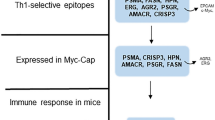
Abstract
Antibody responses to off-target cancer-associated proteins have been detected following immunotherapies for cancer, suggesting these may be the result of antigen spread. We have previously reported that serum antibodies to prostate cancer-associated proteins were detectable using a high-throughput peptide array. We hypothesized that the breadth of antibody responses elicited by a vaccine could serve as a measure of the magnitude of its induced antigen spread. Consequently, sera from patients with prostate cancer, treated prior to or after vaccination in one of four separate clinical trials, were evaluated for antibody responses to an array of 177,604 peptides derived from over 1600 prostate cancer-associated gene products. Antibody responses to the same group of 5680 peptides previously reported were identified following vaccinations in which patients were administered GM-CSF as an adjuvant, but not with vaccine in the absence of GM-CSF. Hence, antibody responses to off-target proteins following vaccination may not necessarily serve as evidence of antigen spread and must be interpreted with particular caution following vaccine strategies that use GM-CSF, as GM-CSF appears to have direct effects on the production of antibodies. The evaluation of T cell responses to non-target antigens is likely a preferred approach for detection of immune-mediated antigen spread.




Similar content being viewed by others
References
Gulley JL, Madan RA, Pachynski R, Mulders P, Sheikh NA, Trager J, Drake CG (2017) Role of antigen spread and distinctive characteristics of immunotherapy in cancer treatment. J Natl Cancer Inst. https://doi.org/10.1093/jnci/djw261
Brossart P, Wirths S, Stuhler G, Reichardt VL, Kanz L, Brugger W (2000) Induction of cytotoxic T-lymphocyte responses in vivo after vaccinations with peptide-pulsed dendritic cells. Blood 96:3102–3108
Ribas A, Glaspy JA, Lee Y et al (2004) Role of dendritic cell phenotype, determinant spreading, and negative costimulatory blockade in dendritic cell-based melanoma immunotherapy. J Immunother 27:354–367. https://doi.org/10.1097/00002371-200409000-00004
Butterfield LH, Ribas A, Dissette VB et al (2003) Determinant spreading associated with clinical response in dendritic cell-based immunotherapy for malignant melanoma. Clin Cancer Res 9:998–1008
Tuohy VK, Kinkel RP (2000) Epitope spreading: a mechanism for progression of autoimmune disease. Arch Immunol Ther Exp 48:347–351
Nesslinger NJ, Ng A, Tsang KY, Ferrara T, Schlom J, Gulley JL, Nelson BH (2010) A viral vaccine encoding prostate-specific antigen induces antigen spreading to a common set of self-proteins in prostate cancer patients. Clin Cancer Res 16:4046–4056
Smith HA, Maricque BB, Eberhardt J, Petersen B, Gulley JL, Schlom J, McNeel DG (2011) IgG responses to tissue-associated antigens as biomarkers of immunological treatment efficacy. J Biomed Biotech 2011:454861
Nguyen MC, Tu GH, Koprivnikar KE, Gonzalez-Edick M, Jooss KU, Harding TC (2010) Antibody responses to galectin-8, TARP and TRAP1 in prostate cancer patients treated with a GM-CSF-secreting cellular immunotherapy. Cancer Immunol Immunother 59:1313–1323. https://doi.org/10.1007/s00262-010-0858-5
GuhaThakurta D, Sheikh NA, Fan LQ et al (2015) Humoral immune response against non-targeted tumor antigens after treatment with sipuleucel-T and its association with improved clinical outcome. Clin Cancer Res. https://doi.org/10.1158/1078-0432.CCR-14-2334
Potluri HK, Ng TL, Newton MA, Zhang J, Maher CA, Nelson PS, McNeel DG (2020) Antibody profiling of patients with prostate cancer reveals differences in antibody signatures among disease stages. J Immunother Cancer. https://doi.org/10.1136/jitc-2020-001510
McNeel DG, Becker JT, Eickhoff JC et al (2014) Real-time immune monitoring to guide plasmid DNA vaccination schedule targeting prostatic acid phosphatase in patients with castration-resistant prostate cancer. Clin Cancer Res 20:3692–3704. https://doi.org/10.1158/1078-0432.ccr-14-0169
McNeel DG, Eickhoff JC, Johnson LE et al (2019) Phase II trial of a DNA vaccine encoding prostatic acid phosphatase (pTVG-HP [MVI-816]) in patients with progressive, nonmetastatic castration-sensitive prostate cancer. J Clin Oncol 37:3507–3517. https://doi.org/10.1200/JCO.19.01701
Kyriakopoulos CE, Eickhoff JC, Ferrari AC, Schweizer MT, Wargowski E, Olson BM, McNeel DG (2020) Multicenter phase I trial of a DNA vaccine encoding the androgen receptor ligand-binding domain (pTVG-AR, MVI-118) in patients with metastatic prostate cancer. Clin Cancer Res 26:5162–5171. https://doi.org/10.1158/1078-0432.CCR-20-0945
Wargowski E, Johnson LE, Eickhoff JC, Delmastro L, Staab MJ, Liu G, McNeel DG (2018) Prime-boost vaccination targeting prostatic acid phosphatase (PAP) in patients with metastatic castration-resistant prostate cancer (mCRPC) using Sipuleucel-T and a DNA vaccine. J Immunother Cancer 6:21. https://doi.org/10.1186/s40425-018-0333-y
Kumar A, Coleman I, Morrissey C et al (2016) Substantial interindividual and limited intraindividual genomic diversity among tumors from men with metastatic prostate cancer. Nat Med 22:369–378. https://doi.org/10.1038/nm.4053
Robinson D, Van Allen EM, Wu YM et al (2015) Integrative clinical genomics of advanced prostate cancer. Cell 162:454. https://doi.org/10.1016/j.cell.2015.06.053
Mishra N, Caciula A, Price A et al. (2018) Diagnosis of Zika virus infection by peptide array and enzyme-linked immunosorbent assay. mBio. 9. doi: https://doi.org/10.1128/mBio.00095-18
Lo KC, Sullivan E, Bannen RM et al (2020) Comprehensive profiling of the rheumatoid arthritis antibody repertoire. Arthritis Rheumatol 72:242–250. https://doi.org/10.1002/art.41089
Team RC (2019) R: a language and environment for statistical computing. R Foundation for Statistical Computing. https://www.R-project.org/.
