Abstract
Purpose
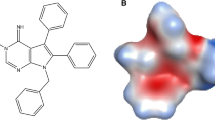
NSC 161128, a phenylurea thiocarbamate, displays activity against the NCI60 anti-cancer cell line panel and xenograft models. The metabolite N-methyl-N′-phenylurea (M10) has been detected in animal plasma; however, detection and quantification of other putative NSC 161128 metabolites have not been undertaken. The purpose of this study was to characterize the pharmacokinetics and metabolism of NSC 161128 in mice and under in vitro conditions.
Methods
An LC–MS/MS assay was developed to evaluate stability and in vitro metabolism of NSC 161128 in liver microsomes and S9 fractions. Single-dose pharmacokinetic profiles for NSC 161128 and its metabolite M10 were obtained following intraperitoneal (I.P.) administration.
Results
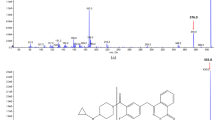
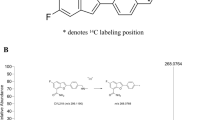
A sensitive and specific positive ionization LC–MS/MS method for measuring NSC 161128 and its metabolites was developed. HPLC separation was achieved under gradient elution using an aqueous methanol mobile phase containing 0.05% formic acid and 0.05% ammonium hydroxide. The assay was linear over the range 1.0–1000 ng/mL. NSC 161128 was stable in aqueous solution and tissue culture media, but not in plasma, where rapid degradation of NSC 161128 to the metabolite M10 was observed. Following I.P. administration of a 200 mg/kg dose to male CD1 mice, the peak plasma concentration of NSC 161128 was 255 ng/mL after 5 min with a plasma half-life of 138 min. Potential bioactivation of NSC 161128 was explored using mouse S9.
Conclusions
An analytical LC–MS/MS method was successfully developed for the detection and quantification of NSC 161128 and its metabolites. These results increase the understanding of NSC 161128 pharmacokinetic and metabolic properties.






Similar content being viewed by others
Data and/or code availability
The data that support the findings of this study are available from the corresponding author, (J.M.R), upon reasonable request.
References
Wiggins HL, Wymant JM, Solfa F, Hiscox SE, Taylor KM, Westwell AD, Jones AT (2015) Disulfiram-induced cytotoxicity and endo-lysosomal sequestration of zinc in breast cancer cells. Biochem Pharmacol 93(3):332–342. https://doi.org/10.1016/j.bcp.2014.12.014
Duan L, Shen H, Zhao G, Yang R, Cai X, Zhang L, Jin C, Huang Y (2014) Inhibitory effect of disulfiram/copper complex on non-small cell lung cancer cells. Biochem Biophys Res Commun 446(4):1010–1016. https://doi.org/10.1016/j.bbrc.2014.03.047
Hoda M, Pajaniradje S, Shakya G, Mohankumar K, Rajagopalan R (2016) Anti-proliferative and apoptosis-triggering potential of disulfiram and disulfiram-loaded polysorbate 80-stabilized PLGA nanoparticles on hepatocellular carcinoma Hep3B cell line. Nanomedicine 12(6):1641–1650. https://doi.org/10.1016/j.nano.2016.02.013
Ketola K, Kallioniemi O, Iljin K (2012) Chemical biology drug sensitivity screen identifies sunitinib as synergistic agent with disulfiram in prostate cancer cells. PLoS ONE 7(12):e51470. https://doi.org/10.1371/journal.pone.0051470
Kast RE, Karpel-Massler G, Halatsch ME (2014) CUSP9* treatment protocol for recurrent glioblastoma: aprepitant, artesunate, auranofin, captopril, celecoxib, disulfiram, itraconazole, ritonavir, sertraline augmenting continuous low dose temozolomide. Oncotarget 5(18):8052–8082. https://doi.org/10.18632/oncotarget.2408
