Abstract
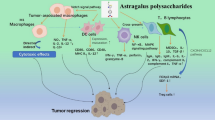
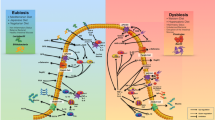
Specific extracts of selected vegetables (SV) have been shown to benefit the survival of stage IIIb/IV non-small cell lung cancer patients in phase I/II studies and is currently in a phase III trial. However, the underlying mechanism of SV-mediated antitumor immune responses has not been elucidated. Our results indicate that SV modulated the NK and adoptive T cell immune responses in antitumor efficacy. Furthermore, antitumor effects of SV were also mediated by innate myeloid cell function, which requires both TLR and β-glucan signaling in a MyD88/TRIF and Dectin-1-dependent manner, respectively. Additionally, SV treatment reduced granulocytic myeloid-derived suppressor cell (MDSC) infiltration into the tumor and limited monocytic MDSC toward the M2-like functional phenotype. Importantly, SV treatment enhanced antigen-specific immune responses by augmenting the activation of antigen-specific TH1/TH17 cells in secondary lymphoid organs and proliferative response, as well as by reducing the Treg population in the tumor microenvironment, which was driven by SV-primed activated M-MDSC. Our results support the idea that SV can subvert immune-tolerance state in the tumor microenvironment and inhibit tumor growth. The present study suggests that features, such as easy accessibility, favorable clinical efficacy, no detectable side effects and satisfactory safety make SV a feasible, appealing and convincing adjuvant therapy for the treatment of cancer patients and prevent tumor recurrence and/or metastases.







Similar content being viewed by others
Availability of data and material
The data analyzed and shown in presented study is available from the corresponding authors upon reasonable request.
References
Siegel RL, Miller KD, Jemal A (2016) Cancer statistics, 2016. CA Cancer J Clin 66:7–30. https://doi.org/10.3322/caac.21332
Yang P (2009) Epidemiology of lung cancer prognosis: quantity and quality of life. Methods Mol Biol 471:469–486. https://doi.org/10.1007/978-1-59745-416-2_24
Rijavec E et al (2014) Ipilimumab in non-small cell lung cancer and small-cell lung cancer: new knowledge on a new therapeutic strategy. Expert Opin Biol Ther 14:1007–1017. https://doi.org/10.1517/14712598.2014.907786
Keating GM (2015) Nivolumab: a review in advanced squamous non-small cell lung cancer. Drugs 75:1925–1934. https://doi.org/10.1007/s40265-015-0492-9
Cappelli LC et al (2016) Inflammatory arthritis and sicca syndrome induced by nivolumab and ipilimumab. Ann Rheum Dis. https://doi.org/10.1136/annrheumdis-2016-209595
Gonzalez-Rodriguez E, Rodriguez-Abreu D, Spanish Group for Cancer I.-B (2016) Immune checkpoint inhibitors: review and management of endocrine adverse events. Oncologist 21:804–816. https://doi.org/10.1634/theoncologist.2015-0509(2016)
Vucenik I, Sakamoto K, Bansal M, Shamsuddin AM (1993) Inhibition of rat mammary carcinogenesis by inositol hexaphosphate (phytic acid). A pilot study. Cancer Lett 75:95–102
Wang HZ, Zhang Y, Xie LP, Yu XY, Zhang RQ (2002) Effects of genistein and daidzein on the cell growth, cell cycle, and differentiation of human and murine melanoma cells(1). J Nutr Biochem 13:421–426
Lu Z et al (2016) S-equol, a secondary metabolite of natural anticancer isoflavone daidzein, inhibits prostate cancer growth in vitro and in vivo, though activating the Akt/FOXO3a pathway. Curr Cancer Drug Targets 16:455–465
Lim W, Jeong M, Bazer FW, Song G (2016) Coumestrol inhibits proliferation and migration of prostate cancer cells by regulating AKT, ERK1/2, and JNK MAPK cell signaling cascades. J Cell Physiol. https://doi.org/10.1002/jcp.25494
Sun AS et al (1999) Phase I/II study of stage III and IV non-small cell lung cancer patients taking a specific dietary supplement. Nutr Cancer 34:62–69. https://doi.org/10.1207/S15327914NC340109
Sun AS et al (2001) Pilot study of a specific dietary supplement in tumor-bearing mice and in stage IIIB and IV non-small cell lung cancer patients. Nutr Cancer 39:85–95. https://doi.org/10.1207/S15327914nc391_12
Ames BN, Gold LS, Willett WC (1995) The causes and prevention of cancer. Proc Natl Acad Sci USA 92:5258–5265
