Abstract
Background
The safety of anticoagulation interruption in patients requiring surgical or invasive procedures remains unclear. We thus performed a systematic review and meta-analyses of randomized controlled trials (RCTs) and non-randomized studies (NRS).
Methods
MEDLINE, Embase and Central databases were searched to March 2017 without date or language restrictions. We considered RCTs and NRS comparing anticoagulation interruption with any anticoagulation (continuation or heparin bridging) in adult surgical patients taking oral anticoagulation. Data were independently extracted. The quality of the evidence was assessed following recommendations from the Cochrane collaboration (GRADE approach). Risk ratios were calculated for 30-day events: thromboembolic (TE) events, major bleeding and mortality. Additional analyses explored the effects of different anticoagulation strategies.
Results
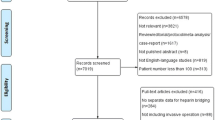
Twelve reports were included: 4 RCTs (2190 participants) and 8 NRS (18993 participants). Trials included mostly participants with atrial fibrillation. Interrupting anticoagulation did not seem to increase TE events (RR 0.65, 95% CI [0.33, 1.30]—4 studies, 2190 participants) and resulted in less bleeding (RR 0.41, 95% CI [0.22, 0.78]—3 studies, 2126 participants) compared to anticoagulation continuation or heparin bridging. The GRADE assessment was moderate. Similar results were found in non-randomized studies, but the quality of the evidence was low. Possible strategy-specific effects were identified: forgoing heparin bridging seemed beneficial, but these effects were less clear with other strategies.
Conclusion
Interrupting anticoagulation in patients requiring invasive procedures did not seem to result in harm and protected against major bleeding. Uncertainty remains regarding the safety of this strategy in indications other than atrial fibrillation and in moderate- to high-risk surgery.
Study registration
http://www.en.anaesthesie.usz.ch/research/Pages/Study-protocols.aspx


Similar content being viewed by others
References
Nielsen VG, Asmis LM (2010) Hypercoagulability in the perioperative period. Best Pract Res Clin Anaesthesiol 24:133–144
Wysokinski WE, McBane RD 2nd (2012) Periprocedural bridging management of anticoagulation. Circulation 126:486–490
Nishimura RA, Otto CM, Bonow RO et al (2014) 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Thorac Cardiovasc Surg 148:e1–e132
Kirchhof P, Benussi S, Kotecha D et al (2016) 2016 ESC guidelines for the management of atrial fibrillation developed in collaboration with EACTS. Eur Heart J 37:2893–2962
Spyropoulos AC, Al-Badri A, Sherwood MW et al (2016) Periprocedural management of patients receiving a vitamin K antagonist or a direct oral anticoagulant requiring an elective procedure or surgery. J Thromb Haemost 14:875–885
Steinberg BA, Kim S, Thomas L et al (2014) Lack of concordance between empirical scores and physician assessments of stroke and bleeding risk in atrial fibrillation: results from the Outcomes Registry for Better Informed Treatment of Atrial Fibrillation (ORBIT-AF) registry. Circulation 129:2005–2012
Eijgenraam P, ten Cate H, ten Cate-Hoek AT (2014) Practice of bridging anticoagulation: guideline adherence and risk factors for bleeding. Neth J Med 72:157–164
Ahmed I, Gertner E, Nelson WB et al (2010) Continuing warfarin therapy is superior to interrupting warfarin with or without bridging anticoagulation therapy in patients undergoing pacemaker and defibrillator implantation. Heart Rhythm 7:745–749
Clark NP, Witt DM, Davies LE et al (2015) Bleeding, recurrent venous thromboembolism, and mortality risks during warfarin interruption for invasive procedures. Jama Int Med 175:1163–1168
Wilson WW, Wilson W (2012) Enoxaparin bridge therapy in patients with nonvalvular atrial fibrillation: a ten year retrospective analysis. J Am Coll Cardiol 59:E605
Wysokinski WE, McBane RD, Daniels PR et al (2008) Periprocedural anticoagulation management of patients with nonvalvular atrial fibrillation. Mayo Clin Proc 83:639–645
Han ZH, Ren XJ, Wang Y (2013) Anticoagulation management of patients with long-term warfarin therapy after valve replacement during the perioperative period of pacemaker implantation. Int J Clin Exp Med 6:594–598
Bernard ML, Shotwell M, Nietert PJ et al (2012) Meta-analysis of bleeding complications associated with cardiac rhythm device implantation. Circ Arrhythm Electrophysiol 5:468–474
Du L, Zhang Y, Wang W et al (2014) Perioperative anticoagulation management in patients on chronic oral anticoagulant therapy undergoing cardiac devices implantation: a meta-analysis. Pacing Clin Electrophysiol 37:1573–1586
