Abstract
Background
Quantifying femoral version is crucial in diagnosing femoral version abnormalities and for accurate pre-surgical planning. There are numerous methods for measuring femoral version, however, reliability studies for most of these methods excluded children with hip deformities.
Objective
To propose a method of measuring femoral version based on a virtual 3D femur model, and systematically compare its reliability to the widely used Murphy’s 2D axial slice technique.
Materials and methods
We searched our imaging database to identify hip/femur CTs performed on children (<18 years old) with a clinical indication of femoral version measurement (September 2021—August 2022). Exclusion criteria were prior hip surgery, and inadequate image quality or field-of-view. Two blinded radiologists independently measured femoral version using the virtual 3D femur model and Murphy’s 2D axial slice method. To assess intrareader variability, we randomly selected 20% of the study sample for re-measurements by the two radiologists >2 weeks later. We analyzed the reliability and correlation of these techniques via intraclass correlation coefficient (ICC), Bland-Altman analysis, and deformity subgroup analysis.
Results
Our study sample consisted of 142 femurs from 71 patients (10.6±4.4 years, male=31). Intra- and inter-reader correlations for both techniques were excellent (ICC≥0.91). However, Bland-Altman analysis revealed that the standard deviation (SD) of the absolute difference between the two radiologists for the Murphy method (mean 13.7°) was larger than that of the 3D femur model technique (mean 4.8°), indicating higher reader variability. In femurs with hip flexion deformity, the SD of the absolute difference for the Murphy technique was 17°, compared to 6.5° for the 3D femur model technique. In femurs with apparent coxa valga deformity, the SD of the absolute difference for the Murphy technique was 10.4°, compared to 5.2° for the 3D femur model technique.
Conclusion
The 3D femur model technique is more reliable than the Murphy's 2D axial slice technique in measuring femoral version, especially in children with hip flexion and apparent coxa valga deformities.








Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Murphy SB, Simon SR, Kijewski PK et al (1987) Femoral anteversion. J Bone Joint Surg Am 69:1169–1176
Reikerås O, Bjerkreim I, Sortland O (1983) Fluoroscopy in measurement of femoral neck anteversion. Acta Radiol Diagn (Stockh) 24:81–83
Sankar WN, Novais E, Koueiter D et al (2018) Analysis of femoral version in patients undergoing periacetabular osteotomy for symptomatic acetabular dysplasia. J Am Acad Orthop Surg 26:545–551
Roth PB (1920) A note on abnormal torsion of the femoral shaft. Proc R Soc Med 13:237–241
Fabricant PD, Fields KG, Taylor SA et al (2015) The effect of femoral and acetabular version on clinical outcomes after arthroscopic femoroacetabular impingement surgery. J Bone Joint Surg Am 97:537–543
Mastel MS, El-Bakoury A, Parkar A et al (2020) Outcomes of femoral de-rotation osteotomy for treatment of femoroacetabular impingement in adults with decreased femoral anteversion. J Hip Preserv Surg 7:755–763
Lerch TD, Antioco T, Meier MK et al (2022) Combined abnormalities of femoral version and acetabular version and McKibbin Index in FAI patients evaluated for hip preservation surgery. J Hip Preserv Surg 9:67–77
Sutter R, Dietrich TJ, Zingg PO, Pfirrmann CWA (2012) Femoral antetorsion: comparing asymptomatic volunteers and patients with femoroacetabular impingement. Radiology 263:475–483
Schaver AL, Oshodi A, Glass NA et al (2022) Cam morphology is associated with increased femoral version: Findings from a collection of 1,321 cadaveric femurs. Arthroscopy 38:831–836
Davids JR, Marshall AD, Blocker ER et al (2003) Femoral anteversion in children with cerebral palsy. Assessment with two and three-dimensional computed tomography scans. J Bone Joint Surg Am 85:481–488
Abel MF, Sutherland DH, Wenger DR, Mubarak SJ (1994) Evaluation of CT scans and 3-D reformatted images for quantitative assessment of the hip. J Pediatr Orthop 14:48–53
Sugano N, Noble PC, Kamaric E (1998) A comparison of alternative methods of measuring femoral anteversion. J Comput Assist Tomogr 22:610–614
Tomczak RJ, Guenther KP, Rieber A et al (1997) MR imaging measurement of the femoral antetorsional angle as a new technique: comparison with CT in children and adults. AJR Am J Roentgenol 168:791–794
Takeuchi S, Goto H, Iguchi H et al (2019) Ultrasonographic assessment of femoral torsion angle based on tilting angles of femoral neck and condylar axis. Ultrasound Med Biol 45:1970–1976
Kuo TY, Skedros JG, Bloebaum RD (2003) Measurement of femoral anteversion by biplane radiography and computed tomography imaging: comparison with an anatomic reference. Invest Radiol 38:221–229
Schmaranzer F, Kallini JR, Miller PE et al (2020) The effect of modality and landmark selection on MRI and CT femoral torsion angles. Radiology 296:381–390
Jarrett DY, Oliveira AM, Zou KH et al (2010) Axial oblique CT to assess femoral anteversion. AJR Am J Roentgenol 194:1230–1233
