Abstract
Purpose
To analyze ROM changes by using a Bayesian method, to compare complication and re-operation rates between open osteocapsular arthroplasty (OPEN) and arthroscopic osteocapsular arthroplasty (ARTHRO) for primary osteoarthritis of the elbow, and find evidence-based tendencies.
Methods
The PubMed, Cochrane Library, and Embase databases were searched. We performed descriptive analysis to compare ARTHRO and OPEN, a Bayesian analysis of ROM changes, and methodological assessment to determine the tendencies of OPEN and ARTHRO.
Results
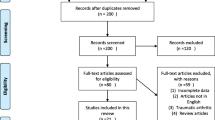
Eighteen articles (625 patients, 634 elbows) were analyzed. There were 11 articles on OPEN and 8 articles on ARTHRO (1 article was a comparative study between OPEN and ARTHRO). According to the Bayesian method, flexion and total arc of flexion-extension increased more with OPEN than with ARTHRO. Further, ARTHRO showed a narrower width in the ROM graph than OPEN. The number of complications was 17 (5.1%) and five (2.0%), and the number of re-operations was 32 (9.5%) and 14 (5.6%) for OPEN and ARTHRO, respectively. By analyzing six high-quality articles, we found three tendencies: OPEN and ARTHRO were both effective for improving pain score, flexion-extension arc, and functional outcome; OPEN did not improve the pronation-supination arc; and there was a weak tendency that OPEN was more effective than ARTHRO for improving the flexion arc.
Conclusion
Both OPEN and ARTHRO improved ROM and clinical scores. The Bayesian method indicated that although OPEN increased the flexion and flexion-extension arc more than ARTHRO, ARTHRO resulted in a relatively consistent surgical outcome. Additionally, OPEN caused relatively higher complication and re-operation rates than ARTHRO.





Similar content being viewed by others
References
Stanley D (1994) Prevalence and etiology of symptomatic elbow osteoarthritis. J Shoulder Elb Surg 3:386–389. https://doi.org/10.1016/s1058-2746(09)80024-4
Gramstad GD, Galatz LM (2006) Management of elbow osteoarthritis. J Bone Joint Surg Am 88:421–430. https://doi.org/10.2106/jbjs.E.00568
Cheung EV, Adams R, Morrey BF (2008) Primary osteoarthritis of the elbow: current treatment options. J Am Acad Orthop Surg 16:77–87. https://doi.org/10.5435/00124635-200802000-00005
Gay DM, Lyman S, Do H, Hotchkiss RN, Marx RG, Daluiski A (2012) Indications and reoperation rates for total elbow arthroplasty: an analysis of trends in New York state. J Bone Joint Surg Am 94:110–117. https://doi.org/10.2106/JBJS.J.01128
Kodama A, Mizuseki T, Adachi N (2018) Macroscopic investigation of failed Kudo type 5 total elbow arthroplasty. J Shoulder Elb Surg 27:1380–1385. https://doi.org/10.1016/j.jse.2018.05.002
Katolik LI (2011) Osteocapsular debridement for elbow arthritis. Hand Clin 27:165–170. https://doi.org/10.1016/j.hcl.2011.03.001
Wada T, Isogai S, Ishii S, Yamashita T (2004) Debridement arthroplasty for primary osteoarthritis of the elbow. J Bone Joint Surg Am 86:233–241. https://doi.org/10.2106/00004623-200402000-00004
Kashiwagi D (1978) Intra-articular changes of the osteoarthritic elbow, especially about the fossa olecrani. Journal of the Japanese Orthopaedic Association 52:1367–1382
Morrey BF (1992) Primary degenerative arthritis of the elbow. Treatment by ulnohumeral arthroplasty J Bone Joint Surg Br 74:409–413. https://doi.org/10.1302/0301-620X.74B3.1587890
Tsuge K, Murakami T, Yasunaga Y, Kanaujia RR (1987) Arthroplasty of the elbow. Twenty years' experience of a new approach J Bone Joint Surg Br 69:116–120. https://doi.org/10.1302/0301-620X.69B1.3818716
Oka Y (2000) Debridement arthroplasty for osteoarthrosis of the elbow: 50 patients followed mean 5 years. Acta Orthop Scand 71:185–190. https://doi.org/10.1080/000164700317413175
