Abstract
Background
There is a paucity of evidence comparing the safety of prepectoral and partial subpectoral implant-based breast reconstruction using acellular dermal matrices (ADM). We performed a meta-analysis to evaluate the postoperative complications of the two approaches.
Methods
PubMed, EMBASE, Web of Science and Cochrane Library were searched to retrieve relevant articles. The rates of the complications were, respectively, pooled, and relative risk (RR) was estimated with 95% confidence intervals (CIs) to compare the incidence between the two cohorts.
Results
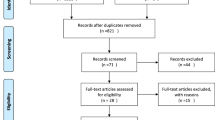
Ten articles reporting on 2667 breast reconstructions were eligible. The hematoma rate was lower in the prepectoral group (RR = 0.590, 95% CI 0.351–0.992). No significant difference was observed in terms of seroma (RR = 1.079, 95% CI 0.489–2.381), skin flap necrosis (RR = 0.936, 95% CI 0.587–1.493), infection (RR = 0.985, 95% CI 0.706–1.375), tissue expander/implant explantation (RR = 0.741, 95% CI 0.506–1.085), wound dehiscence (RR = 1.272, 95% CI 0.605–2.673), capsular contracture (RR = 0.939, 95% CI 0.678–1.300) and rippling (RR = 2.485, 95% CI 0.986–6.261). The RR of animation deformity for the prepectoral group compared with the subpectoral group was 0.040 (95% CI, 0.002–0.853).
Conclusions
This systematic review suggested that with appropriate patient selection, prepectoral breast reconstruction could avoid animation deformity without incurring higher risk of early wound complications, capsular contracture or rippling than partial subpectoral breast reconstruction. Plastic surgeons should complete a comprehensive assessment of the patients before choosing appropriate surgical approaches in clinical practice.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.










Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249
Sinnott CJ, Persing SM, Pronovost M, Hodyl C, McConnell D, Ott Young A (2018) Impact of postmastectomy radiation therapy in prepectoral versus subpectoral implant-based breast reconstruction. Ann Surg Oncol 25(10):2899–2908
Panchal H, Matros E (2017) Current trends in postmastectomy breast reconstruction. Plast Reconstr Surg 140(5):7s–13s
Sigalove S, Maxwell GP, Sigalove NM, Storm-Dickerson TL, Pope N, Rice J, Gabriel A (2017) Prepectoral implant-based breast reconstruction: rationale, indications, and preliminary results. Plast Reconstr Surg 139(2):287–294
Haddock NT, Kadakia Y, Liu YL, Teotia SS (2021) Prepectoral versus subpectoral tissue expander breast reconstruction: a historically controlled, propensity score-matched comparison of perioperative outcomes. Plast Reconstr Surg 148(1):1–9
Chandarana MN, Jafferbhoy S, Marla S, Soumian S, Narayanan S (2018) Acellular dermal matrix in implant-based immediate breast reconstructions: a comparison of prepectoral and subpectoral approach. Gland Surg 7(Suppl 1):s64–s69
Yang JY, Kim CW, Lee JW, Kim SK, Lee SA, Hwang E (2019) Considerations for patient selection: prepectoral versus subpectoral implant-based breast reconstruction. Arch Plast Surg 46(6):550–557
Gurunluoglu R, Gurunluoglu A, Williams SA, Tebockhorst S (2013) Current trends in breast reconstruction survey of American society of plastic surgeons 2010. Ann Plast Surg 70(1):103–110
Breuing KH, Warren SM (2005) Immediate bilateral breast reconstruction with implants and inferolateral AlloDerm slings. Ann Plast Surg 55(3):232–239
Zienowicz RJ, Karacaoglu E (2007) Implant-based breast reconstruction with allograft. Plast Reconstr Surg 120(2):373–381
Spear SL, Parikh PM, Reisin E, Menon NG (2008) Acellular dermis-assisted breast reconstruction. Aesthet Plast Surg 32(3):418–425
