Abstract
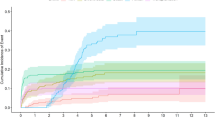
This retrospective cohort study aimed to explore the long-term outcomes of an individualized strategy in patients with pulmonary atresia and intact ventricular septum (PAIVS). We analyzed survival and reintervention rates and identified risk factors for outcomes in patients with PAIVS treated based on individual right heart structures between 1979 and 2019. Ninety-five patients were included in this study. The z-scores of the pulmonary annulus, tricuspid annulus, and right ventricular end-diastolic volume were − 3.30 (− 15.15 to 1.83), − 0.70 (− 4.65 to 2.33), and − 1.51 (− 6.35 to 1.18), respectively. Right ventricular-dependent coronary circulation occurred in 15% of the patients. Among the 63 patients attempting biventricular strategy at first, 55 patients achieved biventricular circulation, 3 patients had one-and-a-half circulation, and 4 patients died perioperatively. Among the 33 patients attempting univentricular strategy at first, 10 patients died before the completion of Fontan operation, 17 patients (48%) accomplished Fontan operation, and 5 patients waited for Fontan operation. In one patient, conversion to biventricular circulation occurred. During the follow-up period of 720 person-years, the 20-year survival rate was significantly higher in patients with biventricular circulation than in those patients with univentricular circulation (93% vs. 67%, P < 0.001). Freedom from reintervention rates at 20 years was significantly lower in patients with biventricular circulation than in those patients with univentricular circulation (29% vs. 72%, P < 0.001). The pulmonary annulus z-score was an independent risk factor for reintervention in patients with biventricular circulation. Patients with biventricular circulation had an acceptable survival rate, but a high reintervention rate. Meanwhile, patients with univentricular circulation had high mortality before the completion of Fontan operation, although the reintervention rate was relatively low.



Similar content being viewed by others
Data Availability
All data will be offered if applicable.
References
Daubeney PE, Wang D, Delany DJ, Keeton BR, Anderson RH, Slavik Z, Flather M, Webber SA, UK and Ireland Collaborative Study of Pulmonary Atresia with Intact Ventricular Septum (2005) Pulmonary atresia with intact ventricular septum: predictors of early and medium-term outcome in a population-based study. J Thorac Cardiovasc Surg 130:1071. https://doi.org/10.1016/j.jtcvs.2005.05.044
Hascoët S, Borrhomée S, Tahhan N, Petit J, Boet A, Houyel L, Lebret E, Ly M, Roussin R, Belli E, Lambert V, Laux D (2019) Transcatheter pulmonary valvuloplasty in neonates with pulmonary atresia and intact ventricular septum. Arch Cardiovasc Dis 112:323–333. https://doi.org/10.1016/j.acvd.2018.11.015
Kotani Y, Kasahara S, Fujii Y, Eitoku T, Baba K, Otsuki S, Kuroko Y, Arai S, Sano S (2016) A staged decompression of right ventricle allows growth of right ventricle and subsequent biventricular repair in patients with pulmonary atresia and intact ventricular septum. Eur J Cardiothorac Surg 50:298–303. https://doi.org/10.1093/ejcts/ezw124
Liava’a M, Brooks P, Konstantinov I, Brizard C, d’Udekem Y (2011) Changing trends in the management of pulmonary atresia with intact ventricular septum: the Melbourne experience. Eur J Cardiothorac Surg 40:1406–1411. https://doi.org/10.1016/j.ejcts.2011.02.036
Ashburn DA, Blackstone EH, Wells WJ, Jonas RA, Pigula FA, Manning PB, Lofland GK, Williams WG, McCrindle BW, Congenital Heart Surgeons Study Members (2004) Determinants of mortality and type of repair in neonates with pulmonary atresia and intact ventricular septum. J Thorac Cardiovasc Surg 127:1000–1007. https://doi.org/10.1016/j.jtcvs.2003.11.057
Hannan RL, Zabinsky JA, Stanfill RM, Ventura RA, Rossi AF, Nykanen DG, Zahn EM, Burke RP (2009) Midterm results for collaborative treatment of pulmonary atresia with intact ventricular septum. Ann Thorac Surg 87:1227–1233. https://doi.org/10.1016/j.athoracsur.2009.01.040
