Abstract
Objective
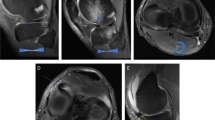
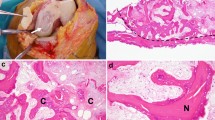
The purpose of this retrospective study is to describe the MRI findings of the “shiny corner” of the knee (bone marrow lesions at the meniscal-covered portions of the tibial plateau) and to determine its association with compromise of the medial meniscal-osteochondral unit.
Materials and methods
A retrospective review of 200 knee MRI exams was performed and images were evaluated in consensus by two musculoskeletal radiologists. Presence and location of a shiny-corner lesion was recorded, which was defined as a focal, peripheral hyperintense lesion on fluid-sensitive images at the superior portion of the medial tibial plateau. Meniscal and root ligament abnormalities were recorded, including tearing, degeneration, and extrusion.
Results
Sixty exams demonstrated a shiny-corner lesion. Shiny corners involved the medial rim of the medial tibial plateau in 50 cases, only involved the posterior rim in seven cases, and only involved the anterior rim in two cases. Patients with shiny corners were older than patients without shiny corners (mean, 53 years vs. 44 years, p = 0.01). The shiny-corner sign was associated with tears of the medial meniscus, root ligament, and meniscal extrusion (p < 0.001). The presence of a shiny-corner lesion could detect a tear of the medial meniscus or root ligaments with a sensitivity, specificity, positive predictive value, and negative predictive value of 62, 97, 95, and 75 %, respectively.
Conclusions
Shiny-corner lesions of the knee are associated with tears of the menisci and root ligaments. This observation supports the concept that the menisci protect the underlying covered portions of the tibial plateau.




Similar content being viewed by others
References
Goodwin DW. MR imaging of the articular cartilage of the knee. Semin Musculoskelet Radiol. 2009;13(4):326–39.
Arno S, Walker PS, Bell CP, Krasnokutsky S, Samuels J, Abramson SB, et al. Relation between cartilage volume and meniscal contact in medial osteoarthritis of the knee. Knee. 2012;19(6):896–901.
Milz S, Putz R. Quantitative morphology of the subchondral plate of the tibial plateau. J Anat. 1994;185(Pt 1):103–10.
Thambyah A, Nather A, Goh J. Mechanical properties of articular cartilage covered by the meniscus. Osteoarthr Cartil/OARS, Osteoarthr Res Soc. 2006;14(6):580–8.
Deneweth JM, Newman KE, Sylvia SM, McLean SG, Arruda EM. Heterogeneity of tibial plateau cartilage in response to a physiological compressive strain rate. J Orthop Res: Off Publ Orthop Res Soc. 2013;31(3):370–5.
Noble J, Alexander K. Studies of tibial subchondral bone density and its significance. J Bone Joint Surg Am Vol. 1985;67(2):295–302.
Pelletier JP, Raynauld JP, Berthiaume MJ, Abram F, Choquette D, Haraoui B, et al. Risk factors associated with the loss of cartilage volume on weight-bearing areas in knee osteoarthritis patients assessed by quantitative magnetic resonance imaging: a longitudinal study. Arthritis Res Ther. 2007;9(4):R74.
Wang Y, Wluka AE, Pelletier JP, Martel-Pelletier J, Abram F, Ding C, et al. Meniscal extrusion predicts increases in subchondral bone marrow lesions and bone cysts and expansion of subchondral bone in osteoarthritic knees. Rheumatology (Oxford). 2010;49(5):997–1004.
Felson DT, McLaughlin S, Goggins J, LaValley MP, Gale ME, Totterman S, et al. Bone marrow edema and its relation to progression of knee osteoarthritis. Ann Intern Med. 2003;139(5 Pt 1):330–6.
Felson DT, Chaisson CE, Hill CL, Totterman SM, Gale ME, Skinner KM, et al. The association of bone marrow lesions with pain in knee osteoarthritis. Ann Intern Med. 2001;134(7):541–9.
Zanetti M, Bruder E, Romero J, Hodler J. Bone marrow edema pattern in osteoarthritic knees: correlation between MR imaging and histologic findings. Radiology. 2000;215(3):835–40.
Roemer FW, Frobell R, Hunter DJ, Crema MD, Fischer W, Bohndorf K, et al. MRI-detected subchondral bone marrow signal alterations of the knee joint: terminology, imaging appearance, relevance and radiological differential diagnosis. Osteoarthritis and Cartilage/OARS, Osteoarthritis Research Society. 2009;17(9):1115–31.