Scheflan M, Allweis TM, Ben Yehuda D, Maisel Lotan A (2020) Meshed acellular dermal matrix in immediate prepectoral implant-based breast reconstruction. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/gox.0000000000003265,November25,2020
Sbitany H, Piper M, Lentz R (2017) Prepectoral breast reconstruction: a safe alternative to submuscular prosthetic reconstruction following nipple-sparing mastectomy. Plast Reconstr Surg 140(3):432–443
Forsberg CG, Kelly DA, Wood BC, Mastrangelo SL, DeFranzo AJ, Thompson JT, David LR, Marks MW (2014) Aesthetic outcomes of acellular dermal matrix in tissue expander/implant-based breast reconstruction. Ann Plast Surg 72(6):S116-120
Spear SL, Schwartz J, Dayan JH, Clemens MW (2009) Outcome assessment of breast distortion following submuscular breast augmentation. Aesthet Plast Surg 33(1):44–48
Nigro LC, Blanchet NP (2017) Animation deformity in postmastectomy implant-based reconstruction. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/gox.0000000000001407,July24,2017
Becker H, Fregosi N (2017) The Impact of animation deformity on quality of life in post-mastectomy reconstruction patients. Aesthet Surg J 37(5):531–536
Darrach H, Kraenzlin F, Khavanin N, Chopra K, Sacks JM (2019) The role of fat grafting in prepectoral breast reconstruction. Gland Surg 8(1):61–66
Ramos Boyero M (2008) Skin-sparing mastectomy: an alternative to conventional mastectomy in breast cancer. Cir Esp 84(4):181–187
Mallon P, Feron JG, Couturaud B, Fitoussi A, Lemasurier P, Guihard T, Cothier-Savay I, Reyal F (2013) The role of nipple-sparing mastectomy in breast cancer: a comprehensive review of the literature. Plast Reconstr Surg 131(5):969–984
Munabi NC, Olorunnipa OB, Goltsman D, Rohde CH, Ascherman JA (2014) The ability of intra-operative perfusion mapping with laser-assisted indocyanine green angiography to predict mastectomy flap necrosis in breast reconstruction: a prospective trial. J Plast Reconstr Aesthet Surg 67(4):449–455
Vidya R, Iqbal FM (2017) A guide to prepectoral breast reconstruction: a new dimension to implant-based breast reconstruction. Clin Breast Cancer 17(4):266–271
Bernini M, Calabrese C, Cecconi L, Santi C, Gjondedaj U, Roselli J, Nori J, Fausto A, Orzalesi L, Casella D (2015) Subcutaneous direct-to-implant breast reconstruction: surgical, functional, and aesthetic results after long-term follow-up. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/gox.0000000000000533,January7,2016
Ribuffo D, Berna G, De Vita R, Di Benedetto G, Cigna E, Greco M, Valdatta L, Onesti MG, Lo Torto F, Marcasciano M, Redi U, Quercia V, Kaciulyte J, Cherubino M, Losco L, Mori FLR, Scalise A (2021) Dual-plane retro-pectoral versus pre-pectoral DTI breast reconstruction: an Italian multicenter experience. Aesthet Plast Surg 45(1):51–60
Li L, Su Y, Xiu B, Huang X, Chi W, Hou J, Zhang Y, Tian J, Wang J, Wu J (2019) Comparison of prepectoral and subpectoral breast reconstruction after mastectomies: a systematic review and meta analysis. Eur J Surg Oncol 45(9):1542–1550
Wagner RD, Braun TL, Zhu HR, Winocour S (2019) A systematic review of complications in prepectoral breast reconstruction. J Plast Reconstr Aesthet Surg 72(7):1051–1059
Tasoulis MK, Iqbal FM, Cawthorn S, MacNeill F, Vidya R (2017) Subcutaneous implant breast reconstruction: time to reconsider? Eur J Surg Oncol 43(9):1636–1646
Hammond DC, Schmitt WP, O’Connor EA (2015) Treatment of breast animation deformity in implant-based reconstruction with pocket change to the subcutaneous position. Plast Reconstr Surg 135(6):1540–1544
Chun YS, Verma K, Rosen H, Lipsitz S, Morris D, Kenney P, Eriksson E (2010) Implant-based breast reconstruction using acellular dermal matrix and the risk of postoperative complications. Plast Reconstr Surg 125(2):429–436
