Abstract
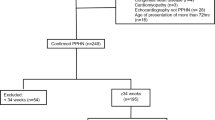
Persistent pulmonary hypertension of the newborn (PPHN) is associated with high morbidity and mortality. This study evaluated clinical outcomes in PPHN in relation to echocardiographic (EC) markers, score of neonatal acute physiology, perinatal extension, version II (SNAPPE II) scores, inotropic agent use, and the amount of fluid received as boluses. In this retrospective chart analysis of 98 neonates with PPHN born at >34 weeks’ gestation, we compared two cohorts of newborns: those who received inhaled nitric oxide and mechanical ventilation only, and who survived to discharge (Group 1); and those who required extracorporeal membrane oxygenation (ECMO) or who died (Group 2). Of 21 EC parameters assessed, seven were significantly different between Group 1 and Group 2. Eleven (24.4 %) newborns in Group 2 had decreased left ventricular (LV) function, compared with three (5.1 %) in Group 1 (p = 0.011). Median SNAPPE II scores were significantly higher in Group 2 than in Group 1 (p < 0.001). Newborns in Group 2 also received a significantly higher amount of fluid as boluses during the first 7 days of hospitalization compared with Group 1 (p = 0.018). Following logistic regression analysis, only the difference in total SNAPPE II score retained statistical significance (p < 0.001); however, the total amount of fluid administered as boluses trended higher (p = 0.087) for newborns in Group 2. Our findings show that SNAPPE II scores may help guide counseling for parents of newborns with PPHN regarding the likelihood of death or the need for ECMO. Limiting fluid boluses may improve outcomes in newborns with high SNAPPE II scores and decreased LV function.
Similar content being viewed by others
Abbreviations
- EC:
-
Echocardiogram
- ECMO:
-
Extracorporeal membrane oxygenation
- EF:
-
Ejection fraction
- FDA:
-
Food and drug administration
- FS:
-
Shortening fraction
- HIE:
-
Hypoxic ischemic encephalopathy
- iNO:
-
Inhaled nitric oxide
- IVSd:
-
Interventricular septal wall thickness in diastole
- IVSs:
-
Interventricular septal wall thickness in systole
- LA:
-
Left atrial
- LV:
-
Left ventricular
- LVIDd:
-
Left ventricular diastolic diameter
- LVPWd:
-
Left ventricular posterior wall thickness in diastole
- LVPWs:
-
Left ventricular posterior wall thickness in systole
- MAS:
-
Meconium aspiration syndrome
- PA:
-
Pulmonary artery
- PDA:
-
Patent ductus arteriosus
- PPHN:
-
Persistent pulmonary hypertension of the newborn
- RA:
-
Right atrial
- RAP:
-
Right atrial pressure
- RDS:
-
Respiratory distress syndrome
- RV:
-
Right ventricular
- RVDd:
-
Right ventricular diastolic diameter
- RVSP:
-
Right ventricular systolic pressure
- SNAPPE II:
-
Score for neonatal acute physiology, perinatal extension, version II
- TR:
-
Tricuspid regurgitation
- TRPG:
-
Tricuspid regurgitation pressure gradient
References
Abman SH et al (2013) Implications of the U.S. Food and Drug Administration warning against the use of sildenafil for the treatment of pediatric pulmonary hypertension. Am J Respir Crit Care Med 187(6):572–575
Bassler D et al (2010) Milrinone for persistent pulmonary hypertension of the newborn. Cochrane Database Syst Rev 11:CD007802
Bennett CC et al (2001) UK collaborative randomised trial of neonatal extracorporeal membrane oxygenation: follow-up to age 4 years. Lancet 357(9262):1094–1096
Cabral JE, Belik J (2013) Persistent pulmonary hypertension of the newborn: recent advances in pathophysiology and treatment. J Pediatr (Rio J) 89(3):226–242
Carcillo JA, Davis AL, Zaritsky A (1991) Role of early fluid resuscitation in pediatric septic shock. JAMA 266(9):1242–1245
Chang SM et al (2007) Pulmonary hypertension and left heart function: insights from tissue Doppler imaging and myocardial performance index. Echocardiography 24(4):366–373
Choi DY et al (2010) Respiratory variation in aortic blood flow velocity as a predictor of fluid responsiveness in children after repair of ventricular septal defect. Pediatr Cardiol 31(8):1166–1170