Cleuziou J, Schreiber C, Eicken A, Hörer J, Busch R, Holper K, Lange R (2010) Predictors for biventricular repair in pulmonary atresia with intact ventricular septum. Thorac Cardiovasc Surg 58:339–344. https://doi.org/10.1055/s-0030-1250101
Guleserian KJ, Armsby LB, Thiagarajan RR, del Nido PJ, Mayer JE Jr (2006) Natural history of pulmonary atresia with intact ventricular septum and right-ventricle-dependent coronary circulation managed by the single-ventricle approach. Ann Thorac Surg 81:2250–2257. https://doi.org/10.1016/j.athoracsur.2005.11.041
Yoshimura N, Yamaguchi M, Ohashi H, Oshima Y, Oka S, Yoshida M, Murakami H, Tei T (2003) Pulmonary atresia with intact ventricular septum: strategy based on right ventricular morphology. J Thorac Cardiovasc Surg 126:1417–1426. https://doi.org/10.1016/s0022-5223(03)01035-3
Wright LK, Knight JH, Thomas AS, Oster ME, St Louis JD, Kochilas LK (2019) Long-term outcomes after intervention for pulmonary atresia with intact ventricular septum. Heart 105:1007–1013. https://doi.org/10.1136/heartjnl-2018-314124
Shaath G, Al Mutairi M, Tamimi O, Alakhfash A, Abolfotouh M, Alhabshan F (2012) Predictors of reintervention in neonates with critical pulmonary stenosis or pulmonary atresia with intact ventricular septum. Catheter Cardiovasc Interv 79:659–664. https://doi.org/10.1002/ccd.23320
Schneider AW, Blom NA, Bruggemans EF, Hazekamp MG (2014) More than 25 years of experience in managing pulmonary atresia with intact ventricular septum. Ann Thorac Surg 98:1680–1686. https://doi.org/10.1016/j.athoracsur.2014.05.085
Schwartz MC, Glatz AC, Dori Y, Rome JJ, Gillespie MJ (2014) Outcomes and predictors of reintervention in patients with pulmonary atresia and intact ventricular septum treated with radiofrequency perforation and balloon pulmonary valvuloplasty. Pediatr Cardiol 35:22–29. https://doi.org/10.1007/s00246-013-0733-1
Humpl T, Söderberg B, McCrindle BW, Nykanen DG, Freedom RM, Williams WG, Benson LN (2003) Percutaneous balloon valvotomy in pulmonary atresia with intact ventricular septum: impact on patient care. Circulation 108:826–832. https://doi.org/10.1161/01.CIR.0000084548.44131.D1
Petit CJ, Glatz AC, Qureshi AM, Sachdeva R, Maskatia SA, Justino H, Goldberg DJ, Mozumdar N, Whiteside W, Rogers LS, Nicholson GT, McCracken C, Kelleman M, Goldstein BH (2017) Outcomes after decompression of the right ventricle in infants with pulmonary atresia with intact ventricular septum are associated with degree of tricuspid regurgitation: results from the congenital catheterization research collaborative. Circ Cardiovasc Interv 10:e004428. https://doi.org/10.1161/CIRCINTERVENTIONS.116.004428
Acknowledgements
We would like to thank the Editage (www.editage.com) for English language editing.
Funding
This research received no grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
JM designed and conducted this study and described the first draft. YS, HD, TF, MK, and HE collected catheterization and echocardiographic data. YS also contributed to data analysis. MW and YO critically reviewed this manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflict of interest to declare.
Ethical Approval
This retrospectively single-institutional cohort study was approved by the Institutional Ethics Committee of Kyushu Hospital, Japan Community Healthcare Organization (approval number 695).
Consent to Participate
In all subjects, their parents or guardians provided informed consent for the procedures, but informed consent for this cohort study was waived owing to the retrospective nature.
Consent for Publication
All authors approved this publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Muneuchi, J., Watanabe, M., Sugitani, Y. et al. Long-Term Outcomes After an Individualized Strategy in Patients with Pulmonary Atresia and Intact Ventricular Septum. Pediatr Cardiol 43, 435–442 (2022). https://doi.org/10.1007/s00246-021-02740-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-021-02740-9