Abstract
Purpose
To intra-individually compare the diagnostic image quality of Dixon and spectral fat suppression at 3 T.
Methods
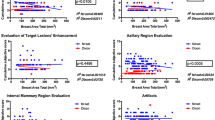
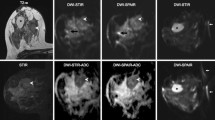
Fifty consecutive patients (mean age 55.1 years) undergoing 3 T breast MRI were recruited for this prospective study. The image protocol included pre-contrast and delayed post-contrast spectral and Dixon fat-suppressed T1w series. Two independent blinded readers compared spectral and Dixon fat-suppressed series by evaluating six ordinal (1 worst to 5 best) image quality criteria (image quality, delineation of anatomical structures, fat suppression in the breast and axilla, lesion delineation and internal enhancement). Breast density and size were assessed. Data analysis included Spearman’s rank correlation coefficient and visual grading characteristics (VGC) analysis.
Results
Four examinations were excluded; 48 examinations in 46 patients were evaluated. In VGC analysis, the Dixon technique was superior regarding image quality criteria analysed (P < 0.01). Smaller breast size and lower breast density were significantly (P < 0.01) correlated with impaired spectral fat suppression quality. No such correlation was identified for the Dixon technique, which showed reconstruction-based water-fat mixups leading to insufficient image quality in 20.8 %.
Conclusions
The Dixon technique outperformed spectral fat suppression in all evaluated criteria (P < 0.01). Non-diagnostic examinations can be avoided by fat and water image reconstruction. The superior image quality of the Dixon technique can improve breast MRI interpretation.
Key Points
• Optimal fat suppression quality is necessary for optimal image interpretation
• Superior fat suppression quality is achieved using the Dixon technique
• Lesion margin and internal enhancement evaluation improves using the Dixon technique
• Superior image quality of the Dixon technique improves breast MRI interpretation





Similar content being viewed by others
References
Houssami N, Ciatto S, Macaskill P, Lord SJ, Warren RM, Dixon JM, Irwig L (2008) Accuracy and surgical impact of magnetic resonance imaging in breast cancer staging: systematic review and meta-analysis in detection of multifocal and multicentric cancer. J Clin Oncol Off J Am Soc Clin Oncol 26(19):3248–3258
Kuhl CK, Schrading S, Bieling HB, Wardelmann E, Leutner CC, Koenig R, Kuhn W, Schild HH (2007) MRI for diagnosis of pure ductal carcinoma in situ: a prospective observational study. Lancet 370(9586):485–492
Warner E, Messersmith H, Causer P, Eisen A, Shumak R, Plewes D (2008) Systematic review: using magnetic resonance imaging to screen women at high risk for breast cancer. Ann Intern Med 148(9):671–679
Benndorf M, Baltzer PAT, Vag T, Gajda M, Runnebaum IB, Kaiser WA (2010) Breast MRI as an adjunct to mammography: Does it really suffer from low specificity? A retrospective analysis stratified by mammographic BI-RADS classes. Acta Radiol 51(7):715–721
Pinker-Domenig K, Bogner W, Gruber S, Bickel H, Duffy S, Schernthaner M, Dubsky P, Pluschnig U, Rudas M et al (2012) High resolution MRI of the breast at 3 T: which BI-RADS® descriptors are most strongly associated with the diagnosis of breast cancer? Eur Radiol 22(2):322–330
Mann RM, Kuhl CK, Kinkel K, Boetes C (2008) Breast MRI: guidelines from the European Society of Breast Imaging. Eur Radiol 18(7):1307–1318
Kuhl C (2007) The current status of breast MR imaging. Part I. Choice of technique, image interpretation, diagnostic accuracy, and transfer to clinical practice. Radiology 244(2):356–378