Evans N, Kluckow M, Currie A (1998) Range of echocardiographic findings in term neonates with high oxygen requirements. Arch Dis Child Fetal Neonatal Ed 78(2):F105–F111
Foland JA et al (2004) Fluid overload before continuous hemofiltration and survival in critically ill children: a retrospective analysis. Crit Care Med 32(8):1771–1776
Fraisse A et al (2004) Doppler echocardiographic predictors of outcome in newborns with persistent pulmonary hypertension. Cardiol Young 14(3):277–283
Konduri GG, Kim UO (2009) Advances in the diagnosis and management of persistent pulmonary hypertension of the newborn. Pediatr Clin North Am 56(3):579–600
Kumar D et al (2004) Predicting outcome in neonatal hypoxic respiratory failure with the score for neonatal acute physiology (SNAP) and highest oxygen index (OI) in the first 24 hours of admission. J Perinatol 24(6):376–381
Lakshminrusimha S et al (2009) Milrinone enhances relaxation to prostacyclin and iloprost in pulmonary arteries isolated from lambs with persistent pulmonary hypertension of the newborn. Pediatr Crit Care Med 10(1):106–112
Lemson J, Nusmeier A, van der Hoeven JG (2011) Advanced hemodynamic monitoring in critically ill children. Pediatrics 128(3):560–571
Marik PE et al (2009) Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: a systematic review of the literature. Crit Care Med 37(9):2642–2647
Nakwan N, Wannaro J (2011) Predicting mortality in infants with persistent pulmonary hypertension of the newborn with the Score for Neonatal Acute Physiology-Version II (SNAP-II) in Thai neonates. J Perinat Med 39(3):311–315
Ochikubo CG et al (1997) Echocardiographic evidence of improved hemodynamics during inhaled nitric oxide therapy for persistent pulmonary hypertension of the newborn. Pediatr Cardiol 18(4):282–287
Peterson AL et al (2009) Correlation of echocardiographic markers and therapy in persistent pulmonary hypertension of the newborn. Pediatr Cardiol 30(2):160–165
Richardson DK et al (2001) SNAP-II and SNAPPE-II: simplified newborn illness severity and mortality risk scores. J Pediatr 138(1):92–100
Skinner JR, Hunter S, Hey EN (1996) Haemodynamic features at presentation in persistent pulmonary hypertension of the newborn and outcome. Arch Dis Child Fetal Neonatal Ed 74(1):F26–F32
St John Sutton MG, Meyer RA (1983) Left ventricular function in persistent pulmonary hypertension of the newborn. Computer analysis of the echocardiogram. Br Heart J 50(6):540–549
Steinhorn RH (2010) Neonatal pulmonary hypertension. Pediatr Crit Care Med 11(2 Suppl):S79–S84
Steinhorn RH, Abman SH (2012) Persistent pulmonary hypertension. In: Devaskar SU, Gleason CA (eds) Avery’s diseases of the newborn. Elsevier, Philadelphia, pp 732–740
Storme L et al (2013) Pathophysiology of persistent pulmonary hypertension of the newborn: impact of the perinatal environment. Arch Cardiovasc Dis 106(3):169–177
Su BH, Peng CT, Tsai CH (2001) Persistent pulmonary hypertension of the newborn: echocardiographic assessment. Acta Paediatr Taiwan 42(4):218–223
Teng RJ, Wu TJ (2013) Persistent pulmonary hypertension of the newborn. J Formos Med Assoc 112(4):177–184
Valdes-Cruz LM, Dudell GG, Ferrara A (1981) Utility of M-mode echocardiography for early identification of infants with persistent pulmonary hypertension of the newborn. Pediatrics 68(4):515–525
Acknowledgments
We wish to thank Dr. Kamat, Professor of Pediatrics at the Children’s Hospital of Michigan, and Dr. Naheed, Division Chair of Pediatric Cardiology at John H Stroger Jr Hospital of Cook County for their valuable suggestions.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mydam, J., Zidan, M. & Chouthai, N.S. A Comprehensive Study of Clinical Biomarkers, Use of Inotropic Medications and Fluid Resuscitation in Newborns with Persistent Pulmonary Hypertension. Pediatr Cardiol 36, 233–239 (2015). https://doi.org/10.1007/s00246-014-0992-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-014-0992-5