Abstract
The most important challenges in acute promyelocytic leukemia (APL) is preventing early death and reducing long-term events, such as second neoplasms (s-NPLs). We performed a retrospective analysis of 2670 unselected APL patients, treated with PETHEMA “chemotherapy based” and “chemotherapy free” protocols. Only de novo APL patients who achieved complete remission (CR) and completed the three consolidation cycles were enrolled into the analysis. Out of 2670 APL patients, there were 118 (4.4%) who developed s-NPLs with the median latency period (between first CR and diagnosis of s-NPL) of 48.0 months (range 2.8–231.1): 43.3 (range: 2.8–113.9) for s-MDS/AML and 61.7 (range: 7.1–231.1) for solid tumour. The 5-year CI of all s-NPLs was of 4.43% and 10 years of 7.92%. Among s-NPLs, there were 58 cases of s-MDS/AML, 3 cases of other hematological neoplasms, 57 solid tumours and 1 non-identified neoplasm. The most frequent solid tumour was colorectal, lung and breast cancer. Overall, the 2-year OS from diagnosis of s-NPLs was 40.6%, with a median OS of 11.1 months. Multivariate analysis identified age of 35 years (hazard ratio = 0.2584; p < 0.0001) as an independent prognostic factor for s-NPLs. There were no significant differences in CI of s-NPLs at 5 years between chemotherapy-based vs chemotherapy-free regimens (hazard ratio = 1.09; p = 0.932). Larger series with longer follow-up are required to confirm the potential impact of ATO+ATRA regimens to reduce the incidence of s-NPLs after front-line therapy for APL.
Similar content being viewed by others
Introduction
Acute promyelocytic leukaemia (APL) is the most curable subtype of adult acute myeloid leukaemia (AML) with a complete remission (CR) rate greater than 90% [1,2,3,4,5,6,7,8,9,10,11,12]. This has been achievable due to improvements in the diagnostic tools and supportive care, as well as the introduction of all-trans-retinoic acid (ATRA) [1,2,3,4,5,6,7,8,9] and arsenic trioxide (ATO) into the treatment [10,11,12]. Nowadays, a part of solving early death, another important challenge in the treatment of APL patients is to reduce the long-term events, such as second neoplasms (s-NPLs).
Though the reported incidence of s-NPLs after APL therapy is relatively low, their outcome seems very poor [13,14,15,16,17,18,19,20,21,22,23]. However, there are only a few studies analysing the risk factors for the development of s-NPLs after APL therapy. Among chemotherapy-based regimens, topoisomerase II inhibitors and alkylating drugs are proved to be associated with s-MDS/AML development [24, 25], but these drugs are not used in APL. It is supposed that chemotherapy-free regimens, based on ATRA plus ATO, could reduce the number of s-MDS/AML in APL survivals [20,21,22]. On the other hand, there is a close correlation between long-term environmental arsenic exposure and an increase in solid tumours incidence [26, 27]. Of note, there is still scarce information in the literature concerning s-NPLs after chemotherapy-free APL regimens [20,21,22].
There are two main s-NPLs categories in APL patients: solid tumours and second myelodysplastic syndrome (s-MDS) or acute myeloid leukemia (s-AML). Previous multicentre study by the PETHEMA (Programa para el Tratamiento de Hemopatías Malignas) group characterized patients with s-MDS/AML developed after chemotherapy-based (AIDA) APL protocols. There are still few data concerning the incidence and outcomes of solid tumours after APL therapy [19,20,21,22,23].
This retrospective multicentre study aims to analyse the incidence, risk factors and clinical outcomes of s-NPLs in de novo APL patients treated with 5 consecutive PETHEMA protocols.
Methods
We performed a retrospective analysis on 2670 unselected newly diagnosed APL patients, who were treated according to PETHEMA “chemotherapy based” (APL1996, 1999, 2005, 2012 and 2017 for high risk) and “chemotherapy free” regimen (2017 for low/intermediate risk) between 11.1996 and 11.2021. Treatment protocols are summarized in Table 1 [4, 5, 28, 29] and study selection in Fig. 1. The study was conducted in accordance with the Declaration of Helsinki. Informed written consent to follow the treatment according to PETHEMA protocol was obtained.
