Abstract
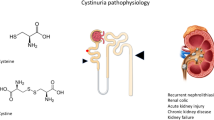
Cystinuria, a genetic disorder of cystine transport, is characterized by excessive excretion of cystine in the urine and recurrent cystine stones in the kidneys and, to a lesser extent, in the bladder. Males generally are more severely affected than females. The disorder may lead to chronic kidney disease in many patients. The cystine transporter (b0,+) is a heterodimer consisting of the rBAT (encoded by SLC3A1) and b0,+AT (encoded by SLC7A9) subunits joined by a disulfide bridge. The molecular basis of cystinuria is known in great detail, and this information is now being used to define genotype–phenotype correlations. Current treatments for cystinuria include increased fluid intake to increase cystine solubility and the administration of thiol drugs for more severe cases. These drugs, however, have poor patient compliance due to adverse effects. Thus, there is a need to reduce or eliminate the risks associated with therapy for cystinuria. Four mouse models for cystinuria have been described and these models provide a resource for evaluating the safety and efficacy of new therapies for cystinuria. We are evaluating a new approach for the treatment of cystine stones based on the inhibition of cystine crystal growth by cystine analogs. Our ongoing studies indicate that cystine diamides are effective in preventing cystine stone formation in the Slc3a1 knockout mouse model for cystinuria. In addition to crystal growth, crystal aggregation is required for stone formation. Male and female mice with cystinuria have comparable levels of crystalluria, but very few female mice form stones. The identification of factors that inhibit cystine crystal aggregation in female mice may provide insight into the gender difference in disease severity in patients with cystinuria.
Similar content being viewed by others
References
Andreassen KH, Pedersen KV, Osther SS, Jung HU, Lildal SK, Osther PJ (2016) How should patients with cystine stone disease be evaluated and treated in the twenty-first century? Urolithiasis 44:65–76. https://doi.org/10.1007/s00240-015-0841-x
Edvardsson VO, Goldfarb DS, Lieske JC, Beara-Lasic L, Anglani F, Milliner DS, Palsson R (2013) Hereditary causes of kidney stones and chronic kidney disease. Pediatr Nephrol 28:1923–1942. https://doi.org/10.1007/s00467-012-2329-z
Eggermann T, Venghaus A, Zerres K (2012) Cystinuria: an inborn cause of urolithiasis. Orphanet J Rare Dis 7:19. https://doi.org/10.1186/1750-1172-7-19
Pereira DJ, Schoolwerth AC, Pais VM (2015) Cystinuria: current concepts and future directions. Clin Nephrol 83:138–146
Saravakos P, Kokkinou V, Giannatos E (2014) Cystinuria: current diagnosis and management. Urology 83:693–699. https://doi.org/10.1016/j.urology.2013.10.013
Sumorok N, Goldfarb DS (2013) Update on cystinuria. Curr Opin Nephrol Hypertens 22:427–431. https://doi.org/10.1097/MNH.0b013e3283621c5d
Thomas K, Wong K, Withington J, Bultitude M, Doherty A (2014) Cystinuria-a urologist’s perspective. Nat Rev Urol 11:270–277. https://doi.org/10.1038/nrurol.2014.51
Biyani CS, Cartledge JJ (2006) Cystinuria—diagnosis and management. EAU-EBU Update Ser 4:175–183
Schwartz BF, Stoller ML (2000) The vesical calculus. Urol Clin N A 27:333–346
Schwentner C, Oswald J, Lunacek A, Bartsch G, Radmayr C (2005) Giant cystine stone in an infant bladder with no evidence of cystinuria-valence of possible pathomechanisms. Urol Int 75:285–287. https://doi.org/10.1159/000087810
Ahmed K, Dasgupta P, Khan MS (2006) Cystine calculi: challenging group of stones. Postgrad Med J 82:799–801. https://doi.org/10.1136/pgmj.2005.044156
