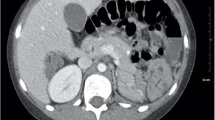
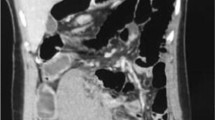
Abstract
The wandering spleen, wandering liver, and wandering kidney are rare diagnoses that can be asymptomatic or are associated with nonspecific symptoms, making the clinical diagnosis elusive. In addition, given the small number of cases, these conditions are not well understood. Major complications of wandering spleen result from torsion of the vascular pedicle with resultant ischemia, physiologic dysfunction, and/or infarction. Wandering liver is commonly associated with bowel obstruction, particularly colonic volvulus, with very rare reports of hepatic ischemia or infarct. Wandering kidneys are not commonly associated with serious complications. In many cases, the wandering spleen, liver or kidney can be found in their anatomic position on static imaging and are only diagnosed during ultrasound or with serial radiographic or cross-sectional imaging with different patient positioning, or with prior studies demonstrating different locations of the involved organ. Treatment approaches for uncomplicated wandering spleen, liver, or kidney include watchful waiting and splenopexy, hepatopexy, or nephropexy, respectively. Complicated wandering spleens are treated with splenectomy. Given the variable clinical presentation of these conditions, imaging plays a pivotal role in diagnosing these rare and often incidentally discovered phenomena.
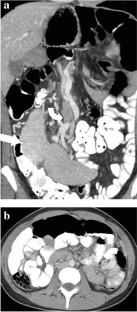







Similar content being viewed by others
References
National Organization for Rare Disorders (NORD). https://rarediseases.org/rare-diseases/wandering-spleen/
Magowska, Anita. “Wandering spleen: a medical enigma, its natural history and rationalization.” World journal of surgery vol. 37,3 (2013): 545-50. doi:https://doi.org/10.1007/s00268-012-1880-x
Richman, Mark et al. “Wandering spleen.” Surgery vol. 155,4 (2014): 728. doi:https://doi.org/10.1016/j.surg.2012.11.015
Varga, Ivan et al. “Anatomic variations of the spleen: current state of terminology, classification, and embryological background.” Surgical and radiologic anatomy : SRA vol. 40,1 (2018): 21-29. doi:https://doi.org/10.1007/s00276-017-1893-0
Desai, D C et al. “Wandering spleen: a challenging diagnosis.” Southern medical journal vol. 90,4 (1997): 439-43. doi:https://doi.org/10.1097/00007611-199704000-00017
Tirkes, Temel et al. “Peritoneal and retroperitoneal anatomy and its relevance for cross-sectional imaging.” Radiographics : a review publication of the Radiological Society of North America, Inc vol. 32,2 (2012): 437-51. doi:https://doi.org/10.1148/rg.322115032
Patel, R R, and K Planche. “Applied peritoneal anatomy.” Clinical radiology vol. 68,5 (2013): 509-20. doi:https://doi.org/10.1016/j.crad.2012.06.135.
Cantone, Noemi et al. “Wandering Spleen and Organoaxial Gastric Volvulus after Morgagni Hernia Repair: A Case Report and Review of the Literature.” Case reports in surgery vol. 2016 (2016): 6450765. doi:https://doi.org/10.1155/2016/6450765
Sodhi, K S et al. “Marfanoid hypermobility syndrome and skeletal abnormalities in a rare case of torsion of wandering spleen.” The British journal of radiology vol. 81,965 (2008): e145-8. doi:https://doi.org/10.1259/bjr/30123041.
Fuentes, Rafael et al. “Hepatocolonic vagrancy: a rare or underrecognized entity?.” AJR. American journal of roentgenology vol. 188,4 (2007): W331-3. doi:https://doi.org/10.2214/AJR.05.0601.
Howenstein, Matthew et al. “Wandering liver: multidetector CT features and the importance of multiplanar reformations.” Emergency radiology vol. 16,2 (2009): 155-7. doi:https://doi.org/10.1007/s10140-008-0707-4.
Mack-Detlefsen, Birte et al. “Laparoscopic hepatopexy: a new surgical approach to hepatoptosis in an 11-year-old boy.” Journal of laparoendoscopic & advanced surgical techniques. Part A vol. 21,6 (2011): 567-9. doi:https://doi.org/10.1089/lap.2010.0485
Nichols, Brandon W et al. “A wandering liver.” Pediatric radiology vol. 40,8 (2010): 1443-5. doi:https://doi.org/10.1007/s00247-010-1586-x.
