Abstract
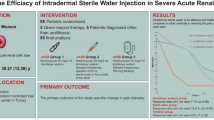
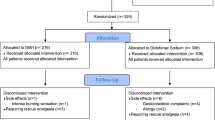
The aim of the study is to determine whether dermal scarification is equally effective for treating acute renal colic compared to diclofenac sodium intramuscular therapy. A prospective, randomized controlled study was conducted with methodologic rigor based on CONSORT criteria. A total of 291 patients, aged ≥18 years, suffering from acute renal colic were included in this trial and randomly assigned in two groups. Patients in the first group (A) received endodermal injection (dermal scarification) of 1 ml normal saline at the area of intensity of pain. The second group (B) received 75 mg diclofenac sodium by intramuscular injection. The success of each method defined the primary end point. Pain intensity before and after treatment was assessed using a visual analog scale. The time onset and the duration of analgesia were also recorded. There was no significant difference between the two groups regarding hematuria (p = 0.158), stone identification at KUB (p = 0.751) and mean pain intensity (p = 0.609) before treatment initiation. The method was successful in 75.5 % of patients in group A and 74.3 % of patients in group B (p = 0.812). Mean pain reduction was comparable, 5.65 ± 3.05 in group A and 5.34 ± 2.99 in group B (p = 0.379), with dermal scarification eliciting its effect considerably faster, whereas the duration of analgesia was longer in the diclofenac group (p < 0.05). In conclusion, dermal scarification could constitute an alternative method for treating renal colic as it is equally effective compared to the standard treatment of diclofenac sodium.



Similar content being viewed by others
References
Davenport K, Timoney AG, Keeley FX (2005) Conventional and alternative methods for providing analgesia in renal colic. BJU Int 95(3):297–300
Holdgate A, Pollock T (2004) Systematic review of the relative efficacy of non-steroidal anti-inflammatory drugs and opioids in the treatment of acute renal colic. BMJ 328(7453):1401
Shokeir AA, Abdulmaaboud M, Farage Y et al (1999) Resistive index in renal colic: the effect of nonsteroidal anti-inflammatory drugs. BJU Int 84(3):249–251
Schulz KF, Altman DG, Moher D, CONSORT Group (2010) CONSORT statement: updated guidelines for reporting parallel group randomised trials. BMJ 340:332
Asgari SA, Asli MM, Madani AH et al (2012) Treatment of loin pain suspected to be renal colic with papaverine hydrochloride: a prospective double-blind randomised study. BJU Int 110(3):449–452
Holdgate A, Pollock T (2005) Nonsteroidal anti-inflammatory drugs (NSAIDs) versus opioids for acute renal colic. Cochrane Database Syst Rev 18(2):CD004137
International Association for the study of Pain (2011) Classification of pain. IASP Press, Seattle
Zhao ZQ (2006) Neural mechanism underlying acupuncture analgesia. Prog Neurol 85(4):355–375
Chang S (2013) The meridian system and mechanism of acupuncture—a comparative review. Part 2: mechanism of acupuncture analgesia. Taiwan J Obstet Gynecol 52(1):14–24
Melzack R, Wall PD (1965) Pain mechanism, a new theory. Science 150:91
Lee YH, Lee WC, Chen MT, Huang JK, Chung C, Chang LS (1992) Acupuncture in the treatment of renal colic. J Urol 147:16–18
Pyne D, Shenker NG (2008) Demystifying acupuncture. Rheumatology 47:1132–1136
Han JS (2003) Acupuncture: neuropeptide release produced by electrical stimulation of different frequencies. Trends Neurosci 26:17–22
Stux G, Pomeranz B (1991) Basics of acupuncture. Springer, Berlin, pp 6–7
Mt Cabyoglu, Ergene N, Tan U (2006) The mechanism of acupuncture and clinical applications. Int J Neurosci 11(2):115–125
Kober A, Dobrovits M, Djavan B et al (2003) Local active warming: an effective treatment for pain, anxiety and nausea caused by renal colic. J Urol 170(3):741–744
Ju BJ, Niu LL (2012) Analysis of therapeutic effect of acupuncture at neiguan (PC 6) and zusanli (ST 36) on acute renal colic. Zhongguo Zhen Jiu 32(11):975–978
Lin Q, Hu YL, Han CW, Li Y (2007) Eye acupuncture for treatment of renal and ureteral colic. Zhongguo Zhen Jiu 27(9):663–664
Iguchi M, Katoh Y, Koike H, Hayashi T, Nakamura M (2002) Randomized trial of trigger point injection for renal colic. Int J Urol 9(9):475–479
Maikranz P, Coe FL, Parks J, Lindheimer MD (1987) Nephrolithiasis in pregnancy. Am J Kidney Dis 9(4):354–358
Nugent-Head A (2013) Ashi points in clinical practice. J Chin Med 101:5–12
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ioannidis, S., Kampantais, S., Ioannidis, A. et al. Dermal scarification versus intramuscular diclofenac sodium injection for the treatment of renal colic: a prospective randomized clinical trial. Urolithiasis 42, 527–532 (2014). https://doi.org/10.1007/s00240-014-0690-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-014-0690-z