Abstract
Acute kidney injury (AKI) following cardiopulmonary bypass (CPB) is associated with increased morbidity and mortality. Serum Cystatin C (CysC) is a novel biomarker synthesized by all nucleated cells that may act as an early indicator of AKI following infant CPB. Prospective observational study of infants (< 1 year) requiring CPB during cardiac surgery. CysC was measured at baseline and 12, 24, 48, and 72 h following CPB initiation. Each post-op percent difference in CysC (e.g. %CysC12h) from baseline was calculated. Clinical variables along with urine output (UOP) and serum creatinine (SCr) were followed. Subjects were divided into two groups: AKI and non-AKI based upon the Kidney Disease Improving Global Outcomes (KDIGO) classification. AKI occurred in 41.9% (18) of the 43 infants enrolled. Patient demographics and baseline CysC levels were similar between groups. CysC levels were 0.97 ± 0.28 mg/L over the study period, and directly correlated with SCr (R = 0.71, p < 0.0001). Although absolute CysC levels were not significant between groups, the %CysC12h was significantly greater in the AKI group (AKI: − 16% ± 22% vs. Non-AKI − 28% ± 9% mg/L; p = 0.003). However, multivariate analysis demonstrated that a lower UOP (Odds Ratio:0.298; 95% CI 0.073, 0.850; p = 0.02) but not %CysC12h was independently associated with AKI. Despite a significant difference in the %CysC12h, only UOP was independently associated with AKI. Larger studies of a more homogenous population are needed to understand these results and to explore the variability in this biomarker seen across institutions.




Similar content being viewed by others
References
Hongsawong N, Khamdee P, Silvilairat S, Chartapisak W (2018) Prevalence and associated factors of renal dysfunction and proteinuria in cyanotic congenital heart disease. Pediatr Nephrol 33:493–501. https://doi.org/10.1007/s00467-017-3804-3
Zheng JY, Xiao YY, Yao Y, Han L (2013) Is serum cystatin C an early predictor for acute kidney injury following cardiopulmonary bypass surgery in infants and young children? Kaohsiung J Med Sci 29:494–499. https://doi.org/10.1016/j.kjms.2013.01.004
Greenberg JH, Zappitelli M, Jia Y, Thiessen-Philbrook HR, de Fontnouvelle CA, Wilson FP, Coca S, Devarajan P, Parikh CR (2018) Biomarkers of AKI progression after Pediatric Cardiac Surgery. J Am Soc Nephrol 29:1549–1556. https://doi.org/10.1681/ASN.2017090989
Algaze CA, Koth AM, Faberowski LW, Hanley FL, Krawczeski CD, Axelrod DM (2017) Acute kidney injury in patients undergoing the extracardiac fontan operation with and without the use of cardiopulmonary bypass. Pediatr Crit Care Med 18:34–43. https://doi.org/10.1097/PCC.0000000000000984
Beken S, Akbulut BB, Albayrak E, Guner B, Unlu Y, Temur B, Aydin S, Odemis E, Erek E, Korkmaz A (2021) Evaluation of neonatal acute kidney injury after critical congenital heart disease surgery. Pediatr Nephrol 36:1923–1929. https://doi.org/10.1007/s00467-020-04890-z
Li S, Krawczeski CD, Zappitelli M, Devarajan P, Thiessen-Philbrook H, Coca SG, Kim RW, Parikh CR, Consortium T-A (2011) Incidence, risk factors, and outcomes of acute kidney injury after pediatric cardiac surgery: a prospective multicenter study. Crit Care Med 39:1493–1499. https://doi.org/10.1097/CCM.0b013e31821201d3
Krawczeski CD, Goldstein SL, Woo JG, Wang Y, Piyaphanee N, Ma Q, Bennett M, Devarajan P (2011) Temporal relationship and predictive value of urinary acute kidney injury biomarkers after pediatric cardiopulmonary bypass. J Am Coll Cardiol 58:2301–2309. https://doi.org/10.1016/j.jacc.2011.08.017
Kellum JA, Lameire N (2012) KDIGO clinical practice guideline for acute kidney injury. Kidney Int. https://doi.org/10.1038/kisup.2012.2
Guignard JP, Drukker A (1999) Why do newborn infants have a high plasma creatinine? Pediatrics. https://doi.org/10.1542/peds.103.4.e49
Selewski DT, Charlton JR, Jetton JG, Guillet R, Mhanna MJ, Askenazi DJ, Kent AL (2015) Neonatal acute kidney injury. Pediatrics 136:e463-473. https://doi.org/10.1542/peds.2014-3819
Feldman H, Guignard JP (1982) Plasma creatinine in the first month of life. Arch Dis Child 57:123–126. https://doi.org/10.1136/adc.57.2.123