Team R (2019) RStudio: integrated development environment for R. RStudio, Inc. https://www.rstudio.com.
Bates D, Machler M, Bolker B, Walker S (2015) Fitting linear mixed-effects models using lme4. J Stat Soft 67:1–48
Luke SG (2017) Evaluating significance in linear mixed-effects models in R. Behav Res Methods 49:1494–1502. https://doi.org/10.3758/s13428-016-0809-y
Kuznetsova A, Brockhoff PB, Christensen RHB (2017) ImerTest package: tests in linear mixed effects models. J Stat Soft 82:1–26
Dranoff G, Jaffee E, Lazenby A et al (1993) Vaccination with irradiated tumor cells engineered to secrete murine granulocyte-macrophage colony-stimulating factor stimulates potent, specific, and long-lasting anti-tumor immunity. Proc Natl Acad Sci U S A 90:3539–3543
Le DT, Picozzi VJ, Ko AH et al (2019) Results from a phase IIb, randomized, multicenter study of GVAX pancreas and CRS-207 compared with chemotherapy in adults with previously treated metastatic pancreatic adenocarcinoma (ECLIPSE study). Clin Cancer Res 25:5493–5502. https://doi.org/10.1158/1078-0432.CCR-18-2992
Nemunaitis J, Jahan T, Ross H et al (2006) Phase 1/2 trial of autologous tumor mixed with an allogeneic GVAX vaccine in advanced-stage non-small-cell lung cancer. Cancer Gene Ther 13:555–562. https://doi.org/10.1038/sj.cgt.7700922
Bendandi M, Gocke CD, Kobrin CB et al (1999) Complete molecular remissions induced by patient-specific vaccination plus granulocyte-monocyte colony-stimulating factor against lymphoma. Nat Med 5:1171–1177
Jager E, Ringhoffer M, Dienes HP et al (1996) Granulocyte-macrophage-colony-stimulating factor enhances immune responses to melanoma-associated peptides in vivo. Int J Cancer 67:54–62
Kusakabe K, Xin KQ, Katoh H et al (2000) The timing of GM-CSF expression plasmid administration influences the Th1/Th2 response induced by an HIV-1-specific DNA vaccine. J Immunol 164:3102–3111. https://doi.org/10.4049/jimmunol.164.6.3102
Choi KJ, Kim JH, Lee YS et al (2006) Concurrent delivery of GM-CSF and B7–1 using an oncolytic adenovirus elicits potent antitumor effect. Gene Ther 13:1010–1020. https://doi.org/10.1038/sj.gt.3302759
Slingluff CL Jr, Petroni GR, Olson WC et al (2009) Effect of granulocyte/macrophage colony-stimulating factor on circulating CD8+ and CD4+ T-cell responses to a multipeptide melanoma vaccine: outcome of a multicenter randomized trial. Clin Cancer Res 15:7036–7044
Burgess AW, Camakaris J, Metcalf D (1977) Purification and properties of colony-stimulating factor from mouse lung-conditioned medium. J Biol Chem 252:1998–2003
Sheng JR, Li L, Ganesh BB, Vasu C, Prabhakar BS, Meriggioli MN (2006) Suppression of experimental autoimmune myasthenia gravis by granulocyte-macrophage colony-stimulating factor is associated with an expansion of FoxP3+ regulatory T cells. J Immunol 177:5296–5306. https://doi.org/10.4049/jimmunol.177.8.5296
Gaudreau S, Guindi C, Menard M, Besin G, Dupuis G, Amrani A (2007) Granulocyte-macrophage colony-stimulating factor prevents diabetes development in NOD mice by inducing tolerogenic dendritic cells that sustain the suppressive function of CD4+CD25+ regulatory T cells. J Immunol 179:3638–3647. https://doi.org/10.4049/jimmunol.179.6.3638
Willart MA, Deswarte K, Pouliot P, Braun H, Beyaert R, Lambrecht BN, Hammad H (2012) Interleukin-1alpha controls allergic sensitization to inhaled house dust mite via the epithelial release of GM-CSF and IL-33. J Exp Med 209:1505–1517. https://doi.org/10.1084/jem.20112691
Mausberg AK, Jander S, Reichmann G (2009) Intracerebral granulocyte-macrophage colony-stimulating factor induces functionally competent dendritic cells in the mouse brain. Glia 57:1341–1350. https://doi.org/10.1002/glia.20853