Patient’s selection for the study. Diagnosis of APL was confirmed by the presence of t(15;17) in conventional cytogenetic analysis, and/or detection of the PML/RARa with fluorescence in situ hybridization (FISH) or standardized reverse transcription-polymerase chain reaction (RT-PCR) analysis with a sensitivity of 103-104. Only de novo APL patients who achieved complete remission (CR) and who completed the three consolidation cycles were enrolled into the analysis. Patients with APL second to prior neoplasm, as they received chemo and/or radiotherapy before diagnosis of APL, were excluded from the analysis. Patients were treated in Spain, the Netherlands, Argentina, Uruguay, Belgium, Czech Republic, Portugal (PETHEMA registry) and Poland (PALG, Polish Adult Leukemia Group registry); n: number, sNPL: second neoplasm
Definitions of CR, molecular remission and persistence, hematological and molecular relapse have been reported previously [30, 31]. Diagnosis of s-MDS/AML was made according to the WHO criteria [32]. APL relapse was ruled out by cytomorphological and cytogenetic/molecular assessments [30, 31]. The diagnosis of other hematological malignancies and solid tumours was confirmed by histopathological analysis of the excised tissues.
The last patient follow-up was updated on December 2022. The following data was collected at diagnosis: age, gender, ECOG (Eastern Cooperative Oncology Group) performance status score, platelet and leucocyte (WBC) counts, Sanz risk score, fever and coagulopathy, FLT3 (FMS-like tyrosine kinase 3) — internal tandem duplication (ITD), karyotype: t(15;17) vs complex karyotype. Complex karyotype was defined as karyotype with minimum 3 independent abnormalities [33]. Survival and cumulative incidence curves were determined using non-parametric methods using Kaplan-Meier estimators [34]. Differences between curves are done by log-rank test and p-value is given [35]. The probability of developing s-NPL was also estimated by cumulative incidence and the estimated variance was calculated using Aalen–Johansen estimators [36, 37]. The cumulative incidence of n-NPL was calculated from the date of CR. For the cumulative incidence analysis, death in CR and relapse of APL were considered competing causes of failure. Multivariate analysis was performed using the Cox proportional hazards model [38]. Overall survival (OS) was calculated from the date of development of s-NPL. The chi-2 test, with Yates’ correction if necessary, and Mann-Whitney U test and t test were used to analyse differences in the distribution between patient subsets of categorical and continuous nonparametric and parametric variables, respectively. Median lifetimes were determined taking into account censored data. Even if median survival has been reached in a group, it was not possible to calculate complete confidence intervals for those median values. The odds ratio was calculated by median-unbiased estimation. Confidence intervals are calculated using exact methods (mid-p). Characteristics selected for inclusion in the multivariate analysis were those for which there was a significant association in univariate analysis (p .05). All p values reported are two-sided. All tests were performed in R version 4.2.1.
Results
Patient selection
Between November 1996 and November 2021, 3364 APL patients were registered and were intended to be treated according to PETHEMA protocols in Spain, the Netherlands, Argentina, Uruguay, Belgium, Czech Republic, Portugal and Poland. Information on enrolment, eligible patients, lost to follow-up, and exclusion from analysis is shown in a flow diagram (Fig. 1). Of them, there were 2670 de novo APL patients who achieved complete remission and completed induction and all consolidation cycles. Patients included into the study, were treated according to subsequent PETHEMA protocols: LPA1996 (n=169), LPA1999 (n=639), LPA2005 (n=1135), LPA2012 (n=469), LPA2017 (n=258). Main clinical and analytical characteristics of patients included into analysis are presented in a Table 2.
Incidence of second NPLs
Median follow-up of the series was 77 months (range, 17 to 158 months) from diagnosis. Out of 2670 APL patients, 118 (4.4%) developed s-NPLs during follow-up with the median latency period (between first CR and diagnosis of s-NPL) of 48.0 months (range: 2.8–231.1): 43.3 (range: 2.8–113.9) for s-MDS/AML and 61.7 (range: 7.1–231.1) for solid tumour (excluding other hematological neoplasms).