Bruneau, Antoine et al. “Abdominal Pain due to a Wandering Liver.” Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract vol. 21,5 (2017): 923-925. doi:https://doi.org/10.1007/s11605-016-3277-x.
Bauones, Salem et al. “Wandering liver: ultrasound and magnetic resonance imaging diagnosis.” Journal of pediatric surgery vol. 47,11 (2012): e21-5. doi:https://doi.org/10.1016/j.jpedsurg.2012.07.007.
Ordonez, Alex et al. “Wandering liver and intestinal malrotation: first report.” Surgical case reports vol. 2,1 (2016): 80. doi:https://doi.org/10.1186/s40792-016-0205-y
Tate, P S. “Hepatic torsion and dislocation with hypotension and colonic obstruction.” The American surgeon vol. 59,7 (1993): 455-8..
Susanto, C R, and Anne I J Arens. “A Wandering Kidney.” Kidney medicine vol. 1,6 402-403. 4 Nov. 2019, doi:https://doi.org/10.1016/j.xkme.2019.08.006
Srirangam, Shalom J et al. “Nephroptosis: seriously misunderstood?.” BJU international vol. 103,3 (2009): 296-300. doi:https://doi.org/10.1111/j.1464-410X.2008.08082.x
Bynum, B. “Floating kidney.” Lancet (London, England) vol. 357,9249 (2001): 76. doi:https://doi.org/10.1016/S0140-6736(05)71581-6
Sood, Akshay, and Craig Rogers. “Floating kidney.” BMJ case reports vol. 2018 bcr2018224921. 17 Apr. 2018, doi:https://doi.org/10.1136/bcr-2018-224921
Sarac, M., Bakal, U., Tartar, T., Canpolat, S., Kara, A., & Kazez, A. (2018). Bochdalek hernia and intrathoracic ectopic kidney: Presentation of two case reports and review of the literature. Nigerian journal of clinical practice, 21(5), 681–686. https://doi-org.treadwell.idm.oclc.org/https://doi.org/10.4103/njcp.njcp_217_17
Tchidjou, Hyppolite K et al. “Wandering spleen: 'presentation in adolescent with high thrombotic risk'.” Blood coagulation & fibrinolysis : an international journal in haemostasis and thrombosis vol. 25,5 (2014): 530-3. doi:https://doi.org/10.1097/MBC.0000000000000081
Reisner, David C, and Constantine M Burgan. “Wandering Spleen: An Overview.” Current problems in diagnostic radiology vol. 47,1 (2018): 68-70. doi:https://doi.org/10.1067/j.cpradiol.2017.02.007.
Emanuels, Carolina S et al. “Displacement of the Spleen Mimicking Renal Cell Cancer Recurrence Post-Nephrectomy: A Case Report.” Journal of kidney cancer and VHL vol. 2,3 130-133. 20 Jun. 2015, doi:https://doi.org/10.15586/jkcvhl.2015.36
Zonca, Pavel et al. “Ectopic liver: different manifestations, one solution.” World journal of gastroenterology vol. 19,38 (2013): 6485-9. doi:https://doi.org/10.3748/wjg.v19.i38.6485.
Blackburn, Simon C, and Michael P Stanton. “Anatomy and physiology of the peritoneum.” Seminars in pediatric surgery vol. 23,6 (2014): 326-30. doi:https://doi.org/10.1053/j.sempedsurg.2014.06.002.
Parolini, Filippo, and Daniele Alberti. “Wandering liver.” Surgery vol. 161,4 (2017): 1174-1175. doi:https://doi.org/10.1016/j.surg.2016.01.021.
Svensson, Jan F et al. “"Wandering liver" in a neonate: case report and review of the literature.” Journal of pediatric surgery vol. 45,3 (2010): 635-8. doi:https://doi.org/10.1016/j.jpedsurg.2009.12.017.
Siddins, M T, and R J Cade. “Hepatocolonic vagrancy: wandering liver with colonic abnormalities.” The Australian and New Zealand journal of surgery vol. 60,5 (1990): 400-3. doi:https://doi.org/10.1111/j.1445-2197.1990.tb07392.x.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethical approval
This study does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Caruso, M.J., Bidani, K. & Singh, A.K. Wandering liver, spleen, and kidney: what the radiologist needs to know. Abdom Radiol 48, 1854–1861 (2023). https://doi.org/10.1007/s00261-022-03789-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03789-7