Sorgi CA, Rose S, Court N et al (2012) GM-CSF priming drives bone marrow-derived macrophages to a pro-inflammatory pattern and downmodulates PGE2 in response to TLR2 ligands. PLoS ONE 7:e40523. https://doi.org/10.1371/journal.pone.0040523
Parajuli B, Sonobe Y, Kawanokuchi J, Doi Y, Noda M, Takeuchi H, Mizuno T, Suzumura A (2012) GM-CSF increases LPS-induced production of proinflammatory mediators via upregulation of TLR4 and CD14 in murine microglia. J Neuroinflammation 9:268. https://doi.org/10.1186/1742-2094-9-268
Shibata Y, Berclaz PY, Chroneos ZC, Yoshida M, Whitsett JA, Trapnell BC (2001) GM-CSF regulates alveolar macrophage differentiation and innate immunity in the lung through PU.1. Immunity 15:557–567. https://doi.org/10.1016/s1074-7613(01)00218-7
Sonderegger I, Iezzi G, Maier R, Schmitz N, Kurrer M, Kopf M (2008) GM-CSF mediates autoimmunity by enhancing IL-6-dependent Th17 cell development and survival. J Exp Med 205:2281–2294. https://doi.org/10.1084/jem.20071119
Harris RJ, Pettitt AR, Schmutz C, Sherrington PD, Zuzel M, Cawley JC, Griffiths SD (2000) Granulocyte-macrophage colony-stimulating factor as an autocrine survival factor for mature normal and malignant B lymphocytes. J Immunol 164:3887–3893. https://doi.org/10.4049/jimmunol.164.7.3887
Ni K, O’Neill HC (1992) Proliferation of the BCL1 B cell lymphoma induced by IL-4 and IL-5 is dependent on IL-6 and GM-CSF. Immunol Cell Biol 70(Pt 5):315–322. https://doi.org/10.1038/icb.1992.40
Snapper CM, Moorman MA, Rosas FR, Kehry MR, Maliszewski CR, Mond JJ (1995) IL-3 and granulocyte-macrophage colony-stimulating factor strongly induce Ig secretion by sort-purified murine B cell activated through the membrane Ig, but not the CD40, signaling pathway. J Immunol 154:5842–5850
McNeel DG, Dunphy EJ, Davies JG et al (2009) Safety and immunological efficacy of a DNA vaccine encoding prostatic acid phosphatase in patients with stage D0 prostate cancer. J Clin Oncol 27:4047–4054
Johnson LE, Frye TP, Arnot AR, Marquette C, Couture LA, Gendron-Fitzpatrick A, McNeel DG (2006) Safety and immunological efficacy of a prostate cancer plasmid DNA vaccine encoding prostatic acid phosphatase (PAP). Vaccine 24:293–303
McNeel DG, Eickhoff JC, Wargowski E, Zahm C, Staab MJ, Straus J, Liu G (2018) Concurrent, but not sequential, PD-1 blockade with a DNA vaccine elicits anti-tumor responses in patients with metastatic, castration-resistant prostate cancer. Oncotarget P9:25586–25596. https://doi.org/10.18632/oncotarget.25387
Kantoff PW, Higano CS, Shore ND et al (2010) Sipuleucel-T immunotherapy for castration-resistant prostate cancer. N Engl J Med 363:411–422
Acknowledgements
We thank Ken Lo for array construction and analysis.
Funding
This work was supported by the National Institutes of Health (R01 CA219154, TL1 TR002375, T32 GM140935, and P30 CA014520). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Douglas G. McNeel has ownership interest, has received research support, and serves as consultant to Madison Vaccines, Inc. which has licensed intellectual property related to this content. None of the other authors have relevant potential conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Précis: Sera from patients treated with vaccination in four separate clinical trials were evaluated for antibody responses to off-target proteins as a measure of antigen spread. Antibodies were only detected in patients administered GM-CSF as an adjuvant.
Hemanth K. Potluri and Tun Lee Ng are co first authors.
Rights and permissions
About this article
Cite this article
Potluri, H.K., Ng, T.L., Newton, M.A. et al. GM-CSF elicits antibodies to tumor-associated proteins when used as a prostate cancer vaccine adjuvant. Cancer Immunol Immunother 71, 2267–2275 (2022). https://doi.org/10.1007/s00262-022-03150-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-022-03150-3