Abstract
Purpose
We aimed to compare outcomes in patients that underwent bilateral anatomic total shoulder arthroplasty (aTSA) vs. aTSA/ reverse total shoulder arthroplasty (rTSA) for rotator cuff-intact glenohumeral osteoarthritis (RCI-GHOA) to further elucidate the role of rTSA in this patient population.
Methods
A single-institution prospectively collected shoulder arthroplasty database was reviewed for patients undergoing bilateral total shoulder arthroplasty (TSA) for RCI-GHOA with a primary aTSA and subsequent contralateral aTSA or rTSA. Outcome scores (SPADI, SST, ASES, UCLA, Constant) and active range of motion (abduction, forward elevation [FE], external and internal rotation [ER and IR]) were evaluated. Clinically relevant benchmarks (minimal clinically important difference [MCID], substantial clinical benefit [SCB], and patient acceptable symptomatic state [PASS]) were evaluated against values in prior literature. Incidence of surgical complications and revision rates were examined in qualifying patients as well as those without <two year follow-up.
Results
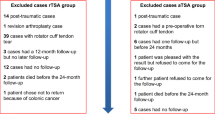
Of the 55 bilateral TSA patients with an intact rotator cuff, 46 underwent aTSA/aTSA and 9 underwent aTSA/rTSA. At the time of the second TSA, patients undergoing aTSA/rTSA were older (71 ± 4 vs. 67 ± 7, P = .032) and more commonly had inflammatory arthritis (44% vs. 11%, P = .031). Mean time to the second TSA was shorter for aTSA/aTSA (2.3 ± 2.8 vs. 4.4 ± 3.6 years, P < .001). Postoperative outcomes were similar after the first aTSAs between groups with similar proportions achieving the MCID, SCB, and PASS (all P > .05). The 2nd TSAs between groups were similar preoperatively, but aTSA/rTSA had superior outcome scores, overhead motion, and active abduction compared to patients that underwent aTSA/aTSA. There were no differences in active ER and IR scores or complication rates between groups.
Conclusion
Patients with RCI-GHOA have excellent clinical outcomes after either aTSA/aTSA or aTSA/rTSA.
Similar content being viewed by others
Data Availability
The data set generated during the current study will be available from the corresponding author upon reasonable request.
References
Friedman RJ, Schoch BS, Eichinger JK et al (2022) Comparison of reverse and anatomic total shoulder arthroplasty in patients with an intact rotator cuff and no previous surgery. J Am Acad Orthop Surg 30:941–948. https://doi.org/10.5435/JAAOS-D-22-00014
Hao KA, Greene AT, Werthel JD, Wright JO, King JJ, Wright TW, Vasilopoulos T, Schoch BS (2023) Clinical outcomes of anatomic versus reverse total shoulder arthroplasty in primary osteoarthritis with preoperative rotational stiffness and an intact rotator cuff: a case control study. J Shoulder Elbow Surg 32(7):e355–e365. https://doi.org/10.1016/j.jse.2022.12.027
Haritinian E-G, Belgaid V, Lino T, Nové-Josserand L (2020) Reverse versus anatomical shoulder arthroplasty in patients with intact rotator cuff. Int Orthop 44:2395–2405. https://doi.org/10.1007/s00264-020-04754-z
Kim H, Kim C-H, Kim M et al (2022) Is reverse total shoulder arthroplasty (rTSA) more advantageous than anatomic TSA (aTSA) for osteoarthritis with intact cuff tendon? A systematic review and meta-analysis. J Orthop Traumatol 23:3. https://doi.org/10.1186/s10195-022-00625-y
Wright MA, Keener JD, Chamberlain AM (2020) Comparison of clinical outcomes after anatomic total shoulder arthroplasty and reverse shoulder arthroplasty in patients 70 years and older with glenohumeral osteoarthritis and an intact rotator cuff: J Am Acad Orthop Surg 28:e222–e229. https://doi.org/10.5435/JAAOS-D-19-00166
Schoch BS, Tams C, Eichinger J et al (2020) Anatomic total shoulder arthroplasty after healed rotator cuff repair: a matched cohort. J Shoulder Elbow Surg 29:2221–2228. https://doi.org/10.1016/j.jse.2020.03.029
Milgrom C, Schaffler M, Gilbert S, van Holsbeeck M (1995) Rotator-cuff changes in asymptomatic adults. The effect of age, hand dominance and gender. J Bone Joint Surg Br 77:296–298
Yamaguchi K, Ditsios K, Middleton WD et al (2006) The demographic and morphological features of rotator cuff disease: a comparison of asymptomatic and symptomatic shoulders. J Bone Jt Surg 88:1699–1704. https://doi.org/10.2106/JBJS.E.00835
Yanik EL, Colditz GA, Wright RW et al (2020) Risk factors for surgery due to rotator cuff disease in a population-based cohort. Bone Jt J 102-B:352–359. https://doi.org/10.1302/0301-620X.102B3.BJJ-2019-0875.R1
Keener JD, Patterson BM, Orvets N, Chamberlain AM (2019) Degenerative rotator cuff tears: refining surgical indications based on natural history data. J Am Acad Orthop Surg 27:156–165. https://doi.org/10.5435/JAAOS-D-17-00480
Heifner JJ, Kumar AD, Wagner ER (2021) Glenohumeral osteoarthritis with intact rotator cuff treated with reverse shoulder arthroplasty: a systematic review. J Shoulder Elbow Surg 30:2895–2903. https://doi.org/10.1016/j.jse.2021.06.010
