.5–192) after LT. TIPS indications were refractory ascites (RA) in 33 patients (69%), variceal bleeding (VB) in 9 patients (19%), others in 6 (12%). Ten patients (21%) received a SG. Technical success rate was 100% in both groups: in two WG recipients, (5%) a second attempt was required. An unconventional approach (combined transhepatic or transplenic access) was needed in 2 WG (5%) and 2 SG recipients (20%). Two procedure-related death occurred in the WG group. After a median follow-up of 22 months (range, 0,1–144), 16 patients (48%) in the RA group did not require post-TIPS paracentesis, in the VB group rebleeding occurred in 3 patients (33%). Fifteen patients (31%) underwent TIPS revision. Overt hepatic encephalopathy occurred in 14 patients (29%). Patient survival at 6 months, 1 year, and 3 years was 77%, 66%, and 43%, respectively.
Conclusions
The feasibility and safety of TIPS creation in SG are comparable to that of WG. TIPS creation using PTFE-covered stents represents a viable option to treat portal hypertensive complications in LT recipients.
Key Points
• TIPS creation using PTFE-covered stents represents a viable option to treat complications of PH in LT recipients.
• TIPS creation in LT SG recipients appears to be safe and feasible as in WG.
• Results from this study may help to refine the management of LT patients with recurrent portal hypertensive complications encouraging physicians to consider TIPS creation as a treatment option in both SG and WG recipients.



Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- CP:
-
Child-Pugh
- HE:
-
Hepatic encephalopathy
- HR:
-
Hazard ratio
- HV:
-
Hepatic vein
- IVC:
-
Inferior vena cava
- LT:
-
Liver transplant
- MELD:
-
Model for end-stage liver disease
- PH:
-
Portal hypertension
- PSG:
-
Portosystemic pressure gradient
- PTFE:
-
Polytetrafluoroethylene
- PV:
-
Portal vein
- PVT:
-
Portal vein thrombosis
- RA:
-
Refractory ascites
- SG:
-
Split graft
- TIPS:
-
Transjugular intrahepatic portosystemic shunt
- US:
-
Ultrasound
- VB:
-
Variceal bleeding
- WG:
-
Whole graft
References
Kotlyar DS, Campbell MS, Reddy KR (2006) Recurrence of diseases following orthotopic liver transplantation. Am J Gastroenterol 101:1370–1378
Bilbao JI, Herrero JI, Martinez-Cuesta A et al (2000) Ascites due to anastomotic stenosis after liver transplantation using the piggyback technique: treatment with endovascular prosthesis. Cardiovasc Intervent Radiol 232:149–151
Bonnel AR, Bunchorntavakul C, Reddy KR (2014) Transjugular intrahepatic portosystemic shunts in liver transplant recipients. Liver Transpl 20:130–139
Amesur NB, Zajko AB, Orons PD et al (1999) Transjugular intrahepatic portosystemic shunt in patients who have undergone liver transplantation. J Vasc Interv Radiol 5:569–573
Lerut JP, Goffette P, Molle G et al (1999) Transjugular intrahepatic portosystemic shunt after adult liver transplantation: experience in eight patients. Transplantation 68:379–384
Abouljoud M, Yoshida A, Kim D et al (2005) Transjugular intrahepatic portosystemic shunts for refractory ascites after liver transplantation. Transplant Proc 37:1248–1250
Vasta F, Luca A, Miraglia R et al (2005) Transjugular intrahepatic portosystemic shunt in adult liver recipient with delayed graft function. Transplant Proc 37:2626–2628
Finkenstedt A, Graziadei IW, Nachbaur K et al (2009) Transjugular intrahepatic portosystemic shunt in liver transplant recipients. World J Gastroenterol 16:1999–2004
Saad WE, Darwish WM, Davies MG, Waldman DL (2010) Transjugular intrahepatic portosystemic shunts in liver transplant recipients for management of refractory ascites: clinical outcome. J Vasc Interv Radiol 21:218–223
King A, Masterton G, Gunson B et al (2011) A case-controlled study of the safety and efficacy of transjugular intrahepatic portosystemic shunts after liver transplantation. Liver Transplant 17:771–778
Van Ha TG, Funaki BS, Ehrhardt J et al (2005) Transjugular intrahepatic portosystemic shunt placement in liver transplant recipients: experiences with pediatric and adult patients. AJR Am J Roentgenol 184:920–925
Saad WE, Darwish WM, Davies MG et al (2013) Transjugular intrahepatic portosystemic shunts in liver transplant recipients: technical analysis and clinical outcome. AJR Am J Roentgenol 200:210–218
