Abstract
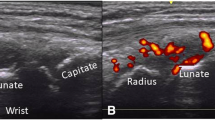
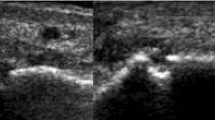
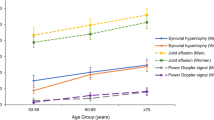
To evaluate the prevalence of musculoskeletal ultrasonography (MSUS) abnormalities in asymptomatic elderly individuals. A cross-sectional controlled study was conducted and MSUS of 23 joints (wrist, metacarpophalangeal-MCP, proximal interphalangeal-PIP, elbow, glenohumeral, hip, knee, ankle, and metatarsophalangeal-MTP joints) was performed in healthy individuals aged 18–29 (young, n = 32) and 60–80 years-old (elderly, n = 32). Quantitative synovial hypertrophy (SH) was measured in mm and a semiquantitative scoring system (0–3) was used to grade SH, power doppler (PD) and bone erosion (BE). Young and elderly participants were 26.2 ± 3.2 and 65.9 ± 4.4 years-old, respectively. As compared to the young participants, elderly individuals had higher SH values in 35% of the joint surfaces (P < 0.05), higher rates of scores 1–3 for SH at the dorsal surface of the 3rd MCP, palmar surface of the 2nd MCP, 2nd PIP, 3rd MCP and 3rd PIP and subtalar joints (17.2 vs. 1.6%, P = 0.002; 29.7 vs. 6.3%, P = 0.001; 12.5 vs. 1.6%, P = 0.016; 21.9 vs. 6.3%, P = 0.011; 21.9 vs. 7.8%, P = 0.025; and 24.2 vs. 6.3%, P = 0.005, respectively), BE at the radiocarpal, ulnocarpal, dorsal surface of the 2nd MCP and posterior area of the glenohumeral joints (10.9 vs. 1.6%, P = 0.028; 12.5 vs. 0%, P = 0.003; 9.4 vs. 0%, P = 0.012; and 29.7 vs. 10.9%, P = 0.008, respectively) and PD at the dorsal surface of the 2nd and 3rd MCP joints (9.4 vs. 0%; P = 0.012 and 7.8 vs. 0%; P = 0.023, respectively). BE scores ≥ 1 were more frequent in the elderly (P < 0.05) in 22 (88%) of the joint surfaces evaluated. MSUS abnormalities are more frequent in asymptomatic elderly individuals as compared to young subjects.

Similar content being viewed by others
Data availability
The data sets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Grassi W (2003) Clinical evaluation versus ultrasonography: who is the winner? J Rheumatol 30(5):908–909
Kane D, Balint PV, Sturrock RD (2003) Ultrasonography is superior to clinical examination in the detection and localization of knee joint effusion in rheumatoid arthritis. J Rheumatol 30(5):966–971
McAlindon T, Kissin E, Nazarian L, Ranganath V, Prakash S, Taylor M, Bannuru RR, Srinivasan S, Gogia M, McMahon MA, Grossman J, Kafaja S, FitzGerald J (2012) American college of rheumatology report on reasonable use of musculoskeletal ultrasonography in rheumatology clinical practice. Arthritis Care Res (Hoboken) 64(11):1625–1640. https://doi.org/10.1002/acr.21836
Möller I, Janta I, Backhaus M, Ohrndorf S, Bong DA, Martinoli C, Filippucci E, Sconfienza LM, Terslev L, Damjanov N, Hammer HB, Sudol-Szopinska I, Grassi W, Balint P, Bruyn GAW, D’Agostino MA, Hollander D, Siddle HJ, Supp G, Schmidt WA, Iagnocco A, Koski J, Kane D, Fodor D, Bruns A, Mandl P, Kaeley GS, Micu M, Ho C, Vlad V, Chávez-López M, Filippou G, Cerón CE, Nestorova R, Quintero M, Wakefield R, Carmona L, Naredo E (2017) The 2017 EULAR standardised procedures for ultrasound imaging in rheumatology. Ann Rheum Dis 76(12):1974–1979. https://doi.org/10.1136/annrheumdis-2017-211585
Frontera WR (2017) Physiologic changes of the musculoskeletal system with aging: a brief review. Phys Med Rehabil Clin N Am 28(4):705–711. https://doi.org/10.1016/j.pmr.2017.06.004
Makris UE, Misra D, Yung R (2017) Gaps in Aging Research as it Applies to Rheumatologic Clinical Care. Clin Geriatr Med 33(1):119–133. https://doi.org/10.1016/j.cger.2016.08.009
Schmidt WA, Schmidt H, Schicke B, Gromnica-Ihle E (2004) Standard reference values for musculoskeletal ultrasonography. Ann Rheum Dis 63(8):988–994. https://doi.org/10.1016/j.cger.2016.08.00936/ard.2003.015081 (10.11 ch as it Applies to Rheumatologic Clinical Care. Clin Geriatr Med 33(1):119-133)
Kim HS, Kim HR, Kim BY, Kim YS, Jung YO, Choi SJ, Kim HO, Hwang J, Lee S, Kim HA, Bang SY, Chai JY, Park SH, Yoon CH (2019) Standardized, musculoskeletal ultrasonographic reference values for healthy Korean adults. Korean J Intern Med 34(6):1372–1380. https://doi.org/10.3904/kjim.2016.397
Ellegaard K, Torp-Pedersen S, Holm CC, Danneskiold-Samsøe B, Bliddal H (2007) Ultrasound in finger joints: findings in normal subjects and pitfalls in the diagnosis of synovial disease. Ultraschall Med 28(4):401–408. https://doi.org/10.1055/s-2007-963170
Padovano I, Costantino F, Breban M, D’Agostino MA (2016) Prevalence of ultrasound synovial inflammatory findings in healthy subjects. Ann Rheum Dis 75(10):1819–1823. https://doi.org/10.1136/annrheumdis-2015-208103
