Abstract
Objectives
To identify magnetic resonance imaging (MRI) features associated with injury type, severity, and liver transplantation (LT)/liver-related death (LRD) in drug-induced liver injury (DILI).
Methods
The eligible DILI patients (2016 to 2020) who underwent contrast abdominal MRI within 3 months of onset were retrospectively analysed at Beijing Friendship Hospital, Capital Medical University. The MRI features independently associated with severity and prognosis were identified by backwards logistic regression. Unadjusted odds ratios (ORs) and 95% confidence intervals (CIs) are given.
Results
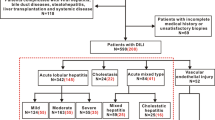
The median age of 180 patients was 55.5 years, with 126 (70.0%) women. The injury types included hepatocellular (135 cases, 75.0%), mixed (23, 12.8%), and cholestatic (22, 12.2%). The proportion of periportal oedema in patients with hepatocellular and mixed injury was significantly higher than that in cholestatic injury (62.2%, 47.8% vs. 18.2%, p < 0.001). For severity, 157 (87.2%) patients had mild to moderate injury, and 23 (12.8%) had severe to fatal/LT. Irregularity of the liver surface (6.56 (95% CI, 1.27–22.84)), transient hepatic attenuation difference (THAD) (3.27 (95% CI, 1.14–9.36)), and splenomegaly (5.86 (95% CI, 1.96–17.53)) were independently associated with severity. Eight (4.4%) patients died/underwent LT. THAD (8.89 (95% CI, 1.35–58.43)), and ascites (64.63 (95% CI, 6.93–602.40)) were independently associated with LT/LRD. The prediction of the new model employing THAD and ascites for LT/LRD within 1 year was 0.959 (95% CI, 0.917–1.000).
Conclusions
Periportal oedema was associated with the type of injury. Irregularity of the liver surface, THAD, and splenomegaly were associated with severity. THAD and ascites may have potential clinical utility in predicting LT/LRD outcomes within 1 year.
Key Points
• Contrast abdominal magnetic resonance imaging features can help clinicians evaluate the type of injury, severity, and poor prognosis of drug-induced liver injury.
• Transient hepatic attenuation difference and ascites have potential clinical utility in the prediction of the poor prognosis of liver transplantation/liver-related death.
• The new model predicting poor prognosis has a relatively high sensitivity of 0.875 and a high specificity of 0.919.





Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- DILI:
-
Drug-induced liver injury
- DWI:
-
Diffusion-weighted imaging
- LRD:
-
Liver-related death
- LT:
-
Liver transplantation
- MRI:
-
Magnetic resonance imaging
- THAD:
-
Transient hepatic attenuation difference
References
Wang W, Lie P, Guo M, He J (2017) Risk of hepatotoxicity in cancer patients treated with immune checkpoint inhibitors: a systematic review and meta-analysis of published data. Int J Cancer 141:1018–1028
Shen T, Liu Y, Shang J et al (2019) Incidence and etiology of drug-induced liver injury in Mainland China. Gastroenterology 156:2230–2241
Ostapowicz G, Fontana R, Schiødt F et al (2002) Results of a prospective study of acute liver failure at 17 tertiary care centers in the United States. Ann Intern Med 137:947–954
Wei G, Bergquist A, Broomé U et al (2007) Acute liver failure in Sweden: etiology and outcome. J Intern Med 262:393–401
Robles-Diaz M, Lucena M, Kaplowitz N et al (2014) Use of Hy’s law and a new composite algorithm to predict acute liver failure in patients with drug-induced liver injury. Gastroenterology 147:109–118.e5
Gasmi B, Kleiner D (2020) Liver histology: diagnostic and prognostic features. Clin Liver Dis 24:61–74
Tian Q, Zhao X, Wang Y et al (2019) Histologic pattern is better correlated with clinical outcomes than biochemical classification in patients with drug-induced liver injury. Mod Pathol 32:1795–1805
Sanai F, Keeffe E (2010) Liver biopsy for histological assessment: the case against. J Gastroenterol 16:124–132
Shu J, Zhao J, Han F, Tang G, Chen X (2017) Chronic hepatitis B: correlation of abnormal features on T2-weighted imaging and dynamic contrast-enhanced imaging with hepatic histopathology. Radiol Med 122:807–813
Ren H, Ye H, An W, Dong J, Liu Y (2017) Study of diffusion weighted imaging in combination with conventional MRI signs for inflammation activity of chronic hepatitis B. Zhonghua Yi Xue Za Zhi 97:1484–1490
Shu J, Zhao J, Han F et al (2013) Oedema of gallbladder wall: correlation with chronic hepatitis B on MR imaging. Radiol Med 118:1102–1108
Chen D, Zhao X, Xu H et al (2022) Noninvasive assessment of APAP (N-acetyl-p-aminophenol)-induced hepatotoxicity using multiple MRI parameters in an experimental rat model. J Magn Reson Imaging. https://doi.org/10.1002/jmri.28203
Gudnason HO, Björnsson HK, Gardarsdottir M et al (2015) Secondary sclerosing cholangitis in patients with drug-induced liver injury. Dig Liver Dis 47:502–507
