Abstract
Purpose
This study aims to investigate the uptake of transradial approach (TRA) and outpatient setting for transarterial chemoembolization (TACE) and transarterial radioembolization (TARE) in the treatment of hepatocellular carcinoma (HCC) among French interventional radiology centers.
Materials and Methods
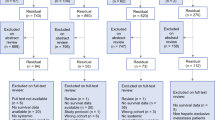
This cross-sectional study was based on a 34-question survey assessing center activity, radial access, and outpatient care. The survey was developed by a working group, tested by two external experts, and distributed to active members of two French radiological societies via a web-based self-reporting questionnaire in March 2022. The survey remained open for eight weeks, with two reminder emails sent to non-responders. Only one answer per center was considered.
Results
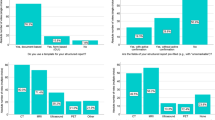
Of the 44 responding centers, 39% (17/44) performed TRA for TACE and/or TARE, with post-procedure patient comfort as main motivation. Among the 27 centers not performing TRA, 33% (9/27) reported a lack of technical experience, but all 27 intended to adopt TRA within two years. Only six centers performed TACE or TARE in an outpatient setting. Reasons limiting its implementation included TACE for HCC not being a suitable intervention (61%, 27/44) and organizational barriers (41%, 18/44). Among centers not performing outpatient TACE or TARE, 34% (13/38) said "No," 34% (13/38) said "Maybe," and 32% (12/38) said "Yes" when asked about adopting it within two years.
Conclusion
French interventional radiologists have low TRA uptake for HCC treatment, but TRA adoption potential exists. Respondents were uncertain about performing TACE or TARE in an outpatient setting within a 2-year horizon.
Graphical Abstract

Similar content being viewed by others
Change history
15 March 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00270-024-03698-w
Abbreviations
- HCC:
-
Hepatocellular carcinoma
- TACE:
-
Transarterial chemoembolization
- TARE:
-
Transarterial radioembolization
- TRA:
-
Transradial approach
- SFICV:
-
French society of interventional and cardiovascular imaging
- SIAD:
-
French society of abdominal and gastrointestinal imaging
References
Fritsche MR, Watchmaker JM, Lipnik AJ, et al. Outpatient Transarterial chemoembolization of hepatocellular carcinoma: review of a same-day discharge strategy. J Vasc Interv Radiol. 2018;29(4):550–5. https://doi.org/10.1016/j.jvir.2017.11.018.
Mitchell JW, O’Connell WG, Kisza P, et al. Safety and feasibility of outpatient transcatheter hepatic arterial embolization for hepatocellular carcinoma. J Vasc Interv Radiol. 2009;20(2):203–8. https://doi.org/10.1016/j.jvir.2008.10.027.
Nasser F, Cavalcante RN, Galastri FL, et al. Safety and feasibility of same-day discharge of patients with hepatocellular carcinoma treated with transarterial chemoembolization with drug-eluting beads in a liver transplantation program. J Vasc Interv Radiol. 2014;25(7):1012–7. https://doi.org/10.1016/j.jvir.2014.02.025.
Prajapati HJ, Rafi S, El-Rayes BF, Kauh JS, Kooby DA, Kim HS. Safety and feasibility of same-day discharge of patients with unresectable hepatocellular carcinoma treated with doxorubicin drug-eluting bead transcatheter chemoembolization. J Vasc Interv Radiol. 2012;23(10):1286–93. https://doi.org/10.1016/j.jvir.2012.07.003.
Iezzi R, Pompili M, Posa A, et al. Transradial versus transfemoral access for hepatic chemoembolization: intrapatient prospective single-center study. J Vasc Interv Radiol. 2017;28(9):1234–9. https://doi.org/10.1016/j.jvir.2017.06.022.
Yamada R, Bracewell S, Bassaco B, et al. Transradial versus transfemoral arterial access in liver cancer embolization: randomized trial to assess patient satisfaction. J Vasc Interv Radiol. 2018;29(1):38–43. https://doi.org/10.1016/j.jvir.2017.08.024PMID-29150395.
Liu LB, Cedillo MA, Bishay V, et al. Patient experience and preference in transradial versus transfemoral access during transarterial radioembolization: a randomized single-center trial. J Vasc Interv Radiol. 2019;30(3):414–20. https://doi.org/10.1016/j.jvir.2018.10.005.