Wang L, Xiang X, Tang Y, Yang Y, Qiu L (2018) Sonographic appearance of fluid in peripheral joints and bursae of healthy asymptomatic Chinese population. Quant Imaging Med Surg 8(8):781–787. https://doi.org/10.21037/qims.2018.09.10
Machado FS, Natour J, Takahashi RD, de Buosi AL, Furtado RN (2014) Sonographic assessment of healthy peripheral joints: evaluation according to demographic parameters. J Ultrasound Med 33(12):2087–2098. https://doi.org/10.7863/ultra.33.12.2087
Backhaus M, Burmester GR, Gerber T, Grassi W, Machold KP, Swen WA, Wakefield RJ, Manger B (2001) Guidelines for musculoskeletal ultrasound in rheumatology. Ann Rheum Dis 60(7):641–649. https://doi.org/10.1136/ard.60.7.641
Wakefield RJ, Balint PV, Szkudlarek M, Filippucci E, Backhaus M, D’Agostino MA, Sanchez EN, Iagnocco A, Schmidt WA, Bruyn GA, Kane D, O’Connor PJ, Manger B, Joshua F, Koski J, Grassi W, Lassere MN, Swen N, Kainberger F, Klauser A, Ostergaard M, Brown AK, Machold KP, Conaghan PG (2005) Musculoskeletal ultrasound including definitions for ultrasonographic pathology. J Rheumatol 32(12):2485–2487
Szkudlarek M, Court-Payen M, Jacobsen S, Klarlund M, Thomsen HS, Østergaard M (2003) Interobserver agreement in ultrasonography of the finger and toe joints in rheumatoid arthritis. Arthritis Rheum 48(4):955–962. https://doi.org/10.1002/art.10877
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33(1):159–174
Terslev L, Torp-Pedersen S, Savnik A, von der Recke P, Qvistgaard E, Danneskiold-Samsoe B, Bliddal H (2003) Doppler ultrasound and magnetic resonance imaging of synovial inflammation of the hand in rheumatoid arthritis: a comparative study. Arthritis Rheum 48(9):2434–2441. https://doi.org/10.1002/art.11245
Millot F, Clavel G, Etchepare F, Gandjbakhch F, Grados F, Saraux A, Rat AC, Fautrel B, Bourgeois P, Fardellone P, IotFEAC ESPOIR (2011) Musculoskeletal ultrasonography in healthy subjects and ultrasound criteria for early arthritis (the ESPOIR cohort). J Rheumatol 38(4):613–620. https://doi.org/10.3899/jrheum.100379
Witt M, Mueller F, Nigg A, Reindl C, Leipe J, Proft F, Stein N, Hammitzsch A, Mayer S, Dechant C, Schulze-Koops H, Grunke M (2013) Relevance of grade 1 gray-scale ultrasound findings in wrists and small joints to the assessment of subclinical synovitis in rheumatoid arthritis. Arthritis Rheum 65(7):1694–1701. https://doi.org/10.1002/art.37954
Kitchen J, Kane D (2015) Greyscale and power doppler ultrasonographic evaluation of normal synovial joints: correlation with pro—and anti-inflammatory cytokines and angiogenic factors. Rheumatology (Oxford) 54(3):458–462. https://doi.org/10.1093/rheumatology/keu354
Terslev L, Torp-Pedersen S, Qvistgaard E, von der Recke P, Bliddal H (2004) Doppler ultrasound findings in healthy wrists and finger joints. Ann Rheum Dis 63(6):644–648. https://doi.org/10.1136/ard.2003.009548
Iagnocco A, Filippucci E, Sakellariou G, Ceccarelli F, Di Geso L, Carli L, Riente L, Delle Sedie A, Valesini G (2013) Ultrasound imaging for the rheumatologist XLIV. ultrasound of the shoulder in healthy individuals. Clin Exp Rheumatol 31(2):165–171
Iagnocco A, Naredo E, Wakefield R, Bruyn GA, Collado P, Jousse-Joulin S, Finzel S, Ohrndorf S, Delle Sedie A, Backhaus M, Berner-Hammer H, Gandjbakhch F, Kaeley G, Loeuille D, Moller I, Terslev L, Aegerter P, Aydin S, Balint PV, Filippucci E, Mandl P, Pineda C, Roth J, Magni-Manzoni S, Tzaribachev N, Schmidt WA, Conaghan PG, D’Agostino MA (2014) Responsiveness in rheumatoid arthritis. a report from the OMERACT 11 ultrasound workshop. J Rheumatol 41(2):379–382. https://doi.org/10.3899/jrheum.131084
Author information
Authors and Affiliations
Contributions
All authors had substantial contribution to the acquisition and analysis of the data presented in this article. All authors revised and agreed on the final version of the work to be published. All authors take full responsibility regarding all aspects of this work. Any questions that may be raised in the future concerning the integrity or this article will be evaluated and properly investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the EPM/UNIFESP’s Ethics Committee (Protocol number 0992/2017; Certificate of Ethical Appreciation Number: 73701617.4.0000.5505).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Matos, A.L., Natour, J., Heldan de Moura Castro, C. et al. Higher rates of ultrasound synovial hypertrophy, bone erosion and power doppler signal in asymptomatic Brazilian elderly versus young adults: a cross-sectional study. Rheumatol Int 43, 941–951 (2023). https://doi.org/10.1007/s00296-022-05212-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-022-05212-2