Abstract
Objectives
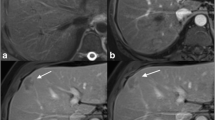
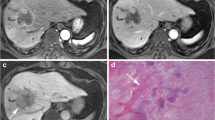
To review the gadoxetic acid disodium (EOB)-enhanced magnetic resonance (MR) imaging features of cholangiolocellular carcinoma (CoCC) of the liver and compare them with those of hepatocellular carcinoma (HCC) and intrahepatic cholangiocarcinoma (ICC).
Methods
EOB-enhanced MR images of 19 patients with CoCC, 23 with ICC, and 51 with HCC were retrospectively evaluated qualitatively and quantitatively. Univariate and multivariate analyses were performed to determine the characteristic MR features of CoCC with histopathological–imaging correlation.
Results
Multivariate logistic regression analysis showed that dot-/band-shaped internal enhancement during the arterial and portal phases (P < 0.001), and larger arterial ring enhancement ratio (CoCC, 0.13 ± 0.04; ICC, 0.074 ± 0.04; P = 0.013) were significantly independently associated with CoCC in contrast to ICC, whereas several MR features including progressive enhancement during the portal and late phases (P < 0.001), target appearance in the hepatocyte phase (P = 0.004), and vessel penetration (P = 0.013) were significantly more frequently associated with CoCC than HCC. The dot-/band-like internal enhancement (78.9% of CoCCs) histopathologically corresponded to the tumour cell nest with vascular proliferations and retained Glisson's sheath structure.
Conclusions
EOB-enhanced MR features of CoCC largely differ from those of HCC but are similar to those of ICC. However, the finding of thicker arterial ring enhancement with dot-/band-like internal enhancement could help differentiate CoCC from ICC.
Key Points
• Gadoxetic acid-enhanced MR features of cholangiolocellular carcinoma (CoCC) resembled those of intrahepatic cholangiocarcinoma (ICC).
• Gadoxetic acid-enhanced MR features of CoCC largely differed from those of hepatocellular carcinoma.
• Dot-/band-like internal enhancement of CoCC may be helpful for differentiating from ICC.
• Arterial ring enhancement of CoCC was larger than that of ICC.





Similar content being viewed by others
Abbreviations
- cHCC-CC:
-
Combined hepatocellular and cholangiocarcinoma
- CoCC:
-
Cholangiolocellular carcinoma
- DW:
-
Diffusion-weighted
- EOB:
-
Gadoxetic acid disodium
- HCC:
-
Hepatocellular carcinoma
- HE:
-
Hematoxylin and eosin
- ICC:
-
Intrahepatic cholangiocarcinoma
- LLC:
-
Lesion-to-liver contrast
- ROI:
-
Region of interest
- SI:
-
Signal intensity
- WHO:
-
World Health Organization
References
Steiner PE, Higginson J (1959) Cholangiolocellular carcinoma of the liver. Cancer 12(4):753–759
Komuta M, Spee B, Vander Borght S et al (2008) Clinicopathological study on cholangiolocellular carcinoma suggesting hepatic progenitor cell origin. Hepatology 47(5):1544–1556
World Health Organization (2010) Classification of tumours of the digestive system, 4th edn. International Agency for Research on Cancer, Lyon
Ariizumi S, Kotera Y, Katagiri S et al (2014) Long-term survival of patients with cholangiolocellular carcinoma after curative hepatectomy. Ann Surg Oncol 21(Suppl 3):S451–S458
Ahn SS, Kim MJ, Lim JS, Hong HS, Chung YE, Choi JY (2010) Added value of gadoxetic acid-enhanced hepatobiliary phase MR imaging in the diagnosis of hepatocellular carcinoma. Radiology 255(2):459–466
Haradome H, Grazioli L, Tinti R et al (2011) Additional value of gadoxetic acid-DTPA-enhanced hepatobiliary phase MR imaging in the diagnosis of early-stage hepatocellular carcinoma: comparison with dynamic triple-phase multidetector CT imaging. J Magn Reson Imaging 34(1):69–78
Zech CJ, Grazioli L, Breuer J, Reiser MF, Schoenberg SO (2008) Diagnostic performance and description of morphological features of focal nodular hyperplasia in Gd-EOB-DTPA-enhanced liver magnetic resonance imaging: results of a multicenter trial. Invest Radiol 43(7):504–511
Grazioli L, Bondioni MP, Haradome H et al (2012) Hepatocellular adenoma and focal nodular hyperplasia: value of gadoxetic acid-enhanced MR imaging in differential diagnosis. Radiology 262(2):520–529