Knoll T, Zollner A, Wendt-Nordahl G, Michel MS, Alken P (2005) Cystinuria in childhood and adolescence: recommendations for diagnosis, treatment, and follow-up. Pediatr Nephrol 20:19–24. https://doi.org/10.1007/s00467-004-1663-1
Asatoor AM, Freedman PS, Gabriel JR, Milne MD, Prosser DI, Roberts JT, Willoughby CP (1974) Amino acid imbalance in cystinuria. J Clin Pathol 27:500–504
Hellier MD, Perrett D, Holdsworth CD (1970) Dipeptide absorption in cystinuria. Br Med J 4:782–783
Goldstein B, Goldfarb DS (2017) Early recognition and management of rare kidney stone disorders. Urol Nurs 37:81–89, 102
Rhodes HL, Yarram-Smith L, Rice SJ, Tabaksert A, Edwards N, Hartley A, Woodward MN, Smithson SL, Tomson C, Welsh GI, Williams M, Thwaites DT, Sayer JA, Coward RJ (2015) Clinical and genetic analysis of patients with cystinuria in the United Kingdom. CJASN 10:1235–1245. https://doi.org/10.2215/cjn.10981114
Wong KA, Mein R, Wass M, Flinter F, Pardy C, Bultitude M, Thomas K (2015) The genetic diversity of cystinuria in a UK population of patients. BJU Int 116:109–116. https://doi.org/10.1111/bju.12894
Barbey F, Joly D, Rieu P, Mejean A, Daudon M, Jungers P (2000) Medical treatment of cystinuria: critical reappraisal of long-term results. J Urol 163:1419–1423
Moore SL, Somani BK, Cook P (2018) Journey of a cystinuric patient with a long-term follow-up from a medical stone clinic: necessity to be SaFER (stone and fragments entirely removed). Urolithiasis. https://doi.org/10.1007/s00240-018-1059-5
Prot-Bertoye C, Lebbah S, Daudon M, Tostivint I, Bataille P, Bridoux F, Brignon P, Choquenet C, Cochat P, Combe C, Conort P, Decramer S, Dore B, Dussol B, Essig M, Gaunez N, Joly D, Le Toquin-Bernard S, Mejean A, Meria P, Morin D, N’Guyen HV, Noel C, Normand M, Pietak M, Ronco P, Saussine C, Tsimaratos M, Friedlander G, Traxer O, Knebelmann B, Courbebaisse M (2015) CKD and Its risk factors among patients with cystinuria. CJASN 10:842–851. https://doi.org/10.2215/cjn.06680714
Nalcacioglu H, Ozden E, Genc G, Yakupoglu YK, Sarikaya S, Ozkaya O (2013) An uncommon cause of acute kidney injury in young children: cystinuria. J Pediatr Urol 9:e58–e63. https://doi.org/10.1016/j.jpurol.2012.08.006
Assimos DG, Leslie SW, Ng C, Streem SB, Hart LJ (2002) The impact of cystinuria on renal function. J Urol 168:27–30
Goldfarb DS (2011) Potential pharmacologic treatments for cystinuria and for calcium stones associated with hyperuricosuria. CJASN 6:2093–2097. https://doi.org/10.2215/cjn.00320111
Font-Llitjos M, Jimenez-Vidal M, Bisceglia L, Di Perna M, de Sanctis L, Rousaud F, Zelante L, Palacin M, Nunes V (2005) New insights into cystinuria: 40 new mutations, genotype–phenotype correlation, and digenic inheritance causing partial phenotype. J Med Genet 42:58–68. https://doi.org/10.1136/jmg.2004.022244
Gaildrat P, Lebbah S, Tebani A, Sudrie-Arnaud B, Tostivint I, Bollee G, Tubeuf H, Charles T, Bertholet-Thomas A, Goldenberg A, Barbey F, Martins A, Saugier-Veber P, Frebourg T, Knebelmann B, Bekri S (2017) Clinical and molecular characterization of cystinuria in a French cohort: relevance of assessing large-scale rearrangements and splicing variants. Mol Genet Genom Med 5:373–389. https://doi.org/10.1002/mgg3.294
Stenson PD, Mort M, Ball EV, Evans K, Hayden M, Heywood S, Hussain M, Phillips AD, Cooper DN (2017) The human gene mutation database: towards a comprehensive repository of inherited mutation data for medical research, genetic diagnosis and next-generation sequencing studies. Hum Genet 136:665–677. https://doi.org/10.1007/s00439-017-1779-6