Brueck M, Bandorski D, Kramer W, Wieczorek M, Höltgen R, Tillmanns H. A randomized comparison of transradial versus transfemoral approach for coronary angiography and angioplasty. Jacc Cardiovasc Intervent. 2009;2(11):1047–54. https://doi.org/10.1016/j.jcin.2009.07.016PMID-19926042.
Karrowni W, Vyas A, Giacomino B, et al. Radial versus femoral access for primary percutaneous interventions in ST-segment elevation myocardial infarction patients a meta-analysis of randomized controlled trials. Jacc Cardiovasc Intervent. 2013;6(8):814–23. https://doi.org/10.1016/j.jcin.2013.04.010PMID-23968700.
Agostoni P, Biondi-Zoccai GGL, Benedictis MLD, et al. Radial versus femoral approach for percutaneous coronary diagnostic and interventional procedures systematic overview and meta-analysis of randomized trials. J Am Coll Cardiol. 2004;44(2):349–56. https://doi.org/10.1016/j.jacc.2004.04.034PMID-15261930.
Posham R, Biederman DM, Patel RS, et al. Transradial approach for noncoronary interventions: a single-center review of safety and Feasibility in the first 1,500 cases. J Vasc Interv Radiol. 2016;27(2):159–66. https://doi.org/10.1016/j.jvir.2015.10.026PMID-26706186.
Jolly SS, Yusuf S, Cairns J, et al. Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): a randomised, parallel group, multicentre trial. Lancet. 2011;377(9775):1409–20. https://doi.org/10.1016/s0140-6736(11)60404-2PMID-21470671.
Mamas MA, Ratib K, Routledge H, et al. Influence of access site selection on PCI-related adverse events in patients with STEMI: meta-analysis of randomised controlled trials. Heart. 2012;98(4):303. https://doi.org/10.1136/heartjnl-2011-300558PMID-22147900.
Brasselet C, Tassan S, Nazeyrollas P, Hamon M, Metz D. Randomised comparison of femoral versus radial approach for percutaneous coronary intervention using abciximab in acute myocardial infarction: results of the FARMI trial. Heart. 2007;93(12):1556. https://doi.org/10.1136/hrt.2007.117309PMID-17639099.
Goldberg SL, Renslo R, Sinow R, French WJ. Learning curve in the use of the radial artery as vascular access in the performance of percutaneous transluminal coronary angioplasty. Catheter Cardio Diag. 1998;44(2):147–52. https://doi.org/10.1002/(sici)1097-0304(199806)44:2%3c147::aid-ccd5%3e3.0.co;2-6PMID-9637436.
Gayed A, Yamada R, Bhatia S, et al. Society of interventional radiology quality improvement standards on radial artery access. J Vasc Interv Radiol. 2021;32(5):761.e761-761.e721. https://doi.org/10.1016/j.jvir.2020.12.013PMID-33933252.
Dehghani P, Mohammad A, Bajaj R, et al. Mechanism and predictors of failed transradial approach for percutaneous coronary interventions. Jacc Cardiovasc Intervent. 2009;2(11):1057–64. https://doi.org/10.1016/j.jcin.2009.07.014PMID-19926044.
Valsecchi O, Vassileva A, Musumeci G, et al. Failure of transradial approach during coronary interventions: anatomic considerations. Catheter Cardio Inte. 2006;67(6):870–8. https://doi.org/10.1002/ccd.20732PMID-16649233.
Bertrand OF, Rao SV, Pancholy S, et al. Transradial approach for coronary angiography and interventions results of the first international transradial practice survey. Jacc Cardiovasc Intervent. 2010;3(10):1022–31. https://doi.org/10.1016/j.jcin.2010.07.013PMID-20965460.
Iezzi R, Posa A, Bilhim T, Guimaraes M. Most common misconceptions about transradial approach in interventional radiology: results from an international survey. Diagnostic Intervent Radiol. 2021;27(5):649–53.
Hadjivassiliou A, Cardarelli-Leite L, Jalal S, et al. Left distal transradial access (ldTRA): a comparative assessment of conventional and distal radial artery size. Cardiovasc Intervent Radiol. 2020;43(6):850–7. https://doi.org/10.1007/s00270-020-02485-7.
Hsieh M-Y, Lin L, Tsai K-C, Wu C-C. Radial artery approach to salvage nonmaturing radiocephalic arteriovenous fistulas. Cardiovasc Intervent Radiol. 2013;36(4):957–63. https://doi.org/10.1007/s00270-012-0533-7.
