Abstract
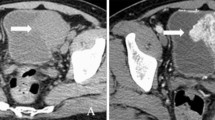
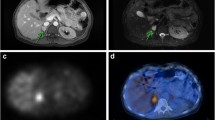
Bladder paragangliomas (bPGL) are rare neuroendocrine tumors arising from the sympathetic paraganglia present in the bladder wall. Bladder PGLs are typically submucosal or intramural but when subserosal may not be readily visible at cystoscopy. The average size at presentation is 3.9 cm (range 1.0–9.1 cm). When small, bPGL are usually spherical, well-marginated and homogeneous. Larger bPGL are typically more complex with peri- and intra-tumoral neovascularity and central necrosis. On ultrasound, increased color Doppler signal is typical. The increased soft tissue resolution of MRI enables localization of bPGL within the bladder wall more accurately than CT. Restricted diffusion and avid contrast enhancement help differentiate small bPGLs from leiomyomas, which have similar appearances on ultrasound and CT. Nuclear medicine techniques identify bPGLs and their metastases with high specificity, 68Ga-DOTATATE PET/CT having largely replaced 123I-mIBG SPECT/CT as the first line functional investigation. Imaging is essential to aid surgical planning, as endoscopic resection is often not possible or incomplete due to tumor location. For patients with advanced disease, 68Ga-DOTATATE PET/CT and 123I-mIBG SPECT/CT assess suitability for peptide receptor radionuclide therapy. Up to 63% of bPGL patients have a germline mutation, most commonly in the SDHB subunit gene, increasing their risk of developing pheochromocytomas and further paragangliomas; lifelong annual biochemical and periodic imaging screening from skull base to pelvis is therefore recommended.
Graphical abstract













Similar content being viewed by others
References
Purnell S, Sidana A, Maruf M, Grant C, Agarwal PK (2017) Genitourinary paraganglioma: Demographic, pathologic, and clinical characteristics in the surveillance, epidemiology, and end results database (2000-2012). Urol Oncol 35:457.e459-457.e414
Lenders JWM, Kerstens MN, Amar L et al (2020) Genetics, diagnosis, management and future directions of research of phaeochromocytoma and paraganglioma: a position statement and consensus of the Working Group on Endocrine Hypertension of the European Society of Hypertension. J Hypertens 38:1443-1456
Beilan JA, Lawton A, Hajdenberg J, Rosser CJ (2013) Pheochromocytoma of the urinary bladder: a systematic review of the contemporary literature. BMC Urol 13:22
Zhai H, Ma X, Nie W et al (2017) Paraganglioma of the Urinary Bladder: A Series of 22 Cases in a Single Center. Clin Genitourin Cancer 15:e765-e771
Martucci VL, Lorenzo ZG, Weintraub M et al (2015) Association of urinary bladder paragangliomas with germline mutations in the SDHB and VHL genes. Urol Oncol 33:167.e113-120
Plouin PF, Amar L, Dekkers OM et al (2016) European Society of Endocrinology Clinical Practice Guideline for long-term follow-up of patients operated on for a phaeochromocytoma or a paraganglioma. Eur J Endocrinol 174:G1-g10
Lu H, Male M, Jiang K, Ye Z, Song D, Xia D (2019) Clinical significance of functional and anatomical classifications in paraganglioma of the urinary bladder. Urol Oncol 37:354.e359-354.e317
Ranaweera M, Chung E (2014) Bladder paraganglioma: A report of case series and critical review of current literature. World journal of clinical cases 2:591-595
Male M, Ye T, Tao J, Chen Z-Q, Peng E (2019) Differentiating Nonfunctional Paraganglioma of the Bladder from Urothelial Carcinoma of the Bladder: Pitfalls and Breakthroughs. BioMed research international 2019:1097149-1097149
Qin J, Zhou G, Chen X (2020) Imaging manifestations of bladder paraganglioma. Ann Palliat Med 9:346-351
Liang J, Li H,Gao L, Yin L, Yin L, Zhang J (2016) Bladder Paraganglioma: Clinicopathology and Magnetic Resonance Imaging Study of Five Patients. Urol J 13:2605-2611
