Abstract
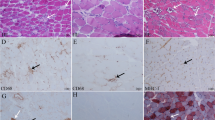
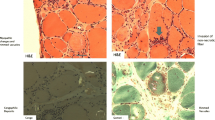
Polymyositis with mitochondrial pathology (PM-Mito) is a rare form of idiopathic inflammatory myopathy with no definite diagnostic criteria and similarities to both PM and sporadic inclusion body myositis (s-IBM). The aim of this study is to address the dilemma of whether PM-Mito is a subtype of inflammatory myopathy or represents a disease falling into the spectrum of s-IBM. Herein, we report four female patients diagnosed with PM-Mito, highlighting their rather atypical clinical and histopathological characteristics that seem to indicate a diagnosis away from s-IBM. Muscle weakness was rather proximal and symmetrical and lacked the selective pattern observed in s-IBM. Patients had large-scale deletions in mtDNA, reflecting the mitochondrial component in the pathology of the disease. Conclusively, our study adds to the limited data in the literature on whether PM-Mito is a distinct form of myositis or represents a prodromal stage of s-IBM. Although the latter seems to be supported by a substantial body of evidence, there are, however, important differences, such as the different patterns of muscle weakness, and the good response to treatment observed in some patients. Larger-scale studies are certainly needed to clarify pathogenesis and clinical characteristics of PM-Mito patients, especially in therapeutic and prognostic terms.


Similar content being viewed by others
References
Amato AA, Greenberg SA (2013) Inflammatory myopathies. Continuum (Minneap Minn) 19(6 Muscle Disease):1615–1633
Lundberg IE, de Visser Μ, Werth VP (2018) Classification of myositis. Nat Rev Rheumatol 14(5):269–278
Blume G, Pestronk A, Frank B, Johns DR (1997) Polymyositis with cytochrome oxidase negative muscle fibers. Early quadriceps weakness and poor response to immunosuppressive therapy. Brain J Neurol 120(1):39–45
Rygiel KA, Miller J, Grady JP, Rocha MC, Taylor RW, Turnbull DM (2015) Mitochondrial and inflammatory changes in sporadic inclusion body myositis. Neuropathol Appl Neurobiol 41:288–303
Oldfors A, Moslemi AR, Jonasson L, Ohlsson M, Kollberg G, Lindberg C (2006) Mitochondrial abnormalities in inclusion-body myositis. Neurology 66(1 suppl 1):S49–S55
Chariot P, Ruet E, Authier FJ, Labes D, Poron F, Gherardi R (1996) Cytochrome c oxidase deficiencies in the muscle of patients with inflammatory myopathies. Acta Neuropathol 91(5):530–536
Varadhachary AS, Weihl CC, Pestronk A (2010) Mitochondrial pathology in immune and inflammatory myopathies. Curr Opin Rheumatol 22(6):651–657
Siepmann T, Tesch M, Krause F, Illigens BMW, Stoltenburg Didinger G (2013) Polymyositis with cytochrome C oxidase negative fibers—a pathological and clinical challenge. Ann Diagn Pathol 17(2):183–186
Temiz P, Weihl CC, Pestronk A (2009) Inflammatory myopathies with mitochondrial pathology and protein aggregates. J Neurol Sci 278(1–2):25–29
Hiniker A, Daniels BH, Lee HS, Margeta M (2013) Comparative utility of LC3, p62 and TDP-43 immunohistochemistry in differentiation of inclusion body myositis from polymyositis and related inflammatory myopathies. Acta Neuropathol Commun 1(1):29
Miller S, Dykes D, Polesky HA (1988) simple salting out procedure for extracting DNA from human nucleated cells. Nucleic Acids Res 16(3):1215
Florence JM, Pandya S, King WM, Robison JD, Baty J, Miller JP, Signore LC (1992) Intrarater reliability of manual muscle test (Medical Research Council scale) grades in Duchenne’s muscular dystrophy. Phys Ther 72(2):115–122
Lindgren U, Roos S, Hedberg Oldfors C, Moslemi AR, Lindberg C, Oldfors Α (2015) Mitochondrial pathology in inclusion body myositis. Neuromuscul Disord 25(4):281–288
Greenberg SA (2016) Inclusion body myositis. Continuum (Minneap Minn) 22(6, Muscle and Neuromuscular Junction Disorders):1871–1888
Simon JP, Marie I, Jouen F, Boyer O, Martinet J (2016) Autoimmune myopathies: where do we stand? Front Immunol 7:234