Yip H-K, Youssef AA, Chang W-N, et al. Feasibility and safety of transradial arterial approach for simultaneous right and left vertebral artery angiographic studies and stenting. Cardiovasc Intervent Radiol. 2007;30(5):840–6. https://doi.org/10.1007/s00270-007-9051-4.
Fohlen A, Tasu JP, Kobeiter H, Bartoli JM, Pelage JP, Guiu B. Transarterial chemoembolization (TACE) in the management of hepatocellular carcinoma: results of a French national survey on current practices. Diagn Interv Imaging. 2018;99(9):527–35. https://doi.org/10.1016/j.diii.2018.03.003.
Steele JR, Wallace MJ, Hovsepian DM, et al. Guidelines for establishing a quality improvement program in interventional radiology. J Vasc Interv Radiol. 2010;21(5):617–25.
Zuckerman RB, Sheingold SH, Orav EJ, Ruhter J, Epstein AM. Readmissions, observation, and the hospital readmissions reduction program. N Engl J Med. 2016;374(16):1543–51.
Hund HC, Frantz SK, Wu H, et al. Six-year evaluation of same-day discharge following conventional transarterial chemoembolization of hepatocellular carcinoma. J Vasc Interv Radiol. 2023;34(3):378–85. https://doi.org/10.1016/j.jvir.2022.11.029.
de Baere T, Ronot M, Chung JW, et al. Initiative on superselective conventional transarterial chemoembolization results (INSPIRE). Cardiovasc Intervent Radiol. 2022;45(10):1430–40.
Vanderbecq Q, Grégory J, Dana J, et al. Improving pain control during transarterial chemoembolization for hepatocellular carcinoma performed under local anesthesia with multimodal analgesia. Diagn Interv Imaging. 2023;104(3):123–32. https://doi.org/10.1016/j.diii.2022.10.013.
Delicque J, Hermida M, Piron L, et al. Intra arterial treatment of hepatocellular carcinoma: comparison of MELD score variations between radio-embolization and chemo-embolization. Diagn Interv Imaging. 2019;100(11):689–97. https://doi.org/10.1016/j.diii.2019.05.006.
Wu SE, Charles HW, Park JS, Goldenberg AS, Deipolyi AR. Obesity conveys poor outcome in patients with hepatocellular carcinoma treated by transarterial chemoembolization. Diagn Interv Imaging. 2017;98(1):37–42. https://doi.org/10.1016/j.diii.2016.06.002.
Gregory J, Tselikas L, Allimant C, et al. Defining textbook outcome for selective internal radiation therapy of hepatocellular carcinoma: an international expert study. Eur J Nucl Med Mol Imaging. 2023;50(3):921–8. https://doi.org/10.1007/s00259-022-06002-5.
Maleux G, Albrecht T, Arnold D, et al. Predictive factors for adverse event outcomes after transarterial radioembolization with yttrium-90 resin microspheres in europe: results from the prospective observational CIRT study. Cardiovasc Intervent Radiol. 2023. https://doi.org/10.1007/s00270-023-03391-4.
Gabr A, Kallini JR, Gates VL, et al. Same-day 90Y radioembolization: implementing a new treatment paradigm. Eur J Nucl Med Mol Imaging. 2016;43(13):2353–9. https://doi.org/10.1007/s00259-016-3438-xPMID-27315059.
Li MD, Chu KF, DePietro A, et al. Same-day yttrium-90 radioembolization: feasibility with resin microspheres. J Vasc Interv Radiol. 2019;30(3):314–9.
Lublóy Á. Factors affecting the uptake of new medicines: a systematic literature review. BMC Health Serv Res. 2014;14(1):469. https://doi.org/10.1186/1472-6963-14-469.
Acknowledgements
The authors would like to express their gratitude to the responders of the participating centers for taking the time to diligently complete the survey.
Funding
This study was not supported by any funding.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
For this type of study informed consent is not required.
Consent for Publication
For this type of study consent for publication is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: This article was originally published under a working title, ‘French Interventional Radiology Centers’ Uptake of Transradial Approach and Outpatient HCC Intra-Arterial Treatments’, which was refined to ‘French Interventional Radiology Centers’ Uptake of Transradial Approach and Outpatient Hepatocellular Carcinoma Intra-Arterial Treatments’.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Grégory, J., Ronot, M., Laurent, V. et al. French Interventional Radiology Centers’ Uptake of Transradial Approach and Outpatient Hepatocellular Carcinoma Intra-Arterial Treatments. Cardiovasc Intervent Radiol 47, 432–440 (2024). https://doi.org/10.1007/s00270-023-03578-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-023-03578-9