Vardanian AJ, Clayton JL, Roostaeian J, Shirvanian V, Da Lio A, Lipa JE, Crisera C, Festekjian JH (2011) Comparison of implant-based immediate breast reconstruction with and without acellular dermal matrix. Plast Reconstr Surg 128(5):403e–410e
Mathew J (2021) Short- to medium-term outcome of prepectoral versus subpectoral direct-to-implant reconstruction using acellular dermal matrix. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/gox.0000000000003747,August5,2021
Kim IK, Park SO, Chang H, Jin US (2018) Inhibition mechanism of acellular dermal matrix on capsule formation in expander-implant breast reconstruction after postmastectomy radiotherapy. Ann Surg Oncol 25(8):2279–2287
Cheng A, Lakhiani C, Saint-Cyr M (2013) Treatment of capsular contracture using complete implant coverage by acellular dermal matrix: a novel technique. Plast Reconstr Surg 132(3):519–529
Spear SL, Seruya M, Clemens MW, Teitelbaum S, Nahabedian MY (2011) Acellular dermal matrix for the treatment and prevention of implant-associated breast deformities. Plast Reconstr Surg 127(3):1047–1058
Kaplan J, Wagner RD, Braun TL, Chu C, Winocour SJ (2019) Prepectoral breast reconstruction. Semin Plast Surg 33(4):236–239
Tomita K, Yano K, Nishibayashi A, Hosokawa K (2015) Effects of subcutaneous versus submuscular tissue expander placement on breast capsule formation. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/gox.0000000000000418,July8,2015
Li Y, Xu G, Yu N, Huang J, Long X (2020) Prepectoral versus subpectoral implant-based breast reconstruction: a meta-analysis. Ann Plast Surg 85(4):437–447
Wells GA, Shea BJ, O'Connell D, Peterson J, Welch V, Losos M, Tugwell P (2000) The Newcastle–Ottawa Scale (NOS) for assessing the quality of non-randomized studies in meta-analysis. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp
Kim JH, Hong SE (2020) A comparative analysis between subpectoral versus prepectoral single stage direct-to-implant breast reconstruction. Medicina (Kaunas). https://doi.org/10.3390/medicina56100537,October13,2020
Manrique OJ, Kapoor T, Banuelos J, Jacobson SR, Martinez-Jorge J, Nguyen MT, Tran NV, Harless CA, Degnim AC, Jakub JW (2020) Single-stage direct-to-implant breast reconstruction: a comparison between subpectoral versus prepectoral implant placement. Ann Plast Surg 84(4):361–365
Plachinski SJ, Boehm LM, Adamson KA, LoGiudice JA, Doren EL (2021) Comparative analysis of prepectoral versus subpectoral implant-based breast reconstruction. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/GOX.0000000000003709,July27,2021
Spear SL, Baker JL (1995) Classification of capsular contracture after prosthetic breast reconstruction. Plast Reconstr Surg 96(5):1119–1123
Siegel RL, Miller KD, Fuchs HE, Jemal AK (2021) Cancer statistics,2021. CA Cancer J Clin 71(1):7–33
Casella D, Di Taranto G, Marcasciano M, Sordi S, Kothari A, Kovacs T, Lo Torto F, Cigna E, Calabrese C, Ribuffo D (2019) Evaluation of prepectoral implant placement and complete coverage with TiLoop bra mesh for breast reconstruction: a prospective study on long-term and patient-reported BREAST-Q outcomes. Plast Reconstr Surg 143(1):1e–9e
Weichman KE, Wilson SC, Saadeh PB, Hazen A, Levine JP, Choi M, Karp NS (2013) Sterile “ready-to-use” AlloDerm decreases postoperative infectious complications in patients undergoing immediate implant-based breast reconstruction with acellular dermal matrix. Plast Reconstr Surg 132(4):725–736
Sorkin M, Qi J, Kim HM, Hamill JB, Kozlow JH, Pusic AL, Wilkins EG (2017) Acellular dermal matrix in immediate expander/implant breast reconstruction: a multicenter assessment of risks and benefits. Plast Reconstr Surg 140(6):1091–1100