Dunn AS, Turpie AG (2003) Perioperative management of patients receiving oral anticoagulants: a systematic review. Arch Int Med 163:901–908
Eijgenraam P, ten Cate H, Ten Cate-Hoek A (2013) Safety and efficacy of bridging with low molecular weight heparins: a systematic review and partial meta-analysis. Curr Pharm Des 19:4014–4023
Proietti R, Porto I, Levi M et al (2015) Risk of pocket hematoma in patients on chronic anticoagulation with warfarin undergoing electrophysiological device implantation: a comparison of different peri-operative management strategies. Eur Rev Med Pharmacol Sci 19:1461–1479
Siegal D, Yudin J, Kaatz S et al (2012) Periprocedural heparin bridging in patients receiving vitamin K antagonists: systematic review and meta-analysis of bleeding and thromboembolic rates. Circulation 126:1630–1639
Douketis JD, Spyropoulos AC, Kaatz S et al (2015) Perioperative bridging anticoagulation in patients with atrial fibrillation. N Engl J Med 373:823–833
Airaksinen KE, Korkeila P, Lund J et al (2013) Safety of pacemaker and implantable cardioverter-defibrillator implantation during uninterrupted warfarin treatment–the FinPAC study. Int J Cardiol 168:3679–3682
Steinberg BA, Peterson ED, Kim S et al (2015) Use and outcomes associated with bridging during anticoagulation interruptions in patients with atrial fibrillation: findings from the Outcomes Registry for Better Informed Treatment of Atrial Fibrillation (ORBIT-AF). Circulation 131:488–494
Douketis JD, Healey JS, Brueckmann M et al (2015) Perioperative bridging anticoagulation during dabigatran or warfarin interruption among patients who had an elective surgery or procedure: substudy of the RE-LY trial. Thromb Haemost 113:625–632
Garcia D, Alexander JH, Wallentin L et al (2014) Management and clinical outcomes in patients treated with apixaban vs warfarin undergoing procedures. Blood 124:3692–3698
Beyer-Westendorf J, Gelbricht V, Forster K et al (2014) Peri-interventional management of novel oral anticoagulants in daily care: results from the prospective Dresden NOAC registry. Eur Heart J 35:1888–1896
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med 151:W65–W94
Reeves BC, Deeks JJ, Higgins JPT, et al. (2011) Chapter 13: including non-randomized studies. In: Higgins JPT, Green S (eds) Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011). The Cochrane Collaboration Available from www.cochrane-handbook.org
Schünemann H, Oxman A, Vist G, et al. (2011) Chapter 12: interpreting results and drawing conclusions. In: Higgins JPT, Green S (eds), Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011). The Cochrane Collaboration Available from www.handbook.cochrane.org
Schulman S, Kearon C, Subcommittee on Control of Anticoagulation of the S, et al. (2005) Definition of major bleeding in clinical investigations of antihemostatic medicinal products in non-surgical patients. J Thromb Haemost 3:692–694
Higgins J, Altman D, Sterne J (2011) Chapter 8: assessing risk of bias in included studies. In: Higgins JPT, Green S (eds) Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011). The Cochrane Collaboration Available from www.handbook.cochrane.org
Deeks J, Higgins J, Altman D (2011) Chapter 9: analysing data and undertaking meta-analyses. In: Higgins JPT, Green S (eds). Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011). The Cochrane Collaboration Available at: www.cochrane-handbook.org
Sedgwick P (2013) Meta-analyses: heterogeneity and subgroup analysis. BMJ 346:f4040
Groenwold RH, Rovers MM, Lubsen J et al (2010) Subgroup effects despite homogeneous heterogeneity test results. BMC Med Res Methodol 10:43
Biase L, Burkhardt JD, Santangeli P et al (2014) Periprocedural stroke and bleeding complications in patients undergoing catheter ablation of atrial fibrillation with different anticoagulation management: results from the Role of Coumadin in Preventing Thromboembolism in Atrial Fibrillation (AF) Patients Undergoing Catheter Ablation (COMPARE) randomized trial. Circulation 129:2638–2644
Birnie DH, Healey JS, Wells GA et al (2013) Pacemaker or defibrillator surgery without interruption of anticoagulation. N Engl J Med 368:2084–2093
Douketis JD, Wang G, Chan N et al (2016) Effect of standardized perioperative dabigatran interruption on the residual anticoagulation effect at the time of surgery or procedure. J Thromb Haemost JTH 14:89–97
Dunn AS, Spyropoulos AC, Turpie AG (2007) Bridging therapy in patients on long-term oral anticoagulants who require surgery: the Prospective Peri-operative Enoxaparin Cohort Trial (PROSPECT). J Thromb Haemost 5:2211–2218
