Abstract
Background
The ‘gentle’ handling of tissue (i.e., ‘respect for tissue’) is a fundamental aspect of surgical performance and learning. To date, there have been no methodological assessments that quantitatively measure ‘gentleness.’ Therefore, the aims of this study were (1) to propose a novel metric for gentle surgical maneuvers, (2) to validate the feasibility of this methodology, and (3) to explore safer surgical techniques through this methodology.
Methods
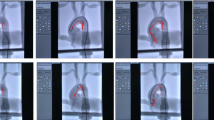
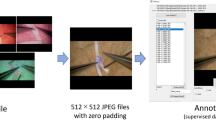
Using surgical video-based motion software, the motion of the carotid artery around plaque was analyzed and quantified during a carotid endarterectomy. Kinematic parameters (minimum and maximum acceleration, and maximum and mean velocity) were compared among the surgical tasks and techniques, as well as between novice and expert surgeons.
Results
The surgical tasks of dissecting the common carotid artery, passing the proximal vessel loops, and ligating vessels showed the highest absolute values of kinematic parameters. Dissections perpendicular to the line of the internal carotid artery tended to show higher kinematic parameters than those in the parallel direction, with blunt dissections typically higher than sharp dissections. The kinematic parameters of novice surgeons were significantly higher than those of experts, and receiver operating curve analysis showed a strong discriminative power.
Conclusion
This study shows that tissue motion parameters could be a novel and feasible surrogate marker for the objective assessment on the ‘gentleness’ of surgical performance. Future studies should be performed to further elucidate the relationship on the direct correlation between tissue kinematic data and clinical outcomes or surgical adverse events.




Similar content being viewed by others
References
Birkmeyer JD, Finks JF, O’Reilly A et al (2013) Surgical skill and complication rates after bariatric surgery. N Engl J Med 369:1434–1442
Sugiyama T, Gan LS, Zareinia K et al (2017) Tool-tissue interaction forces in brain arteriovenous malformation surgery. World Neurosurg 102:221–228
Sugiyama T, Lama S, Gan LS et al (2018) Forces of tool-tissue interaction to assess surgical skill level. JAMA Surg 153:234–242
van Hove PD, Tuijthof GJ, Verdaasdonk EG et al (2010) Objective assessment of technical surgical skills. Br J Surg 97:972–987
Szasz P, Louridas M, Harris KA et al (2015) Assessing technical competence in surgical trainees: a systematic review. Ann Surg 261:1046–1055
Aoun SG, El Ahmadieh TY, El Tecle NE et al (2015) A pilot study to assess the construct and face validity of the Northwestern Objective Microanastomosis Assessment Tool. J Neurosurg 123:103–109
Martin JA, Regehr G, Reznick R et al (1997) Objective structured assessment of technical skill (OSATS) for surgical residents. Br J Surg 84:273–278
Darzi A, Smith S, Taffinder N (1999) Assessing operative skill. Needs to become more objective. BMJ 318:887–888
Kalu PU, Atkins J, Baker D et al (2005) How do we assess microsurgical skill? Microsurgery 25:25–29
Rutherford DN, D’Angelo AL, Law KE et al (2015) Advanced engineering technology for measuring performance. Surg Clin North Am 95:813–826
Zareinia K, Maddahi Y, Gan LS et al (2016) A force-sensing bipolar forceps to quantify tool-tissue interaction forces in microsurgery. IEEE/ASME Trans Mechatron 21:2365–2377
Richstone L, Schwartz MJ, Seideman C et al (2010) Eye metrics as an objective assessment of surgical skill. Ann Surg 252:177–182
Ghasemloonia A, Maddahi Y, Zareinia K et al (2017) Surgical skill assessment using motion quality and smoothness. J Surg Educ 74:295–305
Harada K, Morita A, Minakawa Y et al (2015) Assessing microneurosurgical skill with medico-engineering technology. World Neurosurg 84:964–971