Hermann KL, Egund N (1997) CT Measurement of Anteversion in the Femoral Neck. Acta Radiol 38:527–532
Schmaranzer F, Lerch TD, Siebenrock KA et al (2019) Differences in femoral torsion among various measurement methods increase in hips with excessive femoral torsion. Clin Orthop Relat Res 477:1073–1083
Kaiser P, Attal R, Kammerer M et al (2016) Significant differences in femoral torsion values depending on the CT measurement technique. Arch Orthop Trauma Surg 136:1259–1264
Lerch TD, Kaim T, Hanke MS et al (2023) Assessment of femoral retroversion on preoperative hip magnetic resonance imaging in patients with slipped capital femoral epiphysis: Theoretical implications for hip impingement risk estimation. J Child Orthop 17:116–125
Zhang Z, Ren N, Cheng H et al (2023) Periacetabular osteotomy for Tönnis grade 2 osteoarthritis secondary to hip dysplasia. Int Orthop. https://doi.org/10.1007/s00264-023-05795-w
Meier MK, Wagner M, Brunner A et al (2023) Can gadolinium contrast agents be replaced with saline for direct MR arthrography of the hip? Eur Radiol, A pilot study with arthroscopic comparison. https://doi.org/10.1007/s00330-023-09586-0
Zurmühle CA, Kuner V, McInnes J et al (2021) The crescent sign-a predictor of hip instability in magnetic resonance arthrography. J Hip Preserv Surg 8:164–171
Schmaranzer F, Kheterpal AB, Bredella MA (2021) Best practices: Hip femoroacetabular impingement. AJR Am J Roentgenol 216:585–598
Buly RL, Sosa BR, Poultsides LA et al (2018) Femoral derotation osteotomy in adults for version abnormalities. J Am Acad Orthop Surg 26:e416–e425
Lee YS, Oh SH, Seon JK et al (2007) 3D femoral neck anteversion measurements based on the posterior femoral plane in ORTHODOC® system. Med Biol Eng Comput 45:325–325
Brooks JT, Bomar JD, Jeffords ME et al (2021) Defining a new three-dimensional method for determining femoral torsional pathology in children. J Pediatr Orthop B 30:331–336
Reikerås O, Bjerkreim I, Kolbenstvedt A (1983) Anteversion of the acetabulum and femoral neck in normals and in patients with osteoarthritis of the hip. Acta Orthop Scand 54:18–23
Gittings DJ, Dattilo JR, Fryhofer G et al (2017) Treatment of hip flexion contractures with psoas recession through the middle window of the ilioinguinal approach. JBJS Essent Surg Tech 7:e25
Pinero JR, Goldstein RY, Culver S et al (2012) Hip flexion contracture and diminished functional outcomes in cerebral palsy. J Pediatr Orthop 32:600–604
Tönnis D, Heinecke A (1999) Current concepts review - acetabular and femoral anteversion. J Bone Joint Surg Am 81:1747–1770
Morvan J, Bouttier R, Mazieres B et al (2013) Relationship between hip dysplasia, pain, and osteoarthritis in a cohort of patients with hip symptoms. J Rheumatol 40:1583–1589
Dolan MM, Heyworth BE, Bedi A et al (2011) CT reveals a high incidence of osseous abnormalities in hips with labral tears. Clin Orthop Relat Res 469:831–838
Liu RW, Toogood P, Hart DE et al (2009) The effect of varus and valgus osteotomies on femoral version. J Pediatr Orthop 29:666–675
Morrell DS, Pearson JM, Sauser DD (2002) Progressive bone and joint abnormalities of the spine and lower extremities in cerebral palsy. Radiographics 22:257–268
Mathews SS, Jones MH, Sperling SC (1953) Hip derangements seen in cerebral palsied children. Am J Phys Med 32:213–221
Sauser DD, Hewes RC, Root L (1986) Hip changes in spastic cerebral palsy. AJR Am J Roentgenol 146:1219–1222
Kay RM, Jaki KA, Skaggs DL (2000) The effect of femoral rotation on the projected femoral neck-shaft angle. J Pediatr Orthop 20:736–739
Boese CK, Jostmeier J, Oppermann J et al (2016) The neck shaft angle: CT reference values of 800 adult hips. Skeletal Radiol 45:455–463
Sullivan ES, Jones C, Miller SD et al (2022) Effect of positioning error on the Hilgenreiner epiphyseal angle and the head-shaft angle compared to the femoral neck-shaft angle in children with cerebral palsy. J Pediatr Orthop B 31:160–168
Sullivan ES, Jones C, Miller SD et al (2022) Effect of positioning error on the Hilgenreiner epiphyseal angle and the head-shaft angle compared to the femoral neck-shaft angle in children with cerebral palsy. J Pediatr Orthop B 31:160–168
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15:155–163
Martin Bland J, Altman D (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 327:307–310
Liljequist D, Elfving B, Skavberg Roaldsen K (2019) Intraclass correlation - A discussion and demonstration of basic features. PLoS One 14:e0219854
Cicchetti DV (1994) Guidelines, criteria, and rules of thumb for evaluating normed and standardized assessment instruments in psychology. Psychol Assess 6:284–290
Haghayegh S, Kang H-A, Khoshnevis S et al (2020) A comprehensive guideline for Bland-Altman and intra class correlation calculations to properly compare two methods of measurement and interpret findings. Physiol Meas 41:055012
Anvari A, Halpern EF, Samir AE (2018) Essentials of statistical methods for assessing reliability and agreement in quantitative imaging. Acad Radiol 25:391–396
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