Finney H, Newman DJ, Thakkar H, Fell JME, Price CP (2000) Reference ranges for plasma cystatin C and creatinine measurements in premature infants, neonates, and older children. Arch Dis Child 82:71–75
Krawczeski CD, Vandevoorde RG, Kathman T, Bennett MR, Woo JG, Wang Y, Griffiths RE, Devarajan P (2010) Serum cystatin C is an early predictive biomarker of acute kidney injury after pediatric cardiopulmonary bypass. Clin J Am Soc Nephrol 5:1552–1557. https://doi.org/10.2215/CJN.02040310
Zappitelli M, Krawczeski CD, Devarajan P, Wang Z, Sint K, Thiessen-Philbrook H, Li S, Bennett MR, Ma Q, Shlipak MG, Garg AX, Parikh CR (2011) Early postoperative serum cystatin C predicts severe acute kidney injury following pediatric cardiac surgery. Kidney Int 80:655–662. https://doi.org/10.1038/ki.2011.123
Zappitelli M, Greenberg JH, Coca SG, Krawczeski CD, Li S, Thiessen-Philbrook HR, Bennett MR, Devarajan P, Parikh CR, Translational Research Investigating Biomarker Endpoints in Acute Kidney Injury C (2015) Association of definition of acute kidney injury by cystatin C rise with biomarkers and clinical outcomes in children undergoing cardiac surgery. JAMA Pediatr 169:583–591. https://doi.org/10.1001/jamapediatrics.2015.54
Wald R, Liangos O, Perianayagam MC, Kolyada A, Herget-Rosenthal S, Mazer CD, Jaber BL (2010) Plasma cystatin C and acute kidney injury after cardiopulmonary bypass. Clin J Am Soc Nephrol 5:1373–1379. https://doi.org/10.2215/CJN.06350909
O’Brien SM, Clarke DR, Jacobs JP, Jacobs ML, Lacour-Gayet FG, Pizarro C, Welke KF, Maruszewski B, Tobota Z, Miller WJ, Hamilton L, Peterson ED, Mavroudis C, Edwards FH (2009) An empirically based tool for analyzing mortality associated with congenital heart surgery. J Thorac Cardiovasc Surg 138:1139–1153. https://doi.org/10.1016/j.jtcvs.2009.03.071
Cholette JM, Swartz MF, Rubenstein J, Henrichs KF, Wang H, Powers KS, Daugherty LE, Alfieris GM, Gensini F, Blumberg N (2017) Outcomes using a conservative versus liberal red blood cell transfusion strategy in infants requiring cardiac operation. Ann Thorac Surg 103:206–214. https://doi.org/10.1016/j.athoracsur.2016.05.049
Holliday MA, Segar WE (1957) The maintenance need for water in parenteral fluid therapy. Pediatrics 19:823–832
Goldstein SL, Kirkendall E, Nguyen H, Schaffzin JK, Muething S (2013) Electronic health record identification of nephrotoxin exposure and associated acute kidney injury. Pediatrics 132:e756–e767. https://doi.org/10.1542/peds.2013-0794
Menon S, Goldstein SL, Mottes T, Fei L, Kaddourah A, Terrell T, Arnold P, Bennett MR, Basu RK (2016) Urinary biomarker incorporation into the renal angina index early in intensive care unit admission optimizes acute kidney injury prediction in critically ill children: a prospective cohort study. Nephrol Dial Transplant 31:586–594. https://doi.org/10.1093/ndt/gfv457
Nellis ME, Tucci M, Lacroix J, Spinella PC, Haque KD, Stock A, Steiner ME, Faustino EVS, Zantek ND, Davis PJ, Stanworth SJ, Cholette JM, Parker RI, Demaret P, Kneyber MCJ, Russell RT, Stricker PA, Vogel AM, Willems A, Josephson CD, Luban NLC, Loftis LL, Leteurtre S, Stocker CF, Goobie SM, Karam O, Pediatric Acute Lung I, Sepsis Investigators N, the Pediatric Critical Care Blood Research N (2019) Bleeding assessment scale in critically ill children (BASIC): physician-driven diagnostic criteria for bleeding severity. Crit Care Med 47:1766–1772. https://doi.org/10.1097/CCM.0000000000004025
Walsh MC, Kliegman RM (1986) Necrotizing enterocolitis: treatment based on staging criteria. Pediatr Clin North Am 33:179–201. https://doi.org/10.1016/s0031-3955(16)34975-6
Gaies MG, Gurney JG, Yen AH, Napoli ML, Gajarski RJ, Ohye RG, Charpie JR, Hirsch JC (2010) Vasoactive-inotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass. Pediatr Crit Care Med 11:234–238. https://doi.org/10.1097/PCC.0b013e3181b806fc
Schwartz GJ, Cox C, Seegmiller JC, Maier PS, DiManno D, Furth SL, Warady BA, Munoz A (2020) Recalibration of cystatin C using standardized material in Siemens nephelometers. Pediatr Nephrol 35:279–285. https://doi.org/10.1007/s00467-019-04389-2