Bailar JC 3rd, Gornik HL (1997) Cancer undefeated. N Engl J Med 336:1569–1574. https://doi.org/10.1056/NEJM199705293362206
Bronte V et al (2016) Recommendations for myeloid-derived suppressor cell nomenclature and characterization standards. Nat Commun 7:12150. https://doi.org/10.1038/ncomms12150
Yang WC, Ma G, Chen SH, Pan PY (2013) Polarization and reprogramming of myeloid-derived suppressor cells. J Mol Cell Biol 5:207–209. https://doi.org/10.1093/jmcb/mjt009
Kao J et al (2011) Targeting immune suppressing myeloid-derived suppressor cells in oncology. Crit Rev Oncol Hematol 77:12–19. https://doi.org/10.1016/j.critrevonc.2010.02.004
Chen HM et al (2015) Myeloid-derived suppressor cells as an immune parameter in patients with concurrent sunitinib and stereotactic body radiotherapy. Clin Cancer Res 21:4073–4085. https://doi.org/10.1158/1078-0432.CCR-14-2742
Pan PY et al (2008) Reversion of immune tolerance in advanced malignancy: modulation of myeloid-derived suppressor cell development by blockade of stem-cell factor function. Blood 111:219–228. https://doi.org/10.1182/blood-2007-04-086835
Ma G et al (2011) Paired immunoglobin-like receptor-B regulates the suppressive function and fate of myeloid-derived suppressor cells. Immunity 34:385–395. https://doi.org/10.1016/j.immuni.2011.02.004
Ma J et al (2010) The M1 form of tumor-associated macrophages in non-small cell lung cancer is positively associated with survival time. BMC Cancer 10:112. https://doi.org/10.1186/1471-2407-10-112
Xiong L et al (2004) Regulating antigen presentation–anti-tumor immuno-therapy by integrative Chinese and Western medicine. Zhongguo Zhong Xi Yi Jie He Za Zhi 24:847–851
Chan GC, Chan WK, Sze DM (2009) The effects of beta-glucan on human immune and cancer cells. J Hematol Oncol 2:25. https://doi.org/10.1186/1756-8722-2-25
Batbayar S, Lee DH, Kim HW (2012) Immunomodulation of fungal beta-glucan in host defense signaling by Dectin-1. Biomol Ther (Seoul) 20:433–445. https://doi.org/10.4062/biomolther.2012.20.5.433
Ma J, Becker C, Lowell CA, Underhill DM (2012) Dectin-1-triggered recruitment of light chain 3 protein to phagosomes facilitates major histocompatibility complex class II presentation of fungal-derived antigens. J Biol Chem 287:34149–34156. https://doi.org/10.1074/jbc.M112.382812
Albeituni SH, Yan J (2013) The effects of beta-glucans on dendritic cells and implications for cancer therapy. Anticancer Agents Med Chem 13:689–698
Tian J et al (2013) beta-Glucan enhances antitumor immune responses by regulating differentiation and function of monocytic myeloid-derived suppressor cells. Eur J Immunol 43:1220–1230. https://doi.org/10.1002/eji.201242841
Eisenstein S et al (2013) Myeloid-derived suppressor cells as a vehicle for tumor-specific oncolytic viral therapy. Cancer Res 73:5003–5015. https://doi.org/10.1158/0008-5472.CAN-12-1597
Ozao-Choy J et al (2009) The novel role of tyrosine kinase inhibitor in the reversal of immune suppression and modulation of tumor microenvironment for immune-based cancer therapies. Cancer Res 69:2514–2522. https://doi.org/10.1158/0008-5472.CAN-08-4709
Movahedi K et al (2010) Different tumor microenvironments contain functionally distinct subsets of macrophages derived from Ly6C(high) monocytes. Cancer Res 70:5728–5739. https://doi.org/10.1158/0008-5472.CAN-09-4672
Geissmann F, Jung S, Littman DR (2003) Blood monocytes consist of two principal subsets with distinct migratory properties. Immunity 19:71–82
Dambuza IM, Brown GD (2015) C-type lectins in immunity: recent developments. Curr Opin Immunol 32:21–27. https://doi.org/10.1016/j.coi.2014.12.002
Albeituni SH et al (2016) Yeast-derived particulate beta-glucan treatment subverts the suppression of myeloid-derived suppressor cells (MDSC) by inducing polymorphonuclear MDSC apoptosis and monocytic MDSC differentiation to APC in cancer. J Immunol 196:2167–2180. https://doi.org/10.4049/jimmunol.1501853
Zhao Y et al (2016) Dectin-1-activated dendritic cells trigger potent antitumour immunity through the induction of Th9 cells. Nat Commun 7:12368. https://doi.org/10.1038/ncomms12368
Goodridge HS et al (2009) Differential use of CARD9 by Dectin-1 in macrophages and dendritic cells. J Immunol 182:1146–1154