Tsuge K, Mizuseki T (1994) Debridement arthroplasty for advanced primary osteoarthritis of the elbow. Results of a new technique used for 29 elbows. J Bone Joint Surg Br 76:641–646. https://doi.org/10.1302/0301-620x.76b4.8027156
Minami M, Kato S, Kashiwagi D (1996) Outerbridge-Kashiwagi's method for arthroplasty of osteoarthritis of the elbow — 44 elbows followed for 8–16 years. J Orthop Sci 1:11–15. https://doi.org/10.1007/BF01234111
Antuna SA, Morrey BF, Adams RA, O'Driscoll SW (2002) Ulnohumeral arthroplasty for primary degenerative arthritis of the elbow: long-term outcome and complications. J Bone Joint Surg Am 84:2168–2173. https://doi.org/10.2106/00004623-200212000-00007
Phillips NJ, Ali A, Stanley D (2003) Treatment of primary degenerative arthritis of the elbow by ulnohumeral arthroplasty. A long-term follow-up J Bone Joint Surg Br 85:347–350. https://doi.org/10.1302/0301-620x.85b3.13201
Tashjian RZ, Wolf JM, Ritter M, Weiss AP, Green A (2006) Functional outcomes and general health status after ulnohumeral arthroplasty for primary degenerative arthritis of the elbow. J Shoulder Elb Surg 15:357–366. https://doi.org/10.1016/j.jse.2005.08.004
Rettig LA, Hastings H 2nd, Feinberg JR (2008) Primary osteoarthritis of the elbow: lack of radiographic evidence for morphologic predisposition, results of operative debridement at intermediate follow-up, and basis for a new radiographic classification system. J Shoulder Elb Surg 17:97–105. https://doi.org/10.1016/j.jse.2007.03.014
Hattori Y, Doi K, Sakamoto S, Hoshino S, Dodakundi C (2011) Capsulectomy and debridement for primary osteoarthritis of the elbow through a medial trans-flexor approach. J Hand Surg Am 36:1652–1658. https://doi.org/10.1016/j.jhsa.2011.07.018
Cha SM, Shin HD, Kim KC, Park IY (2014) Outcomes of the mini-open Outerbridge-Kashiwagi procedure according to preoperative radiocapitellar joint status. J Hand Surg Am 39:209–218. https://doi.org/10.1016/j.jhsa.2013.10.016
Forster MC, Clark DI, Lunn PG (2001) Elbow osteoarthritis: prognostic indicators in ulnohumeral debridement--the Outerbridge-Kashiwagi procedure. J Shoulder Elb Surg 10:557–560. https://doi.org/10.1067/mse.2001.118416
Sarris I, Riano FA, Goebel F, Goitz RJ, Sotereanos DG (2004) Ulnohumeral arthroplasty: results in primary degenerative arthritis of the elbow. Clin Orthop Relat Res 420:190–193. https://doi.org/10.1097/00003086-200403000-00026
Ugurlu M, Senkoylu A, Ozsoy H, Demirkale I, Kilicarslan K, Dogan M (2009) Outcome of ulnohumeral arthroplasty in osteoarthritis of the elbow. Acta Orthop Belg 75:606–610
Redden JF, Stanley D (1993) Arthroscopic fenestration of the olecranon fossa in the treatment of osteoarthritis of the elbow. Arthroscopy 9:14–16. https://doi.org/10.1016/s0749-8063(05)80337-8
Ogilvie-Harris DJ, Gordon R, MacKay M (1995) Arthroscopic treatment for posterior impingement in degenerative arthritis of the elbow. Arthroscopy 11:437–443. https://doi.org/10.1016/0749-8063(95)90198-1
Krishnan SG, Harkins DC, Pennington SD, Harrison DK, Burkhead WZ (2007) Arthroscopic ulnohumeral arthroplasty for degenerative arthritis of the elbow in patients under fifty years of age. J Shoulder Elb Surg 16:443–448. https://doi.org/10.1016/j.jse.2006.09.001
Adams JE, Wolff LH 3rd, Merten SM, Steinmann SP (2008) Osteoarthritis of the elbow: results of arthroscopic osteophyte resection and capsulectomy. J Shoulder Elb Surg 17:126–131. https://doi.org/10.1016/j.jse.2007.04.005
Kovachevich R, Steinmann SP (2012) Arthroscopic ulnar nerve decompression in the setting of elbow osteoarthritis. J Hand Surg Am 37:663–668. https://doi.org/10.1016/j.jhsa.2012.01.003
MacLean SB, Oni T, Crawford LA, Deshmukh SC (2013) Medium-term results of arthroscopic debridement and capsulectomy for the treatment of elbow osteoarthritis. J Shoulder Elb Surg 22:653–657. https://doi.org/10.1016/j.jse.2013.01.030
