Abstract
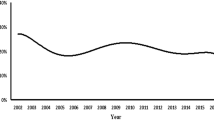
Without surgical treatment, neonatal hypoplastic left heart syndrome (HLHS) mortality in the first year of life exceeds 90 % and, in spite of improved surgical outcomes, many families still opt for non-surgical management. The purpose of this study was to investigate trends in neonatal HLHS management and to identify characteristics of patients who did not undergo surgical palliation. Neonates with HLHS were identified from a serial cross-sectional analysis using the Healthcare Cost and Utilization Project’s Kids’ Inpatient Database from 2000 to 2012. The primary analysis compared children undergoing surgical palliation to those discharged alive without surgery using a binary logistic regression model. Multivariate logistic regression was conducted to determine factors associated with treatment choice. A total of 1750 patients underwent analysis. Overall hospital mortality decreased from 35.3 % in 2000 to 22.9 % in 2012. The percentage of patients undergoing comfort care discharge without surgery also decreased from 21.2 to 14.8 %. After controlling for demographics and comorbidities, older patients at presentation were less likely to undergo surgery (OR 0.93, 0.91–0.96), and patients in 2012 were more likely to undergo surgery compared to those in prior years (OR 1.5, 1.1–2.1). Discharge without surgical intervention is decreasing with a 30 % reduction between 2000 and 2012. Given the improvement in surgical outcomes, further dialogue about ethical justification of non-operative comfort or palliative care is warranted. In the meantime, clinicians should present families with surgical outcome data and recommend intervention, while supporting their option to refuse.
Similar content being viewed by others
Abbreviations
- HLHS:
-
Hypoplastic left heart syndrome
- ICD9-CM:
-
International Classification of Diseases, Ninth Revision, Clinical Modification
- KID:
-
Healthcare Cost and Utilization Project’s Kids’ Inpatient Database
References
Atallah J, Dinu IA, Joffe AR et al (2008) Two-year survival and mental and psychomotor outcomes after the Norwood procedure: an analysis of the modified Blalock-Taussig shunt and right ventricle-to-pulmonary artery shunt surgical eras. Circulation 118:1410–1418
Bailey L (1985) Role of cardiac replacement in the neonate. J Heart Transplant. 4:506–509
Botto LD, Correa A, Erickson JD (2001) Racial and temporal variations in the prevalence of heart defects. Pediatrics 107:E32
Boucek RJ, Chrisant M (2004) Cardiac transplantation for hypoplastic left heart syndrome. Cardiol Young 14:83–87
Chang RKR, Chen AY, Klitzner TS (2002) Clinical management of infants with hypoplastic left heart syndrome in the United States, 1988–1997. Pediatrics 110:292–298
Ellinger MK, Rempel GR (2010) Parental decision making regarding treatment of hypoplastic left heart syndrome. Adv Neonatal Care. 10(6):316–322
Galantowicz M, Cheatham JP (2005) Lessons learned from the development of a new hybrid strategy for the management of hypoplastic left heart syndrome. Pediatr Cardiol, 26:190–199. Erratum in Pediatr Cardiol 2005;26:307
Goldberg CS, Mussatto K, Licht D, Wernovsky G (2011) Neurodevelopment and quality of life for children with hypoplastic left heart syndrome: current knowns and unknowns. Cardiol Young 21(suppl 2):88–92
Hill SL, Galantowicz M, Cheatham JP (2003) Emerging strategies in the treatment of HLHS: combined transcatheter and surgical techniques. Pediatr Cardiol Today. 1:1–4
Hoehn KS, Wernovsky G, Rychik J et al (2004) Parental decision-making in congenital heart disease. Cardiol Young 14:1–6