Yao L, Stanczak J, Boutin RD. Presumptive subarticular stress reactions of the knee: MRI detection and association with meniscal tear patterns. Skeletal Radiol. 2004;33(5):260–4.
Kim NR, Choi JY, Hong SH, Jun WS, Lee JW, Choi JA, et al. “MR corner sign”: value for predicting presence of ankylosing spondylitis. AJR Am J Roentgenol. 2008;191(1):124–8.
Jevtic V, Kos-Golja M, Rozman B, McCall I. Marginal erosive discovertebral “Romanus” lesions in ankylosing spondylitis demonstrated by contrast enhanced Gd-DTPA magnetic resonance imaging. Skeletal Radiol. 2000;29(1):27–33.
De Smet AA. How I diagnose meniscal tears on knee MRI. Am J Roentgenol. 2012;199(3):481–99.
Sanders TG, Medynski MA, Feller JF, Lawhorn KW. Bone contusion patterns of the knee at MR imaging: footprint of the mechanism of injury. Radiographics. 2000; 20 Spec No:S135-151.
De Smet AA, Tuite MJ. Use of the “two-slice-touch” rule for the MRI diagnosis of meniscal tears. AJR Am J Roentgenol. 2006;187(4):911–4.
Stoller DW, Martin C, Crues 3rd JV, Kaplan L, Mink JH. Meniscal tears: pathologic correlation with MR imaging. Radiology. 1987;163(3):731–5.
Costa CR, Morrison WB, Carrino JA. Medial meniscus extrusion on knee MRI: is extent associated with severity of degeneration or type of tear? AJR Am J Roentgenol. 2004;183(1):17–23.
Miller TT, Staron RB, Feldman F, Cepel E. Meniscal position on routine MR imaging of the knee. Skeletal Radiol. 1997;26(7):424–7.
Peterfy CG, Guermazi A, Zaim S, Tirman PF, Miaux Y, White D, et al. Whole-organ magnetic resonance imaging score (WORMS) of the knee in osteoarthritis. Osteoarthritis and Cartilage/OARS, Osteoarthritis Research Society. 2004;12(3):177–90.
Roemer FW, Neogi T, Nevitt MC, Felson DT, Zhu Y, Zhang Y, et al. Subchondral bone marrow lesions are highly associated with, and predict subchondral bone attrition longitudinally: the most study. Osteoarthritis and Cartilage/OARS, Osteoarthritis Research Society. 2010;18(1):47–53.
Bergin D, Hochberg H, Zoga AC, Qazi N, Parker L, Morrison WB. Indirect soft-tissue and osseous signs on knee MRI of surgically proven meniscal tears. AJR Am J Roentgenol. 2008;191(1):86–92.
Muriuki MG, Tuason DA, Tucker BG, Harner CD. Changes in tibiofemoral contact mechanics following radial split and vertical tears of the medial meniscus an in vitro investigation of the efficacy of arthroscopic repair. J Bone Joint Surg Am Vol. 2011;93(12):1089–95.
Bjorkengren AG, AlRowaih A, Lindstrand A, Wingstrand H, Thorngren KG, Pettersson H. Spontaneous osteonecrosis of the knee: value of MR imaging in determining prognosis. AJR Am J Roentgenol. 1990;154(2):331–6.
Lecouvet FE, van de Berg BC, Maldague BE, Lebon CJ, Jamart J, Saleh M, et al. Early irreversible osteonecrosis versus transient lesions of the femoral condyles: prognostic value of subchondral bone and marrow changes on MR imaging. AJR Am J Roentgenol. 1998;170(1):71–7.
Nakagawa S, Kadoya Y, Todo S, Kobayashi A, Sakamoto H, Freeman MA, et al. Tibiofemoral movement 3: full flexion in the living knee studied by MRI. J Bone Joint Surg Br Vol. 2000;82(8):1199–200.
Acknowledgments
Eric Y. Chang, MD, gratefully acknowledges grant support from the VA Clinical Science Research and Development Career Development Award (IK2CX000749).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chang, E.Y., Chen, K.C. & Chung, C.B. The shiny corner of the knee: a sign of meniscal osteochondral unit dysfunction. Skeletal Radiol 43, 1403–1409 (2014). https://doi.org/10.1007/s00256-014-1958-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-014-1958-7