Johri N, Cooper B, Robertson W, Choong S, Rickards D, Unwin R (2010) An update and practical guide to renal stone management. Nephron Clin Pract 116:c159–171. https://doi.org/10.1159/000317196
DeBerardinis RJ, Coughlin CRII, Kaplan P (2008) Penicillamine therapy for pediatric cystinuria: experience from a cohort of American children. J Urol 180:2620–2623. https://doi.org/10.1016/j.juro.2008.08.057
Wood K, Keys T, Mufarrij P, Assimos DG (2011) Impact of stone removal on renal function: a review. Rev Urol 13:73–89
Asplin JR, Penniston K, Goldfarb DS (2013) Monosodium urate stones are rare, and urine pH is not low in cystinuria. Am J Kidney Dis 62:179–180. https://doi.org/10.1053/j.ajkd.2013.03.041
Zee T, Bose N, Zee J, Beck JN, Yang S, Parihar J, Yang M, Damodar S, Hall D, O’Leary MN, Ramanathan A, Gerona RR, Killilea DW, Chi T, Tischfield J, Sahota A, Kahn A, Stoller ML, Kapahi P (2017) α-Lipoic acid treatment prevents cystine urolithiasis in a mouse model of cystinuria. Nat Med 23:288–290. https://doi.org/10.1038/nm.4280
Erickson SB, Vrtiska TJ, Canzanello VJ, Lieske JC (2011) Cystone(R) for 1 year did not change urine chemistry or decrease stone burden in cystine stone formers. Urol Res 39:197–203. https://doi.org/10.1007/s00240-010-0334-x
Modersitzki F, Pizzi L, Grasso M, Goldfarb DS (2014) Health-related quality of life (HRQoL) in cystine compared with non-cystine stone formers. Urolithiasis 42:53–60. https://doi.org/10.1007/s00240-013-0621-4
Parr JM, Desai D, Winkle D (2015) Natural history and quality of life in patients with cystine urolithiasis: a single centre study. BJU Int 116(Suppl 3):31–35. https://doi.org/10.1111/bju.13169
Streeper NM, Wertheim ML, Nakada SY, Penniston KL (2017) Cystine stone formers have impaired health-related quality of life compared with noncystine stone formers: a case-referent study piloting the Wisconsin stone quality of life questionnaire among patients with cystine stones. J Endourology 31(S1):S48–Ss53. https://doi.org/10.1089/end.2016.0564
Chabrol B, Martens K, Meulemans S, Cano A, Jaeken J, Matthijs G, Creemers JW (2009) Deletion of C2orf34, PREPL and SLC3A1 causes atypical hypotonia-cystinuria syndrome. BMJ Case Rep. https://doi.org/10.1136/bcr.08.2008.0719
Martens K, Jaeken J, Matthijs G, Creemers JW (2008) Multi-system disorder syndromes associated with cystinuria type I. Curr Mol Med 8:544–550
Parvari R, Brodyansky I, Elpeleg O, Moses S, Landau D, Hershkovitz E (2001) A recessive contiguous gene deletion of chromosome 2p16 associated with cystinuria and a mitochondrial disease. Am J Hum Genet 69:869–875. https://doi.org/10.1086/323624
de Rojas T, Aparicio C, de Lucas C, Martinez B, Gil-Fournier B, Ramiro-Leon S (2016) Cystinuria in a patient with 19q12q13.1 deletion. CEN Case Rep 5:67–69. https://doi.org/10.1007/s13730-015-0193-y
Lee EH, Kim YH, Hwang JS, Kim SH (2010) Non-type I cystinuria associated with mental retardation and ataxia in a Korean boy with a new missense mutation (G173R) in the SLC7A9 gene. J Korean Med Sci 25:172–175. https://doi.org/10.3346/jkms.2010.25.1.172
Tohge R, Sakamoto S, Takahashi M (2016) A case of cystinuria presenting with cerebellar ataxia and dementia. Pract Neurol 16:296–299. https://doi.org/10.1136/practneurol-2016-001374
Astrea G, Munteanu I, Cassandrini D, Lillis S, Trovato R, Pegoraro E, Cioni G, Mercuri E, Muntoni F, Battini R (2015) A diagnostic dilemma in a family with cystinuria type B resolved by muscle magnetic resonance. Pediatr Neurol 52:548–551. https://doi.org/10.1016/j.pediatrneurol.2015.01.018