Jacobs JP, O’Brien SM, Chai PJ, Morell VO, Lindberg HL, Quintessenza JA (2008) Management of 239 patients with hypoplastic left heart syndrome and related malformations from 1993 to 2007. Ann Thorac Surg 85:1691–1697
Jenkins KJ, Gauvreau K, Newburger JW, Spray TL, Moller JH, Iezzoni LI (2002) Consensus-based method for risk adjustment for surgery for congenital heart disease. J Thorac Cardiovasc Surg 123:110–118
Karamlou T, Diggs BS, Ungerleider RM, Welke KF (2010) Evolution of treatment options and outcomes for hypoplastic left heart syndrome over an 18-year period. J Thorac Cardiovasc Surg 139:119–127
Kon AA (2008) Healthcare providers must offer palliative treatment to parents of neonates with hypoplastic left heart syndrome. Arch Pediatr Adolesc Med 162(9):844–848
Kon AA, Prsa M, Rohlicek CV (2013) Choices doctors would make if their infant had hypoplastic left heart syndrome: comparison of survey data from 1999 and 2007. Pediatr Cardiol 34(2):348–353
Mercurio MR, Peterec SM, Weeks B (2008) Hypoplastic left heart syndrome, extreme prematurity, comfort care only, and the principle of justice. Pediatrics 122:186–189
Morris SA, Ethen MK, Penny DJ et al (2014) Prenatal diagnosis, birth location, surgical center, and neonatal mortality in infants with hypoplastic left heart syndrome. Circulation 129(3):285–292
Norwood W, Kirklin J (1980) Hypoplastic left heart syndrome: experience with palliative surgery. Am J Cardiol 45:87–91
Norwood W, Lang P, Casteneda A, Campbell D (1981) Experience with operations for hypoplastic left heart syndrome. JThorac Cardiovasc Surg. 82:511–519
Norwood WI, Lang P, Hansen DD (1983) Physiologic repair of aortic atresia-hypoplastic left heart syndrome. N Engl J Med 308:23–26
Osiovich H, Phillipos E, Byrne P, Robertson M (2000) Hypoplastic left heart syndrome: “to treat or not to treat”. J Perinatol 20(6):363–365
Prsa M, Holly CD, Carnevale FA, Justino H, Rohlicek CV (2010) Attitudes and practices of cardiologists and surgeons who manage HLHS. Pediatrics 125(3):e625–e630
Ross LF, Frader J (2009) Hypoplastic left heart syndrome: a paradigm case for examining conscientious objection in pediatric practice. J Pediatr 155:12–15
Tabbutt S, Nord AS, Jarvik GP et al (2008) Neurodevelopmental outcomes after staged palliation for hypoplastic left heart syndrome. Pediatrics 121:476–483
Tabbutt S, Ghanayem N, Ravishankar C et al (2012) Risk factors for hospital morbidity and mortality after the Norwood procedure: a report from the pediatric heart network single ventricle reconstruction trial. J Thorac Cardiovasc Surg 144(4):882–895
The Kids’ Inpatient Database. Healthcare cost and utilization project (HCUP) website. http://www.hcup-us.ahrq.gov/kidoverview.jsp. Accessed 1 July 2015
Wernovsky G (2008) The paradigm shift toward surgical intervention for neonates with hypoplastic left heart syndrome. Arch Pediatr Adolesc Med 162(9):849–853
Wernovsky G, Ghanayem N, Ohye RG et al (2007) Hypoplastic left heart syndrome: consensus and controversies in 2007. Cardiol Young 17(Suppl 2):75–86
Yates AR, Hoffman TM, Boettner B, Feltes TF, Cua CL (2011) Initial counseling prior to palliation for hypoplastic left heart syndrome. Congenit Heart Dis 6(4):347–358
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial relationships relevant to this article to disclose. The authors have no conflicts of interest relevant to this article to disclose.
Rights and permissions
About this article
Cite this article
Kane, J.M., Canar, J., Kalinowski, V. et al. Management Options and Outcomes for Neonatal Hypoplastic Left Heart Syndrome in the Early Twenty-First Century. Pediatr Cardiol 37, 419–425 (2016). https://doi.org/10.1007/s00246-015-1294-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-015-1294-2