Abstract
Background
Various techniques have been used for the execution of carotid endarterectomy; primary (PC), patch closure (CP) and eversion technique (ET).The superiority of any of them is still unproven. The aim of this study was to compare the long-term outcomes of each technique in terms of cerebrovascular event (CVE), restenosis, survival and major cardiac event (MACE).
Methods
Between 2007 and 2018, a retrospective analysis of prospectively recorded data from three European tertiary centers was undertaken including 1.357 patients. Demographics, comorbidities and medical treatment were analyzed in relation to long-term outcomes. Freedom from CVE, restenosis (> 70%), survival and MACE were estimated with Kaplan–Meier analysis curve.
Results
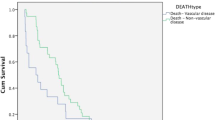
The mean age was 69.5 ± 8 (72% males;79% asymptomatic). 472 (35%) were treated with PC, 504 (37%) with CP and 381 (28%) with ET. Differences among groups were observed in age (P < 0.001), gender (P < 0.01), hypertension (P = 0.01), dyslipidemia (P < 0.001) and statin treatment (P < 0.001). The mean follow-up was 4.7 ± 3 years (median: 5 years). Seventy-three patients presented a CVE during 8 years of follow-up. The freedom from CVE including all techniques was 96% (SE 0.6%), 93% (SE 1%) and 89% (SE 1.6%), at 2, 5 and 8 years of follow-up, respectively, with no difference between groups (P .289). Freedom from restenosis was at 96% (SE 0.7%) and 89% (SE 5%) at 5 and 10 years, respectively, for all methods without differences. ET was associated with a higher mortality rate (P < 0.001) and MACE rate (P < 0.001).
Conclusions
Excellent outcomes were achieved with all types of closure techniques with low rates of MACE and other adverse events during long-term follow-up after CEA.





Similar content being viewed by others
References
Naylor AR, Ricco JB, de Borst GJ et al (2018) Editor’s choice: management of atherosclerotic carotid and vertebral artery disease: 2017 clinical practice guidelines of the European Society for Vascular Surgery (ESVS). Eur J Vasc Endovasc Surg 55:3–81
Abbott AL, Paraskevas KI, Kakkos SK et al (2015) Systematic review of guidelines for the management of asymptomatic and symptomatic carotid stenosis. Stroke 46:3288–3301
Ren S, Li X, Wen J et al (2018) Systematic review of randomized controlled trials of different types of patch materials during carotid endarterectomy. PLoS ONE 8:e55050
Halliday A, Harrison M, Hayter E et al (2010) 10-year stroke prevention after successful carotid endarterectomy for asymptomatic stenosis (ACST-1): a multicentre randomised trial. Lancet 376:1074–1084
Klarin D, Cambria RP, Ergul EA et al (2018) Risk factor profile and anatomic features of previously asymptomatic patients presenting with carotid-related stroke. J Vasc Surg 68:1390–1395
Archie JP Jr (2000) A fifteen-year experience with carotid endarterectomy after a formal operative protocol requiring highly frequent patch angioplasty. J Vasc Surg 31:724–735
Bond R, Rerkasem K, Naylor AR et al (2004) Systematic review of randomized controlled trials of patch angioplasty versus primary closure and different types of patch materials during carotid endarterectomy. J Vasc Surg 40:1126–1135
Huizing E, Vos CG, van den Akker PJ et al (2019) A systematic review of patch angioplasty versus primary closure for carotid endarterectomy. J Vasc Surg 69:1962–74.e4
Goodney PP, Nolan BW, Eldrup-Jorgensen J et al (2010) Restenosis after carotid endarterectomy in a multicenter regional registry. J Vasc Surg 52:897–904
Muto A, Nishibe T, Dardik H et al (2009) Patches for carotid artery endarterectomy: current materials and prospects. J Vasc Surg 50:206–213
Texakalidis P, Giannopoulos S, Charisis N et al (2018) A meta-analysis of randomized trials comparing bovine pericardium and other patch materials for carotid endarterectomy. J Vasc Surg 68:1241–56.e1
Kim JH, Cho YP, Kwon TW et al (2012) Ten-year comparative analysis of bovine pericardium and autogenous vein for patch angioplasty in patients undergoing carotid endarterectomy. Ann Vasc Surg 26:353–358
Cunningham EJ, Bond R, Mehta Z et al (2002) Long-term durability of carotid endarterectomy for symptomatic stenosis and risk factors for late postoperative stroke. Stroke 33:2658–2663
Edenfield L, Blazick E, Healey C et al (2019) Long-term impact of the vascular study group of new England carotid patch quality initiative. J Vasc Surg 69:1801–1806
Ballotta E, Toniato A, Da Giau G et al (2014) Durability of eversion carotid endarterectomy. J Vasc Surg 59:1274–1281
Maertens V, Maertens H, Kint M et al (2016) Complication rate after carotid endarterectomy comparing patch angioplasty and primary closure. Ann Vasc Surg 30:248–252
Wallaert JB, Cronenwett JL, Bertges DJ et al (2013) Optimal selection of asymptomatic patients for carotid endarterectomy based on predicted 5-year survival. J Vasc Surg 58:112–118
Demirel S, Goossen K, Bruijnen H et al (2017) Systematic review and meta-analysis of post-carotid endarterectomy hypertension after eversion versus conventional carotid endarterectomy. J Vasc Surg 65:868–882
Black JH 3rd, Ricotta JJ, Jones CE (2010) Long-term results of eversion carotid endarterectomy. Ann Vasc Surg 24:92–99
Ballotta E, Meneghetti G, Manara R et al (2007) Long-term survival and stroke-free survival after eversion carotid endarterectomy for asymptomatic severe carotid stenosis. J Vasc Surg 46:265–270
Acknowledgments
None
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Informed consent
Obtained from all individual participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nana, P., Spanos, K., Piffaretti, G. et al. Long-term Durability and Safety of Carotid Endarterectomy Closure Techniques. World J Surg 44, 3545–3554 (2020). https://doi.org/10.1007/s00268-020-05604-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-020-05604-0