Baker BG, Irri R, MacCallum V, Chattopadhyay R, Murphy J, Harvey JR (2018) A prospective comparison of short-term outcomes of subpectoral and prepectoral strattice-based immediate breast reconstruction. Plast Reconstr Surg 141(5):1077–1084
Nahabedian MY, Cocilovo C (2017) Two-stage prosthetic breast reconstruction: a comparison between prepectoral and partial subpectoral techniques. Plast Reconstr Surg 140(6):22S-30S
Calobrace MB, Stevens WG, Capizzi PJ, Cohen R, Godinez T, Beckstrand M (2018) Risk factor analysis for capsular contracture: a 10-year Sientra study using round, smooth, and textured implants for breast augmentation. Plast Reconstr Surg 141(4S):20S-28S
Biggs TM, Yarish RS (1990) Augmentation mammaplasty: a comparative analysis. Plast Reconstr Surg 85(3):368–372
Schlenker JD, Bueno RA, Ricketson G, Lynch JB (1978) Loss of silicone implants after subcutaneous mastectomy and reconstruction. Plast Reconstr Surg 62(6):853–861
Puckett CL, Croll GH, Reichel CA, Concannon MJ (1987) A critical look at capsule contracture in subglandular versus subpectoral mammary augmentation. Aesthet Plast Surg 11(1):23–28
Zhu L, Mohan AT, Abdelsattar JM, Wang Z, Vijayasekaran A, Hwang SM, Tran NV, Saint-Cyr M (2016) Comparison of subcutaneous versus submuscular expander placement in the first stage of immediate breast reconstruction. J Plast Reconstr Aesthet Surg 69(4):e77-86
Ho G, Nguyen TJ, Shahabi A, Hwang BH, Chan LS, Wong AK (2012) A systematic review and meta-analysis of complications associated with acellular dermal matrix-assisted breast reconstruction. Ann Plast Surg 68(4):346–356
Ksander GA, Gray L (1985) Reduced capsule formation around soft silicone rubber prostheses coated with solid collagen. Ann Plast Surg 14(4):351–360
Komorowska-Timek E, Oberg KC, Timek TA, Gridley DS, Miles DAG (2009) The effect of AlloDerm envelopes on periprosthetic capsule formation with and without radiation. Plast Reconstr Surg 123(3):807–816
Basu CB, Leong M, Hicks MJ (2010) Acellular cadaveric dermis decreases the inflammatory response in capsule formation in reconstructive breast surgery. Plast Reconstr Surg 126(6):1842–1847
Stump A, Holton LH 3rd, Connor J, Harper JR, Slezak S, Silverman RP (2009) The use of acellular dermal matrix to prevent capsule formation around implants in a primate model. Plast Reconstr Surg 124(1):82–91
Liu J, Hou J, Li Z, Wang B, Sun J (2020) Efficacy of acellular dermal matrix in capsular contracture of implant-based breast reconstruction: a single-arm meta-analysis. Aesthet Plast Surg 44(3):735–742
Highton L, Johnson R, Kirwan C, Murphy J (2017) Prepectoral implant-based breast reconstruction. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/gox.0000000000001488,September19,2017
Nealon KP, Weitzman RE, Sobti N, Gadd M, Specht M, Jimenez RB, Ehrlichman R, Faulkner HR, Austen WG, Liao EC (2020) Prepectoral direct-to-implant breast reconstruction: safety outcome endpoints and delineation of risk factors. Plast Reconstr Surg 145(5):E898–E908
Marques M, Brown SA, Oliveira I, Mnds C, Morales-Helguera A, Rodrigues A, Amarante J (2010) Long-term follow-up of breast capsule contracture rates in cosmetic and reconstructive cases. Plast Reconstr Surg 126(3):769–778
Acknowledgements
This research was supported by CAMS Innovation Fund for Medical Sciences (CIFMS) (No. 2020-I2M-C&T-B-082) to Dr. Chunjun Liu.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial interests relating to the work described and declare no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, L., Liu, C. Postoperative Complications Following Prepectoral Versus Partial Subpectoral Implant-Based Breast Reconstruction Using ADM: A Systematic Review and Meta-analysis. Aesth Plast Surg 47, 1260–1273 (2023). https://doi.org/10.1007/s00266-023-03296-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03296-0