Walters JD, Denard PJ, Brockmeier SF, Werner BC (2021) The relationship of bilateral shoulder arthroplasty timing and postoperative complications. J Shoulder Elbow Surg 30:317–323. https://doi.org/10.1016/j.jse.2020.06.010
Levy O, Walecka J, Arealis G et al (2017) Bilateral reverse total shoulder arthroplasty—functional outcome and activities of daily living. J Shoulder Elbow Surg 26:e85–e96. https://doi.org/10.1016/j.jse.2016.09.010
Malahias M-A, Brilakis E, Chytas D et al (2019) Functional outcomes of bilateral reverse total shoulder arthroplasty: a systematic review. Joints 7:188–198. https://doi.org/10.1055/s-0041-1730974
Stevens CG, Struk AM, Wright TW (2014) The functional impact of bilateral reverse total shoulder arthroplasty. J Shoulder Elbow Surg 23:1341–1348. https://doi.org/10.1016/j.jse.2013.12.012
Flurin P-H, Marczuk Y, Janout M et al (2013) (2013) Comparison of outcomes using anatomic and reverse total shoulder arthroplasty. Bull Hosp Jt Dis 71(2):101–107
Roche C, Kumar V, Overman S et al (2021) Validation of a machine learning–derived clinical metric to quantify outcomes after total shoulder arthroplasty. J Shoulder Elbow Surg 30:2211–2224. https://doi.org/10.1016/j.jse.2021.01.021
Simovitch R, Flurin P-H, Wright T et al (2018) Quantifying success after total shoulder arthroplasty: the minimal clinically important difference. J Shoulder Elbow Surg 27:298–305. https://doi.org/10.1016/j.jse.2017.09.013
Simovitch R, Flurin P-H, Wright T et al (2018) Quantifying success after total shoulder arthroplasty: the substantial clinical benefit. J Shoulder Elbow Surg 27:903–911. https://doi.org/10.1016/j.jse.2017.12.014
Gerber C, Pennington SD, Nyffeler RW (2009) Reverse total shoulder arthroplasty. J Am Acad Orthop Surg 17:284–295. https://doi.org/10.5435/00124635-200905000-00003
Chalmers PN, Keener JD (2016) Expanding roles for reverse shoulder arthroplasty. Curr Rev Musculoskelet Med 9:40–48. https://doi.org/10.1007/s12178-016-9316-0
Parada SA, Flurin P-H, Wright TW et al (2021) Comparison of complication types and rates associated with anatomic and reverse total shoulder arthroplasty. J Shoulder Elbow Surg 30:811–818. https://doi.org/10.1016/j.jse.2020.07.028
Steen BM, Cabezas AF, Santoni BG et al (2015) Outcome and value of reverse shoulder arthroplasty for treatment of glenohumeral osteoarthritis: a matched cohort. J Shoulder Elbow Surg 24:1433–1441. https://doi.org/10.1016/j.jse.2015.01.005
Latif V, Denard PJ, Young AA et al (2012) Bilateral anatomic total shoulder arthroplasty versus reverse shoulder arthroplasty. Orthopedics 35:e479-485. https://doi.org/10.3928/01477447-20120327-25
Cox RM, Padegimas EM, Abboud JA et al (2018) Outcomes of an anatomic total shoulder arthroplasty with a contralateral reverse total shoulder arthroplasty. J Shoulder Elbow Surg 27:998–1003. https://doi.org/10.1016/j.jse.2017.12.005
Mellano CR, Kupfer N, Thorsness R et al (2017) Functional results of bilateral reverse total shoulder arthroplasty. J Shoulder Elbow Surg 26:990–996. https://doi.org/10.1016/j.jse.2016.10.011
Saini SS, Pettit R, Puzzitiello RN et al (2022) Clinical outcomes after reverse total shoulder arthroplasty in patients with primary glenohumeral osteoarthritis compared with rotator cuff tear arthropathy: does preoperative diagnosis make a difference? J Am Acad Orthop Surg 30:e415–e422. https://doi.org/10.5435/JAAOS-D-21-00797
Acknowledgements
None.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Dr. LMT, KAH, and Dr. JJK. The first draft of the manuscript was written by Dr. LMT and VEB, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The University of Florida Institutional Review Board (IRB) has approved this study as exempt (IRB#: 202201657).
Competing interests
Mr. Hao is a paid consultant for LinkBio Corp. Dr. Schoch receives royalties from Exactech, Innomed and Responsive Arthroscopy. Dr. King is a paid consultant for Exactech, Inc. and LinkBio Corp. Dr. Farmer is a paid consultant for Exactech, Inc. and Arthrex. Dr. Wright is a paid consultant and receives royalties from Exactech, Inc. The other authors, their immediate families, and any research foundations with which they are affiliated have not received any financial payments or other benefits from any commercial entity related to the subject of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Turnbull, L.M., Hao, K.A., Bindi, V.E. et al. Anatomic versus reverse total shoulder arthroplasty outcomes after prior contralateral anatomic total shoulder arthroplasty in patients with bilateral primary osteoarthritis with an intact rotator cuff. International Orthopaedics (SICOT) 48, 801–807 (2024). https://doi.org/10.1007/s00264-023-06044-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-06044-w