Fan DG, Wu CL, Huang HJ et al (2020) [Paraganglioma of urinary bladder: a clinicopathological features analysis of 23 cases]. Zhonghua Bing Li Xue Za Zhi 49:311-316
Wang H, Ye H, Guo A et al (2011) Bladder paraganglioma in adults: MR appearance in four patients. Eur J Radiol 80:e217-220
Wang EY, Pak JS, Virk RK et al (2020) Bladder Preservation for Patients With Bladder Paragangliomas: Case Series and Review of the Literature. Urology 143:194-205
Withey SJ, Perrio S, Christodoulou D et al (2019) Imaging Features of Succinate Dehydrogenase–deficient Pheochromocytoma-Paraganglioma Syndromes. RadioGraphics 39:1393-1410
Chang Y-K, Chiang IN, Chen C-H et al (2015) Paragangliomas of the urinary bladder: A report of 6 cases and review of the literature. Urological Science 26:111-114
Li Y, Guo A, Tang J et al (2014) Evaluation of sonographic features for patients with urinary bladder paraganglioma: a comparison with patients with urothelial carcinoma. Ultrasound Med Biol 40:478-484
Huang L, Kong Q, Liu Z, Wang J, Kang Z, Zhu Y (2018) The Diagnostic Value of MR Imaging in Differentiating T Staging of Bladder Cancer: A Meta-Analysis. Radiology 286:502-511
Woo S, Suh CH, Kim SY, Cho JY, Kim SH (2017) Diagnostic performance of MRI for prediction of muscle-invasiveness of bladder cancer: A systematic review and meta-analysis. Eur J Radiol 95:46-55
Jacques AE, Sahdev A, Sandrasagara M et al (2008) Adrenal phaeochromocytoma: correlation of MRI appearances with histology and function. Eur Radiol 18:2885-2892
Moran CA, Albores-Saavedra J, Wenig BM, Mena H (1997) Pigmented extraadrenal paragangliomas. A clinicopathologic and immunohistochemical study of five cases. Cancer 79:398-402
Mou JW, Lee KH, Tam YH, Cheung ST, Chan KW, Thakre A (2008) Urinary bladder pheochromocytoma, an extremely rare tumor in children: case report and review of the literature. Pediatr Surg Int 24:479-480
Chen M, Lipson SA, Hricak H (1997) MR imaging evaluation of benign mesenchymal tumors of the urinary bladder. American Journal of Roentgenology 168:399-403
Wong-You–Cheong JJ, Woodward PJ, Manning MA, Sesterhenn IA (2006) Neoplasms of the Urinary Bladder: Radiologic-Pathologic Correlation. RadioGraphics 26:553-580
Chung AD, Schieda N, Flood TA et al (2015) Suburothelial and extrinsic lesions of the urinary bladder: radiologic and pathologic features with emphasis on MR imaging. Abdom Imaging 40:2573-2588
Kim JC, Kim KH, Jung S (2003) Small cell carcinoma of the urinary bladder: CT and MR imaging findings. Korean journal of radiology 4:130-135
Parra LA, Swanson SK, Salomao MA, Yang M (2020) Multifocal Urinary Bladder Paragangliomas With Negative 68Ga-DOTATATE Uptake and Positive 123I-MIBG Uptake. Clin Nucl Med 45:e156-e157
Maurice JB, Troke R, Win Z et al (2012) A comparison of the performance of 68Ga-DOTATATE PET/CT and 123I-MIBG SPECT in the diagnosis and follow-up of phaeochromocytoma and paraganglioma. Eur J Nucl Med Mol Imaging 39:1266-1270
Moses WW (2011) Fundamental Limits of Spatial Resolution in PET. Nuclear instruments & methods in physics research Section A, Accelerators, spectrometers, detectors and associated equipment 648 Supplement 1:S236-S240
Khalil MM, Tremoleda JL, Bayomy TB, Gsell W (2011) Molecular SPECT Imaging: An Overview. International Journal of Molecular Imaging 2011:796025
Bhatia KS, Ismail MM, Sahdev A et al (2008) 123I-metaiodobenzylguanidine (MIBG) scintigraphy for the detection of adrenal and extra-adrenal phaeochromocytomas: CT and MRI correlation. Clin Endocrinol (Oxf) 69:181-188
Koopmans KP, Jager PL, Kema IP, Kerstens MN, Albers F, Dullaart RP (2008) 111In-octreotide is superior to 123I-metaiodobenzylguanidine for scintigraphic detection of head and neck paragangliomas. J Nucl Med 49:1232-1237
Janssen I, Blanchet EM, Adams K et al (2015) Superiority of [68Ga]-DOTATATE PET/CT to Other Functional Imaging Modalities in the Localization of SDHB-Associated Metastatic Pheochromocytoma and Paraganglioma. Clin Cancer Res 21:3888-3895