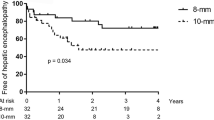
Miraglia R, Maruzzelli L, Tuzzolino F, Petridis I, Luca A (2017) Transjugular intrahepatic portosystemic shunts in patients with cirrhosis with refractory ascites: comparison of clinical outcomes by using 8- and 10-mm PTFE-covered stents. Radiology 284:281–288
Longo JM, Bilbao JI, Rousseau HP et al (1992) Color Doppler-US guidance in transjugular placement of intrahepatic portosystemic shunts. Radiology 184:281–284
Miraglia R, Gerasia R, Maruzzelli L et al (2017) Radiation doses to operators performing transjugular intrahepatic portosystemic shunt using a flat-panel detector-based system and ultrasound guidance for portal vein targeting. Eur Radiol 27:1783–1786
Liang HL, Liu WC, Huang JS et al (2011) TIPS in patients with cranial porta hepatis: ultrasound-guided transhepatic portohepatic-portocaval puncture in single needle pass. AJR Am J Roentgenol 196:914–918
Raza SA, Walser E, Hernandez A et al (2006) Transhepatic puncture of portal and hepatic veins for TIPS using a single-needle pass under sonographic guidance. AJR Am J Roentgenol 87:W87–W91
Chen Y, Ye P, Li Y et al (2015) Percutaneous transhepatic balloon-assisted transjugular intrahepatic portosystemic shunt for chronic, totally occluded, portal vein thrombosis with symptomatic portal hypertension: procedure technique, safety, and clinical applications. Eur Radiol 25:3431–3437
Habib A, Desai K, Hickey R et al (2015) Portal vein recanalization-transjugular intrahepatic portosystemic shunt using the transsplenic approach to achieve transplant candidacy in patients with chronic portal vein thrombosis. J Vasc Interv Radiol 26:499–506
La Mura V, Abraldes JG, Berzigotti A et al (2010) Right atrial pressure is not adequate to calculate portal pressure gradient in cirrhosis: a clinical-hemodynamic correlation study. Hepatology 51:2108–2116
Kliewer MA, Hertzberg BS, Heneghan JP et al (2000) Transjugular intrahepatic portosystemic shunts (TIPS): effects of respiratory state and patient position on the measurement of Doppler velocities. AJR Am J Roentgenol 175:149–152
Dariushnia SR, Haskal ZJ, Midia M et al (2016) Quality improvement guidelines for transjugular intrahepatic portosystemic shunts. J Vasc Interv Radiol 27:1–7
Chen B, Wang W, Tam MD, Quintini C, Fung JJ, Li X (2015) Transjugular intrahepatic portosystemic shunt in liver transplant recipients: indications, feasibility, and outcomes. Hepatol Int 9:391–398
El Atrache M, Abouljoud M, Sharma S et al (2012) Transjugular intrahepatic portosystemic shunt following liver transplantation: can outcomes be predicted? Clin Transplant 26:657–661
Saad W (2014) Transjugular Intrahepatic Portosystemic Shunt before and after Liver Transplantation. Semin Intervent Radiol 31:243–247
Bureau C, Thabut D, Oberti F et al (2017) Transjugular intrahepatic portosystemic shunts with covered stents increase transplant-free survival of patients with cirrhosis and recurrent ascites. Gastroenterology. 152:157–163
García-Pagán JC, Caca K, Bureau C et al (2010) Early use of TIPS in patients with cirrhosis and variceal bleeding. N Engl J Med 362:2370–2379
Bureau C, García-Pagán JC, Layrargues GP et al (2007) Patency of stents covered with polytetrafluoroethylene in patients treated by transjugular intrahepatic portosystemic shunts: long-term results of a randomized multicentre study. Liver Int 27:742–747
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Luigi Maruzzelli.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Fabio Tuzzolino kindly provided statistical advice for this manuscript.
Informed consent
Our retrospective cohort study was reviewed and approved by the institutional research review board, and informed consent form was waived. Informed written consent to the TIPS procedure was obtained from all patients.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Maruzzelli, L., D’Amico, M., Tuzzolino, F. et al. Clinical outcomes of transjugular intrahepatic portosystemic shunt with PTFE-covered stents after liver transplantation and technical results in split and whole liver graft recipients. Eur Radiol 33, 2612–2619 (2023). https://doi.org/10.1007/s00330-022-09259-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09259-4