Grober ED, Roberts M, Shin EJ et al (2010) Intraoperative assessment of technical skills on live patients using economy of hand motion: establishing learning curves of surgical competence. Am J Surg 199:81–85
Sarkiss CA, Philemond S, Lee J et al (2016) Neurosurgical Skills assessment: measuring technical proficiency in neurosurgery residents through intraoperative video evaluations. World Neurosurg 89:1–8
Sugiyama T (2017) Mastering intracranial microvascular anastomoses—basic techniques and surgical pearls. MEDICUS SHUPPAN Publishers Co., Ltd, Osaka, p 209
Sugiyama T, Kazumata K, Asaoka K et al (2015) Reappraisal of microsurgical revascularization for anterior circulation ischemia in patients with progressive stroke. World Neurosurg 84:1579–1588
Bonrath EM, Gordon LE, Grantcharov TP (2015) Characterising ‘near miss’ events in complex laparoscopic surgery through video analysis. BMJ Qual Saf 24:516–521
Glarner CE, Hu YY, Chen CH et al (2014) Quantifying technical skills during open operations using video-based motion analysis. Surgery 156:729–734
McGoldrick RB, Davis CR, Paro J et al (2015) Motion Analysis for microsurgical training: objective measures of dexterity, economy of movement, and ability. Plast Reconstr Surg 136:231e–240e
Maniglia AJ, Han DP (1991) Cranial nerve injuries following carotid endarterectomy: an analysis of 336 procedures. Head Neck 13:121–124
Muller M, Reiche W, Langenscheidt P et al (2000) Ischemia after carotid endarterectomy: comparison between transcranial Doppler sonography and diffusion-weighted MR imaging. AJNR Am J Neuroradiol 21:47–54
Oikawa K, Kato T, Oura K et al (2017) Preoperative cervical carotid artery contrast-enhanced ultrasound findings are associated with development of microembolic signals on transcranial Doppler during carotid exposure in endarterectomy. Atherosclerosis 260:87–93
Udesh R, Natarajan P, Thiagarajan K et al (2017) Transcranial Doppler monitoring in carotid endarterectomy: a systematic review and meta-analysis. J Ultrasound Med 36:621–630
Smith JL, Evans DH, Gaunt ME et al (1998) Experience with transcranial Doppler monitoring reduces the incidence of particulate embolization during carotid endarterectomy. Br J Surg 85:56–59
Alcantara SD, Wuamett JC, Lantis JC 2nd et al (2014) Outcomes of combined somatosensory evoked potential, motor evoked potential, and electroencephalography monitoring during carotid endarterectomy. Ann Vasc Surg 28:665–672
Malcharek MJ, Ulkatan S, Marino V et al (2013) Intraoperative monitoring of carotid endarterectomy by transcranial motor evoked potential: a multicenter study of 600 patients. Clin Neurophysiol 124:1025–1030
Uchino H, Nakamura T, Kuroda S et al (2012) Intraoperative dual monitoring during carotid endarterectomy using motor evoked potentials and near-infrared spectroscopy. World Neurosurg 78:651–657
Sutherland GR, Lama S, Gan LS et al (2013) Merging machines with microsurgery: clinical experience with neuroArm. J Neurosurg 118:521–529
Moccia S, Wirkert SJ, Kenngott H et al (2018) Uncertainty-aware organ classification for surgical data science applications in laparoscopy. IEEE Trans Biomed Eng 65:2649–2659
Gaunt ME, Martin PJ, Smith JL et al (1994) Clinical relevance of intraoperative embolization detected by transcranial Doppler ultrasonography during carotid endarterectomy: a prospective study of 100 patients. Br J Surg 81:1435–1439
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no personal, financial, or institutional interest in any of the drugs, materials, or devices described in this manuscript.
Informed consent
Informed consent was obtained from all individual participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sugiyama, T., Nakamura, T., Ito, Y. et al. A Pilot Study on Measuring Tissue Motion During Carotid Surgery Using Video-Based Analyses for the Objective Assessment of Surgical Performance. World J Surg 43, 2309–2319 (2019). https://doi.org/10.1007/s00268-019-05018-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05018-7