Gringhuis SI et al (2012) Dectin-1 is an extracellular pathogen sensor for the induction and processing of IL-1beta via a noncanonical caspase-8 inflammasome. Nat Immunol 13:246–254. https://doi.org/10.1038/ni.2222
Dennehy KM et al (2008) Syk kinase is required for collaborative cytokine production induced through Dectin-1 and Toll-like receptors. Eur J Immunol 38:500–506. https://doi.org/10.1002/eji.200737741
Saeed S et al (2014) Epigenetic programming of monocyte-to-macrophage differentiation and trained innate immunity. Science 345:1251086. https://doi.org/10.1126/science.1251086
Quintin J et al (2012) Candida albicans infection affords protection against reinfection via functional reprogramming of monocytes. Cell Host Microbe 12:223–232. https://doi.org/10.1016/j.chom.2012.06.006
Loures FV et al (2014) Dectin-1 induces M1 macrophages and prominent expansion of CD8+IL-17+ cells in pulmonary paracoccidioidomycosis. J Infect Dis 210:762–773. https://doi.org/10.1093/infdis/jiu136
Lefevre L et al (2010) PPARgamma ligands switched high fat diet-induced macrophage M2b polarization toward M2a thereby improving intestinal Candida elimination. PLoS ONE 5:e12828. https://doi.org/10.1371/journal.pone.0012828
Coste A et al (2003) PPARgamma promotes mannose receptor gene expression in murine macrophages and contributes to the induction of this receptor by IL-13. Immunity 19:329–339
Lee DH, Kim HW (2014) Innate immunity induced by fungal beta-glucans via Dectin-1 signaling pathway. Int J Med Mushrooms 16:1–16
Rosinsky C, Antony PA (2016) A role for pre-mNK cells in tumor progression. J Immunother Cancer 4:16. https://doi.org/10.1186/s40425-016-0120-6
Orr MT et al (2013) MyD88 and TRIF synergistic interaction is required for TH1-cell polarization with a synthetic TLR4 agonist adjuvant. Eur J Immunol 43:2398–2408. https://doi.org/10.1002/eji.201243124
Kumar P, John V, Marathe S, Das G, Bhaskar S (2015) Mycobacterium indicus pranii induces dendritic cell activation, survival, and Th1/Th17 polarization potential in a TLR-dependent manner. J Leukoc Biol 97:511–520. https://doi.org/10.1189/jlb.1A0714-361R
Tassi I et al (2009) Requirement of phospholipase C-gamma2 (PLCgamma2) for Dectin-1-induced antigen presentation and induction of TH1/TH17 polarization. Eur J Immunol 39:1369–1378. https://doi.org/10.1002/eji.200839313
Osorio F et al (2008) DC activated via Dectin-1 convert Treg into IL-17 producers. Eur J Immunol 38:3274–3281. https://doi.org/10.1002/eji.200838950
MacDonald RS et al (2005) Environmental influences on isoflavones and saponins in soybeans and their role in colon cancer. J Nutr 135:1239–1242
Poonyachoti S, Deachapunya C (2012) Modulatory effects of phytoestrogens on the expression of Fas ligand and the release of cytochrome C in normal and cancerous endometrial cells. J Med Assoc Thai 95(Suppl 12):S105-112
Acknowledgements
The authors thank Ms. Marcia Meseck for editing the manuscript. The authors thanks Dr. Jun Yan (University of Louisville) for providing the bone marrow of Dectin-1 KO C57BL/6 mice for this study.
Author information
Authors and Affiliations
Contributions
Dr. Hui-Ming Chen performed most of the research, analyzed data and wrote the manuscript; Dr. Linus Sun and Dr. Ping-Ying Pan made contributions to interpretation of data and intellectual content. Dr. Lu-Hai Wang and Dr. Shu-Hsia Chen made substantial contribution to the conception or design of the research, important intellectual content, project supervision and wrote the manuscript with valuable contribution from all other authors.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing financial interests.
Ethics approval
All animal experiments were done in accordance with approved guidelines for animal experimentation of the Mount Sinai School of Medicine.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, HM., Sun, L., Pan, PY. et al. Nutrient supplements from selected botanicals mediated immune modulation of the tumor microenvironment and antitumor mechanism. Cancer Immunol Immunother 70, 3435–3449 (2021). https://doi.org/10.1007/s00262-021-02927-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-021-02927-2