The 5-year CI of all s-NPLs was of 4.43% and 10 years of 7.92%. The CI according to protocols (APL1996, 1999, 2005, 2012, 2017) was as follow: 4.33% vs 3.69% vs 4.91% vs 5.14% vs 1.27% (5 years) and 8.94% vs 6.07% vs 9.61% vs 8.83% vs incomplete observation (10 years) (Table 3, Supplementary Fig. 1).
Among s-NPLs, there were 58 cases of s-MDS/AML, 3 cases of other hematological neoplasms (2 myeloproliferative neoplasms and 1 Hodgkin lymphoma), 57 solid tumours and 1 non-identified neoplasm. CI according to the type of s-NPLs is presented in Table 3, Supplementary Fig. 2.
Information concerning the type of solid tumour was available in 54/57 (94.7%) patients. The most frequent solid tumour was colorectal, followed by lung and breast cancer (Fig. 2A).
Regarding s-MDS/AML, there was information concerning karyotype abnormalities in 34/58 cases (58.6%) and the most frequent cytogenetic abnormalities were complex karyotype, monosomy of 7, and del 7q (Fig. 2B).
Risk factors for development of s-NPLs
In patients developing s-NPLs there was a slight predominance of female sex (57.6%) and the median age at time of diagnosis of APL was higher vs APL without s-APLs: 55 (range from 13 to 84) vs 43 (range from 2 to 87) years. There were no differences in the Sanz risk score distribution (Table 2).
The following risk factors were analysed as possible risk factors for development of all s-NPLs and s-MDS/AML and solid tumour separately: age, gender, ECOG and Sanz risk score, fever and coagulopathy, WBC and platelet counts, karyotype t(15;17) vs t(15:17)+others, FLT3-ITD mutation at diagnosis of APL, chemotherapy-based vs chemotherapy free regimens. Multivariate analysis identified only age ≤ 35 years (hazard ratio = 0.2584; p < 0.0001) as an independent prognostic factor for all s-NPLs (Table 3, Fig. 3B); we found no significant risk factor for development of s-MDS/AML or solid tumour separately probably due to low number of patients.
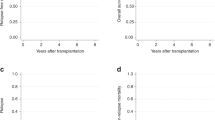
Respect to type of therapy, all cases with s-MDS/AML (n=117) received chemotherapy-based PETHEMA protocols (APL96 – n=14, APL99 – n=35, APL2005- n=69 and APL2012 – n=12). After chemotherapy-free protocol, there was only one case of s-NPL and it was a solid tumour. CI of s-NPLs according to chemotherapy-based vs chemotherapy-free regimens is presented in a Fig. 3A. In multivariate analysis, there were no significant differences of s-NPLs development between chemotherapy-based vs chemotherapy-free regimens (hazard ratio = 1.09; p =0.932).
Outcomes of patients developing s-NPLs
Overall, the 2-year OS from diagnosis of s-NPLs was 40.6%, with a median OS of 11.1 months (Fig. 4A, Table 4). The 2-year OS from diagnosis of s-MDS/AML and from diagnosis of solid tumours was 31.5 % vs 47.4% with median OS of 9.4 months vs 13.7 months respectively (Fig. 4B). In all patients who died, the main cause of death was s-NPLs itself.
Discussion
Our study shows that s-NPLs, both s-MDS/AML and second solid tumours, represent a relatively frequent and poor prognosis late complication in patients with APL. The only risk factor related with the development of all s-NPLs was older age (> 35 years old at diagnosis of APL). Our data suggest a potential reduction in incidence of s-NPLs after chemotherapy-free regimens. Nevertheless, longer follow-up is needed to affirm that chemotherapy-free protocols could reduce the risk of developing s-NPLs. As APL is currently the most curable subtype of AML, all efforts should be focused on reducing long-term toxicities, including s-NPLs.