Gallay L, Petiot P (2016) Sporadic inclusion-body myositis: recent advances and the state of the art in 2016. Rev Neurol (Paris) 172(10):581–586
Mastaglia FL, Needham M (2015) Inclusion body myositis: a review of clinical and genetic aspects, diagnostic criteria and therapeutic approaches. J Clin Neurosci 22(1):6–13
Oh TH, Brumfield KA, Hoskin TL, Stolp KA, Murray JA, Bassford JR (2007) Dysphagia in inflammatory myopathy: clinical characteristics, treatment strategies, and outcome in 62 patients. Mayo Clin Proc 82:441–447
Oldfors A, Moslemi AR, Fyhr IM, Holme E, Larsson NG, Lindberg C (1995) Mitochondrial DNA deletions in muscle fibers in inclusion body myositis. J Neuropathol Exp Neurol 54:581–587
Santorelli FM, Sciacco M, Tanji K, Shanske S, Vu TH, Golzi V, Pestronk A (1996) Multiple mitochondrial DNA deletions in sporadic inclusion body myositis: a study of 56 patients. Ann Neurol 39(6):789–795
Rygiel KA, Tuppen HA, Grady JP (2016) Complex mitochondrial DNA rearrangements in individual cells from patients with sporadic inclusion body myositis. Nucleic Acids Res 44:5313–5329
Lamperti C, Zeviani M (2009) Encephalomyopathies caused by abnormal nuclear-mitochondrial intergenomic cross-talk. Acta Myol 28(1):2–11
Moslemi AR, Lindberg C, Oldfors A (1997) Analysis of multiple mitochondrial DNA deletions in inclusion body myositis. Hum Mutat 10(5):381–386
Griggs RC, Askanas V, DiMauro S, Engel A, Karpati G, Mendell JR, Rowland LP (1995) Inclusion body myositis and myopathies. Ann Neurol 38:705–713
Wallace DC (2010) Mitochondrial DNA mutations in disease and aging. Environ Mol Mutagen 51(5):440–450
Delalande S, de Seze J, Fauchais AL, Hachulla E, Stojkovic T, Ferriby D, Dubucquoi S, Pruvo JP, Vermersch P, Hatron PY (2004) Neurologic manifestations in primary Sjögren syndrome: a study of 82 patients. Medicine 83(5):280–291
Fauchais AL, Martel C, Gondran G, Lambert M, Launav D, Jauberteau MO, Hachulla E, Vidal E, Hatron PY (2010) Immunological profile in primary Sjögren syndrome: clinical significance, prognosis and long-term evolution to other auto-immune disease. Autoimmun Rev 9(9):595–609
Rojana-Udomsart A, Needham M, Luo YB, Fabian V, Walters S, Zilko PJ, Mastaglia FL (2011) The association of sporadic inclusion body myositis and Sjögren’s syndrome in carriers of HLA-DR3 and the 8.1 MHC ancestral haplotype. Clin Neurol Neurosurg 113(7):559–563
Finsterer J, Stöllberger C, Grossegger C, Kroiss A (1999) Hypothyroid myopathy with unusually high serum creatine kinase values. Horm Res 52(4):205–208
Modi G (2000) Cores in hypothyroid myopathy: a clinical, histological and immunofluorescence study. J Neurol Sci 175(1):28–32
Brady S, Squier W, Hilton-Jones D (2013) Clinical assessment determines the diagnosis of inclusion body myositis independently of pathological features. J Neurol Neurosurg Psychiatry 84:1240–1246
Brady S, Squier W, Sewry C, Hanna M, Hilton-Jones D, Holton JL (2014) A retrospective cohort study identifying the principal pathological features useful in the diagnosis of inclusion body myositis. BMJ Open 4(4):e004552
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
GKP: study concept and design, writing, revising the manuscript, accepts responsibility for all research, giving final approval. CK: study concept, mtDNA analysis and interpretation of data, revising the manuscript, giving final approval. SX: acquisition, analysis and interpretation of data. MC: analysis and interpretation of data. EK: study design, drafting, revising the manuscript, giving final approval. CP: study concept, drafting, revising the manuscript, giving final approval.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there are no conflicts of interest.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Papadimas, G.K., Kokkinis, C., Xirou, S. et al. Polymyositis with mitochondrial pathology or atypical form of sporadic inclusion body myositis: case series and review of the literature. Rheumatol Int 39, 1459–1466 (2019). https://doi.org/10.1007/s00296-019-04314-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-019-04314-8