Fontana R, Seeff L, Andrade R et al (2010) Standardization of nomenclature and causality assessment in drug-induced liver injury: summary of a clinical research workshop. Hepatology 52:730–742
Bénichou C (1990) Criteria of drug-induced liver disorders. Report of an international consensus meeting. J Hepatol 11:272–276
Aithal G, Watkins P, Andrade R et al (2011) Case definition and phenotype standardization in drug-induced liver injury. Clin Pharmacol Ther 89:806–815
Medina-Caliz I, Robles-Diaz M, Garcia-Muñoz B et al (2016) Definition and risk factors for chronicity following acute idiosyncratic drug-induced liver injury. J Hepatol 65:532–542
Colagrande S, Centi N, La Villa G, Villari N (2004) Transient hepatic attenuation differences. AJR Am J Roentgenol 183:459–464
Runner G, Corwin M, Siewert B, Eisenberg R (2014) Gallbladder wall thickening. AJR Am J Roentgenol 202:W1–W12
Barakat F, Kaisers U, Busch T et al (2009) Periportal oedema of the liver: correlation with clinical and paraclinical parameters in polytraumatic patients. Clin Imaging 33:39–43
Hikita H, Nakagawa H, Tateishi R et al (2013) Perihepatic lymph node enlargement is a negative predictor of liver cancer development in chronic hepatitis C patients. J Gastroenterol 48:366–373
Yang D, Zhang J, Han D, Jin E, Yang Z (2017) The role of apparent diffusion coefficient values in characterization of solid focal liver lesions: a prospective and comparative clinical study. Sci China Life Sci 60:16–22
Kleiner D, Chalasani N, Lee W et al (2014) Hepatic histological findings in suspected drug-induced liver injury: systematic evaluation and clinical associations. Hepatology 59:661–670
Ishak K, Baptista A, Bianchi L et al (1995) Histological grading and staging of chronic hepatitis. J Hepatol 22:696–699
Cannella R, Sartoris R, Grégory J et al (2021) Quantitative magnetic resonance imaging for focal liver lesions: bridging the gap between research and clinical practice. Br J Radiol 94:20210220
Katabathina V, Dasyam A, Dasyam N, Hosseinzadeh K (2014) Adult bile duct strictures: role of MR imaging and MR cholangiopancreatography in characterization. Radiographics 34:565–586
Vernuccio F, Dioguardi Burgio M, Barbiera F et al (2019) CT and MR imaging of chemotherapy-induced hepatopathy. Abdom Radiol (NY) 44:3312–3324
Andrade R, Lucena M, Kaplowitz N et al (2006) Outcome of acute idiosyncratic drug-induced liver injury: long-term follow-up in a hepatotoxicity registry. Hepatology 44:1581–1588
Fontana R, Watkins P, Bonkovsky H et al (2009) Drug-Induced Liver Injury Network (DILIN) prospective study: rationale, design and conduct. Drug Saf 32:55–68
Siegel M, Herman T (1992) Periportal low attenuation at CT in childhood. Radiology 183:685–688
Grudzinski IP, Ruzycka M, Cieszanowski A et al (2019) MRI-based preclinical discovery of DILI: a lesson from paracetamol-induced hepatotoxicity. Regul Toxicol Pharmacol 108:104478
Ferin P, Lerner R (1985) Contracted gallbladder: a finding in hepatic dysfunction. Radiology 154:769–770
Jüttner H, Ralls P, Quinn M, Jenney J (1982) Thickening of the gallbladder wall in acute hepatitis: ultrasound demonstration. Radiology 142:465–466
Kim A, Han S, Tran D et al (2013) Abdominal imaging can misdiagnose submassive hepatic necrosis as cirrhosis in acute liver failure. Clin Transpl 27:E339–E345
Mckenzie C, Colonne C, Yeo J, Fraser S (2018) Splenomegaly: Pathophysiological bases and therapeutic options. Int J Biochem Cell Biol 94:40–43
Walsh K, Leen E, Macsween R, Morris A (1998) Hepatic blood flow changes in chronic hepatitis C measured by duplex Doppler color sonography: relationship to histological features. Dig Dis Sci 43:2584–2590
Chundru S, Kalb B, Arif-Tiwari H et al (2014) MRI of diffuse liver disease: characteristics of acute and chronic diseases. Diagn Interv Radiol 20:200–208
Devarbhavi H, Joseph T, Sunil Kumar N et al (2021) The Indian network of drug-induced liver injury: etiology, clinical features, outcome and prognostic markers in 1288 patients. J Clin Exp Hepatol 11:288–298
Romero M, Palmer S, Kahn J et al (2014) Imaging appearance in acute liver failure: correlation with clinical and pathology findings. Dig Dis Sci 59:1987–1995
Landis J, Koch G (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Funding
This study has received funding from the National Natural Science Foundation of China. (No. 81900526; 82103902; 82071876).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Xinyan Zhao.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Min Li (Beijing, China) has kindly provided statistical advice for this manuscript.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(PDF 240 kb)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, T., Yang, D., Wee, A. et al. Identification of MRI features associated with injury type, severity, and prognosis in drug-induced liver injury. Eur Radiol 33, 666–677 (2023). https://doi.org/10.1007/s00330-022-09041-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09041-6