Hammerstingl C, Omran H, Bonn Registry of Alternative Anticoagulation to Prevent Vascular E (2009) Bridging of oral anticoagulation with low-molecular-weight heparin: experience in 373 patients with renal insufficiency undergoing invasive procedures. Thromb Haemost 101:1085–1090
Revigliono JI, Cornavaca T, Becerra F et al (2014) Perioperative control of vitamin K antagonists in elective surgery. Medicina 74:385–390
Rowley CP, Bernard ML, Brabham WW et al (2013) Safety of continuous anticoagulation with dabigatran during implantation of cardiac rhythm devices. Am J Cardiol 111:1165–1168
Schulman S, Carrier M, Lee AY et al (2015) Perioperative management of dabigatran: a prospective cohort study. Circulation 132:167–173
Douketis J, Weitz J, Murphy S et al (2015) Perioperative adverse outcomes in patients with atrial fibrillation taking edoxaban or warfarin: analysis of the ENGAGE AF-TIMI 48 trial. J Am Coll Cardiol 65:A2092
Giudici MC, Paul DL, Bontu P et al (2004) Pacemaker and implantable cardioverter defibrillator implantation without reversal of warfarin therapy. Pacing Clin Electrophysiol 27:358–360
Mima Y, Yasaka M, Wakugawa Y et al (2015) Safety and management of antithrombotic therapy with intra-arterial catheter procedures. Intern Med 54:2115–2120
Nandoe Tewarie RD, Bartels RH (2010) The perioperative use of oral anticoagulants during surgical procedures for carpal tunnel syndrome. A preliminary study. Acta Neurochir 152:1211–1213
Sherwood MW, Douketis JD, Patel MR et al (2014) Outcomes of temporary interruption of rivaroxaban compared with warfarin in patients with nonvalvular atrial fibrillation: results from the rivaroxaban once daily, oral, direct factor Xa inhibition compared with vitamin K antagonism for prevention of stroke and embolism trial in atrial fibrillation (ROCKET AF). Circulation 129:1850–1859
Shipkov H, Irthum C, Seguin P et al (2015) Evaluation of the risk of post-operative bleeding complications in skin cancer surgery without interruption of anticoagulant/antithrombotic medication: a prospective cohort study. J Plast Surg Hand Surg 49:242–246
Woods K, Douketis JD, Kathirgamanathan K et al (2007) Low-dose oral vitamin K to normalize the international normalized ratio prior to surgery in patients who require temporary interruption of warfarin. J Thromb Thrombolysis 24:93–97
Cano O, Munoz B, Tejada D et al (2012) Evaluation of a new standardized protocol for the perioperative management of chronically anticoagulated patients receiving implantable cardiac arrhythmia devices. Heart Rhythm 9:361–367
Deharo JC, Sciaraffia E, Leclercq C et al (2016) Perioperative management of antithrombotic treatment during implantation or revision of cardiac implantable electronic devices: the European Snapshot Survey on Procedural Routines for Electronic Device Implantation (ESS-PREDI). Europace 18:778–784
Cheng A, Nazarian S, Brinker JA et al (2011) Continuation of warfarin during pacemaker or implantable cardioverter-defibrillator implantation: a randomized clinical trial. Heart Rhythm Off J Heart Rhythm Soc 8:536–540
Steib A, Barre J, Mertes M et al (2010) Can oral vitamin K before elective surgery substitute for preoperative heparin bridging in patients on vitamin K antagonists? J Thromb Haemost 8:499–503
Garcia DA, Regan S, Henault LE et al (2008) Risk of thromboembolism with short-term interruption of warfarin therapy. Arch Intern Med 168:63–69
Jaffer AK, Brotman DJ, Bash LD et al (2010) Variations in perioperative warfarin management: outcomes and practice patterns at nine hospitals. Am J Med 123:141–150
McBane RD, Wysokinski WE, Daniels PR et al (2010) Periprocedural anticoagulation management of patients with venous thromboembolism. Arterioscler Thromb Vasc Biol 30:442–448
Essebag V, Verma A, Healey JS et al (2016) Clinically significant pocket hematoma increases long-term risk of device infection: BRUISE CONTROL INFECTION study. J Am Coll Cardiol 67:1300–1308
Hirsh J, Anand SS, Halperin JL et al (2001) Guide to anticoagulant therapy: Heparin: a statement for healthcare professionals from the American Heart Association. Circulation 103:2994–3018
January CT, Wann LS, Alpert JS et al (2014) 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society. Circulation 130:2071–2104
Acknowledgements
This work was supported by institutional funds, Institute of Anesthesiology, University of Zurich and University Hospital of Zurich, Switzerland. The funding organization had no role in the design and conduct of the study; in the collection, management, analysis or interpretation of the data; or in the preparation, review or approval of the manuscript.