Fu R, Ceballos-Picot I, Torres RJ, Larovere LE, Yamada Y, Nguyen KV, Hegde M, Visser JE, Schretlen DJ, Nyhan WL, Puig JG, O’Neill PJ, Jinnah HA (2014) Genotype–phenotype correlations in neurogenetics: Lesch–Nyhan disease as a model disorder. Brain 137:1282–1303. https://doi.org/10.1093/brain/awt202
Wambach JA, Casey AM, Fishman MP, Wegner DJ, Wert SE, Cole FS, Hamvas A, Nogee LM (2014) Genotype–phenotype correlations for infants and children with ABCA3 deficiency. Am J Resp Crit Care Med 189:1538–1543. https://doi.org/10.1164/rccm.201402-0342OC
Kim JH, Park E, Hyun HS, Lee BH, Kim GH, Lee JH, Park YS, Kang HG, Ha IS, Cheong HI (2017) Genotype and phenotype analysis in pediatric patients with cystinuria. J Korean Med Sci 32:310–314. https://doi.org/10.3346/jkms.2017.32.2.310
Mahdavi M, Koulivand L, Khorrami M, Mirsafaie M, Kheirollahi M (2018) In silico analysis of SLC3A1 and SLC7A9 mutations in Iranian patients with cystinuria. Mol Biol Rep. https://doi.org/10.1007/s11033-018-4269-6
Martell HJ, Wong KA, Martin JF, Kassam Z, Thomas K, Wass MN (2017) Associating mutations causing cystinuria with disease severity with the aim of providing precision medicine. BMC Genom 18(Suppl 5):550. https://doi.org/10.1186/s12864-017-3913-1
Wong KA, Wass M, Thomas K (2016) The role of protein modelling in predicting the disease severity of cystinuria. Eur Urol 69:543–544. https://doi.org/10.1016/j.eururo.2015.10.039
Tostivint I, Royer N, Nicolas M, Bourillon A, Czerkiewicz I, Becker PH, Muller F, Benoist JF (2017) Spectrum of mutations in cystinuria patients presenting with prenatal hyperechoic colon. Clin Genet 92:632–638. https://doi.org/10.1111/cge.13079
Kato T (1977) Renal handling of dibasic amino acids and cystine in cystinuria. Clin Sci Mol Med 53:9–15
Stephens AD, Perrett D (1976) Cystinuria: a new genetic variant. Clin Sci Mol Med 51:27–32
Brodehl J, Gellissen K, Kowalewski S (1967) Isolated cystinuria (without lysin-, ornithin and argininuria) in a family with hypocalcemic tetany. Monatsschrift fur Kinderheilkunde 115:317–320
Chillaron J, Roca R, Valencia A, Zorzano A, Palacin M (2001) Heteromeric amino acid transporters: biochemistry, genetics, and physiology. Am J Physiol Renal Physiol 281:F995–F1018. https://doi.org/10.1152/ajprenal.2001.281.6.F995
Fernandez E, Carrascal M, Rousaud F, Abian J, Zorzano A, Palacin M, Chillaron J (2002) rBAT-b(0,+)AT heterodimer is the main apical reabsorption system for cystine in the kidney. Am J Physiol Renal Physiol 283:F540–F548. https://doi.org/10.1152/ajprenal.00071.2002
Feliubadalo L, Arbones ML, Manas S, Chillaron J, Visa J, Rodes M, Rousaud F, Zorzano A, Palacin M, Nunes V (2003) Slc7a9-deficient mice develop cystinuria non-I and cystine urolithiasis. Hum Mol Genet 12:2097–2108. https://doi.org/10.1093/hmg/ddg228
Di Giacopo A, Rubio-Aliaga I, Cantone A, Artunc F, Rexhepaj R, Frey-Wagner I, Font-Llitjos M, Gehring N, Stange G, Jaenecke I, Mohebbi N, Closs EI, Palacin M, Nunes V, Daniel H, Lang F, Capasso G, Wagner CA (2013) Differential cystine and dibasic amino acid handling after loss of function of the amino acid transporter b0,+AT (Slc7a9) in mice. Am J Physiol Renal Physiol 305:F1645–F1655. https://doi.org/10.1152/ajprenal.00221.2013
Nagamori S, Wiriyasermkul P, Guarch ME, Okuyama H, Nakagomi S, Tadagaki K, Nishinaka Y, Bodoy S, Takafuji K, Okuda S, Kurokawa J, Ohgaki R, Nunes V, Palacin M, Kanai Y (2016) Novel cystine transporter in renal proximal tubule identified as a missing partner of cystinuria-related plasma membrane protein rBAT/SLC3A1. Proc Natl Acad Sci 113:775–780. https://doi.org/10.1073/pnas.1519959113
Ercolani M, Sahota A, Schuler C, Yang M, Evan AP, Reimer D, Barone JG, Tischfield JA, Levin RM (2010) Bladder outlet obstruction in male cystinuria mice. Int Urol Nephrol 42:57–63. https://doi.org/10.1007/s11255-009-9597-y