Erlandsen EJ, Randers E, Kristensen JH (1999) Evaluation of the dade behring N latex cystatin C assay on the dade behring nephelometer II system. Scand J Clin Lab Invest 59:1–8. https://doi.org/10.1080/00365519950185940
Khwaja A (2012) KDIGO clinical practice guidelines for acute kidney injury. Nephron 120:c179–c184. https://doi.org/10.1159/000339789
Pierce CB, Muñoz A, Ng DK, Warady BA, Furth SL, Schwartz GJ (2021) Age- and sex-dependent clinical equations to estimate glomerular filtration rates in children and young adults with chronic kidney disease. Kidney Int 99:948–956. https://doi.org/10.1016/j.kint.2020.10.047
Akcan-Arikan A, Zappitelli M, Loftis LL, Washburn KK, Jefferson LS, Goldstein SL (2007) Modified RIFLE criteria in critically ill children with acute kidney injury. Kidney Int 71:1028–1035. https://doi.org/10.1038/sj.ki.5002231
Mehta RL, Kellum JA, Shah SV, Molitoris BA, Ronco C, Warnock DG, Levin A, the Acute Kidney Injury N (2007) Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care 11:R31. https://doi.org/10.1186/cc5713
Sutherland SM, Byrnes JJ, Kothari M, Longhurst CA, Dutta S, Garcia P, Goldstein SL (2015) AKI in hospitalized children: comparing the pRIFLE, AKIN, and KDIGO definitions. Clin J Am Soc Nephrol 10:554. https://doi.org/10.2215/CJN.01900214
Ristikankare A, Poyhia R, Kuitunen A, Skrifvars M, Hammainen P, Salmenpera M, Suojaranta-Ylinen R (2010) Serum cystatin C in elderly cardiac surgery patients. Ann Thorac Surg 89:689–694. https://doi.org/10.1016/j.athoracsur.2009.11.018
Koyner JL, Bennett MR, Worcester EM, Ma Q, Raman J, Jeevanandam V, Kasza KE, O’Connor MF, Konczal DJ, Trevino S, Devarajan P, Murray PT (2008) Urinary cystatin C as an early biomarker of acute kidney injury following adult cardiothoracic surgery. Kidney Int 74:1059–1069. https://doi.org/10.1038/ki.2008.341
Hassinger AB, Backer CL, Lane JC, Haymond S, Wang D, Wald EL (2012) Predictive power of serum cystatin C to detect acute kidney injury and pediatric-modified RIFLE class in children undergoing cardiac surgery. Pediatr Crit Care Med 13:435–440. https://doi.org/10.1097/PCC.0b013e318238b43c
Cantinotti M, Giordano R, Scalese M, Molinaro S, Storti S, Murzi B, Pak V, Poli V, Iervasi G, Clerico A (2017) Diagnostic accuracy and prognostic valued of plasmatic Cystatin-C in children undergoing pediatric cardiac surgery. Clin Chim Acta 471:113–118. https://doi.org/10.1016/j.cca.2017.05.031
Zhang Z, Lu B, Sheng X, Jin N (2011) Cystatin C in prediction of acute kidney injury: a systemic review and meta-analysis. Am J Kidney Dis 58:356–365. https://doi.org/10.1053/j.ajkd.2011.02.389
Nakhjavan-Shahraki B, Yousefifard M, Ataei N, Baikpour M, Ataei F, Bazargani B, Abbasi A, Ghelichkhani P, Javidilarijani F, Hosseini M (2017) Accuracy of cystatin C in prediction of acute kidney injury in children; serum or urine levels: which one works better? A systematic review and meta-analysis. BMC Nephrol 18:120. https://doi.org/10.1186/s12882-017-0539-0
Ho J, Tangri N, Komenda P, Kaushal A, Sood M, Brar R, Gill K, Walker S, MacDonald K, Hiebert BM, Arora RC, Rigatto C (2015) Urinary, plasma, and serum biomarkers’ utility for predicting acute kidney injury associated with cardiac surgery in adults: a meta-analysis. Am J Kidney Dis 66:993–1005. https://doi.org/10.1053/j.ajkd.2015.06.018
Bellomo R, Auriemma S, Fabbri A, D’Onofrio A, Katz N, McCullough PA, Ricci Z, Shaw A, Ronco C (2008) The pathophysiology of cardiac surgery-associated acute kidney injury (CSA-AKI). Int J Artif Organs 31:166–178. https://doi.org/10.1177/039139880803100210
Abu-Omar Y, Ratnatunga C (2006) Cardiopulmonary bypass and renal injury. Perfusion 21:209–213. https://doi.org/10.1191/0267659106pf870oa
Acknowledgements
We thank the Pediatric Cardiac Care Center Staff for their hard work in making this a success: (1) Nursing Staff for excellent communication and timely sample collection, (2) PICU and NICU Fellows, Attending Physicians and Advanced Practice Providers for their enthusiasm and dedication to all aspects of the project, (3) Partial financial support was awarded by: Clausen and Bradford Fellowship Award. University of Rochester Medical Center. Abadeer M, Cholette J. October 16, 2020. Status: Awarded. Amount: $25,000.