A.T. conceived, supervised and supported the study. J.I.N. collated the data, performed the statistical analysis and drafted the initial manuscript and multimedia. S.D.B. and M.A.B. interpreted the images. D.Y.J. and D.A. conceived and implemented the 3D model. E.L. helped perform the statistical analysis. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
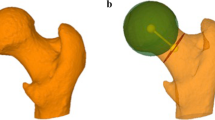
The virtual 3D femur model method applied to two different patients. A femur from a patient without coxa valga or hip flexion deformity (first femur), and a femur from a patient with both coxa valga and hip flexion deformity (second femur) are illustrated. The virtual 3D femur model method consists of rotating the entire model in the sagittal direction to allow an axial point-of-view of both femoral condyles and the femoral neck. The user has the option of viewing the femur from a caudal-to-cranial point-of-view (where the angle was assessed as 20º and 23º on the first and second femurs, respectively), or from a cranial-to-caudal point-of-view (where the angle was assessed as 19º and 22º on the first and second femurs, respectively). The center of rotation is the mid femoral shaft, and a single angle is drawn between the femoral neck axis and the posterior aspect of the femoral condyles. (MP4 1797 kb)
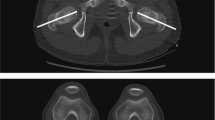
Murphy’s 2D axial slice methodology applied to a femur from a patient without coxa valga or hip flexion deformity. The center of the femoral head is determined by triangulation with coronal images. The cursor is placed at the center of femoral head on the axial plane while the CT images are advanced caudally to the base of the femoral neck, which is defined as at the level of the lesser trochanter. The proximal angle is formed by the line connecting these two points and the horizontal plane (8º on this example). The axial CT images demonstrating the posterior aspects of the femoral condyles are identified. The distal angle is drawn between a line tangential to the posterior margin of the femoral condyles and the horizontal plane (9º on example). In this example, there was internal rotation of the femoral condyles, and therefore, the distal angle was added to the proximal angle to determine the overall angle of torsion, resulting in 17º of femoral version. (MP4 3486 kb)
The effect of hip flexion on the lesser trochanter and femoral head positioning. In the example, the same femur is measured three times – in a position simulating no hip flexion, and in other two positions simulating increasing degrees of hip flexion. The movie clip aims to illustrate the femur of a patient laying in the CT scanner. To understand this example, the reader needs to imagine how the axial CT slices would look like in the three different positions. In the first position, the patient lays flat on the table, and the femoral condyles and femoral neck are aligned to the horizontal plane. The femoral head is anterior to the femoral neck, and the femoral version is measured as 16º. Both the 3D femur model method and the Murphy method would arrive to a similar measurement. In the following two positions, the patient lays down with the hips slightly flexed and substantially flexed, respectively. An increase in the hip flexion angle causes the femoral head to shift in relation to the base of the femoral neck (specifically, at the level of the lesser trochanter). The hip flexion positions the femoral head posteriorly to the femoral neck. If the second position were to be measured on CT slices via the Murphy method, the posteriorly positioned femoral head would result in an apparent retroversion, as depicted by the proximal angle being measured as -18º and the distal angle measured as 4º in external rotation, resulting in a femoral version of -22º. The third position further exaggerates this artifact by representing a patient laying with the hips substantially flexed. The increased flexion exaggerates the shift in position of the femoral head in regards to the femoral neck. The proximal angle becomes -33º and the distal angle becomes 8º in external rotation, resulting in a femoral version of -41º. The same femur had three different femoral version measurement based on different degrees of hip flexion, ranging from positive when the flexion was not present, to negative when it was. This explains the negative values observed in the flexed subgroup of our analysis. Since the entire length of the femur is not visible on the 2D axial slices, it becomes challenging to visualize and account for this false impression of retroversion. On the 3D femur model, the entire femur is seen and its position aligned to the horizontal plane, thus avoiding projectional misinterpretations and allowing accurate measurements of femoral version. (MP4 1137 kb)
Online Resources 4-6
(PDF 373 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Iwasaka-Neder, J., Bixby, S.D., Bedoya, M.A. et al. Virtual 3D femur model to assess femoral version: comparison to the 2D axial slice approach. Pediatr Radiol 53, 2411–2423 (2023). https://doi.org/10.1007/s00247-023-05758-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-023-05758-8