Abstract
Background
There currently is no consensus on how to accurately predict early rebleeding and death after a major variceal bleed. This study investigated the relative predictive performances of the original Child–Pugh (CP), model for end-stage liver disease (MELD) and a four-category recalibrated Child–Pugh (rCP).
Methods
This prospective study included all adult patients admitted to Groote Schuur Hospital with acute esophageal variceal bleeding secondary to alcoholic cirrhosis, between January 2000 and December 2017. CP and rCP grades and MELD score were calculated on admission, and the predictive ability in discriminating in-hospital rebleeding and death was compared by area under receiver-operating characteristic (AUROC) curves.
Results
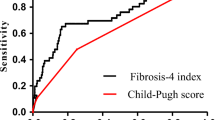
During the study period, 403 consecutive adult patients were treated for bleeding esophageal varices of whom 225 were secondary to alcoholic cirrhosis. Twenty-four (10.6%) patients were CP grade A, 88 (39.1%) grade B and 113 (50.2%) grade C on hospital admission. MELD scores ranged from 6 to 40. Thirty-one (13.8%) patients rebleed, and 41 (18.2%) patients died. There was no difference in the discriminatory capacity of the CP (AUROC 0.59, 95% CI 0.50–0.670) and MELD (AUROC 0.62, 95% CI 0.51–0.73) to predict rebleeding (p = 0.72), or between the Child–Pugh (AUROC 0.75, 95% CI 0.71–0.81) and MELD (AUROC 0.71, 95% CI 0.62–0.80) to predict death (p = 0.35). The rCP classification (A–D) had a significantly improved discriminatory capacity (AUROC 0.83 95% CI 0.77–0.89) compared to the CP score (A–C) and MELD to predict death (p = 0.004).
Conclusion
A recalibrated Child–Pugh score outperforms the original Child–Pugh grade and MELD score in predicting in-hospital death in patients with bleeding esophageal varices secondary to alcoholic cirrhosis.


Similar content being viewed by others
References
Garcia-Tsao G, Bosch J (2010) Management of varices and variceal hemorrhage in cirrhosis. N Engl J Med 62:823–832
Hernández-Gea V, Berbel C, Baiges A, García-Pagán JC (2018) Acute variceal bleeding: risk stratification and management (including TIPS). Hepatol Int 12(Supplement 1):81–90
de Franchis R (2015) Expanding consensus in portal hypertension: report of the Baveno VI Consensus Workshop: stratifying risk and individualizing care for portal hypertension. J Hepatol 63:743–752
Augustin S, González A, Genescà J (2010) Acute esophageal variceal bleeding: current strategies and new perspectives. World J Hepatol 27(2):261–274
Amitrano L, Guardascione MA, Manguso F et al (2012) The effectiveness of current acute variceal bleed treatments in unselected cirrhotic patients: refining short-term prognosis and risk factors. Am J Gastroenterol 107:1872–1878
Augustin S, Altamirano J, Gonzalez A et al (2011) Effectiveness of combined pharmacologic and ligation therapy in high-risk patients with acute esophageal variceal bleeding. Am J Gastroenterol 106:1787–1795
Fortune BE, Garcia-Tsao G, Ciarleglio M et al (2017) Child-Turcotte-Pugh class is best at stratifying risk in variceal hemorrhage: analysis of a US multicenter prospective study. J Clin Gastroenterol 51:446–453
Christensen E (2004) Prognostic models including the Child-Pugh, MELD and Mayo risk scores -where are we and where should we go? J Hepatol 41:344–350
Malinchoc M, Kamath PS, Gordon FD et al (2000) A model to predict poor survival in patients undergoing transjugular intrahepatic portosystemic shunts. Hepatology 31:864–871
Child CG, Turcotte JG (1964) Surgery and portal hypertension. The liver and portal hypertension. Saunders, Philadelphia, pp 50–64
Pugh RN, Murray-Lyon IM, Dawson JL et al (1973) Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 60:646–649
Augustin S, Millan L, Gonzalez A et al (2011) Prognostic evaluation of patients with acute variceal bleeding. Dis Markers 31:155–164
Trieu JA, Bilal M, Hmoud B (2018) Factors associated with waiting time on the liver transplant list: an analysis of the United Network for Organ Sharing (UNOS) database. Ann Gastroenterol 31:84–89
Krige JE, Kotze UK, Bornman PC, Shaw JM, Klipin M (2006) Variceal recurrence, rebleeding, and survival after endoscopic injection sclerotherapy in 287 alcoholic cirrhotic patients with bleeding esophageal varices. Ann Surg 244:764–770
Krige JEJ. Beningfield SJ (2018) Endoscopic therapy in the management of esophageal varices: injection sclerotherapy and variceal ligation. In: Nyhus, Baker, Fischer (ed) Mastery of surgery, 7th edn. Philadelphia, pp 1384–1398
Krige JEJ, Bornman PC (2007) Endoscopic therapy in the management of esophageal varices: injection sclerotherapy and variceal ligation. In: Blumgart L (ed) Surgery of the liver, biliary tract and pancreas, 4th edn. Saunders, Elsevier, Philadelphia, pp 1579–1593
Al Sibae MR, Cappell MS (2011) Accuracy of MELD scores in predicting mortality in decompensated cirrhosis from variceal bleeding, hepatorenal syndrome, alcoholic hepatitis, or acute liver failure as well as mortality after non-transplant surgery or TIPS. Dig Dis Sci 56:977–987
D’Amico G, De Franchis R (2003) Upper digestive bleeding in cirrhosis. Post-therapeutic outcome and prognostic indicators. Hepatology 38:599–612
Thomopoulos K, Theocharis G, Mimidis K et al (2006) Improved survival of patients presenting with acute variceal bleeding. Prognostic indicators of short- and long-term mortality. Dig Liver Dis 38:899–904
Chalasani N, Kahi C, Francois F et al (2003) Improved patient survival after acute variceal bleeding: a multicenter, cohort study. Am J Gastroenterol 98:653–659
Boix J, Lorenzo-Zuniga V, Moreno de Vega V et al (2007) Sclerotherapy and esophageal variceal bleeding: time to forget it, or not? Endoscopy 39:478
Carbonell N, Pauwels A, Serfaty L et al (2004) Improved survival after variceal bleeding in patients with cirrhosis over the past two decades. Hepatology 40:652–659
Reverter E, Tandon P, Augustin S et al (2014) A MELD-based model to determine risk of mortality among patients with acute variceal bleeding. Gastroenterology 146:412–419
Augustin S, Muntaner L, Altamirano JT et al (2009) Predicting early mortality after acute variceal hemorrhage based on classification and regression tree analysis. Clin Gastroenterol Hepatol 7:1347–1354
Kaplan DE, Dai F, Skanderson M, Aytaman A et al (2016) Recalibrating the Child-Turcotte-Pugh Score to improve prediction of transplant-free survival in patients with Cirrhosis. Dig Dis Sci 61:3309–3320
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Krige, J., Spence, R.T., Jonas, E. et al. A New Recalibrated Four-Category Child–Pugh Score Performs Better than the Original Child–Pugh and MELD Scores in Predicting In-Hospital Mortality in Decompensated Alcoholic Cirrhotic Patients with Acute Variceal Bleeding: a Real-World Cohort Analysis. World J Surg 44, 241–246 (2020). https://doi.org/10.1007/s00268-019-05211-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05211-8