Abstract
Objective
To help surgical trainees reach a deep understanding of plastic operations, we developed and evaluated an economical and convenient model using plasticine for plastic surgical training.
Methods
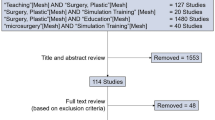
From Sep of 2012 to Dec of 2014, we invited 57 medical interns to participate in a program designed for the qualitative evaluation of this model. In this program, 57 interns were asked to simulate certain surgical operations under guidance of the experienced staff of our department using the plasticine model. The value of the plasticine model was evaluated through questionnaire surveys. Their acceptance of the plasticine model, as well as the benefits and the flaws, was evaluated by the questionnaire survey.
Results
All the participants completed the training session as well as the questionnaire, all of whom felt that the plasticine model had increased their familiarity with the surgical procedure they were assigned. By remodeling plasticine, the trainees understood either the brief surgical procedures or some confusing operative details in plastic surgery. In the questionnaire surveys, the trainees showed considerable consensus with the training program. The flaws of this method were also listed. The flaws generally reflected that “it is difficult to model into a vivid image” and “it is not suitable for all the operation”.
Conclusions
Overall, the plasticine model is accepted by the participants in this survey. This model is economical and versatile, and could be used as a complementary training tool for novices in simulated operation training of plastic surgery.
No Level Assigned
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.









Similar content being viewed by others
References
Reznick RK, MacRae H (2006) Teaching surgical skills—changes in the wind. N Engl J Med 355(25):2664–2669
Ji C, Zhang J, Liang W, Pan S, Chen Y, Zhang J, Yao Y (2014) Correcting glanular dislocation in hypospadias with up-to-tip technique and double wing flaps. Ann Plast Surg. (Epub ahead of print)
Bucher L (1991) Evaluating the affective domain. Consider a Likert scale. J Nurses Staff Dev 7(5):234–238
Jabbour N, Dobratz EJ, Dresner HS, Hilger PA (2011) Assessing fundamental 2-dimensional understanding of basic soft tissue techniques. J Surg Educ 68(3):178–184
Pieper SD, Laub DR Jr, Rosen JM (1995) A finite-element facial model for simulating plastic surgery. Plast Reconstr Surg 96(5):1100–1105
Schendel S, Montgomery K, Sorokin A, Lionetti G (2005) A surgical simulator for planning and performing repair of cleft lips. J Craniomaxillofacial Surg 33(4):223–228
Loh CY, Gunn E, Pennell DJ, Athanassopoulos T (2014) Pinnaplasty: a porcine training model. J Plast Reconstr Aesthet Surg 67(6):868–869
García JMM, Da Costa ASA, Schmitz TR, Estomba CMC, Zavarce MIH (2014) Temporal bone dissection practice using a chicken egg. Otol Neurotol 35(6):941–943
Morani AD (1992) Art in medical education: especially plastic surgery. Aesthet Plast Surg 16(3):213–218
Fitts PM, Posner MI (1967) Human performance. Brooks/Cole, Belmont
Yang B, Zhang ZS, Xiao L, Wang LH, Xu CL, Sun YH (2010) A novel training model for retroperitoneal laparoscopic dismembered pyeloplasty. J Endourol 24(8):1345–1349
Gadzhiev N, Brovkin S, Grigoryev V, Tagirov N, Korol V, Petrov S (2014) Sculpturing in urology, or how to make percutaneous nephrolithotomy easier. J Endourol. (Epub ahead of print)
Röhrich E, Thali M, Schweitzer W (2012) Skin injury model classification based on shape vector analysis. BMC Med Imaging 6(12):32
Yang Y, Paton NI (2005) Laser scanning as a tool for assessment of HIV-related facial lipoatrophy: evaluation of accuracy and reproducibility. HIV Med 6(5):321–325
Liang YH, Yuan M, Li G, Shemesh H, Wesselink PR, Wu MK (2012) The ability of cone-beam computed tomography to detect simulated buccal and lingual recesses in root canals. Int Endod J 45(8):724–729
Ang ET, Sugand K, Hartman M, Seow CS, Bay BH, Abrahams P (2012) Singapore’s anatomical future: quovadis? Anat Sci Educ 5(4):234–240
Krontiris-Litowitz J (2003) Using manipulatives to improve learning in the undergraduate neurophysiology curriculum. Adv Physiol Educ 27(1–4):109–119
Acknowledgments
This work has no sources of financial support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Ji, C., Li, R., Liang, W. et al. Plasticine Model: An Useful Surgical Training in Plastic Surgery. Aesth Plast Surg 40, 174–181 (2016). https://doi.org/10.1007/s00266-015-0602-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-015-0602-9