Generally, the occurrence of s-NPL in survivors of adult cancer has risen from 9 to 19% of all neoplasms diagnosed in 1975–1979 and in 2005–2009 respectively [39]. In case of APL patients, data respect s-NPL are very rare. According to previous publications, the crude incidence of s-MDS/AML ranges between 0.97 and 6.5% [17, 18], and according to a previous PETHEMA analysis the 6-year CI of s-MDS/AML was 2.2% [14]. This result was confirmed in the present publication (a 5-year CI of s-MDS/AML was of 2.8%), while a 10-year CI was almost double (4.03%). The crude incidence of second solid tumours ranges between 1.52 and 18%, but the number of reports is even more limited [14, 20, 21]. In the present study, with longer follow-up, we enlarge the prior PETHEMA series and we analyse the CI of solid tumours and other hematological malignancies as well, resulting in an overall s-NPLs CI of 4.4% at 5-year CI and 7.9% at 10 years. Of note, we show that with longer follow-up, the CI of s-NPLs will clearly increase, in particular for solid tumours were 10-year CI was more than double that of 5-year CI (3.7% vs 1.5%). Unfortunately, we could not compare our series with an age-matched cohort of non-APL populations, but give the younger median age of APL patients (between 40 and 45 years old), our findings clearly suggest that developing and being treated of APL is leading to a higher risk of s-NPLs.
Like in previous publications [13,14,15,16,17,18,19,20,21,22,23], we corroborate that prognosis of s-NPLs is very poor (40.6% of 2-year OS, with a median OS of 11.1 months) and even worse for s-MDS/AML cases. In case of s-MDS/AML, it is certainly related to the presence of adverse cytogenetic abnormalities observed at time of diagnosis of second neoplasm. Moreover, it could be related to cumulative toxicity of previous therapies, including that for APL. Importantly, in our series, the main cause of death after development of s-NPLs was always related to resistance to therapy, progression of second neoplasm or side effects related with the treatment of s-NPLs.
Risk factors for s-NPLs development are still not clearly defined. In a present study, we observed that s-MDS/AML cases occurred only among APL patients treated with chemotherapy-based regimens. According to previous PETHEMA analyses, the incidence of s-MDS/AML between patients treated with APL96 vs anthracycline-reinforced APL99 protocol was similar. Intermediate risk APL patients obtain higher dose of anthracycline that could be a risk for s-MDS/AML development [14]. Nevertheless, we have not observed correlation between Sanz risk score and all s-NPLs or s-MDS/AML development. The impact of maintenance therapy with methotrexate and mercaptopurine is still not clear [14]; however, all patients (except one treated with APL2017 protocol) who developed s-NPLs, received maintenance therapy. The diagnosis of s-MDS/AML with abnormal karyotype (complex karyotype, abnormalities of chromosome 5 or 7) suggests a close relationship with prior cytotoxic agents [14,15,16,17,18, 24, 25]. Complex karyotype and chromosome 5 and 7 abnormalities are associated with use of alkylating agents. In APL therapy topoisomerase II inhibitors (anthracyclines) are used, which have been shown to be associated with the 11q23 rearrangement (KMT2A, previously MLL) [24, 25]. In this context, the role of topoisomerase II inhibitors in leukemogenesis of s-MDS/AML in APL patients remains unclear. Moreover, at the time of diagnosis of APL, additional chromosomal abnormalities (trisomy 8 and abnormalities in chromosome 7 among others) are quite frequent (28–30%) [33, 40,41,42]. Probably, due to low number of patients with additional karyotype, the present study was not able to determine the role of additional chromosomal abnormalities on the development of s-NPL nor s-MDS/AML in APL patients after achieving of CR.
The age more than 35 years old was suggested as an independent risk factor for development of s-MDS/AML [14]. Based on the present analysis, we confirmed that age of 35 or more is an independent risk factor for development for all s-NPLs but not for s-AML/MDS and solid tumours separately.
Data concerning the incidence of s-NPLs after chemotherapy-free regimens are still scarce, but they seem to be equal [20,21,22] or less frequent than after chemotherapy-based regimens. There is a close correlation between exposure to inorganic arsenic and an increase in lung, kidney, liver, bladder and skin cancers incidence [26, 27]. We were unable to show reduction of s-NPLs after chemotherapy-free regimens compared to AIDA-based protocols probably due to: (1) the limited number of patients treated with chemotherapy-free regimens; and (2) the shorter follow-up of these patients, which is very relevant taking into account that median latency to occurrence of solid tumours overlaps with longer follow-up of ATO+ATRA patients in our series.