Lim TK, Koh KH, Lee HI, Shim JW, Park MJ (2014) Arthroscopic debridement for primary osteoarthritis of the elbow: analysis of preoperative factors affecting outcome. J Shoulder Elb Surg 23:1381–1387. https://doi.org/10.1016/j.jse.2014.01.009
Kim SJ, Kim JW, Lee SH, Choi JW (2017) Retrospective comparative analysis of elbow arthroscopy used to treat primary osteoarthritis with and without release of the posterior band of the medial collateral ligament. Arthroscopy 33:1506–1511. https://doi.org/10.1016/j.arthro.2017.02.013
Ozbaydar MU, Tonbul M, Altan E, Yalaman O (2006) Arthroscopic treatment of symptomatic loose bodies in osteoarthritic elbows. Acta Orthop Traumatol Turc 40:371–376
Yan H, Cui GQ, Wang JQ, Yin Y, Ao YF (2011) Arthroscopic debridement of osteoarthritic elbow in professional athletes. Chin Med J 124:4223–4228. https://doi.org/10.3760/cma.j.issn.0366-6999.2011.24.019
Merolla G, Buononato C, Chillemi C, Paladini P, Porcellini G (2015) Arthroscopic joint debridement and capsular release in primary and post-traumatic elbow osteoarthritis: a retrospective blinded cohort study with minimum 24-month follow-up. Musculoskelet Surg 99(Suppl 1):S83–S90. https://doi.org/10.1007/s12306-015-0365-0
McLaughlin RE 2nd, Savoie FH 3rd, Field LD, Ramsey JR (2006) Arthroscopic treatment of the arthritic elbow due to primary radiocapitellar arthritis. Arthroscopy 22:63–69. https://doi.org/10.1016/j.arthro.2005.10.013
Kelly EW, Bryce R, Coghlan J, Bell S (2007) Arthroscopic debridement without radial head excision of the osteoarthritic elbow. Arthroscopy 23:151–156. https://doi.org/10.1016/j.arthro.2006.10.008
Bornu BC, Clement X, Kempf JF, Clavert P (2015) Arthroscopic elbow joint release with radial head resection arthroplasty: 12 cases. Orthop Traumatol Surg Res 101:735–739. https://doi.org/10.1016/j.otsr.2015.07.009
Kwak JM, Kholinne E, Sun Y, Lim S, Koh KH, Jeon IH (2019) Clinical outcome of osteocapsular arthroplasty for primary osteoarthritis of the elbow: comparison of arthroscopic and open procedure. Arthroscopy 35:1083–1089. https://doi.org/10.1016/j.arthro.2018.11.057
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716. https://doi.org/10.1046/j.1445-2197.2003.02748.x
Huisstede BM, Miedema HS, van Opstal T et al (2006) Interventions for treating the posterior interosseus nerve syndrome: a systematic review of observational studies. J Peripher Nerv Syst 11:101–110. https://doi.org/10.1111/j.1085-9489.2006.00074.x
Escobar MD, West M (1995) Bayesian density estimation and inference using mixtures. J Am Stat Assoc 90:577–588. https://doi.org/10.1080/01621459.1995.10476550
Neal RM (2000) Markov chain sampling methods for Dirichlet process mixture models. J Comput Graph Stat 9:249–265. https://doi.org/10.1080/10618600.2000.10474879
Jara A, Hanson TE, Quintana FA, Müller P, Rosner GL (2011) DPpackage: Bayesian non- and semi-parametric Modelling in R. J Stat Softw 40:1–30
Kodde IF, van Rijn J, van den Bekerom MP, Eygendaal D (2013) Surgical treatment of post-traumatic elbow stiffness: a systematic review. J Shoulder Elb Surg 22:574–580. https://doi.org/10.1016/j.jse.2012.11.010
Funding
Each author certifies that he has no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Preparation of methods and data collection were performed by Dong Min Kim, Minkyu Han, and Myung Jin Shin. Data analysis was mainly performed by Minkyu Han and In-Ho Jeon. The first draft of the manuscript was written by Dong Min Kim, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest in relation to this paper.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, D.M., Han, M., Jeon, IH. et al. Range-of-motion improvement and complication rate in open and arthroscopic osteocapsular arthroplasty for primary osteoarthritis of the elbow: a systematic review. International Orthopaedics (SICOT) 44, 329–339 (2020). https://doi.org/10.1007/s00264-019-04458-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-019-04458-z