McInnes MD, Hibbert RM, Inácio JR, Schieda N (2015) Focal nodular hyperplasia and hepatocellular adenoma: accuracy of gadoxetic acid-enhanced MR imaging – a systematic review. Radiology 277(2):413–423
Palmucci S (2014) Focal liver lesions detection and characterization: the advantages of gadoxetic acid-enhanced liver MRI. World J Hepatol 6(7):477–485
Merkle EM, Zech CJ, Bartolozzi C et al (2016) Consensus report from the 7th international forum for liver magnetic resonance imaging. Eur Radiol 26(3):674–682
Neri E, Bali MA, Ba-Ssalamah A et al (2016) ESGAR consensus statement on liver MR imaging and clinical use of liver-specific contrast agents. Eur Radiol 26(4):921–931
Motosugi U, Ichikawa T, Nakajima H et al (2009) Cholangiolocellular carcinoma of the liver: imaging findings. J Comput Assist Tomogr 33(5):682–688
Kadono M, Kimura K, Imamura J et al (2011) A case of a large cholangiolocellular carcinoma. Clin J Gastroenterol 4(5):340–346
Haradome H, Grazioli L, Tsunoo M et al (2010) Can MR fluoroscopic triggering technique and slow rate injection provide appropriate arterial phase images with reducing artifacts on gadoxetic acid-DTPA (Gd-EOB-DTPA)-enhanced hepatic MR imaging? J Magn Reson Imaging 32(2):334–340
Granata V, Catalano O, Fusco R et al (2015) The target sign in colorectal liver metastases: an atypical Gd-EOB-DTPA "uptake" on the hepatobiliary phase of MR imaging. Abdom Imaging 40(7):2364–2371
Fukukura Y, Hamanoue M, Fujiyoshi F et al (2000) Cholangiolocellular carcinoma of the liver: CT and MR findings. J Comput Assist Tomogr 24(5):809–812
Asayama Y, Tajima T, Okamoto D et al (2010) Imaging of cholangiolocellular carcinoma of the liver. Eur J Radiol 75(1):e120–e125
Koh J, Chung YE, Nahm JH et al (2016) Intrahepatic mass-forming cholangiocarcinoma: prognostic value of preoperative gadoxetic acid-enhanced MRI. Eur Radiol 26(2):407–416
Kang Y, Lee JM, Kim SH, Han JK, Choi BI (2012) Intrahepatic mass-forming cholangiocarcinoma: enhancement patterns on gadoxetic acid-enhanced MR images. Radiology 264(3):751–760
Jeong HT, Kim MJ, Chung YE, Choi JY, Park YN, Kim KW (2013) Gadoxetate disodium-enhanced MRI of mass-forming intrahepatic cholangiocarcinomas: imaging-histologic correlation. AJR Am J Roentgenol 201(4):W603–W611
Kim SH, Lee CH, Kim BH et al (2012) Typical and atypical imaging findings of intrahepatic cholangiocarcinoma using gadolinium ethoxybenzyl diethylenetriamine pentaacetic acid-enhanced magnetic resonance imaging. J Comput Assist Tomogr 36(6):704–709
Ha S, Lee CH, Kim BH et al (2012) Paradoxical uptake of Gd-EOB-DTPA on the hepatobiliary phase in the evaluation of hepatic metastasis from breast cancer: is the "target sign" a common finding? Magn Reson Imaging 30(8):1083–1090
Park MJ, Kim YK, Park HJ, Hwang J, Lee WJ (2013) Scirrhous hepatocellular carcinoma on gadoxetic acid-enhanced magnetic resonance imaging and diffusion-weighted imaging: emphasis on the differentiation of intrahepatic cholangiocarcinoma. J Comput Assist Tomogr 37(6):872–881
Acknowledgements
We are grateful to Kazuhito Nakayasu (Kondo Photo Process Co., Ltd.) for providing professional statistical advice.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Tadatoshi Takayama
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Funding
The authors state that this work has not received any funding.
Statistics and biometry
Kazuhito Nakayasu (Kondo Photo Process Co., Ltd.) kindly provided statistical advice.
Ethical approval
Institutional Review Board approval was obtained.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Methodology
• Retrospective
• Case-control/observational study
• Multicenter study
Rights and permissions
About this article
Cite this article
Haradome, H., Unno, T., Morisaka, H. et al. Gadoxetic acid disodium-enhanced MR imaging of cholangiolocellular carcinoma of the liver: imaging characteristics and histopathological correlations. Eur Radiol 27, 4461–4471 (2017). https://doi.org/10.1007/s00330-017-4811-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-4811-2