King K, Chen C, Alexopoulos D et al (2011) Functional imaging of SDHx-related head and neck paragangliomas: comparison of 18F-fluorodihydroxyphenylalanine, 18F-fluorodopamine, 18F-fluoro-2-deoxy-d-glucose PET, 123I-metaiodobenzylguanidine scintigraphy, and 111In-pentetreotide scintigraphy. Journal of Clinical Endocrinology and Metabolism 96:2779-2785
Wittekind C, Brierley J, Lee A, van Eycken E (2019) TNM Supplement: A Commentary on Uniform Use, 5th Edition edn. Wiley-Blackwell
Brierley JD, Gospodarowicz MK, Wittekind C (2017) TNM classification of malignant tumours. John Wiley & Sons
Lloyd R, De Lellis R, Heitz P, Eng C (2004) World Health Organization classification of tumours: pathology and genetics of tumours of the endocrine organs. International Agency for Research on Cancer (IARC) Press, Lyon
Srirangalingam U, Banerjee A, Patki P et al (2017) Succinate Dehydrogenase B (SDHB)-Associated Bladder Paragangliomas. Clin Genitourin Cancer 15:e131-e136
Fliedner SMJ, Lehnert H, Pacak K (2010) Metastatic paraganglioma. Seminars in oncology 37:627-637
Cheng L, Leibovich BC, Cheville JC et al (2000) Paraganglioma of the urinary bladder. Cancer 88:844-852
Ayala-Ramirez M, Feng L, Johnson MM et al (2011) Clinical risk factors for malignancy and overall survival in patients with pheochromocytomas and sympathetic paragangliomas: primary tumor size and primary tumor location as prognostic indicators. J Clin Endocrinol Metab 96:717-725
Vanderveen KA, Thompson SM, Callstrom MR et al (2009) Biopsy of pheochromocytomas and paragangliomas: potential for disaster. Surgery 146:1158-1166
Sanjoaquín MT, Fraile JR, Gutiérrez A, Canal MI, Navia J (2000) Hypertensive crisis during a transurethral resection of the bladder: nondiagnosed bladder paraganglioma. Anesth Analg 90:556-558
Chen H, Sippel RS, O'Dorisio MS, Vinik AI, Lloyd RV, Pacak K (2010) The North American Neuroendocrine Tumor Society consensus guideline for the diagnosis and management of neuroendocrine tumors: pheochromocytoma, paraganglioma, and medullary thyroid cancer. Pancreas 39:775-783
Wang C, Richmond R, Eldesouki E (2015) Anesthetic management for resection of para-aortic paraganglioma and unexpected aortic resection: A case report. Exp Ther Med 9:1542-1544
García MIDO, Palasí R, Gómez RC, Marco JLP, Merino-Torres JF (2019) Surgical and pharmacological management of functioning pheochromocytoma and paraganglioma. Exon Publications:63–80
Niemeijer ND, Alblas G, van Hulsteijn LT, Dekkers OM, Corssmit EP (2014) Chemotherapy with cyclophosphamide, vincristine and dacarbazine for malignant paraganglioma and pheochromocytoma: systematic review and meta-analysis. Clin Endocrinol (Oxf) 81:642-651
Nastos K, Cheung VTF, Toumpanakis C et al (2017) Peptide Receptor Radionuclide Treatment and (131)I-MIBG in the management of patients with metastatic/progressive phaeochromocytomas and paragangliomas. J Surg Oncol 115:425-434
Gimenez-Roqueplo AP, Dahia PL, Robledo M (2012) An update on the genetics of paraganglioma, pheochromocytoma, and associated hereditary syndromes. Horm Metab Res 44:328-333
Richards S, Aziz N, Bale S et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genetics in Medicine 17:405-423
Ellard S, Baple EL, Berry I et al (2019) ACGS Best Practice Guidelines for Variant Classification 2019,
Lenders JWM, Duh Q-Y, Eisenhofer G et al (2014) Pheochromocytoma and Paraganglioma: An Endocrine Society Clinical Practice Guideline. The Journal of Clinical Endocrinology & Metabolism 99:1915-1942
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no funding and no conflicts of interest. No patient-identifiable information is used in the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Withey, S.J., Christodoulou, D., Prezzi, D. et al. Bladder paragangliomas: a pictorial review. Abdom Radiol 47, 1414–1424 (2022). https://doi.org/10.1007/s00261-022-03443-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03443-2