Nechushtan H, Hamamreh Y, Nidal S, Gotfried M, Baron A, Shalev YI, Nisman B, Peretz T, Peylan-Ramu N (2015) A phase IIb trial assessing the addition of disulfiram to chemotherapy for the treatment of metastatic non-small cell lung cancer. Oncologist 20(4):366–367. https://doi.org/10.1634/theoncologist.2014-0424
Schweizer MT, Lin J, Blackford A, Bardia A, King S, Armstrong AJ, Rudek MA, Yegnasubramanian S, Carducci MA (2013) Pharmacodynamic study of disulfiram in men with non-metastatic recurrent prostate cancer. Prostate Cancer Prostatic Dis 16(4):357–361. https://doi.org/10.1038/pcan.2013.28
Huang J, Chaudhary R, Cohen AL, Fink K, Goldlust S, Boockvar J, Chinnaiyan P, Wan L, Marcus S, Campian JL (2019) A multicenter phase II study of temozolomide plus disulfiram and copper for recurrent temozolomide-resistant glioblastoma. J Neurooncol 142(3):537–544. https://doi.org/10.1007/s11060-019-03125-y
Skrott Z, Mistrik M, Andersen KK, Friis S, Majera D, Gursky J, Ozdian T, Bartkova J, Turi Z, Moudry P, Kraus M, Michalova M, Vaclavkova J, Dzubak P, Vrobel I, Pouckova P, Sedlacek J, Miklovicova A, Kutt A, Li J, Mattova J, Driessen C, Dou QP, Olsen J, Hajduch M, Cvek B, Deshaies RJ, Bartek J (2017) Alcohol-abuse drug disulfiram targets cancer via p97 segregase adaptor NPL4. Nature 552(7684):194–199. https://doi.org/10.1038/nature25016
Kannappan V, Ali M, Small B, Rajendran G, Elzhenni S, Taj H, Wang W, Dou QP (2021) Recent advances in repurposing disulfiram and disulfiram derivatives as copper-dependent anticancer agents. Front Mol Biosci 8:741316. https://doi.org/10.3389/fmolb.2021.741316
Teicher BA, Andrews PA (eds) (2004) Anticancer drug development guide. Cancer drug discovery and development, 1 edn. Humana Press, Totowa
Papaioannou M, Mylonas I, Kast RE, Bruning A (2014) Disulfiram/copper causes redox-related proteotoxicity and concomitant heat shock response in ovarian cancer cells that is augmented by auranofin-mediated thioredoxin inhibition. Oncoscience 1(1):21–29. https://doi.org/10.18632/oncoscience.5
Acknowledgements
This project was supported in part with federal funds from the National Cancer Institute, National Institute of Health, under Contract Number N01-CM-2011-0014. The project was also funded in part by the Mayo Clinic Cancer Center Support Grant Number P30 CA15083.
Funding
This project was supported in part with federal funds from the National Cancer Institute, National Institute of Health, under Contract Number N01-CM-2011-0014. The project was also funded in part by the Mayo Clinic Cancer Center Support Grant Number P30 CA15083.
Author information
Authors and Affiliations
Contributions
The authors confirm contribution to the paper as follows: study conception and design: RAK, JMC, MMA, and JMR; data collection: RAK, CAW, RMM; analysis and interpretation of results: EJK, RAK, JMC, MMA, and JMR; draft manuscript preparation: EJK. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
R.A.K. is currently employed by Nuventra Pharma Sciences, but at the time of the study was a research fellow at Mayo Clinic. The other authors have no conflict of interest related to the conduct of this study to disclose.
Ethics approval
All applicable international, national, and/or institutional guidelines for the care and use animals were followed.
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Koubek, E.J., Kudgus, R.A., Walden, C.A. et al. Mouse pharmacokinetics and metabolism of the phenylurea thiocarbamate NSC 161128. Cancer Chemother Pharmacol 90, 161–174 (2022). https://doi.org/10.1007/s00280-022-04440-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-022-04440-4