Abstract
Background
Neuroblastoma (NBL) is the most common extracranial solid tumor in children. Despite a good overall prognosis in NBL patients, the outcome of children with stage 4 disease, even with multimodal intensive therapy, remains poor. The role of extended surgical resection of the primary tumor is in numerous studies controversial. The aim of this study was to retrospectively analyze the impact of radical surgical resection on the overall- and event-free survival of stage 4 NBL patients.
Methods
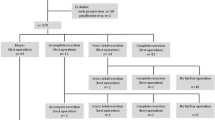
We retrospectively analyzed patient charts of 40 patients with stage 4 NBL treated in our institution between January 1990 and May 2012. All clinical and pathological findings of stage 4 NBL patients were included. Extent of surgery was assessed from the operation records and was classified as non-radical (tumor biopsy, partial 50–90% resection) or radical (near-complete >90% resection, complete resection). Overall- (OS) and event-free (EFS) survival was assessed using the Kaplan–Meier analysis and log-rank test. A multivariate Cox regression analysis was used to demonstrate independency.
Results
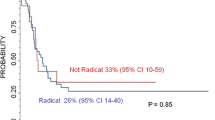
In total, 29/40 patients were operated radically (>90% resection), whereas 11 patients received subtotal resection or biopsy only. OS and EFS were significantly increased in patients with radical operation compared with non-radical resection (p = 0.0003 for OS, p = 0.004 for EFS; log-rank test). A multivariate Cox regression analysis revealed radical operation as a significant and independent parameter for OS and EFS.
Conclusions
Our data indicate that radical (over 90% resection) surgery improves OS and EFS in stage 4 NBL patients.




Similar content being viewed by others
References
Weinstein JL, Katzenstein HM, Cohn SL (2003) Advances in the diagnosis and treatment of neuroblastoma. Oncologist 8:278–292
Brodeur GM, Pritchard J, Berthold F et al (1993) Revisions of the international criteria for neuroblastoma diagnosis, staging, and response to treatment. J Clin Oncol 11:1466–1477
Maris JM (2010) Recent advances in neuroblastoma. NEJM 362:2202–2211
Matthay KK, Villablanca JG, Seeger RC et al (1999) Treatment of high risk neuroblastoma with intensive chemotherapy, radiotherapy, autologous bone marrow transplantation, and 13-cis-retinoic acid. NEJM 341:1165–1173
Berthold F, Boos J, Burdach S et al (2005) Myeloablative megatherapy with autologous stem-cell rescue versus oral maintenance chemotherapy as consolidation treatment in patients with high-risk neuroblastoma: a randomised controlled trial. Lancet Oncol 6:649–658
Perez CA, Matthay KK, Atkinson JB et al (2000) Biologic variables in the outcome of stages 1 and 2 neuroblastoma treated with surgery as primary therapy: a childrens cancer group study. J Clin Oncol 18:18–26
Matthay KK, Sather HN, Seeger RC et al (1989) Excellent outcome of stage 2 neuroblastoma is independent of residual disease and radiation therapy. J Clin Oncol 7:236–244
Matthay KK, Perez C, Seeger RC et al (1998) Successful treatment of stage 3 neuroblastoma based on prospective biologic staging: a childrens cancer group study. J Clin Oncol 16:1256–1264
Englum BR, Rialon KL, Speicher PJ et al (2015) Value off surgical resection in children with high-risk neuroblastoma. Pediatr Blood Cancer 62:1529–1535
Yeung F, Chung PH, Tam PK et al (2015) Is complete resection of high-risk stage 4 neuroblastoma associated with better survival? J Pediatr Surg 50:2107–2111
Rich BS, McEvoy MP, Kelly NE et al (2011) Resectability and operative morbidity after chemotherapy in neuroblastoma patients with encasement of major visceral arteries. J Pediatr Surg 46:103–107
Simon T, Häberle B, Hero B et al (2013) Role of surgery in the treatment of patients with stage 4 neuroblastoma age 18 months or older at diagnosis. J Clin Oncol 31:752–758
La Quaglia MP, Kushner BH, Su W et al (2004) The impact of gross total resection on local control and survival in high risk neuroblastoma. J Pediatr Surg 39:412–417
Escobar MA, Grosfeld JL, Powell RL et al (2006) Long-term outcomes in patients with stage 4 neuroblastoma. J Pediatr Surg 41:377–381
Sultan I, Ghandour K, Al-Jumaily U et al (2009) Local control of the primary tumour in metastatic neuroblastoma. Eur J Cancer 45:1728–1732
Von Schweinitz D, Hero B, Berthold F (2002) The impact of surgical radicality on outcome in childhood neuroblastoma. Eur J Pediatr Surg 12:402–409
Castel V, Tovar JA, Costa E et al (2002) The role of surgery in stage 4 neuroblastoma. J Pediatr Surg 37:1574–1578
Adkins S, Sawin R, Gerbing RB et al (2004) Efficacy of complete resection for high-risk neuroblastoma: a childrens cancer group study. J Pediatr Surg 39:931–936
McGregor LM, Rao BN, Davidoff AM et al (2005) The impact of early resection of primary neuroblastoma on the survival of children older than 1 year of age with stage 4 disease. Cancer 104:2837–2846
Von Allmen D, Davidoff AM, London WB et al (2017) Impact of extent of resection on local control and survival in patients from the COG A3973 study with high-risk neuroblastoma. J Clin Oncol 35:208–216
Von Allmen D, Grupp S, Diller L et al (2005) Agressive surgical therapy and radiotherapy for patients with high-risk neuroblastoma treated with rapid sequence tandem transplant. J Pediatr Surg 40:936–941
La Quaglia MP (2015) The role of primary tumor resection in neuroblastoma: when and how much. Pediatr Blood Cancer 62:1516–1517
Acknowledgments
This study is part of the doctoral thesis work of the author Katherin Vollmer.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the studies involving human participants (treatment of patients) are in accordance with the ethical standards of the institutional research committee and with the 1964 Helsiniki declaration and its later amendments or comparable ethical standards. For this type of study (retrospective data analysis), formal consent is not required (Ethical committee of the University Hospital Frankfurt, Decision No. 253/13).
Rights and permissions
About this article
Cite this article
Vollmer, K., Gfroerer, S., Theilen, TM. et al. Radical Surgery Improves Survival in Patients with Stage 4 Neuroblastoma. World J Surg 42, 1877–1884 (2018). https://doi.org/10.1007/s00268-017-4340-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4340-9