The incidental occurrence of s-NPLs in APL patients cannot be ruled out. Many risk factors such as increased body mass index (BMI), diet, cigarette smoking, low physical activity could be responsible for the development of s-NPLs in the general population. Interestingly, the majority (59%) of APL patients are overweight or obese (BMI ≥25) [43].
Our study has several limitations related to retrospective design; there are missing data concerning the molecular and cytogenetical analysis at time of diagnosis of APL and of s-NPLs. The number of patients with s-NPL and in particular the group of patients treated with ATRA plus ATO is very small and with short follow-up period. Despite these limitations, this study was performed on a large group of APL patients treated homogenously.
To conclude, s-NPLs are relatively frequent in APL patients. We report higher incidence than previous reports as patients had substantial follow-up. The development of s-NPLs was associated with dismal outcomes, highlighting the need of preventive strategies, long-term monitoring and high suspicion after APL therapy. Further studies are needed in order to assess the potential reduction of the risk of s-NPLs among patients treated with chemotherapy-free regimens.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Lo-Coco F, Ammatuna E, Montesinos P et al (2008) Acute promyelocytic leukemia: recent advances in diagnosis and management. Semin Oncol 35:401–409
Sanz MA, Grimwade D, Tallman MS et al (2009) Management of acute promyelocytic leukemia: recommendations from an expert panel on behalf of the European LeukemiaNet. Blood 113:1875–1891
Fenaux P, Chastang C, Chevret S et al (1999) A randomized comparison of all trans retinoic acid (ATRA) followed by chemotherapy and ATRA plus chemotherapy and the role of maintenance therapy in newly diagnosed acute promyelocytic leukemia. The European APL Group. Blood 14:1192–1200
Sanz MA, Martin G, Gonzalez M et al (2004) Risk adapted treatment of acute promyelocytic leukemia with all trans retinoic acid and anthracycline monochemotherapy: a multicenter study by the PETHEMA group. Blood 103:1237–1243
Sanz MA, Montesinos P, Rayon C et al (2010) Risk adapted treatment of acute promyelocytic leukemia based on all-trans retinoic acid and anthracycline with addition of cytarabine in consolidation therapy for high-risk patients: further improvements in treatment outcome. Blood 115:5137–5146
Mandelli F, Diverio D, Avvisati G et al (1997) Molecular remission in PML/RAR alpha-positive acute promyelocytic leukemia by combined all-trans retinoic acid and idarubicin (AIDA) therapy. Gruppo Italiano-Malattie Ematologiche Maligne dell'Adulto and Associazione Italiana di Ematologia ed Oncologia Pediatrica Cooperative Groups. Blood 90:1014–1021
Lengfelder E, Haferlach C, Saussele S et al (2010) High dose ara-C in the treatment of newly diagnosed acute promyelocytic leukemia: long-term results of the German AMLCG. Leukemia 2009;23:2248-58. Lo CoCo Blood 116:3171–3179
Tallman MS, Andersen JW, Schiffer CA et al (1997) All-trans-retinoic acid in acute promyelocytic leukemia. N Engl J Med 337:1021–1028
Huang ME, Ye YC, Chen SR et al (1988) Use of all-trans retinoic acid in the treatment of acute promyelocytic leukemia. Blood 72:572
Estey E, Garcia-Manero G, Ferrajoli A et al (2006) Use of all-trans retinoic acid plus arsenic trioxide as an alternative to chemotherapy in untreated acute promyelocytic leukemia. Blood 107:3469–3473
Lo-Coco F, Avvisati G, Vignetti M et al (2013) Retinoic acid and arsenic trioxide for acute promyelocytic leukemia. N Engl J Med. 369:111–121
Platzbecker U, Avvisati G, Cicconi L et al (2017) Improved outcomes with retinoic acid and arsenic trioxide compared with retinoic acid and chemotherapy in non-high-risk acute promyelocytic leukemia: final results of the randomized Italian-German APL0406 trial. J Clin Oncol 35:605–612