Funding
Partial funding for the study was provided by the Clausen and Bradford Fellowship Award. University of Rochester Medical Center. Abadeer M, Cholette J. October 16, 2020. Status: Awarded. Amount: $25,000.
Author information
Authors and Affiliations
Contributions
MA drafted/submitted the IRB proposal, organized, implemented and collected samples and data for the research study, applied for funding via the Clausen and Bradford Award, helped with data analysis and wrote the main manuscript text. MFS helped with editing several versions of the manuscript and performed the majority of complex data analysis, and created Figs. 1, 2, 3, 4, S1, S2, and S4, and Tables 5, S1, and S2. SDM helped with sample processing and revision of IRB proposal, and troubleshooting logistics for the study. AMG helped with establishing the study protocol, running sample analysis and troubleshooting logistical issues ALK was formerly the principal investigator, helped with editing the IRB proposal and manuscript, and supplied the laboratory space and freezer for sample processing. GJS helped with manuscript editing, and supplied the laboratory personnel and equipment for running serum cystatin C. He supplied expertise on the interpretation of serum cystatin C values and was an invaluable resource. PB helped with editing the IRB proposal, troubleshooting logistics and helped supply institutional funding for the study. GMA was the principal CT surgeon operating on subjects included in the study, and permitted study sample collection in the OR JMC is the current principal investigator, helped with multiple abstract and manuscript revisions, and troubleshooting logistics
Corresponding author
Ethics declarations
Conflict of interest
The individual authors listed have no relevant financial disclosures or conflicts of interest in relation to the content of this research. This study did receive financial funding as outlined above.
Informed Consent
Informed written consent was obtained from all parent guardians along with written assent or script assent from pediatric subjects when age-appropriate.
Research Involving Human Participants
Study approval was obtained from the Research Subjects Review Board to ensure that rights and welfare of human subjects is protected
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
246_2022_3080_MOESM1_ESM.jpeg
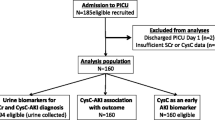
Fig. S1: Flow diagram of children who underwent a prospective observational trial to examine serum Cystatin C as a marker for Acute Kidney Injury (AKI). Abbreviations: ECMO-Extra-corporeal membrane oxygenation; CPB-Cardiopulmonary bypass. (JPEG 299 kb)
246_2022_3080_MOESM2_ESM.jpeg
Fig. S2: Box and Whisker Plots between infants that developed acute kidney injury (AKI-grey) and those who did not (no-AKI-white) demonstrate: S2a) The glomerular filtration rate (GFR) as estimated by Cystatin C (CysC), S2b) The percent change in GFR from baseline as estimated by CysC, S2c) The GFR as estimated by the serum creatinine (SCr), S2d) The percent change in GFR from baseline as estimated by SCr. *Denotes P value < 0.05. **Denotes P value of < 0.01 (JPEG 577 kb)
246_2022_3080_MOESM3_ESM.jpeg
Fig. S3 S3a) Linear regression (solid line) between 12 hour percent change in CysC (12hr-%CysC) and intra-operative net fluid balance (%), S3b) Linear regression (solid line) between %CysC12hr and hemofiltration volume towards end of cardiopulmonary bypass, S3c) Linear regression (solid line) between %CysC and net fluid balance for each subject during post-operative days (POD) 0 – 3, S3d) Linear regression (solid line) between mediastinal tube output and urine output on POD 0 – 2. Dotted lines reflect the 95% confidence intervals. (JPEG 542 kb)
246_2022_3080_MOESM4_ESM.jpeg
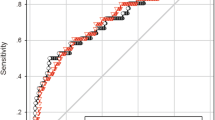
Fig. S4 Receiver operator characteristics curve utilizing the combination of urine output (UOP) and percent change of CysC at 12 hrs (12 hr %CysC) to predict AKI. Abbreviation: AUC-Area Under the Curve (JPEG 248 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Abadeer, M., Swartz, M.F., Martin, S.D. et al. Using Serum Cystatin C to Predict Acute Kidney Injury Following Infant Cardiac Surgery. Pediatr Cardiol 44, 855–866 (2023). https://doi.org/10.1007/s00246-022-03080-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-022-03080-y