Abstract
Background
Postoperative chylous ascites (CA) following pancreatic surgery is uncommon. If left untreated, it leads to malnutrition, immunodeficiency and increased postoperative morbidity and mortality. The aim of this study was to seek out risk factors associated with CA onset and conservative treatment (CT) failure in order to determine better management of CA following pancreatic resection.
Materials and methods
All consecutive patients who underwent pancreatic surgery between 2004 and 2014 were reviewed retrospectively. Main demographic, clinical and pathological data were searched for CA risk factors. Patients with CA successfully treated with CT alone were compared to those requiring additional bipedal lymphangiography (BPLAG) in order to seek out risk factors associated with CT failure.
Results
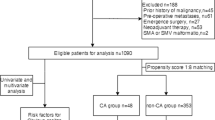
Fifteen patients (2.4 %) developed CA after pancreatic surgery. Para-aortic lymph node sampling and early enteral feeding were found to be independent risk factors for postoperative CA (OR 6.36, p = 0.024 and OR 12.18, p = 0.02, respectively). CT was successful in ten patients, and five patients required additional BPLAG to achieve CA resolution. Statistical analysis revealed no significant risk factors for CT failure, including total lymph node count (p = 0.196), para-aortic lymph node sampling (p = 0.661) or maximum chyle loss per day (p = 0.758).
Conclusions
Owing to postoperative CA rarity, there is no consensus in treatment. Early on, CT should be attempted in all patients with CA. BPLAG is a safe and efficient procedure that should be discussed earlier in the step-up therapeutic management.


Similar content being viewed by others
References
Press OW, Press NO, Kaufman SD (1982) Evaluation and management of chylous ascites. Ann Intern Med 96:358–364
Pabst TS III, McIntyre KE Jr, Schilling JD, Hunter GC, Bernhard VM (1993) Management of chyloperitoneum after abdominal aortic surgery. Am J Surg 166:194–199
Bonner GM, Warren JM (1998) A review of the nutritional management of chyle leakage in adults. J Hum Nutr Diet 11:105–114
Leibovitch I, Mor Y, Golomb J, Ramon J (2002) The diagnosis and management of postoperative chylous ascites. J Urol 167:449–457
Aalami OO, Allen DB, Organ CH (2000) Chylous ascites: a collective review. Surgery 128:761–778
Kuboki S, Shimizu H, Yoshidome H, Ohtsuka M, Kato A, Yoshitomi H et al (2013) Chylous ascites after hepatopancreatobiliary surgery. Br J Surg 100:522–527
Kaas R, Rustman LD, Zoetmulder FAN (2001) Chylous ascites after oncological abdominal surgery: incidence and treatment. Eur J Surg Oncol EJSO 27:187–189
Evans JG, Spiess PE, Kamat AM, Wood CG, Hernandez M, Pettaway CA et al (2006) Chylous ascites after post-chemotherapy retroperitoneal lymph node dissection: review of the M. D. Anderson experience. J Urol 176:1463–1467
Deso S, Ludwig B, Kabutey N-K, Kim D, Guermazi A (2012) Lymphangiography in the Diagnosis and Localization of Various Chyle Leaks. Cardiovasc Interv Radiol 35:117–126
Matsumoto T, Yamagami T, Kato T, Hirota T, Yoshimatsu R, Masunami T et al (2008) The effectiveness of lymphangiography as a treatment method for various chyle leakages. Br J Radiol 82:286–290
Lee EW, Shin JH, Ko HK, Park J, Kim SH, Sung K-B (2014) Lymphangiography to treat postoperative lymphatic leakage: a technical review. Korean J Radiol 15:724
Tulunay G, Ureyen I, Turan T, Karalok A, Kavak D, Ozgul N et al (2012) Chylous ascites: analysis of 24 patients. Gynecol Oncol 127:191–197
Malik HZ, Crozier J, Murray L, Carter R (2007) Chyle leakage and early enteral feeding following pancreatico-duodenectomy: management options. Dig Surg 24:418–422
Assumpcao L, Cameron JL, Wolfgang CL, Edil B, Choti MA, Herman JM et al (2008) Incidence and management of chyle leaks following pancreatic resection: a high volume single-center institutional experience. J Gastrointest Surg 12:1915–1923
Hidden G (1979) Physiologie de la circulation lymphatique. Anat Clin 1:331–345
Van der Gaag NA, Verhaar AC, Haverkort EB, Busch ORC, van Gulik TM, Gouma DJ (2008) Chylous Ascites after Pancreaticoduodenectomy: introduction of a Grading System. J Am Coll Surg 207:751–757
Loukas M, Wartmann CT, Louis RG, Tubbs RS, Salter EG, Gupta AA et al (2007) Cisterna chyli: a detailed anatomic investigation. Clin Anat 20:683–688
Schwarz L, Lupinacci RM, Svrcek M, Lesurtel M, Bubenheim M, Vuarnesson H et al (2014) Para-aortic lymph node sampling in pancreatic head adenocarcinoma: para-aortic lymph node sampling in pancreatic head adenocarcinoma. Br J Surg 101:530–538
Huang Q, Jiang Z-W, Jiang J, Li N, Li J-S (2004) Chylous ascites: treated with total parenteral nutrition and somatostatin. World J Gastroenterol 10:2588–2591
Giovannini I, Giuliante F, Chiarla C, Giordano M, Ardito F, Vellone M et al (2008) External lymphatic fistula after intra-abdominal lymphadenectomy for cancer. Treatment with total parenteral nutrition and somatostatin. Nutrition 24:1220–1223
Kim EA, Park H, Jeong SG, Lee C, Lee JM, Park CT (2014) Octreotide therapy for the management of refractory chylous ascites after a staging operation for endometrial adenocarcinoma: octreotide for chylous ascites. J Obst Gynaecol Res 40:622–626
Alejandre-Lafont E, Krompiec C, Rau WS, Krombach GA (2011) Effectiveness of therapeutic lymphography on lymphatic leakage. Acta Radiol 52:305–311
Jeffrey JD (1990) The management of Chyle Fistula. Laryngoscope 100(07):771–774
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tabchouri, N., Frampas, E., Marques, F. et al. Chylous Ascites Management After Pancreatic Surgery. World J Surg 41, 1054–1060 (2017). https://doi.org/10.1007/s00268-016-3772-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3772-y