Pagano L, Gimema F, Pulsoni A et al (2004) Second malignancy after treatment of adult acute myeloid leukemia: cohort study on adult patients enrolled in the GIMEMA trials. Leukemia 18:651–653
Montesinos P, González JD, González J et al (2010) Therapy-related myeloid neoplasms in patients with acute promyelocytic leukemia treated with all-trans-retinoic acid and anthracycline-based chemotherapy. J Clin Oncol 28:3872–3879
Zompi S, Viguié F (2002) Therapy-related acute myeloid leukemia and myelodysplasia after successful treatment of acute promyelocytic leukemia. Leuk Lymphoma 43:275–280
Batzios C, Hayes LA, He SZ, Quach H, McQuilten ZK, Wall M, Campbell LJ (2009) Secondary clonal cytogenetic abnormalities following successful treatment of acute promyelocytic leukemia. Am J Hematol 84:715–719 Erratum in: Am J Hematol. 2010;85:550
Lobe I, Rigal-Huguet F, Vekhoff A, Desablens B, Bordessoule D, Mounier C, Ferrant A, Sanz M, Fey M, Chomienne C, Chevret S, Degos L, Fenaux P, European APL group experience (2003) Myelodysplastic syndrome after acute promyelocytic leukemia: the European APL group experience. Leukemia 17:1600–1604
Latagliata R, Petti MC, Fenu S et al (2002) Therapy-related myelodysplastic syndrome-acute myelogenous leukemia in patients treated for acute promyelocytic leukemia: an emerging problem. Blood 99:822–824
Lenzi L, Lee-Jones L, Mostofa MA, de Andrade DP, Ribeiro RC, Figueiredo BC (2020) Second primary malignancy after acute promyelocytic leukemia: a population-based study. Cancers (Basel) 12:3610
Kayser S, Rahmé R, Martínez-Cuadrón D et al (2020) Outcome of older (≥70 years) APL patients frontline treated with or without arsenic trioxide-an International Collaborative Study. Leukemia 34:2333–2341
Norsworthy KJ, Avagyan A, Bird ST et al (2020) Second cancers in adults with acute promyelocytic leukemia treated with or without arsenic trioxide: a SEER-medicare analysis. Leukemia 34:3082–3084
Eghtedar A, Rodriguez I, Kantarjian H, O'Brien S, Daver N, Garcia-Manero G, Ferrajoli A, Kadia T, Pierce S, Cortes J, Ravandi F (2015) Incidence of secondary neoplasms in patients with acute promyelocytic leukemia treated with all-trans retinoic acid plus chemotherapy or with all-trans retinoic acid plus arsenic trioxide. Leuk Lymphoma 56:1342–1345
Giri S, Pathak R, Aryal MR et al (2017) Second primary malignancy in acute promyelocytic leukemia: a surveillance, epidemiology and end results database study. Futur Oncol 13:1455–1457
Pedersen-Bjergaard J, Andersen MK, Christiansen DH (2000) Therapy-related acute myeloid leukemia and myelodysplasia after high-dose chemotherapy and autologous stem cell transplantation. Blood 95:3273–3279
Pedersen-Bjergaard J, Philip P, Larsen SO et al (1993) Therapy-related myelodysplasia and acute myeloid leukemia. Cytogenetic characteristics of 115 consecutive cases and risk in seven cohorts of patients treated intensively for malignant diseases in the Copenhagen series. Leukemia 7:1975–1986
Chen QY, DesMarais T, Costa M (2019) Metals and mechanisms of carcinogenesis. Annu Rev Pharmacol Toxicol 59:537–554
Liu G, Song Y, Li C et al (2021) Arsenic compounds: the wide application and mechanisms applied in acute promyelocytic leukemia and carcinogenic toxicology. Eur J Med Chem 221:113519
Treatment of acute promyelocytic leukemia PETHEMA LPA 2012, PETHEMA/PALG protocol
Treatment of acute promyelocytic leukemia PETHEMA LPA 2017, PETHEMA/PALG protocol
Cheson BD, Bennett JM, Kopecky KJ et al (2003) Revised recommendations of the International Working Group for Diagnosis, Standardization of Response Criteria, Treatment Outcomes, and Reporting Standards for Therapeutic Trials in Acute Myeloid Leukemia. J Clin Oncol 21:4642–4649