Sardanelli F, Boetes C, Borisch B, Decker T, Federico M, Gilbert FJ, Helbich T, Heywang-Köbrunner SH, Kaiser WA, et al (2010) Magnetic resonance imaging of the breast: recommendations from the EUSOMA working group. Eur J Cancer 46(8):1296–1316
Pinker K, Grabner G, Bogner W, Gruber S, Szomolanyi P, Trattnig S, Heinz-Peer G, Weber M, Fitzal F et al (2009) A combined high temporal and high spatial resolution 3 Tesla MR imaging protocol for the assessment of breast lesions: initial results. Investig Radiol 44(9):553–558
Pinker K, Bogner W, Baltzer P, Trattnig S, Gruber S, Abeyakoon O, Bernathova M, Zaric O, Dubsky P, et al (2014) Clinical application of bilateral high temporal and spatial resolution dynamic contrast-enhanced magnetic resonance imaging of the breast at 7 T. Eur Radiol 24(4):913-20
Kuhl CK (2007) Breast MR imaging at 3 T. Magn Reson Imaging Clin N Am 15(3):315–320, vi
Ma J (2008) Dixon techniques for water and fat imaging. J Magn Reson Imaging JMRI 28(3):543–558
Dixon WT (1984) Simple proton spectroscopic imaging. Radiology 153(1):189–194
Le-Petross H, Kundra V, Szklaruk J, Wei W, Hortobagyi GN, Ma J (2010) Fast three-dimensional dual echo dixon technique improves fat suppression in breast MRI. J Magn Reson Imaging JMRI 31(4):889–894
Dogan BE, Ma J, Hwang K, Liu P, Yang WT (2011) T1-weighted 3D dynamic contrast-enhanced MRI of the breast using a dual-echo Dixon technique at 3 T. J Magn Reson Imaging JMRI 34(4):842–851
Båth M, Månsson LG (2007) Visual grading characteristics (VGC) analysis: a non-parametric rank-invariant statistical method for image quality evaluation. Br J Radiol 80(951):169–176
Wokke BH, Bos C, Reijnierse M, van Rijswijk CS, Eggers H, Webb A, Verschuuren JJ, Kan HE (2013) Comparison of dixon and T1-weighted MR methods to assess the degree of fat infiltration in Duchenne muscular dystrophy patients. J Magn Reson Imaging JMRI 38(3):619–624
Kim HK, Lindquist DM, Serai SD, Mariappan YK, Wang LL, Merrow AC, McGee KP, Ehman RL, Laor T (2013) Magnetic resonance imaging of pediatric muscular disorders: recent advances and clinical applications. Radiol Clin N Am 51(4):721–742
Rosenkrantz AB, Mannelli L, Kim S, Babb JS (2011) Gadolinium-enhanced liver magnetic resonance imaging using a 2-point Dixon fat-water separation technique: impact upon image quality and lesion detection. J Comput Assist Tomogr 35(1):96–101
Costelloe CM, Kundra V, Ma J, Chasen BA, Rohren EM, Bassett RL Jr, Madewell JE (2012) Fast Dixon whole-body MRI for detecting distant cancer metastasis: a preliminary clinical study. J Magn Reson Imaging JMRI 35(2):399–408
Barger AV, DeLone DR, Bernstein MA, Welker KM (2006) Fat signal suppression in head and neck imaging using fast spin-echo-IDEAL technique. Am J Neuroradiol 27(6):1292–1294
Acknowledgments
The scientific guarantor of this publication is Pascal A.T. Baltzer. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. One of the authors has significant statistical expertise. Institutional Review Board approval was obtained. Written informed consent was obtained from all subjects (patients) in this study. Methodology: prospective, observational, performed at one institution
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Clauser, P., Pinker, K., Helbich, T.H. et al. Fat saturation in dynamic breast MRI at 3 Tesla: is the Dixon technique superior to spectral fat saturation? A visual grading characteristics study. Eur Radiol 24, 2213–2219 (2014). https://doi.org/10.1007/s00330-014-3189-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3189-7