Abstract
Purpose
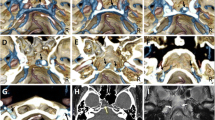
Although the craniocervical junction has a complex anatomical structure associated with clinical diseases, its ventral venous network has not been well studied. This study aimed to clarify the extracranial ventral venous structure at the craniocervical junction.
Methods
Head computed tomography digital subtraction venography (CT-DSV) images of 273 patients (age 6 months to 93 years) taken at our department were retrospectively analyzed. We analyzed the frequency and anatomical features of the venous channels, as well as their upstream and downstream connections with the surrounding channels at the ventral craniocervical junction, from the level of the hypoglossal canal to the second cervical vertebra.
Results
In 54% of the cases, the vein descended from the anterior condylar confluence, running medially along the basioccipital and fusing with its counterpart in the midline at the level of the atlanto-occipital membrane. Furthermore, 24% of this vein was connected caudally to the anterior external vertebral venous plexus. We also identified venous channels, either as a sole vein or venous plexus, on the tip of the odontoid process (10%), which has not been well described previously. The vein around the odontoid process was connected to several veins, including the aforementioned vein anterior to the condyle and the anterior internal vertebral venous plexus.
Conclusions
CT-DSV analysis revealed a detailed venous architecture ventral to the craniocervical junction. Venous structures identified in this study may be involved in diseases in this area.



Similar content being viewed by others
Abbreviations
- ACC:
-
Anterior condylar confluence
- AEVVP:
-
Anterior external vertebral venous plexus
- AIVVP:
-
Anterior internal vertebral venous plexus
- CT-DSV:
-
Computed tomography digital subtraction venography
- CCJ:
-
Craniocervical junction
- DAVF:
-
Dural arteriovenous fistula
- Pre-VVP:
-
Prevertebral venous plexus
References
San Millán Ruíz D, Gailloud P, Rüfenacht DA et al (2002) The craniocervical venous system in relation to cerebral venous drainage. AJNR Am J Neuroradiol 23:1500–1508
Tanoue S, Kiyosue H, Sagara Y et al (2010) Venous structures at the craniocervical junction: anatomical variations evaluated by multidetector row CT. Br J Radiol 83:831–840
Tubbs RS, Demerdash A, Loukas M et al (2018) Intracranial connections of the vertebral venous plexus: anatomical study with application to neurosurgical and endovascular procedures at the craniocervical junction. Oper Neurosurg (Hagerstown) 14:51–57
Carpenter K, Decater T, Iwanaga J et al (2021) Revisiting the Vertebral venous plexus-a comprehensive review of the literature. World Neurosurg 145:381–395
Takahashi S, Sakuma I, Omachi K et al (2005) Craniocervical junction venous anatomy around the suboccipital cavernous sinus: evaluation by MR imaging. Eur Radiol 15:1694–1700
Caruso RD, Rosenbaum AE, Chang JK, Joy SE (1999) Craniocervical junction venous anatomy on enhanced MR images: the suboccipital cavernous sinus. AJNR Am J Neuroradiol 20:1127–1131
Spittau B, Millán DS, El-Sherifi S et al (2015) Dural arteriovenous fistulas of the hypoglossal canal: systematic review on imaging anatomy, clinical findings, and endovascular management. J Neurosurg 122:883–903
Cyril C, Ofélia M, Hervé D (2013) Dural arteriovenous fistula involving the anterior condylar canal. J Neuroimaging 23:425–428
Miyachi S, Ohshima T, Izumi T et al (2008) Dural arteriovenous fistula at the anterior condylar confluence. Interv Neuroradiol 14:303–311
Signorelli F, Olivi A, De Giorgio F et al (2020) A 360° Approach to the Craniovertebral junction in a cadaveric laboratory setting: historical insights, current, and future perspectives in a comparative study. World Neurosurg 140:564–573
Mizutani K, Toda M, Kurasawa J et al (2017) Analysis of the venous channel within the clivus using multidetector computed tomography digital subtraction venography. Neuroradiology 59:213–219
de Oliveira E, Rhoton AL Jr, Peace D (1985) Microsurgical anatomy of the region of the foramen magnum. Surg Neurol 24:293–352
Schwaber MK, Netterville JL, Maciunas R (1990) Microsurgical anatomy of the lower skullbase–a morphometric analysis. Am J Otol 11:401–405
Funaki T, Matsushima T, Peris-Celda M et al (2013) Focal transnasal approach to the upper, middle, and lower clivus. Oper Neurosurg (Hagerstown) 73:ons155–ons191
Schaeffer JP (1953) Morris’ Human Anatomy, 11th ed. New York, NY: The BlakistonCompany.
Mizutani K, Akiyama T, Yoshida K (2019) The anterior condylar arteriovenous fistula from the viewpoint of the osseous venous anatomy. J Neuroendovascular Ther 13:97–104
Batson OV (1940) The function of the vertebral veins and their role in the spread of metastases. Ann Surg 112:138–149
Mizutani K, Akiyama T, Minami Y et al (2018) Intraosseous venous structures adjacent to the jugular tubercle associated with an anterior condylar dural arteriovenous fistula. Neuroradiology 60:487–496
Jung C, Kwon BJ, Kwon O-K et al (2009) Intraosseous cranial dural arteriovenous fistula treated with transvenous embolization. AJNR Am J Neuroradiol 30:1173–1177
Mizutani K, Toda M, Yoshida K (2015) Analysis of the intercavernous sinuses using multidetector computed tomography digital subtraction venography (CT-DSV). Clin Neurol Neurosurg 131:31–34
Scahill RI, Frost C, Jenkins R et al (2003) A longitudinal study of brain volume changes in normal aging using serial registered magnetic resonance imaging. Arch Neurol 60:989–994
Shin W, Horowitz S, Ragin A et al (2007) Quantitative cerebral perfusion using dynamic susceptibility contrast MRI: evaluation of reproducibility and age- and gender-dependence with fully automatic image postprocessing algorithm. Magn Reson Med 58:1232–1241
Buijs PC, Krabbe-Hartkamp MJ, Bakker CJ et al (1998) Effect of age on cerebral blood flow: measurement with ungated two-dimensional phase-contrast MR angiography in 250 adults. Radiology 209:667–674
Von Lüdinghausen M, Prescher A, Kageya I, Yoshimura K (2006) The median atlanto-occipital joint in advanced age. Spine 31:E430–E436
Peters B, Parizel PM, Van Goethem JW (2020) Age-related changes to the craniocervical ligaments in asymptomatic subjects: a prospective MR study. Eur Spine J 29:1029–1035
Favaloro EJ, Franchini M, Lippi G (2014) Aging hemostasis: changes to laboratory markers of hemostasis as we age - a narrative review. Semin Thromb Hemost 40:621–633
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
Funding
This research did not receive any specific grants from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the ethics committee of Keio University School of Medicine.
Consent to participate
This study waived the need for informed consent (given the study design) under the ethical standards of the 1964 Declaration of Helsinki and its later amendments.
Consent to publish
This study waived the need for informed consent (given the study design) under the ethical standards of the 1964 Declaration of Helsinki and its later amendments.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Presentation in meeting: The contents of this study were presented at the 37th Annual Meeting of the Japanese Society of Neuroendovascular Therapy.
Rights and permissions
About this article
Cite this article
Yamada, H., Mizutani, K., Akiyama, T. et al. Extracranial prevertebral venous network of the craniocervical junction: CT-digital subtraction venography analysis. Neuroradiology 64, 2227–2233 (2022). https://doi.org/10.1007/s00234-022-02980-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-02980-3