Sanz MA, Fenaux P, Tallman MS et al (2019) Management of acute promyelocytic leukemia: updated recommendations from an expert panel of the European LeukemiaNet. Blood 133:1630–1643
Arber DA, Orazi A, Hasserjian R et al (2016) The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 127:2391–2405
Labrador J, Luño E, Vellenga E et al (2019) Clinical significance of complex karyotype at diagnosis in pediatric and adult patients with de novo acute promyelocytic leukemia treated with ATRA and chemotherapy. Leuk Lymphoma 60:1146–1155
Kaplan EL, Meier P (1958) Nonparametric estimations from incomplete observations. J Am Stat Assoc 53:457–481
Mantel N (1966) Evaluation of survival data and two new rank order statistics arising in its consideration. Cancer Chemother Rep 50:163–170
Gray RJ (1988) A class of K-sample test for comparing the cumulative incidence of a competing risk. Ann Stat 16:1141–1154
Aalen O (1978) Nonparametric estimation of partial transition probabilities in multiple decrement models. Ann Stat 6:534–545
Cox DR (1972) Regression models and life tables (with discussion). J R Stat Soc B 34:187–220
Morton LM, Onel K, Curtis RE et al (2014) The rising incidence of second cancers: patterns of occurrence and identification of risk factors for children and adults. Am Soc Clin Oncol Educ Book:e57–e67
Andersen MK, Pedersen-Bjergaard J (2002) Therapy-related MDS and AML in acute promyelocytic leukemia. Blood 100:1928–1929 author reply 1929
Cervera J, Montesinos P, Hernández-Rivas JM et al (2010) Additional chromosome abnormalities in patients with acute promyelocytic leukemia treated with all-trans retinoic acid and chemotherapy. Haematologica 95:424–431
Sessarego M, Fugazza G, Balleari E et al (1997) High frequency of trisomy 8 in acute promyelocytic leukemia: a fluorescence in situ hybridization study. Cancer Genet Cytogenet 97:161–164
Sobas M, Rodriguez-Veiga R, Vellenga E et al (2020) PETHEMA, HOVON, PALG, GATLA cooperative groups. Characteristics and outcome of adult patients with acute promyelocytic leukemia and increased body mass index treated with the PETHEMA Protocols. Eur J Haematol. 104(3):162–169
Acknowledgements
The authors thank all PALG members for data collection and to all patients for their collaboration in this study.
Funding
This work was partially financed with FEDER funds (CIBERONC (CB16/12/00284)) and with Instituto de Investigación Sanitaria La Fe funds (2016/0158).
Author information
Authors and Affiliations
Contributions
M.S. conceived the study, included data of patients, analysed and interpreted the data, wrote the manuscript; M.Sk. analysed and interpreted the data; P.M. conceived the study, analysed and interpreted the data, wrote the manuscript; S.G. performed the statistical analysis, analysed and interpreted the data; .K-P.W., P-J.B., C.E., O.G., G.F, A.M., C.M., M-C.D., A.E., G.J., G.A., A.L., S.O., S.J., S.M., M.P, V.S.,V.B., L.J., I.A., C.L., M.J., N.G., L;A;, B J., L M., R.C., P.M., P.A., C.E. included data of patients treated in their institutions. All authors reviewed the manuscript and contributed to the final draft.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All procedures performed in present study were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments. The patient signed informed consent to participate in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sobas, M., Knopinska-Posluszny, W., Piątkowska-Jakubas, B. et al. Incidence, risk factors, and outcomes of second neoplasms in patients with acute promyelocytic leukemia: the PETHEMA-PALG experience. Ann Hematol 103, 451–461 (2024). https://doi.org/10.1007/s00277-023-05582-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-023-05582-y