Livrozet M, Vandermeersch S, Mesnard L, Thioulouse E, Jaubert J, Boffa JJ, Haymann JP, Baud L, Bazin D, Daudon M, Letavernier E (2014) An animal model of type A cystinuria due to spontaneous mutation in 129S2/SvPasCrl mice. PloS One 9:e102700. https://doi.org/10.1371/journal.pone.0102700
Peters T, Thaete C, Wolf S, Popp A, Sedlmeier R, Grosse J, Nehls MC, Russ A, Schlueter V (2003) A mouse model for cystinuria type I. Hum Mol Genet 12:2109–2120. https://doi.org/10.1093/hmg/ddg189
Espino M, Font-Llitjos M, Vilches C, Salido E, Prat E, Lopez de Heredia M, Palacin M, Nunes V (2015) Digenic inheritance in cystinuria mouse model. PloS One 10:e0137277. https://doi.org/10.1371/journal.pone.0137277
Fattah H, Hambaroush Y, Goldfarb DS (2014) Cystine nephrolithiasis. Transl Androl Urol 3:228–233. https://doi.org/10.3978/j.issn.2223-4683.2014.07.04
Zisman AL, Evan AP, Coe FL, Worcester EM (2015) Do kidney stone formers have a kidney disease? Kidney Int 88:1240–1249. https://doi.org/10.1038/ki.2015.254
Slavkovic A, Radovanovic M, Siric Z, Vlajkovic M, Stefanovic V (2002) Extracorporeal shock wave lithotripsy for cystine urolithiasis in children: outcome and complications. Int Urol Nephrol 34:457–461
Gurdal M, Ayyildiz A, Huri E, Kanberoglu H, Karaman MI (2003) A huge bladder cystine stone. Int Urol Nephrol 35:497–499
O’Regan S, Robitaille P, Mongeau JG, Homsy Y (1980) Cystine calcium bladder calculus in a 2-year-old child. J Urol 123:770
Mizukami K, Raj K, Osborne C, Giger U (2016) Cystinuria associated with different SLC7A9 gene variants in the cat. PloS One 11:e0159247. https://doi.org/10.1371/journal.pone.0159247
Salido EC, Li XM, Lu Y, Wang X, Santana A, Roy-Chowdhury N, Torres A, Shapiro LJ, Roy-Chowdhury J (2006) Alanine-glyoxylate aminotransferase-deficient mice, a model for primary hyperoxaluria that responds to adenoviral gene transfer. Proc Natl Acad Sci 103:18249–18254. https://doi.org/10.1073/pnas.0607218103
Font-Llitjos M, Feliubadalo L, Espino M, Cleries R, Manas S, Frey IM, Puertas S, Colell G, Palomo S, Aranda J, Visa J, Palacin M, Nunes V (2007) Slc7a9 knockout mouse is a good cystinuria model for antilithiasic pharmacological studies. Am J Physiol Renal Physiol 293:F732–F740. https://doi.org/10.1152/ajprenal.00121.2007
Hu L, Yang Y, Aloysius H, Albanyan H, Yang M, Liang JJ, Yu A, Shtukenberg A, Poloni LN, Kholodovych V, Tischfield JA, Goldfarb DS, Ward MD, Sahota A (2016) l-Cystine diamides as l-cystine crystallization inhibitors for cystinuria. J Med Chem 59:7293–7298. https://doi.org/10.1021/acs.jmedchem.6b00647
Lee MH, Sahota A, Ward MD, Goldfarb DS (2015) Cystine growth inhibition through molecular mimicry: a new paradigm for the prevention of crystal diseases. Curr Rheumatol Rep 17:33. https://doi.org/10.1007/s11926-015-0510-7
Poloni LN, Zhu Z, Garcia-Vazquez N, Yu AC, Connors DM, Hu L, Sahota A, Ward MD, Shtukenberg AG (2017) Role of molecular recognition in l-cystine crystal growth inhibition. Cryst Growth Design 17:2767–2781. https://doi.org/10.1021/acs.cgd.7b00236
Sahota A, Parihar JS, Capaccione KM, Yang M, Noll K, Gordon D, Reimer D, Yang I, Buckley BT, Polunas M, Reuhl KR, Lewis MR, Ward MD, Goldfarb DS, Tischfield JA (2014) Novel cystine ester mimics for the treatment of cystinuria-induced urolithiasis in a knockout mouse model. Urology 84:1249.e1249–1249.e1215. https://doi.org/10.1016/j.urology.2014.07.043
Shim M, Park HK (2014) Multimodal treatments of cystine stones: an observational, retrospective single-center analysis of 14 cases. Korean J Urol 55:515–519. https://doi.org/10.4111/kju.2014.55.8.515