Author contributions
Hovaguimian and Spahn conceived and designed the study; Hovaguimian, Köppel and Spahn acquired, analyzed and interpreted the data; Hovaguimian drafted the manuscript; Hovaguimian, Köppel and Spahn critically revised the manuscript for important intellectual content; Hovaguimian performed statistical analysis; Spahn obtained the funding for the study; Hovaguimian provided administrative, technical and material support; Spahn supervised the study; Dr Hovaguimian had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Dr Spahn affirms that this manuscript is an honest, accurate and transparent account of the study being reported; that no important aspects of the study have been omitted; and that any discrepancies from the study as planned (and, if relevant, registered) have been explained.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Declaration of interest
Dr FH and Dr SK were supported by institutional funds during the realization of this work (institutional funds, Institute of Anesthesiology, University of Zurich and University Hospital of Zurich, Switzerland); Dr DRS reports that his academic department is/has been receiving grant support from the Swiss National Science Foundation, Berne, Switzerland, the Ministry of Health (Gesundheitsdirektion) of the Canton of Zurich, Switzerland, for Highly Specialized Medicine, the Swiss Society of Anesthesiology and Reanimation (SGAR), Berne, Switzerland, the Swiss Foundation for Anesthesia Research, Zurich, Switzerland, Bundesprogramm Chancengleichheit, Berne, Switzerland, CSL Behring, Berne, Switzerland, Vifor SA, Villars-sur-Glane, Switzerland. Prof DRS was the chair of the ABC Faculty and is the co-chair of the ABC-Trauma Faculty, which both are managed by Physicians World Europe GmbH, Mannheim, Germany, and sponsored by unrestricted educational grants from Novo Nordisk Health Care AG, Zurich, Switzerland, CSL Behring GmbH, Marburg, Germany, and LFB Biomedicaments, Courtaboeuf Cedex, France. In the past 5 years, Dr DRS has received honoraria or travel support for consulting or lecturing from the following companies: Abbott AG, Baar, Switzerland, AMGEN GmbH, Munich, Germany, AstraZeneca AG, Zug, Switzerland, Baxter AG, Volketswil, Switzerland, Baxter S.p.A., Roma, Italy, Bayer (Schweiz) AG, Zurich, Switzerland, Bayer Pharma AG, Berlin, Germany, B. Braun Melsungen AG, Melsungen, Germany, Boehringer lngelheim (Schweiz) GmbH, Basel, Switzerland, Bristol-Myers-Squibb, Rueil-Malmaison Cedex, France, and Baar, Switzerland, CSL Behring GmbH, Hattersheim am Main, Germany, and Berne, Switzerland, Curacyte AG, Munich, Germany, Daiichi Sankyo (Schweiz) AG, Thalwil, Switzerland, Ethicon Biosurgery, Sommerville, New Jersey, USA, Fresenius SE, Bad Homburg v.d.H., Germany, Galenica AG, Bern, Switzerland (including Vifor SA, Villars-sur-Glane, Switzerland), GlaxoSmithKline GmbH & Co. KG, Hamburg, Germany, Janssen-Cilag AG, Baar, Switzerland, Janssen-Cilag EMEA, Beerse, Belgium, LFB Biomedicaments, Courtaboeuf Cedex, France, Merck Sharp & Dahme AG, Luzern, Switzerland, Novo Nordisk A/S, Bagsvard, Denmark, Octapharma AG, Lachen, Switzerland, Organon AG, Pfaffikon/SZ, Switzerland, Oxygen Biotherapeutics, Costa Mesa, CA, PAION Deutschland GmbH, Aachen, Germany, Pharmacosmos A/S, Holbaek, Denmark, Photonics Healthcare B.V., Utrecht, Netherlands, ratiopharm Arzneimittel Vertriebs GmbH, Vienna, Austria, Roche Diagnostics International Ltd, Reinach, Switzerland, Roche Pharma (Schweiz) AG, Reinach, Switzerland, Sarstedt AG & Co., Sevelen, Switzerland, and Numbrecht, Germany, Schering-Plough International, Inc., Kenilworth, New Jersey, USA, Tern International GmbH, Munich, Germany, Verum Diagnostica GmbH, Munich, Germany, Vifor Pharma Deutschland GmbH, Munich, Germany, Vifor Pharma Osterreich GmbH, Vienna, Austria, Vifor (International) AG, St. Gallen, Switzerland.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hovaguimian, F., Köppel, S. & Spahn, D.R. Safety of Anticoagulation Interruption in Patients Undergoing Surgery or Invasive Procedures: A Systematic Review and Meta-analyses of Randomized Controlled Trials and Non-randomized Studies. World J Surg 41, 2444–2456 (2017). https://doi.org/10.1007/s00268-017-4072-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4072-x