Mandal T, Ward MD (2013) Determination of specific binding interactions at L-cystine crystal surfaces with chemical force microscopy. J Am Chem Soc 135:5525–5528. https://doi.org/10.1021/ja401309d
Rimer JD, An Z, Zhu Z, Lee MH, Goldfarb DS, Wesson JA, Ward MD (2010) Crystal growth inhibitors for the prevention of l-cystine kidney stones through molecular design. Science 330:337–341. https://doi.org/10.1126/science.1191968
Shtukenberg AG, Zhu Z, An Z, Bhandari M, Song P, Kahr B, Ward MD (2013) Illusory spirals and loops in crystal growth. Proc Natl Acad Sci 110:17195–17198. https://doi.org/10.1073/pnas.1311637110
Yang Y, Albanyan H, Lee S, Aloysius H, Liang JJ, Kholodovych V, Sahota A, Hu L (2018) Design, synthesis, and evaluation of l-cystine diamides as l-cystine crystallization inhibitors for cystinuria. Bioorg Med Chem Lett. https://doi.org/10.1016/j.bmcl.2018.03.024
Claes DJ, Jackson E (2012) Cystinuria: mechanisms and management. Pediatr Nephrol 27:2031–2038. https://doi.org/10.1007/s00467-011-2092-6
Coe FL, Evan A, Worcester E (2005) Kidney stone disease. J Clin Invest 115:2598–2608
Masotti A, Laurenzi C, Boenzi S, Pastore A, Taranta A, Bellomo F, Muraca M, Dionisi-Vici C, Bertucci P, Dello Strologo L, Emma F (2014) Gender-related effects on urine l-cystine metastability. Amino Acids 46:415–427. https://doi.org/10.1007/s00726-013-1631-9
Aggarwal KP, Narula S, Kakkar M, Tandon C (2013) Nephrolithiasis: molecular mechanism of renal stone formation and the critical role played by modulators. Biomed Res Int 292953:21. https://doi.org/10.1155/2013/292953
Baumann JM, Affolter B (2014) From crystalluria to kidney stones, some physicochemical aspects of calcium nephrolithiasis. World J Nephrol 3:256–267
Khan SR, Pearle MS, Robertson WG, Gambaro G, Canales BK, Doizi S, Traxer O, Tiselius H-G (2017) Kidney stones. Nat Rev Dis Primers 2:16008. https://doi.org/10.1038/nrdp.2016.8
Rimer JD, Kolbach-Mandel AM, Ward MD, Wesson JA (2017) The role of macromolecules in the formation of kidney stones. Urolithiasis 45:57–74. https://doi.org/10.1007/s00240-016-0948-8
Ratkalkar VN, Kleinman JG (2011) Mechanisms of Stone Formation. Clin Rev Bone Miner Metabol 9:187–197. https://doi.org/10.1007/s12018-011-9104-8
Wesson JA, Ganne V, Beshensky AM, Kleinman JG (2005) Regulation by macromolecules of calcium oxalate crystal aggregation in stone formers. Urol Res 33:206–212. https://doi.org/10.1007/s00240-004-0455-1
Funding
This work was supported in part by the Human Genetics Institute of New Jersey and by NIH Grant R01DK112782.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Goldfarb has received consulting fees from Retrophin. The other authors declare that they have no relevant financial interests. The work described in this manuscript on cystine diamides has been licensed by Rutgers University to PharmaKrysto. Rutgers University is the assignee of Patent Number US 9,248,453 B2 entitled “Cystine diamide analogs for the prevention of cystine stone formation in cystinuria” and New York University is the assignee of Patent Number US 8,450,089 B2 entitled “Compounds as L-cystine crystallization inhibitors and uses thereof”.
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the Institutional Animal Care and Use Committee of Rutgers University.
Rights and permissions
About this article
Cite this article
Sahota, A., Tischfield, J.A., Goldfarb, D.S. et al. Cystinuria: genetic aspects, mouse models, and a new approach to therapy. Urolithiasis 47, 57–66 (2019). https://doi.org/10.1007/s00240-018-1101-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-018-1101-7